Diabetes and Coronary Artery Disease By Jean Molinary

Diabetes and Coronary Artery Disease By Jean Molinary, DO

Screening for Diabetes in Adults • ADA: Risk based, or starting at the age of 45, then every 3 years if normal
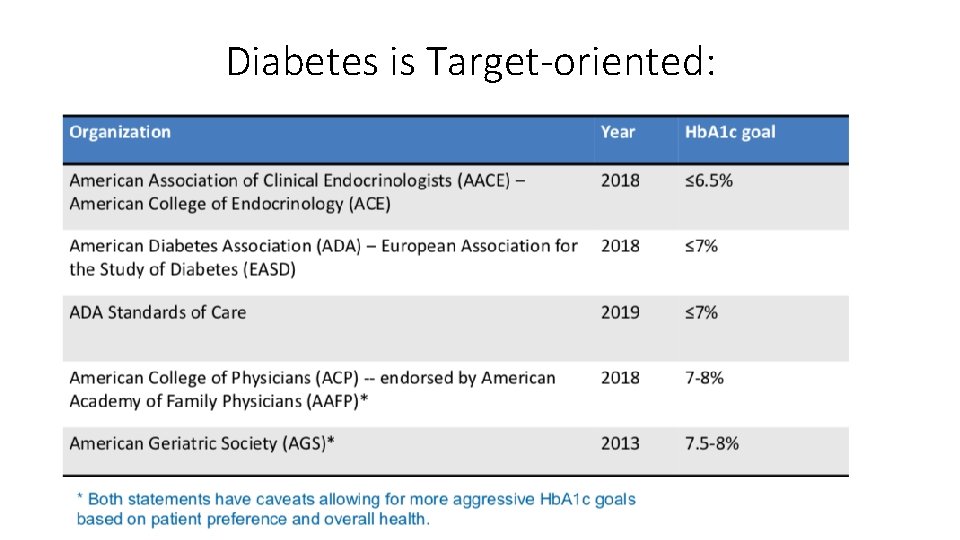

Diabetes is Target-oriented:
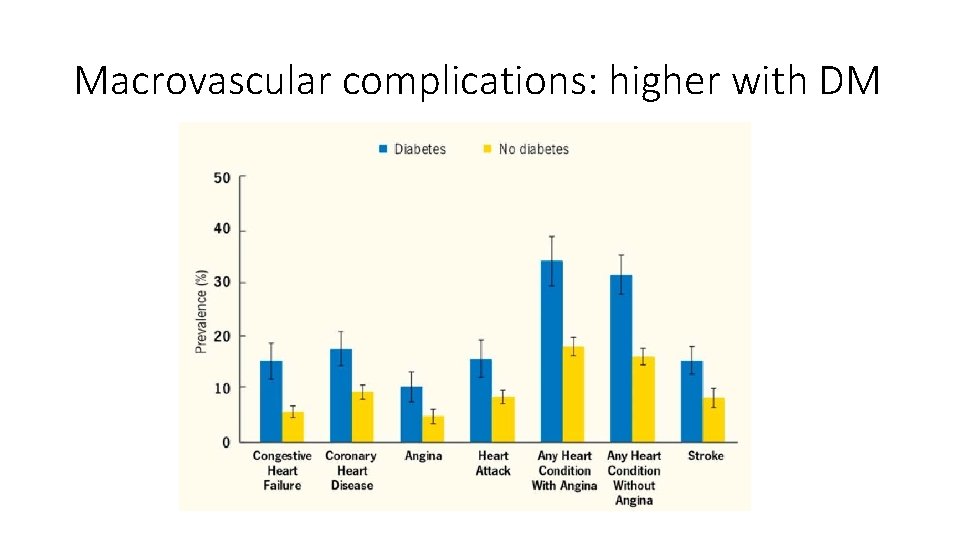
Macrovascular complications: higher with DM
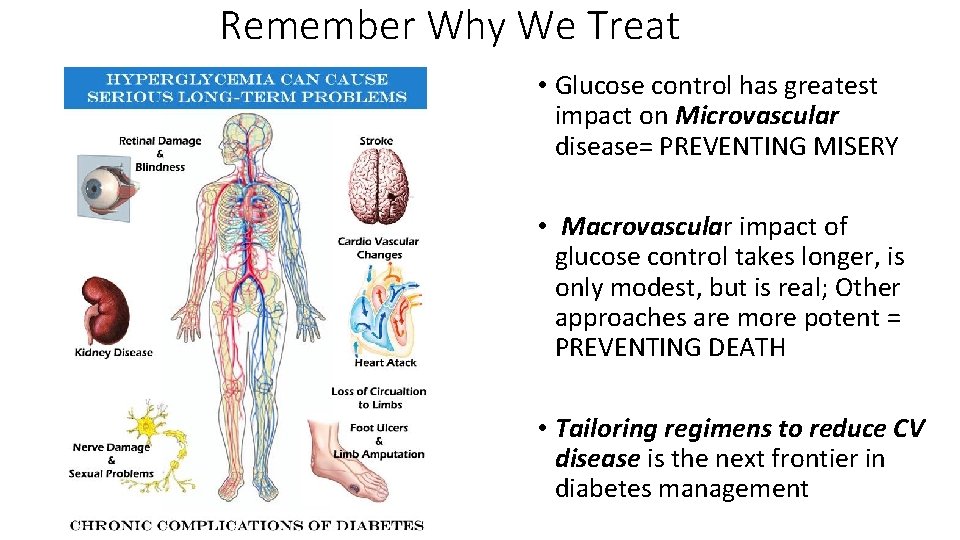
Remember Why We Treat • Glucose control has greatest impact on Microvascular disease= PREVENTING MISERY • Macrovascular impact of glucose control takes longer, is only modest, but is real; Other approaches are more potent = PREVENTING DEATH • Tailoring regimens to reduce CV disease is the next frontier in diabetes management

