DIABETES INSULN VE ORAL ANTIDIABETICS EBRU ARIOLU NAN

DIABETES, INSULİN VE ORAL ANTIDIABETICS EBRU ARIOĞLU İNAN, Ph. D

Aims: Having knowledge about; • Pancreatic hormones and their roles • Diabetes • Types of diabetes • Antidiabetic drugs • Insulin types • Complications and adverse effects of insulin • Features, action of mechanism and adverse effects of all antidiabetic drugs • New drugs for diabetes

Content • • Pancreatic hormones Glucose metabolism Diabetes Types of diabetes Antidiabetic drugs Insulin New drugs

Pancreas, Islet of Langerhans • • Alpha cells; glucagon, proglucagon Beta cells; insulin, C peptid, proinsulin, amylin Delta cells; somatostatine Epsilon cells; ghreline

Type 1 Diabetes • • • Selective beta cell damage Partial/complete insulin secretion deficiency İmmun based or idiopathic Usually before age of 30 Weak genetic predisposition Insulin replacement

Type 2 diabetes • Relative insulin deficiency and insulin resistance • Insulin secretion is not effective because of insulin resistance on target tissues • Usually after age of 30 • Oral antidiabetics (insulin if needed) • Ketoasidosis is not seen but may occur due to infections, some drugs (glucocorticoids…), stress • Fatal nonketotic hyperosmolar coma due to dehydratation

Gestational diabetes • • Seen in pregnancy (prevalance %7) OGTT between weeks of 24 -28 Usually not seen after term Type 2 diabetes risk in the future

Gestational Diabetes • • Fasting BG> 95 mg/dl 1. hour BG>180 mg/dl 2. hour BG>155 mg/dl 3. hour BG>140 mg/dl • 100 g glucose loading • No diet or excercise for at least 3 days • After 14 -hour fasting • 2 values out of the range is enough for diagnosis

Diabetes insipidus • 1. neurogenic: due to antidiuretci hormon (ADH) deficiency • 2. nephrogenic: due to abolished sensitivity of the kidneys to ADH effect • 3. gestagenic: due to ADH deficiency in pregnancy • 4. dipsogenic: due to excessive thirst and fluid intake

Prediabetes • Fasting blood glucose: 100 -125 mg/dl • 75 g OGTT, 2 -hour BG 140 -199 mg/dl • Hb. A 1 C %5. 7 -6. 5

Diabetes • • Fasting blood glucose 126 mg/dl or higher 75 g OGTT, 2 -hour BG higher than 200 mg/dl’den fazladır Hb. A 1 C %6. 5 or higher Random BG 200 mg/dl or higher

Diabetic complications • • • Peripheral neuropathy Stroke Myocardical infarction Periphearl artery disease Diabetic retinopathy Cataract Glaucoma Diabetic foot Diabetic nephropathy

• Type 1 diabetes is treated with insulin • It is discovered by Banthing and Best

Insulin secretion Glucose is taken into beta cell by GLUT 2, it is converted to glucose-6 -phosphate by glucokinase, ATP sensitive K+ channels are closed due to increased ATP levels, depolarization occurs, Ca++ chanells are opened, Ca++ enters into the cell, insulin is secreted

Insulin in the circulation • 5 -15 μU 7 ml (30 -90 pmol/L), in healthy person • Increased to 60 -90μU/ml’ye (360 -540 pmol/L) after a meal

Metabolism of insulin • Metabolized in liver and kidney • Liver clears %60 of it • Kidney clears %35 -40 of it

Insulin receptor • Insulin receptor is abundant in the membranes of most of the tissues • Insulin is bound to receptor in picomolar levels with high affinity • Receptor has 2 heterodimers bound covalently, each heterodimer has one extracellular alpha unit and beta unit embedded to the membrane • Beta unit has tyrosinekinase activity • Receptor is activated when insulin is bound to alpha unit which causes a conformational change, beta units are getting closer, tyrosine part in the beta unit is phosphorylated, thyrosine kinases are directed to cytoplasmic proteins

