DIABETES AND HEART FAILURE POPPY BROOKS LEAD ACP

DIABETES AND HEART FAILURE POPPY BROOKS: LEAD ACP CARDIAC SUPPORT , COMMITTEE MEMBER BRITISH SOCIETY FOR HEART FAILURE NURSE FORUM

Understanding what heart failure is and the different types of heart failure. Learning objectives To consider how the mechanisms of both conditions are related. Prescribing considerations in the diabetic patient with heart failure.

WHAT IS HEART FAILURE? HTTPS: //WWW. YOUTUBE. COM/WATCH? V=M 4 AC 0 -X 4 ZWQ

Heart failure is a complex clinical syndrome of symptoms and signs that suggest the efficiency of the heart as a pump is impaired. It is caused by structural or functional abnormalities of the heart. Around 920, 000 people in the UK today have been diagnosed with heart failure. Both the incidence and prevalence of heart failure increase steeply with age, and the average at diagnosis is 77. Improvements in care have increased survival for people with ischaemic heart disease, and treatments for heart failure have become more effective. But the overall prevalence of heart failure is rising because of population ageing and increasing rates of obesity. NICE 2018 Definition of heart failure

New York Heart Association Classification

TYPES OF HEART FAILURE v Heart failure secondary to reduced ejection fraction HFr. EF v Heart failure with mid range ejection fraction HFmr. EF v Heart failure with preserved ejection fraction HFp. EF
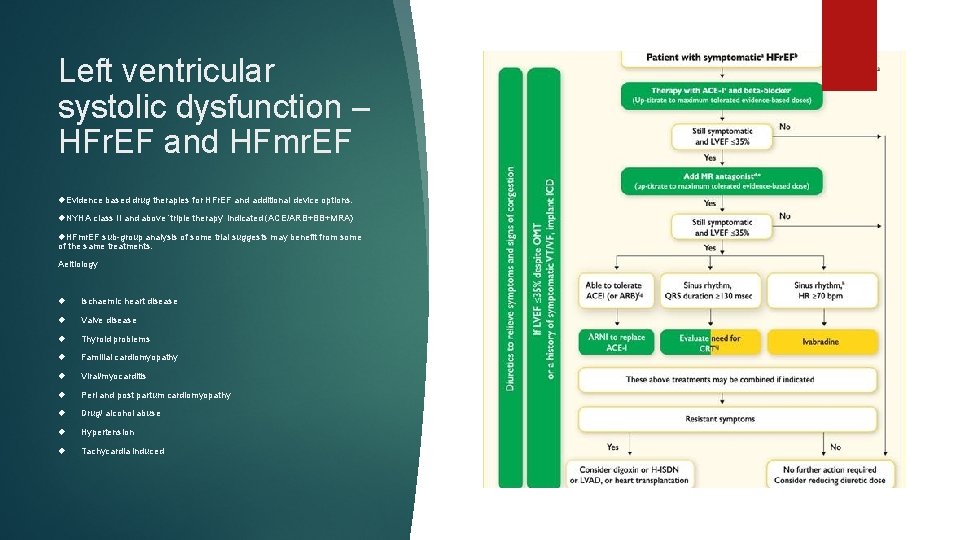
Left ventricular systolic dysfunction – HFr. EF and HFmr. EF Evidence based drug therapies for HFr. EF and additional device options. NYHA class II and above ‘triple therapy’ indicated (ACE/ARB+BB+MRA) HFmr. EF sub-group analysis of some trial suggests may benefit from some of the same treatments. Aeitiology Ischaemic heart disease Valve disease Thyroid problems Familial cardiomyopathy Viral/myocarditis Peri and post partum cardiomyopathy Drug/ alcohol abuse Hypertension Tachycardia induced

HFp. EF Same signs and symptoms but a different underlying issue. Instead of the heart not squeezing the blood out effectively it is not filling properly in the first place. Treatment includes managing comorbidities well and offloading congestion. Despite many trials there are sadly no proven disease modifying therapies. Accounts for at least 50% of heart failure admissions. Community HF team not currently commissioned to see this group of patients.


Heart failure and diabetes Diabetes in an independent risk factor for both types of heart failure. Both type 1 and type 2 diabetes increase risk of heart failure. Similar risk factor profile for type II diabetes and acquired heart disease. Advanced age, duration of the disease, insulin use, presence of ischaemic heart disease and elevated creatinine are all risk factors for heart failure in diabetic patients.