What outcomes do we really care about in diabetes? CLINICALLY IMPORTANT OUTCOMES: - Macrovascular: MI, stroke, CV death - Microvascular: renal disease, neuropathy, retinopathy - adverse events SURROGATE (INTERMEDIATE) OUTCOMES: - Hb. A 1 c lowering - failure of monotherapy to lower glucose levels
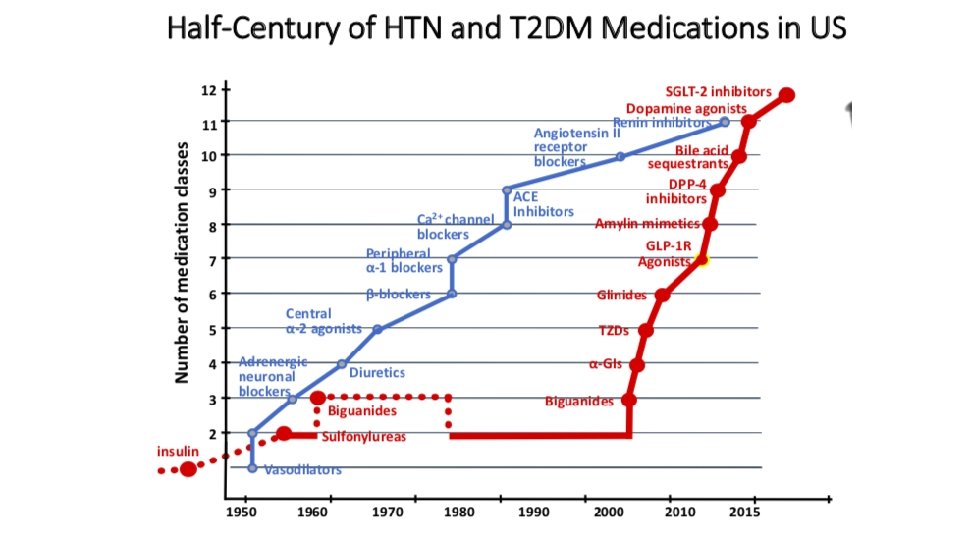

