Diabetes in Pregnancy Dr Hennie Lombaard Physiological changes

Diabetes in Pregnancy Dr Hennie Lombaard

Physiological changes • • Fasting glucose levels decreased Serum levels increased after a meal. Doubling of insulin production Anti–insulin hormones: – Human placental lactogen – Glucagon – Cortisol

Physiological changes • Renal tubular threshold decrease • In normal pregnancy starvation leads to a breakdown of triglyceride, this leads to liberation of fatty acids and ketone bodies.
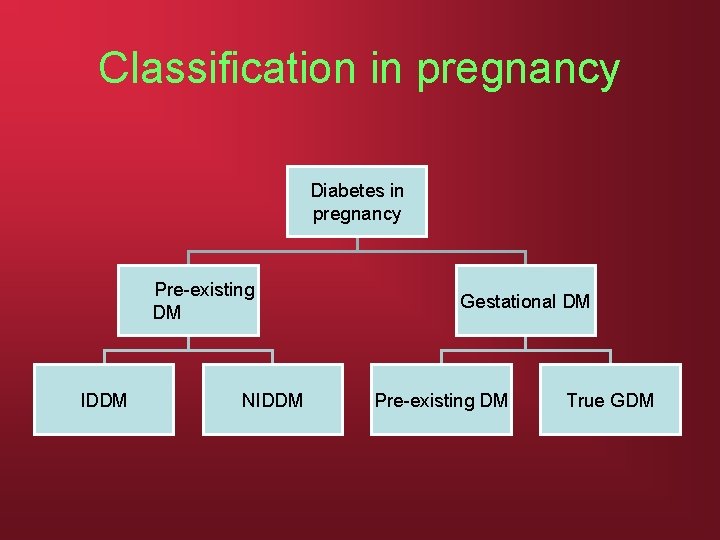
Classification in pregnancy Diabetes in pregnancy Pre-existing DM IDDM NIDDM Gestational DM Pre-existing DM True GDM

Diagnosis of Diabetes Mellitus • Random glucose: > 11, 1 mmol/l • Fasting plasma glucose > 7, 0 mmol/l • Hb. A 1 C >6. 5

Diagnosis of GDM • Fasting plasma glucose >5. 1 • OGTT 1 hour value: – >10 • OGTT 2 hour value: – >8. 5

Effect of pregnancy on pre-existing DM • Increase need of Insulin • Deterioration of nephropathy • 2 fold increased risk of deterioration in retinopathy • Hypoglycaemia more common • Women with autonomic neuropathy experience deterioration of their symptoms.

Effect of DM on pregnancy: • Increased risk of miscarriage • Increased risk of pre-eclampsia (1% increase in Hb. A 1 C cause a 60% increase in risk of PET) • DM nephropathy associated with normochromic normocytic anemia, severe oedema and proteinuria. • Increased c/section rate • Increased risk of infection.

Fetal complications of DM • Congenital abnormalities: HBA 1 c < 8% risk is 5% and HBA 1 c > 10% risk is 25% • • Increased neonatal mortality Increased perinatal mortality Macrosomia Late stillbirth Premature delivery Neonatal hypoglycaemia Polycytheamia Jaundice

Management: • Maternal near normal normoglycemia • Increased home glucose monitoring • Target values: – < 5, 0 – 5, 5 mmol/l capillary fasting – < 7, 0 – 7, 5 mmol/l post preandial. • Strict adherence to low-sugar, low-fat, high -fibre diet is important. Patients require 3 snacks.

Management: • Basal bolus regimen with short acting before meals and intermediate acting insulin at bedtime. • Opthalmological examination • FBC, UCE, 24 hr urine protein creatinine clearance and ECG. • Strict hypertension control.

Obstetric Management: • • • Early dating scan 11 - 14 weeks nuchal translucency scan 20 – 22 weeks detail anatomy scan Regular growth scans in the 3 rd trimester Pregnancies not allowed to continue past 40 weeks

Obstetric management: • The Academic Complex protocol: – If not macrosomic and good control: • Deliver at 38 weeks and if not confirm at 38 weeks with a positive PG – If a macrosomic fetus or poor control do PG from 35 weeks and deliver if mature

Intrapartum management: • IV dextrose infusion 500 ml/8 hr with short acting insulin and aim for capillary glucose of 5 -8 mmol/l • Do hourly sliding scale. • Give potassium replacement or check potassium regularly. • After delivery of the placenta half the insulin infusion.

