Diabetes Health Needs Assessment Greg Fell Greg fellbradford

Diabetes Health Needs Assessment Greg Fell Greg. fell@bradford. nhs. uk

Structure and contents right click on the hyperlink 1. 2. 3. Risk Factors and prevalence Prevalence of diabetes Health outcomes associated with diabetes a) Emergency admissions – i. ii. b) 4. direct complicaitons and microvascular Emergency admissions – cardiovascular Mortality associated with diabetes Services available for treating diabetes a) b) c) d) e) 5. 6. Primary Care GPw. SI – Satellite Clinics Diabetic Retinopathy Screening Dietetics Secondary care – Outpatient Overview of Programme Budget. Key messages, recommendations and issues for service design a) b) c) d) e) Do we under implement lifestyle interventions and prevention. There is scope for system and scale development. Obesity as a future risk should not be ignored. Prevalence varies across the alliances. Diagnosed and actual Outcomes associated with diabetes are expressed principally as cardiovascular end points. It is possible to estimate the scale of the link. Primary Care services achieve improving outcomes, but there is variation across practices and alliances. Variations in exception reporting has been suggested as a quick win Primary care improvement – what are the options f) g) h) i) 7. The quality and reach of self care for diagnosed diabetic patients is untested in this HNA. GPSI satellite clinics – locations and capacity – correlations with % prevalence. Secondary Care services Data issues – what data do (and should) we record: socio-demographics and outcomes. Next steps

1) Risk Factor prevalence Obesity Back to top
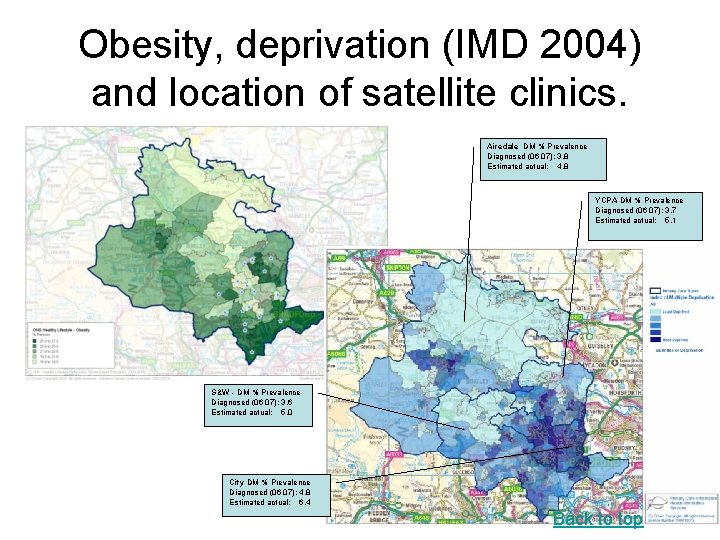
Obesity, deprivation (IMD 2004) and location of satellite clinics. Airedale DM % Prevalence Diagnosed (06 07): 3. 8 Estimated actual: 4. 8 YCPA DM % Prevalence Diagnosed (06 07): 3. 7 Estimated actual: 5. 1 S&W - DM % Prevalence Diagnosed (06 07): 3. 6 Estimated actual: 5. 0 City DM % Prevalence Diagnosed (06 07): 4. 8 Estimated actual: 6. 4 Back to top