Outcome: Macrovascular (CV) events • Since 2008, the FDA has required evidence demonstrating the CV safety for newly approved glucose-lowering medications (CV outcome trials). • A large number of CV outcome trials have now been conducted demonstrating CV non-inferiority and/or superiority of newer glucose lowering medications (e. g. DPP- 4’s, SGLT-2’s, GLP-1 RA’s). • Primary outcome: 3 -point MACE (CV death, MI, stroke) • CV effects appear to be independent of effects on Hb. A 1 c.
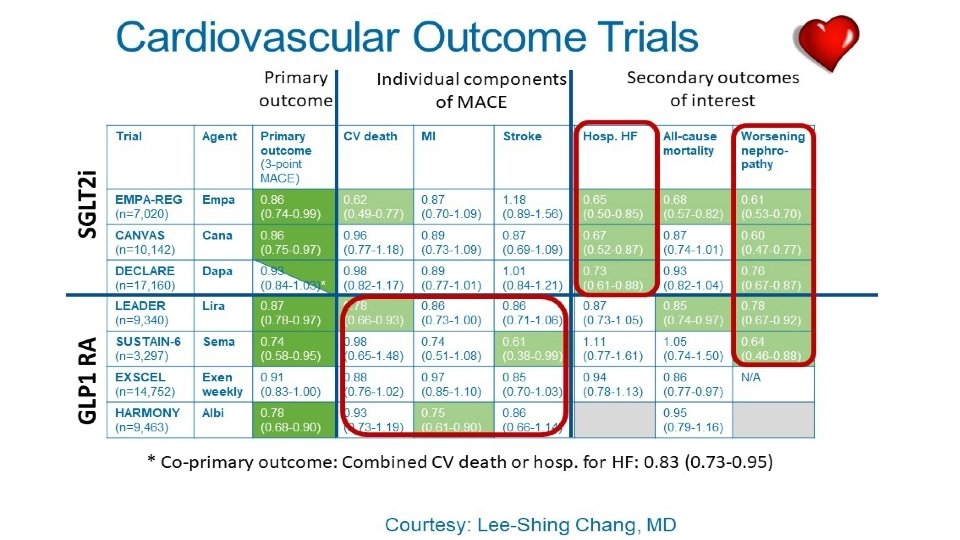

