Diabetes Caring for residents with diabetes Katharine Ramage

Diabetes Caring for residents with diabetes Katharine Ramage DSN/Professional Education Lead Diabetes MCN

Learning Outcomes � Develop an awareness of the different types of diabetes � Understand why it is important to manage diabetes � Demonstrate knowledge of what must be considered when caring for individuals with diabetes � Recognise signs, symptoms and risk factors for hypo and hyperglycaemia � Develop an understanding of when action is required and what to do

What is Diabetes? � Diabetes is a common condition that can affect both adults and children � Diabetes is diagnosed by measuring the amount of glucose (sugar) in the blood � The pancreas does not produce enough insulin or the body does not respond how it should to the insulin it produces

Type 1 Diabetes � Autoimmune � Can cause – Insulin deficiency develop at any age � Lifelong � Insulin condition should NEVER be withheld in a person with Type 1 diabetes � High risk of ketones/DKA � Ketones illness should be checked when BG high/in

Type 2 Diabetes � Most common form – up to 90% � High glucose levels caused by insulin resistance/relative insulin deficiency � Usually develops in older adults, but increasingly seen in younger people – particularly if overweight or obese � Can be treated by diet, oral medications, injectable medication, including insulin – or a combination

Why is it important to manage well? � People with diabetes have: - Increased rates of hospital admission - High levels of physical and cognitive disability - Increased risk of pressure sore development - High rates of complications - Increased susceptibility to infection

What to consider? � Type of Diabetes � Treatment � Dietary and it’s aims and lifestyle factors � Blood glucose and ketone monitoring requirements � Target blood glucose levels � Foot care � Hypoglycaemia management � Hyperglycaemia management � Complications � Review/screening � Specialist � End referral of life care � Individual care plan

Individual Care Plan � Should include: - Type of diabetes - Treatment - Dietary requirements - Target blood glucose levels - Requirement for monitoring - Foot care - Role of care staff in managing or supporting self care

Self-care � Many people with diabetes will be capable of self -managing independently, or with assistance � Important to provide appropriate support � Recognise any difficulties or factors that may interfere with self-care � Be aware that poor mental health can affect management of diabetes – consider changes in normal mental health ie: mood, appearance, anxiety

Medical Review - Routine � Appointments to screen for complications at least annually if able to attend � Eye screening � Blood samples, including Hb. A 1 c � Urine samples � Weight � BP � Foot screening – feet should be checked on a regular basis � If unable to attend, review should be carried out by GP in the home
Possible Complications � Heart disease � Stroke � Nerve � Eye damage (neuropathy) disease (retinopathy) � Kidney � High disease (nephropathy) blood pressure � Problems � High with circulation cholesterol � Erectile dysfunction

Recognising Hypoglycaemia � Low blood glucose (below 4 mmol/L) � The most common side effect of insulin and certain oral medications for diabetes � Must be excluded in a person with diabetes who becomes acutely unwell, drowsy, unconscious, unable to cooperate, aggressive

Risk Factors � Increasing � No age or inadequate blood glucose monitoring � Cognitive impairment/dementia � Reduced carbohydrate intake for any reason � Previous severe hypoglycaemia � Impaired � Weight awareness loss

Possible causes � Missed � Less or delayed meals carbohydrate than normal � Incorrect or inappropriate insulin or oral medication doses � Failure to monitor blood glucose adequately � Vomiting
Signs and symptoms Trembling/ shaking Drowsiness Confusion Dizziness Sweating Poor coordination Aggressive behaviour Irritability Poor communication Loss of consciousness

How do you treat a Hypo?

Treatment � Once hypoglycaemia is identified, the treatment should be given without delay � Quick-acting carbohydrate required to return the glucose level to normal ie: glucose tablets, glucose drink, jelly babies � Follow up with more complex carbohydrate snack ie: toast, small sandwich, biscuits - or next meal if due

What next? Consider the cause of the hypo - Can this be avoided in future? Is a medical review required? Is a review of medication required? Does the individual care plan require an update?