2) Prevalence of diabetes Back to top
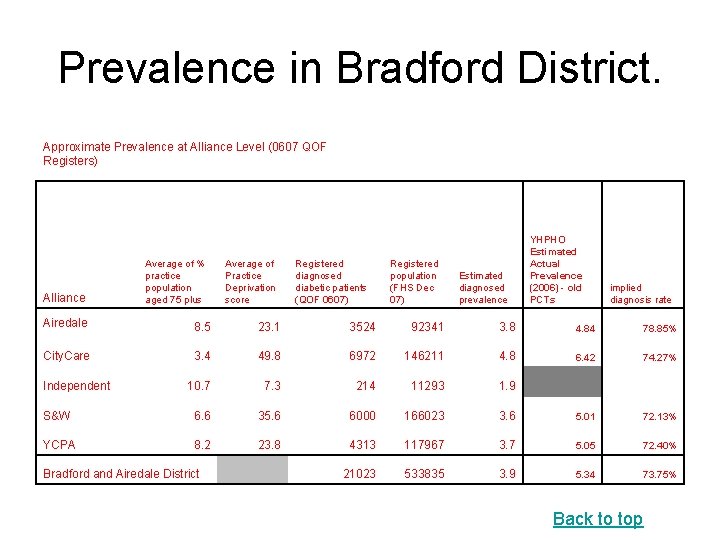
Prevalence in Bradford District. Approximate Prevalence at Alliance Level (0607 QOF Registers) Alliance Average of % practice population aged 75 plus Average of Practice Deprivation score Airedale 8. 5 23. 1 3524 92341 3. 8 4. 84 78. 85% City. Care 3. 4 49. 8 6972 146211 4. 8 6. 42 74. 27% 10. 7 7. 3 214 11293 1. 9 S&W 6. 6 35. 6 6000 166023 3. 6 5. 01 72. 13% YCPA 8. 2 23. 8 4313 117967 3. 7 5. 05 72. 40% 21023 533835 3. 9 5. 34 73. 75% Independent Bradford and Airedale District Registered diagnosed diabetic patients (QOF 0607) Registered population (FHS Dec 07) YHPHO Estimated Actual Prevalence (2006) - old PCTs Estimated diagnosed prevalence implied diagnosis rate Back to top
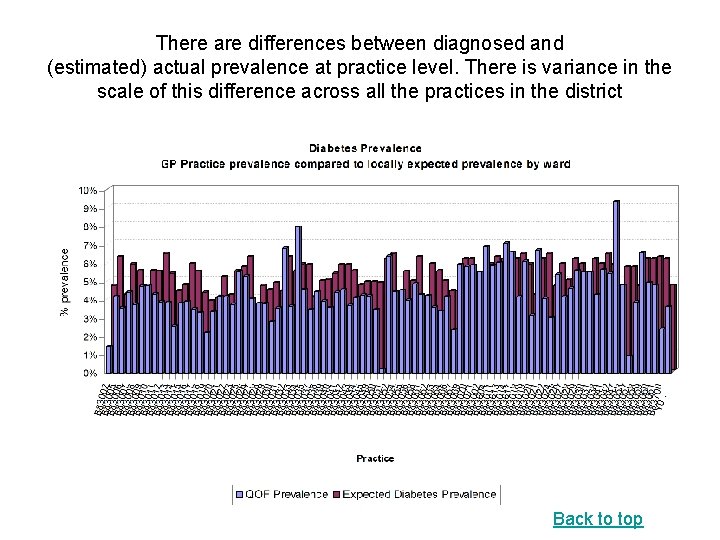
There are differences between diagnosed and (estimated) actual prevalence at practice level. There is variance in the scale of this difference across all the practices in the district Back to top

3) Health outcomes associated with diabetes a) Emergency Admission – i. ii. b) Direct complications and micro vascular, cardiovascular Mortality risk Back to top

i) Emergency Admissions – direct complications and microvascular. Back to top

Reason for admission. Direct complications and microvascular. Back to top

Ethnicity of patients admitted for direct complications and microvascular. Back to top

Age and sex profile of admitted patients – numbers (aggregate numbers over 7 yrs) Back to top
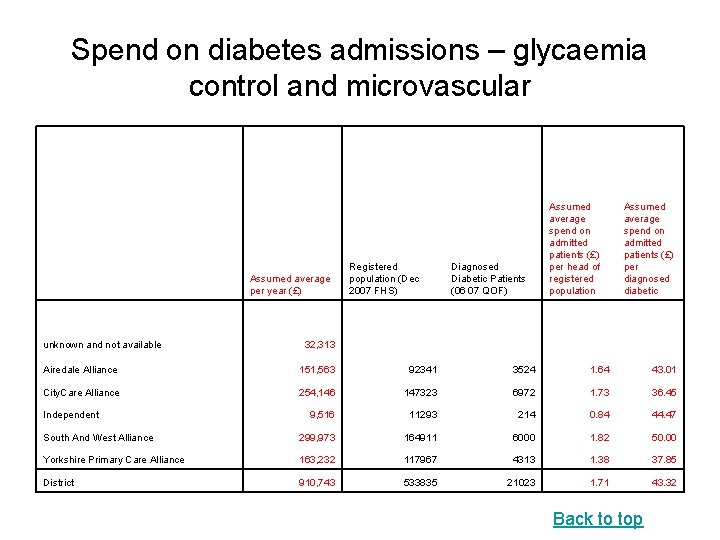
Spend on diabetes admissions – glycaemia control and microvascular Assumed average per year (£) unknown and not available 32, 313 Registered population (Dec 2007 FHS) Diagnosed Diabetic Patients (06 07 QOF) Assumed average spend on admitted patients (£) per head of registered population Assumed average spend on admitted patients (£) per diagnosed diabetic Airedale Alliance 151, 563 92341 3524 1. 64 43. 01 City. Care Alliance 254, 146 147323 6972 1. 73 36. 45 9, 516 11293 214 0. 84 44. 47 South And West Alliance 299, 973 164911 6000 1. 82 50. 00 Yorkshire Primary Care Alliance 163, 232 117967 4313 1. 38 37. 85 District 910, 743 533835 21023 1. 71 43. 32 Independent Back to top