Contra indications for pregnancy: • • Ischaemic heart disease Untreated proliferative retinopathy Severe gastroparesis Severe renal impairment

Gestational diabetes mellitus: • Definition: National Diabetes Data Group (1985) – Carbohydrate intolerance of variable severity with onset or first recognition during the present pregnancy.

Clinical features: • Asymptomatic and develop in the 2 nd or 3 rd trimester • More commonly diagnosed in women: – A family history of DM – Previous large-for-gestational-age infants – Obesity – Advanced maternal age – Certain ethnic groups

Importance of GDM: • Women dx with GDM at increased risk for type 2 DM • Some women have pre-existing DM • GDM is associated with adverse pregnancy outcome

Screening: Clinical risk factors: • Previous GDM • Family history of DM • Previous macrosomic baby • Previous unexplained stillbirths • • Obesity Glycosuria Polyhydramnios Large-for-gestationalage infants • Certain ethnic groups.

Management: • • Diet advice the same as for DM Obese women get a calorie reduced diet Home glucose monitoring Persistent hyperglycaemia an indication to start insulin. Fasting > 5, 5 mmol/l or post prandial > 7, 5 -8, 0 mmol/l • Metformin can be used in pregnancy • Glibenclamide does not cross the placenta and may be an alternative

Intrapartum management: • Women on oral or low insulin do not need continuous insulin therapy. • Women on large insulin needs continuous insulin therapy. • Women with GDM require a formal OGTT 6 weeks after delivery

Hypertension in Pregnancy

Physiological changes • Decrease in BP in 1 st trimester until the 22 nd to 24 th week of pregnancy • BP drops immediately post partum

Risk factors • General – Age – Obesity • Genetic – If their mother had PET risk is 25% – If a woman’s sister had PET her risk is 3540%

• Obstertirc factors – Primiparity (2 -3 fold risk) – Multiple pregnancy (2 fold) – Previous PET (7 fold) – Long birth interval (2 -3 fold if 10 years) – Hydrops – Hydatiforme mole – Triploidy

• Medical factors – Pre-existing hypertension – Renal disease – Diabetes – Antiphosfolipid antibodies – Connective tissue disorders – Inherited thrombophilia

Diagnosis: • Systolic BP > 140 mm. Hg or a diastolic BP > 90 mm. Hg on more than 2 occasions at least 6 hours apart • A BP of more than 160/110 mm. Hg • For gestational or pre-eclampsia it is with onset after 20 weeks.

Diagnosis PET • Hypertension with onset of 1 of the following: – Renal impairment – Liver impairment – Haematological impairment – Neurological impairment – Growth restriction