Hyperglycaemia � Excess glucose in the blood (over 12 mmol/L) - If persistent can cause unpleasant symptoms and long-term consequences � Many possible causes � Possible life-threatening complications: - Diabetic Ketoacidosis (DKA) - Hyperosmolar Hyperglycaemic State (HHS)

Possible causes � Illness (eg: infection) � Dietary factors – Sugary drinks, extra snacking, large amount of carbohydrate � Stress � Insufficient � Certain treatment medications (eg: steroids) � Injection � Problems site issues with insulin (eg: inappropriate storage)

Signs and symptoms � Thirst, dry mouth � Tiredness � Blurred vision � Increased urine output - Consider hyperglycaemia in residents with urinary incontinence - Increased risk of UTI � Poorly healing wounds

Hyperglycaemia in Care Homes � Target blood glucose for elderly people usually higher – around 6 -12 mmol/L, but will be specific to the individual � Higher target to reduce risk of Hypoglycaemia � Important to avoid prolonged high blood glucose levels due to the risk of HHS and DKA � High blood glucose causes unpleasant symptoms and should not be ignored

What next? Consider the cause of high blood glucose - Can this be avoided in future? Is a medical review required? Is a review of medication required? Does the individual care plan require an update?

Not to be ignored � If the patient is unwell and you are concerned, seek medical advice - Inability to swallow/not able to keep fluids down - Vomiting - Persistent Diarrhoea - Persistently high glucose - Underlying infection

Further learning to assist with caring for residents with diabetes � Blood glucose monitoring -competencies, training for carers/HCSWs � Dietary factors -Diabetes Specialist Dietitian � Foot care -Diabetes Specialist Podiatrist -CPR for Diabetic Feet e-learning, FRAME modules for foot screening