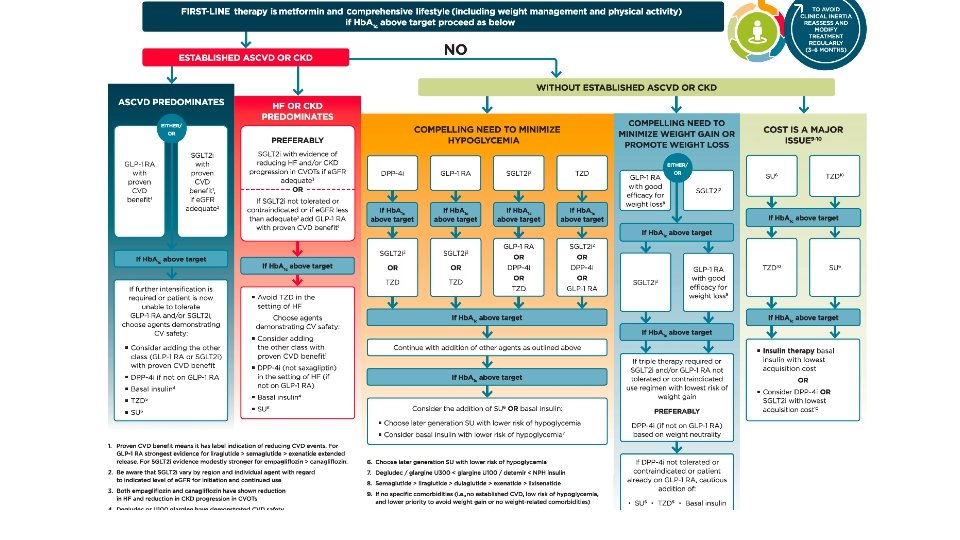
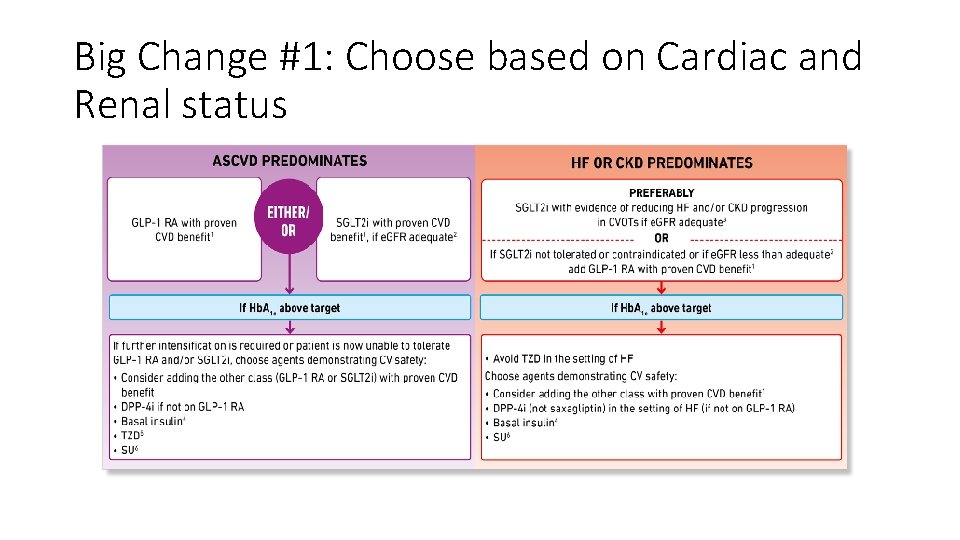
Big Change #1: Choose based on Cardiac and Renal status

Mechanisms of Cardio-renal Benefit: SGLT-2 Inhibitors vs GLP-1 Receptor Agonists

GLP-1 RA vs. SGLT-2 Inhibitor - Positives • GLP-1 – RA • Greater A 1 c reduction • Greater weight loss • No hypoglycemia • Probably more anti- atherogenic potential • Indicated for all levels of GFR (except for exenatide) • Can be once weekly • SGLT-2 inhibitor • Oral • No hypoglycemia • Better for heart failure • Probably better for CKD • Lower cost • Not depend upon Beta-cell function

GLP-1 RA vs. SGLT-2 Inhibitor - Negatives GLP-1 – RA SGLT-2 inhibitor • Injection • Less A 1 c lowering • Nausea • Genital mycotic infections • Higher cost • Volume depletion • Lesser efficacy with lower ���� -cell • DKA reserve • Less effective at low GFR

GLP-1 RA: Safety Warnings • Acute Kidney Injury • Pancreatitis • Medullary Cancer of the Thyroid • Gallbladder conditions (Liraglutide) • Retinopathy (Semaglutide)