ii) Emergency Admissions – cardiovascular (estimations based on population attributable risk) Back to top
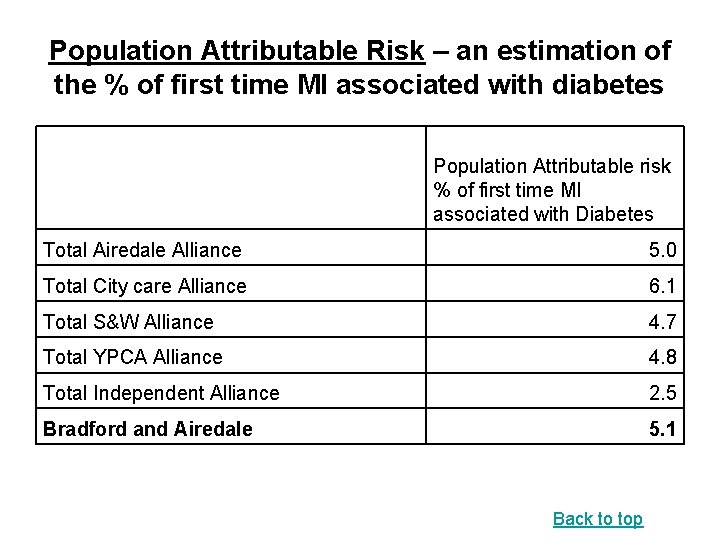
Population Attributable Risk – an estimation of the % of first time MI associated with diabetes Population Attributable risk % of first time MI associated with Diabetes Total Airedale Alliance 5. 0 Total City care Alliance 6. 1 Total S&W Alliance 4. 7 Total YPCA Alliance 4. 8 Total Independent Alliance 2. 5 Bradford and Airedale 5. 1 Back to top
Micro and Macro Vascular risks compared High outcome Low outcome Back to top

b) Mortality associated with diabetes Back to top
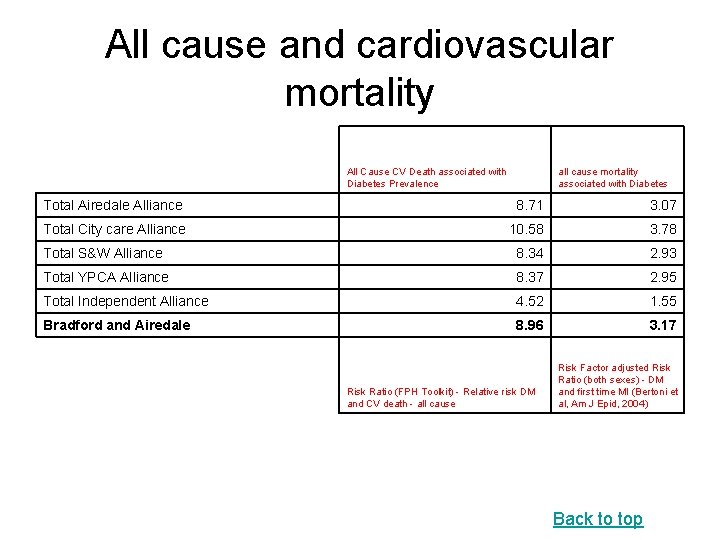
All cause and cardiovascular mortality All Cause CV Death associated with Diabetes Prevalence all cause mortality associated with Diabetes Total Airedale Alliance 8. 71 3. 07 Total City care Alliance 10. 58 3. 78 Total S&W Alliance 8. 34 2. 93 Total YPCA Alliance 8. 37 2. 95 Total Independent Alliance 4. 52 1. 55 Bradford and Airedale 8. 96 3. 17 Risk Ratio (FPH Toolkit) - Relative risk DM and CV death - all cause Risk Factor adjusted Risk Ratio (both sexes) - DM and first time MI (Bertoni et al, Am J Epid, 2004) Back to top
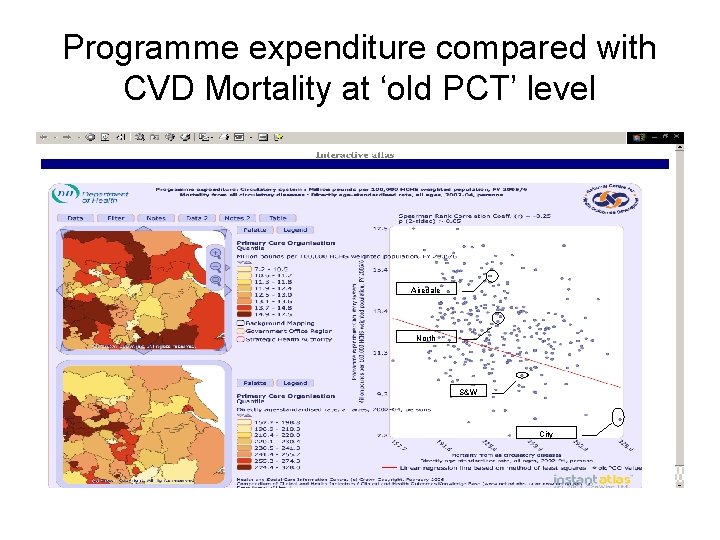
Programme expenditure compared with CVD Mortality at ‘old PCT’ level Airedale North S&W City