Risk of early mortality and cardiovascular disease in type 1 diabetes: a comparison with type 2 diabetes, a nationwide study You-Bin Lee, Kyungdo Han, Bongsung Kim, Seung-Eun Lee, Ji Eun Jun, Jiyeon Ahn, Gyuri Kim, Sang-Man Jin & Jae Hyeon Kim Cardiovascular Diabetology volume 18, Article number: 157 (2019) https: //cardiab. biomedcentral. com/articles/10. 1186/s 12933 -019 -0953 -7#citeas

Mechanisms of cardiac dysfunction in diabetes Atherosclerotic disease. The switch of glucose to fatty acid oxidation has a negative effect on cardiac contractility and function. Impaired microvascular endothelial function. Increased myocardial fibrosis. Activation of the renin angiotensin aldosterone system (RAAS). Alterations in myofibrillar regulatory contractile proteins. Reduced myocardial energy reserves. Oxidative stress. Inflammation.

What if my diabetic patient has heart failure symptoms but no diagnosis? Advise urgent GP appointment Should have NTpro. BNP blood test #onesimplebloodtest NTpro. BNP levels < 400 pg/m. L heart failure is unlikely NTpro. BNP levels 400 -2000 pg/m. L- referral for open access echocardiography within 6 weeks If NTpro. BNP levels >2000 referral for urgent Cardiologist/ Heart Failure ACP appointment within 2 weeks. Will have echocardiogram at appointment. ECG and Cx. R (if no recent available)will also usually be done

Prescribing in heart failure with diabetes

Prescribing considerations for the heart failure specialist Diuretics can exacerbate diabetes – latent diabetes may become overt and insulin doses may need to increase. Whilst non selective beta blockers may have an effect of glycaemic control, the products licensed in heart failure are in the more selective group (bisoprolol, carvedilol and nebivolol). ACE Inhibitors and angiotensin receptor blockers have mortality benefits for patients with HFr. EF in patients regardless of diabetic status. Mineralocorticoid receptor antagonists (MRAs) reduce proteinuria in diabetic nephropathy and also have mortality benefits in HFr. EF. May have some use also in some phenotypes of HFp. EF.

Sacubitril Valsartan (Entresto) Angiotensin receptor neprilysin inhibitor (ARNI) Significant mortality reduction in HFr. EF – PARADIGM trial (2014) Risk of fatal angioedema if co-administered with ACE- Inhibitor Specialist initiation only Concomitant use with aliskeren containing products (amlodipine, tekturna) in diabetic or renally impaired patients is contrainidicated Reduces the incidence of insulin initiation in T 2 DM patients with HFr. EF There may be patients suitable who are no longer under our care and could be referred back to us.

Prescribing considerations for diabetic specialist Insulin therapy can exacerbate fluid retention. Many oral glucose lowering agents are associated with a risk of heart failure hospitalisation. Glucose-lowering agents may favour the development of heart failure through several pathophysiological mechanisms related to the increased insulin levels, water retention and low glucose availability for the heart and muscles. Rosiglitazone- withdrawn due to cardiovascular complications. ‘U shaped curve’ of glycaemic control and outcomes in heart failure – ‘sweet spot’ (Hb. A 1 c 7. 1– 7. 8 %) suggested by several trials

Oral glucose lowering agents and heart failure

DAPA-HF 2019

DAPA-HF Results § “Among patients with heart failure and a reduced ejection fraction, the risk of worsening heart failure or death from cardiovascular causes was lower among those who received dapagliflozin than among those who received placebo, regardless of the presence or absence of diabetes. ”

DAPA-HF next steps NICE tag expected in June for use in LVSD If HF team are to prescribe will need to be written into treatment guidelines Cross collaboration between our services to safely manage these patients? Patients in the trial had a LVEF of <40% A cut off of 30 ml/min was used for those with renal impairment A good number of trial participants patients were on ‘triple therapy’ for heart failure already

SGLTT-2 and HF

SGLT-2 and HF EMPA-HEART showed reverse cardiac remodelling on MRI in T 2 DM patients treated with empagiflozin DEFINE-HF improvement in QOL scoring for dapagiflozin treated patients with LVSD EMPERIAL-REDUCED/PRESERVED did not meet primary endpoints of improved 6 min walk tests for patients treated with Empagiflozin Ongoing trials to establish class effect and whethere is benefit in HFp. EF Also trials investigating potential renal benefits of SGLT-2 inhibitors

Renal impairment Common in both heart failure and diabetes Renal implications of medications used for both diseases Hypovolaemia risk Benefits of HF treatments often outweigh risks of renal effects 2019 Consensus guidance published by Renal Association and British Society for Heart Failure

In Conclusion We are still only learning about the complex relationship between heart failure and diabetes. I as a heart failure nurse definitely need to learn more about diabetes and think about whether my patients could have undiagnosed diabetes. Diabetic patients are at very high risk of developing heart failure. The treatments of either condition can affect the stability of the other. Collaboration between our two services is key to providing safe and effective care to this group of patients.
- Slides: 25