IRS (insulin receptor substrate) • IRS, one of the cytoplasmic proteins which is phosphorylated by thyrosine kinases • After phosphorylation, IRS activates other kinases in the energy metabolism • It also stimulates mitogenic pathyways (Ras, MAPK system…)

Target tissues of insulin • Liver • Skeletal muscle • Adipose tissue

• After insulin is bound to its receptor, GLUTs (glucose transporters) is translocated to the membrane, act as a gate and bind glucose and takes into the cell • GLUT 1 (all tissues), GLUT 2 (pancreas beta cells, liver, kidney, gut), GLUT 3 (brain, placenta), GLUT 4 (muscle, adipose tissue), GLUT 5 (gut, kidney)

Effects of insulin In the liver: • Inhibition of glycogenolysis • Inhibition of convertion of fatty acides and aminoacides to keta acides • Inhibition of convertion of aminoacides to glucose • Storage of glucose as glycogen • Increased formation of VLDL and triglycerides

Effects of insulin In the skeletal muscle: • Increased protein synthesis • Increased aminoacide transport • Increased ribosomal protein synthesis • Increased glycogen synthesis • Increased glucose transport

Effects of insulin In the adipose tissue: Increased storage of triglyceride

Stimulatory factors of insulin secretion • Humoral: glucose, mannose, arginine, fatty acides, aminoacides • Neural: beta adrenergic stimulation, vagal stimulation • Drugs: sulphonylureas, meglitinides, isoprenaline, acetylcholine

Discovery of Insulin • Frederick Banting and Charles have discovered insulin in 1921 • First human trial on Leonard Thompson, 1922, it was succesfull • Nobel price in 1923 to the discovery of insulin

Diabetic ketoacidosis May be fatal Mostly seen in type 1 diabetes Rarely in type 2 diabetes (due to sepsis, pancreatitis, high dose steroids) The formation of ketoacids from fatty acids is increased, acidosis is observed Symptoms; nausea, vomiting, abdominal pain, deep breath (Kussmaul), altered mental status, increased keton and glucose in blood and urine • Blood p. H, 7. 3 or lower • Low bicarbonate levels • Treatment; agresive intravenous hydratation, insulin (reguler, iv), potasium and regulating the electrolyte balance • • •

Hiperosmolar hyperglycemic coma Mostly seen in T 2 DM Characterized with hyperglycemia and dehydratation Caused by inadequate fluid intake (geriatric patients) Phenytoin, steroids, diuretics, beta blockers, peritoneal dialysis, hemodialysis may result in this coma • Symptoms; impaired mental status, seizures, blood glucose is 600 mg/dl or higher, serum osmalility is higher than 320 mmol/l • No acidosis • Treatment; agresive rehydratation, reestablishing glucose and alectrolyte balance, low dose insulin treatment is possible. • •
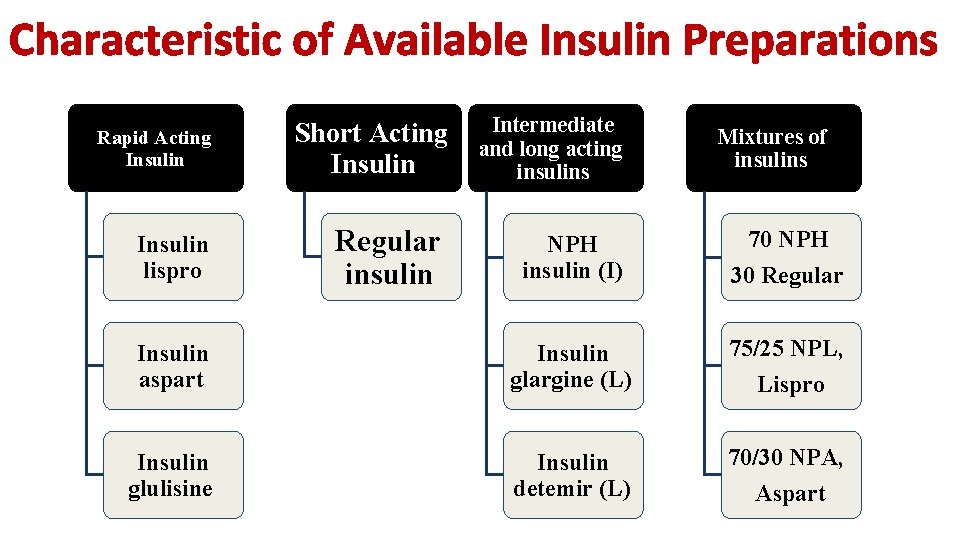
Characteristic of Available Insulin Preparations Short Acting Insulin Intermediate and long acting insulins Regular insulin NPH insulin (I) 70 NPH 30 Regular Insulin aspart Insulin glargine (L) 75/25 NPL, Lispro Insulin glulisine Insulin detemir (L) 70/30 NPA, Aspart Rapid Acting Insulin lispro Mixtures of insulins
Complication of Insulin Therapy Hypoglycemia Insulin allergy Immune insulin resistance Lipodystrophy Increased cancer risk