4) Services available for treating diabetes a) b) c) d) e) Primary Care Dietetics Diabetic Retinopathy Screening GPw. SI – Satellite Clinics Secondary care – Outpatient Back to top

a) Primary Care Data from QOF, Px Back to top

DM 12 at practice level, with exception reporting. Back to top

DM 12 – range of BP Control achieved across all practices Back to top

DM 17 – Cholesterol control with exception coding Back to top

Range of % of diabetic patients with controlled cholesterol at practice level. Back to top

There is a relationship between % of DM patients achieving cholesterol control and deprivation Back to top

Range of % of diabetic patients with controlled HBA 1 C at practice level. Back to top

DM 20. With Exception Codes. There is a high proportion of exceptions and approx 50% of patients (taking into account exceptions) are not achieving glycaemic control. Back to top

b) Dietetics
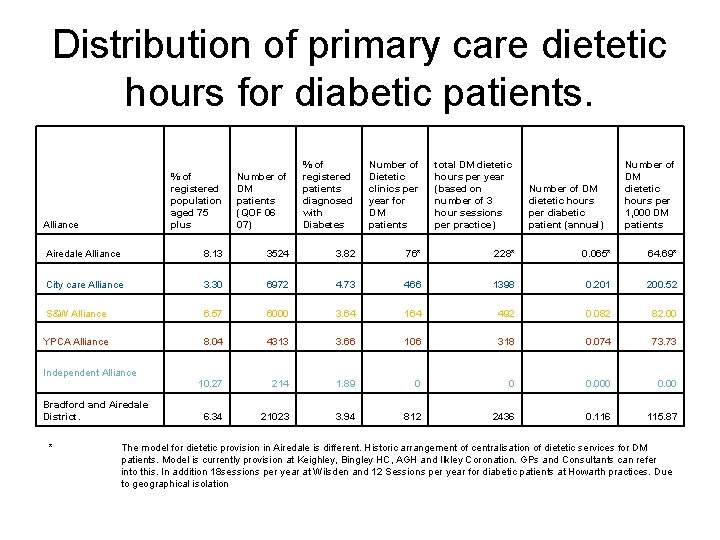
Distribution of primary care dietetic hours for diabetic patients. % of registered population aged 75 plus Number of DM patients (QOF 06 07) % of registered patients diagnosed with Diabetes Number of Dietetic clinics per year for DM patients total DM dietetic hours per year (based on number of 3 hour sessions per practice) Airedale Alliance 8. 13 3524 3. 82 76* 228* 0. 065* 64. 69* City care Alliance 3. 30 6972 4. 73 466 1398 0. 201 200. 52 S&W Alliance 6. 57 6000 3. 64 164 492 0. 082 82. 00 YPCA Alliance 8. 04 4313 3. 66 106 318 0. 074 73. 73 10. 27 214 1. 89 0 0 0. 00 6. 34 21023 3. 94 812 2436 0. 116 115. 87 Alliance Number of DM dietetic hours per diabetic patient (annual) Number of DM dietetic hours per 1, 000 DM patients Independent Alliance Bradford and Airedale District. * The model for dietetic provision in Airedale is different. Historic arrangement of centralisation of dietetic services for DM patients. Model is currently provision at Keighley, Bingley HC, AGH and Ilkley Coronation. GPs and Consultants can refer into this. In addition 18 sessions per year at Wilsden and 12 Sessions per year for diabetic patients at Howarth practices. Due to geographical isolation
c) Diabetic Retinopathy Screening