Who to refer to � Residents own GP - Medical review, intercurrent illness � District Nurse – Support with Blood glucose monitoring, insulin administration � Community Diabetes Specialist Nurse – advice regarding diabetes medication, diabetes management � Podiatrist – concerns about feet
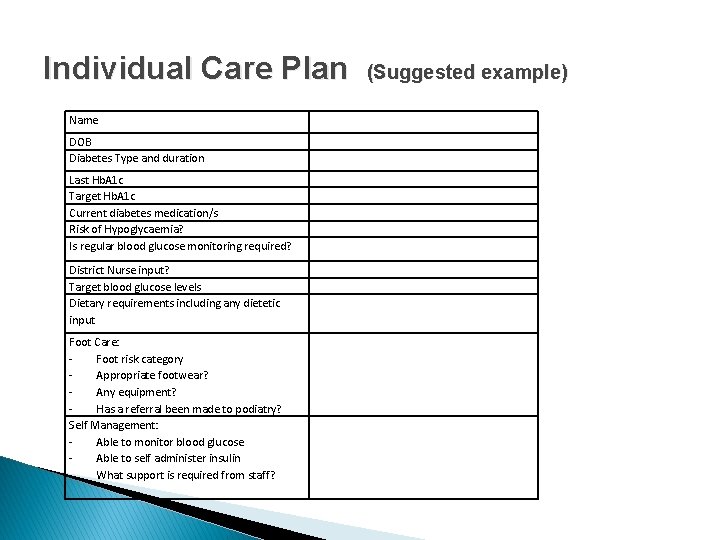
Individual Care Plan Name DOB Diabetes Type and duration Last Hb. A 1 c Target Hb. A 1 c Current diabetes medication/s Risk of Hypoglycaemia? Is regular blood glucose monitoring required? District Nurse input? Target blood glucose levels Dietary requirements including any dietetic input Foot Care: Foot risk category Appropriate footwear? Any equipment? Has a referral been made to podiatry? Self Management: Able to monitor blood glucose Able to self administer insulin What support is required from staff? (Suggested example)
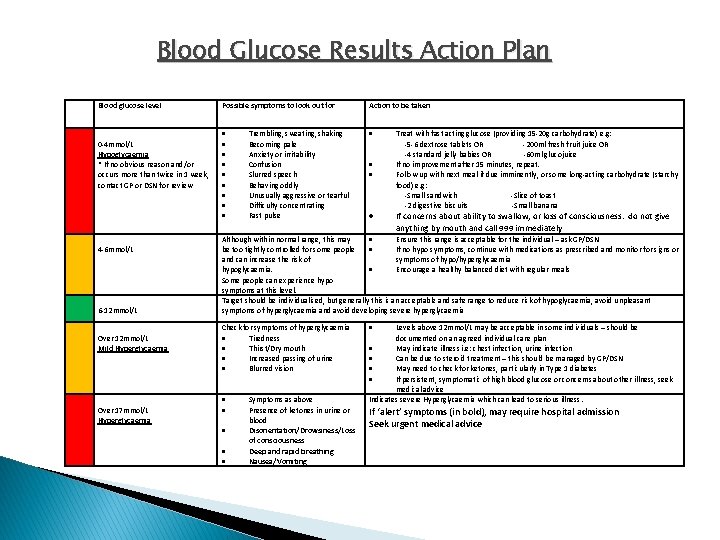
Blood Glucose Results Action Plan Blood glucose level 0 -4 mmol/L Hypoglycaemia * If no obvious reason and/or occurs more than twice in 1 week, contact GP or DSN for review 4 -6 mmol/L 6 -12 mmol/L Over 12 mmol/L Mild Hyperglycaemia Over 17 mmol/L Hyperglycaemia Possible symptoms to look out for Action to be taken Trembling, sweating, shaking Becoming pale Anxiety or irritability Confusion Slurred speech Behaving oddly Unusually aggressive or tearful Difficulty concentrating Fast pulse Treat with fast acting glucose (providing 15 -20 g carbohydrate) e. g: -5 -6 dextrose tablets OR -200 ml fresh fruit juice OR -4 standard jelly babies OR -60 ml glucojuice If no improvement after 15 minutes, repeat. Follow up with next meal if due imminently, or some long-acting carbohydrate (starchy food) e. g: -Small sandwich -Slice of toast -2 digestive biscuits -Small banana If concerns about ability to swallow, or loss of consciousness: do not give anything by mouth and call 999 immediately Although within normal range, this may Ensure this range is acceptable for the individual – ask GP/DSN be too tightly controlled for some people If no hypo symptoms, continue with medications as prescribed and monitor for signs or and can increase the risk of symptoms of hypo/hyperglycaemia hypoglycaemia. Encourage a healthy balanced diet with regular meals Some people can experience hypo symptoms at this level. Target should be individualised, but generally this is an acceptable and safe range to reduce risk of hypoglycaemia, avoid unpleasant symptoms of hyperglycaemia and avoid developing severe hyperglycaemia Check for symptoms of hyperglycaemia Tiredness Thirst/Dry mouth Increased passing of urine Blurred vision Symptoms as above Presence of ketones in urine or blood Disorientation/Drowsiness/Loss of consciousness Deep and rapid breathing Nausea/Vomiting Levels above 12 mmol/L may be acceptable in some individuals – should be documented on an agreed individual care plan May indicate illness i. e: chest infection, urine infection Can be due to steroid treatment – this should be managed by GP/DSN May need to check for ketones, particularly in Type 1 diabetes If persistent, symptomatic of high blood glucose or concerns about other illness, seek medical advice Indicates severe Hyperglycaemia which can lead to serious illness. If ‘alert’ symptoms (in bold), may require hospital admission Seek urgent medical advice

Contacts Katharine Ramage – Diabetes MCN Professional Education Lead/DSN Katharine. ramage@nhslothian. scot. nhs. uk Edinburgh Community Diabetes Specialist Nurses: communitydiabetesteam@nhslothian. scot. nhs. uk West Lothian Community Diabetes Specialist Nurses: 01506 522238 Royal Infirmary DSNs: 0131 242 1471 Western General DSNs: 0131 537 1746
- Slides: 29