Management: STABILIZATION: Admit High Care Obstetrics Unit Intra venous line: Ringer lactate 100 ml bolus ivi over 20 min (The normal 300 ml bolus is made up out of 100 ml Ringers lactate and 200 ml Saline) Magnesium Sulphate FLUID MANAGEMENT 4 gr Magnesium sulphate in 200 ml saline over 20 min ivi 5 gr Magnesium sulphate with 1 ml Lignocaine imi in each buttock. If any is absent Delay second doses with another 4 hours or only give half t If signs of over dose he dose. Maintenance: 5 gr four hourly Check before next dosage: Urine output > 30 ml/hr Tendon reflexes present Respiratory rate more than 16/min If signs of over dose Give calcium gluconate
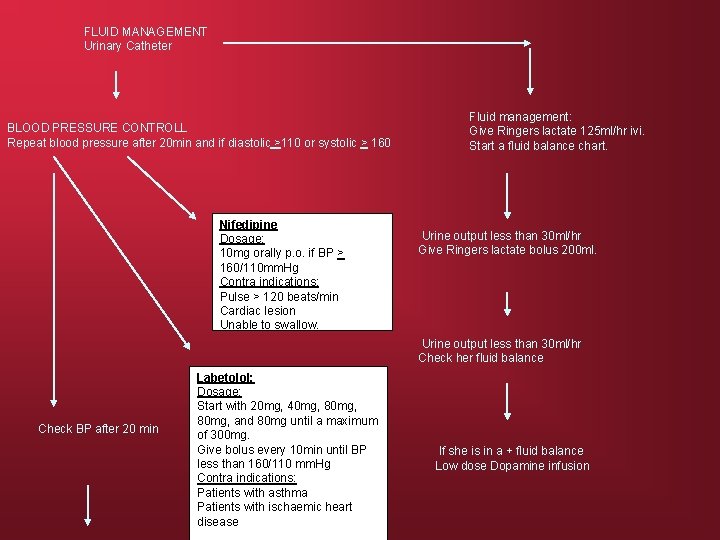
FLUID MANAGEMENT Urinary Catheter BLOOD PRESSURE CONTROLL Repeat blood pressure after 20 min and if diastolic >110 or systolic > 160 Nifedipine Dosage: 10 mg orally p. o. if BP > 160/110 mm. Hg Contra indications: Pulse > 120 beats/min Cardiac lesion Unable to swallow. Fluid management: Give Ringers lactate 125 ml/hr ivi. Start a fluid balance chart. Urine output less than 30 ml/hr Give Ringers lactate bolus 200 ml. Urine output less than 30 ml/hr Check her fluid balance Check BP after 20 min Labetolol: Dosage: Start with 20 mg, 40 mg, 80 mg, and 80 mg until a maximum of 300 mg. Give bolus every 10 min until BP less than 160/110 mm. Hg Contra indications: Patients with asthma Patients with ischaemic heart disease If she is in a + fluid balance Low dose Dopamine infusion
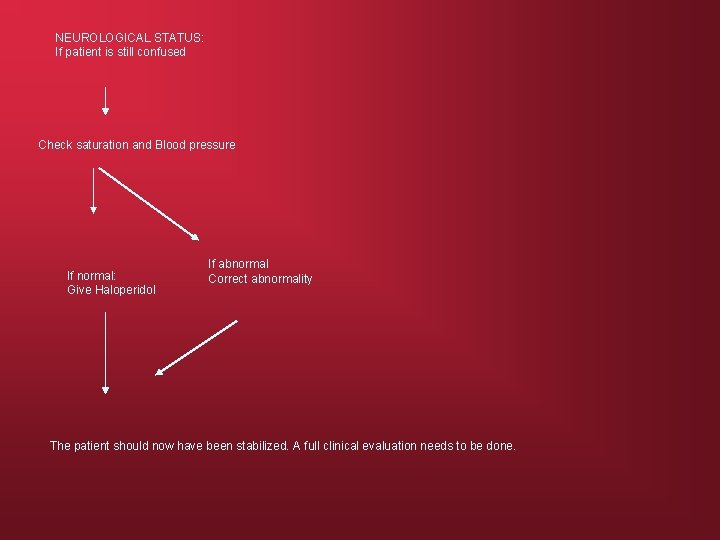
NEUROLOGICAL STATUS: If patient is still confused Check saturation and Blood pressure If normal: Give Haloperidol If abnormal Correct abnormality The patient should now have been stabilized. A full clinical evaluation needs to be done.

EVALUATION: Mother • • CNS Resp. System CVS Liver Renal Hematological Immune system Musculosceletal • Systemic clinical exam that include. – High care observations. – GCS, RR, BP, pulse, Sats, fluid balance chart. • Biochemical eval. – Hematocrit, platelets. – Creatinine, AST. – 24 hour protein clearance.

EVALUATION: Fetus • Sonar. – – – Estimated fetal weight. Structural abnormalities. Amniotic fluid index. Doppler umbilical art. Trans cerebellar diameter. Middle cerebral artery Doppler. – Ductus Venousus waveform. • CTG – If regarded as viable – 6 hourly

Once the mother is stable and the foetus is stable decide on further management. Better in Better out. Indications for delivery: Foetal distress Intra uterine death Expected weight more than 2 kg or sure gestation more than 34 weeks. Any signs of maternal organ invovement Platelets < 100 AST > 80 Creatinine > 100 Uncontrollable hypertension Eclampsia Proven lung maturity Foetal abnormality Expectant management: Only if mother and foetus stable and no indication for delivery: Keep in High care/High risk until hand over round. Transfer to Silver white firm 6 hourly CTG Daily full clinical evaluation Twice weekly biochemical and haematological evaluation. Place on Disprin half tablet daily Place on Calcium daily

Drugs: • Methyldopa – Depression – Liver function test abnormalities – Haemolytic anaemia • Calcium channel blockers – Headache – Facial flushing • Labetolol

Prophylaxis: • Low-dose aspirin: – Hypertension and renal disease – Hypertension and diabetes – Women at risk of PET – Women who had PET – Antiphospholipid syndrome • Calcium – If calcium depleted diet 2 gr/day

Prophylaxis: • Folic acid – 5 mg/day especially if hyperhomocysteinaemia

Conclusion: • PET is a dangerous disease and aggressive management is needed. • Patients should be in a high care firm for the expectant management.
- Slides: 38