DR Screening

c) GPw. SI Satellite clinics Back to top
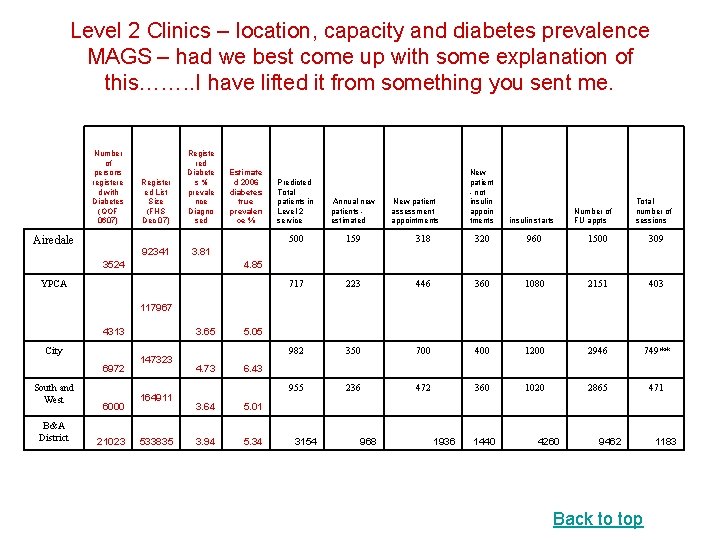
Level 2 Clinics – location, capacity and diabetes prevalence MAGS – had we best come up with some explanation of this……. . I have lifted it from something you sent me. Number of persons registere d with Diabetes (QOF 0607) Airedale Register ed List Size (FHS Dec 07) Registe red Diabete s % prevale nce Diagno sed 92341 3. 81 3524 Estimate d 2006 diabetes true prevalen ce % New patient - not insulin appoin tments Predicted Total patients in Level 2 service Annual new patients - estimated 500 159 318 320 960 1500 309 717 223 446 360 1080 2151 403 982 350 700 400 1200 2946 749** 955 236 472 360 1020 2865 471 New patient assessment appointments insulin starts Number of FU appts Total number of sessions 4. 85 YPCA 117967 4313 City 6972 South and West B&A District 6000 21023 3. 65 147323 164911 533835 4. 73 5. 05 6. 43 3. 64 5. 01 3. 94 5. 34 3154 968 1936 1440 4260 9462 Back to top 1183

d) OPD utilisation ? ? ? Treat with suspicion DM Nurse OPD appointments are under what they should be ? ? ? where is the medic appts? ? Back to top