Inhaled Insulin The only inhaled insulin on the market is Afrezza. It's fast acting, so you take it only at mealtimes. It comes in 4 -unit and 8 -unit cartridges that you pop into a small gadget, like the ones people with asthma use. Those with asthma, COPD or who smoke should not use this medication. Long Acting Insulin degludec (Tresiba) is an injectable form of insulin that lasts up to 42 hours. It is used once daily for type 1 or type 2 diabetes. It also comes premixed with insulin aspart (Ryzodeg 70/30).
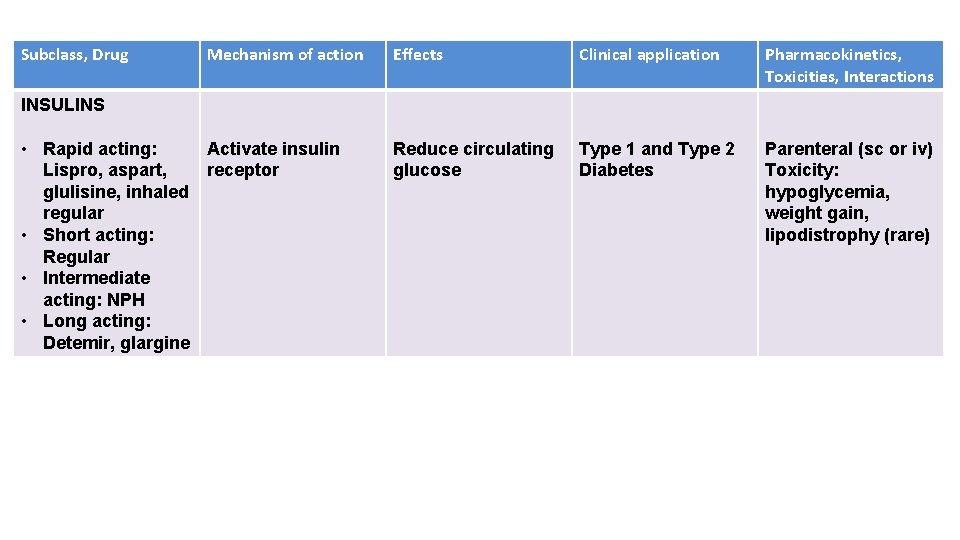
Subclass, Drug Mechanism of action Effects Clinical application Pharmacokinetics, Toxicities, Interactions Reduce circulating glucose Type 1 and Type 2 Diabetes Parenteral (sc or iv) Toxicity: hypoglycemia, weight gain, lipodistrophy (rare) INSULINS • Rapid acting: Activate insulin Lispro, aspart, receptor glulisine, inhaled regular • Short acting: Regular • Intermediate acting: NPH • Long acting: Detemir, glargine
- Slides: 31