Opth and Chiropady are the areas mostly involved in DM care Back to top

Utilisation by speciality and age Back to top

5) Overview of Programme Budget. Back to top

There is an approximate 7 fold difference in diabetic medication spend per patient at HBA 1 C target Back to top
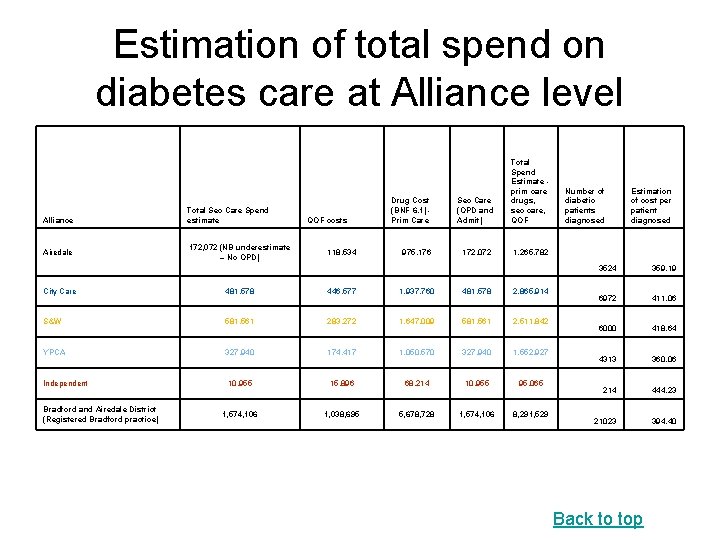
Estimation of total spend on diabetes care at Alliance level Alliance Airedale Total Sec Care Spend estimate 172, 072 (NB underestimate – No OPD) QOF costs 118, 534 Drug Cost (BNF 6. 1) - Prim Care 975, 176 Sec Care (OPD and Admit) Total Spend Estimate - prim care drugs, sec care, QOF 172, 072 1, 265, 782 City Care 481, 578 446, 577 1, 937, 760 481, 578 2, 865, 914 S&W 581, 561 283, 272 1, 647, 009 581, 561 2, 511, 842 YPCA 327, 940 174, 417 1, 050, 570 327, 940 1, 552, 927 Independent 10, 955 15, 896 68, 214 10, 955 95, 065 1, 574, 106 1, 038, 695 5, 678, 728 1, 574, 106 8, 291, 529 Bradford and Airedale District (Registered Bradford practice) Number of diabetic patients diagnosed Estimation of cost per patient diagnosed 3524 359. 19 6972 411. 06 6000 418. 64 4313 360. 06 214 444. 23 21023 394. 40 Back to top

Micro vascular outcomes and total estimated spend on DM care at practice level Blue line is mean for district. Back to top

6) Key messages, recommendations and issues for service design a) b) c) d) e) f) g) h) i) Do we under implement lifestyle interventions and prevention. There is scope for system and scale development. Obesity as a future risk should not be ignored. Prevalence varies across the alliances. Diagnosed and actual Outcomes associated with diabetes are expressed principally as cardiovascular end points. It is possible to estimate the scale of the link. Primary Care services achieve improving outcomes, but there is variation across practices and alliances. Variations in exception reporting has been suggested as a quick win The quality and reach of self care for diagnosed diabetic patients is untested and un-researched in this HNA. GPSI satellite clinics – locations and capacity – correlations with % prevalence. Secondary Care services Data issues – what data do (and should) we record: sociodemographics and outcomes. Back to top

a) • • Do we under implement lifestyle interventions and prevention. There is scope for system and scale development. Lifestyle interventions. American and Finnish studies have reported excellent results. – 58% preventable / Significant delay in onset / Delay in development of complications. Do we under implement these interventions? What is the role we need to develop for a range of support services What of ‘industrialisation’? Systematise and scale. Equality component to this! Development of Cardiovascular Risk Screening, as per recent DH announcement will assist greatly with this process – especially system and scale. – Issues re equality and the capacity in services to ‘treat’ those identified as high risk remain unresolved issues. The notion of a ‘health gain schedule’, as part of a contract with all providers. Setting out a minimum suite of lifestyle interventions to be systematically applied. Careful commissioning needed. This crosses over into many other disease areas. Some considerations: – Appropriate, intense and repeated social marketing. Continually reinforce healthy living messages – appropriate to a range of target audiences – Weight management, smoking cessation, Exercise, Health trainers – Community development – in some parts of the district……. use the expertise, on the ground knowledge and contacts to access groups that might not otherwise come to health care services. – Smoking cessation – macro vascular risk - how much / how intense efforts to goes in to help diabetic smokers to stop Back to top

b) Obesity as a future risk should not be ignored. • Under-ascertainment of obesity in primary care. – Understandable given the weight given in QOf? – If not picked up, possibly not well managed. – Even minor weight loss can confer significant health benefits. – Capacity in weight management pathway. Pharmacological and non pharmacological interventions – particularly the latter. Back to top

c) Prevalence varies across the alliances. Diagnosed and actual • • Incidence – certain population groups more likely to develop diabetes. – Ethnicity risk, over an above deprivation. – People living in socio economically deprived areas (most likely lifestyle risk). – Older people. 21, 000 diagnosed diabetics, 3. 9% (3. 7 – 4. 8%) True population prevalence is greater – estimated in 2006 to be 5. 4% – Bradford estimates commonly seen as significantly under estimates – ethnicity as a genetic risk / ethnic profile of the district is not the same as England – Strong correlation with deprivation – 60% female, 40% male (approaching 50: 50 in city) – Much higher prevalence as age increases Some evidence that some pop groups less likely to access services once diagnosed – or poorer control if they do access. – Not all about deprivation – some practices in the most deprived areas achieve highly. Back to top

d) Outcomes associated with diabetes are expressed principally as cardiovascular end points. It is possible to estimate the scale of the link. • Relatively few deaths directly attributable to diabetes. • Approx 9% of CV deaths, 3% all cause mortality and 5% of first time MI admits attributable to diabetes. Back to top

e) Primary Care services achieve improving outcomes, but there is variation across practices and alliances. Variations in exception reporting has been suggested as a quick win Macro vascular • BP recording good and improving – 22% of non exempted DM patients do not meet BP control target. 60% in the worst performing practice, 5% in the best. • Chol recording good and improving. – 20% of non exempted DM patients do not meet Chol targets. 45% in worst, 3% in best. – For chol – deprivation profile of registered patients is a significant factor, as is age profile. (Less of an issue for BP control. ) Microvascular • 35% of non exempted patients don’t meet HBA 1 C targets. 70% in worst performing practice, 3% in best. • • EXPLORING DIFFERENCES IN EXCEPTION REPORTING is a key area for consideration. The figures above don’t take into account the variability in exemptions. The QOF data gives suggestions as to which practices to target service improvement and support activities Back to top

Primary Care Improvement – what are the options Some options: • The QOF data suggest where improvements are needed. • Not all about deprivation – some practices in deprived areas achieve. • ‘buddying’ and partnering – high and low performing practices. Clinical and organisational. • Robust performance management, and use of powers in contract to introduce competition where appropriate to do so. • Role of GPSI in supporting clinical and organisational aspects of care • Role of CD workers – explore fully. In the broader context of CVD • GPSI buddying supporting poorly performing practices • Access strategies / user interface – informed by social marketing and strong community development – getting a REAL understanding of the target market and preferred communication styles. Back to top

f) The quality and reach of self care for diagnosed diabetic patients is untested in this HNA. • No data here on self care. • Most people see their Dr only 1 or 2 per year – thus for 363 days, self care • NICE (and NSF) – recommend structured group education – provided locally – HCC review DM services nationally (2006) – 11% of DM patients had received self care support / advice of any type (regardless of whether meets NICE standard)……socio economic / ethnic divide presumably sharp……. (though not tested) – Funding for self care made available from DH – but in the baseline – thus local prioritisation • How good are our self care programmes? – Under implemented (esp in areas / pop with most need? ) – Culturally and ethnically sensitive – Language / reading age / AV material etc……. . health trainers etc…. Back to top

g) GPSI satellite clinics – locations and capacity – correlations with % prevalence. • Prevalence should tell us something about location. • Capacity in City. Care equals need, especially given the complexity of the population. • Equality across the whole district, and geographic accessibility to pockets of high prevalence outside City. Care needs to be tested and assessed. • Language support may need to be addressed, written and translation Back to top

h) Secondary Care services Admits • 2400 over a 7 year period – admits directly related to DM and micro vascular complications. • Length of stay is shortening over time. • Men seem more likely to be admitted (despite lower prevalence) • Static trend in admissions • Average spend on admitted patients per diagnosed diabetic patient varies from £ 36 (Citycare) to £ 50 (S&W). OPD • 30, 000 OPD appointments over 4 year. • Bradford FT ONLY. No Airedale OPD data • Chiefly chiropody (67%), opth (19%), dietician (7%). • First Attendance to Follow up – 1: 10, relatively static. – S&W, YCPA higher rate than City Care Back to top

i) Data issues – what data do (and should) we record: socio-demographics and outcomes. • This review considered routinely available data. • Is there a need for more detailed review, plus addition of additional audits of specific areas of care? This might include: – Within primary care, satellite clinics, secondary care……. • Agree a clear and common set of clinical quality, organisational performance and public health data for ongoing analysis. A core data set. • Analyst capacity within Performance and Information Directorate to undertake needs consideration if this is taken forward. Back to top

7) Next Steps

Next Steps • This Health Needs Assessment might inform development of future services • It is only one of the considerations • Patient experience, user involvement not sought during this HNA. It should be. • Some options for change already on the table. – Prioritisation of these and other developments – A range of perspectives to be considered in this (clinical, patient, corporate). And a mechanism for doing so. PBMA approach is recommended. Back to top
- Slides: 54