GLP-1 agonists common cautions and concerns Not so Real • GI intolerance - Very common with exenatide, semaglutide, liraglutide • Gallstone disease - Liraglutide • Pancreatitis – Low risk - In Practice, often Gallstone mediated - FDA has previously warned of an increased (post-marketing) risk of acute pancreatitis among users of exenatide, but this risk appears low and not clearly related to taking the drug - Liraglutide and semaglutide: elevated amylase and lipase activity, without symptoms of acute pancreatitis. • Thyroid cancer Medullary TC: An increased incidence of C-cell neoplasia in rodents, however, no established mechanism in humans and no increased incidence of nodular disease or any form of thyroid cancer • Hypotension Systolic blood pressure fell by 3. 6 mm Hg in the liraglutide 1. 8 mg group compared with 0. 7 mm Hg in the glimepiride group; clinically harmful low BP not described, not seen in practice • Pancreatic Cancer Multiple metananalyses or prospectively followed subjects show NO increased risk across all agents
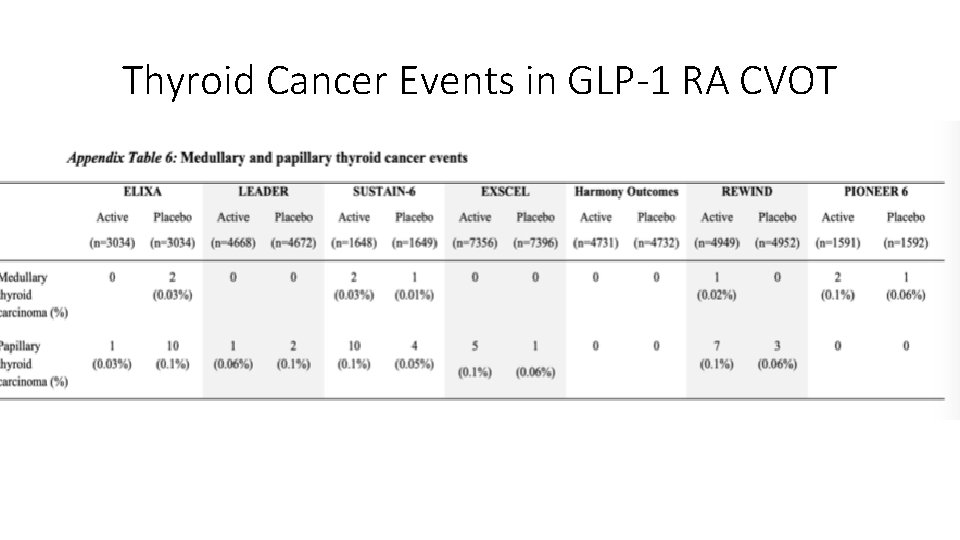
Thyroid Cancer Events in GLP-1 RA CVOT
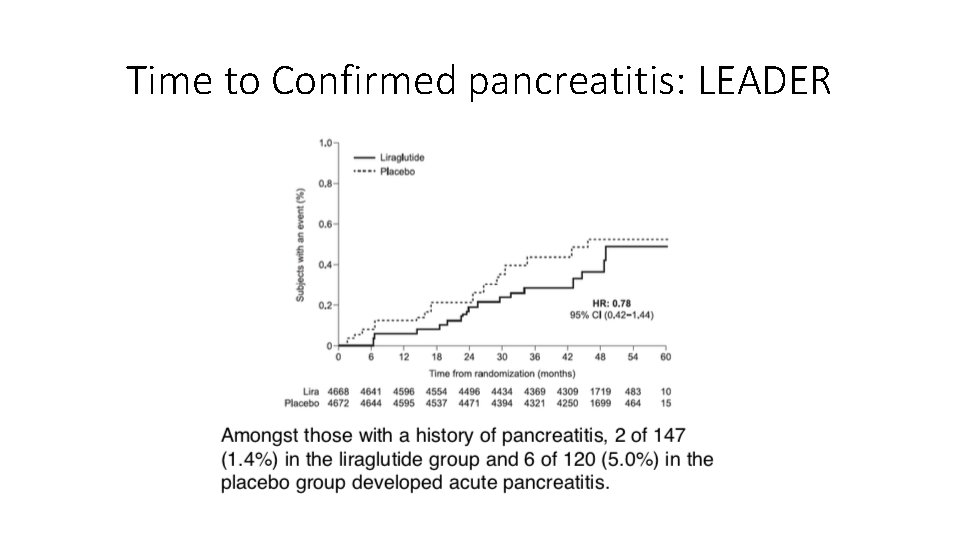
Time to Confirmed pancreatitis: LEADER

SGLT-2 Inhibitor: Safety Warnings • Acute Kidney Injury • Volume Depletion • Hyperkalemia • UTI’s • Genital Infections/Fournier’s gangrene • Diabetic Ketoacidosis • Amputations (canagliflozin, ertugliflozin)
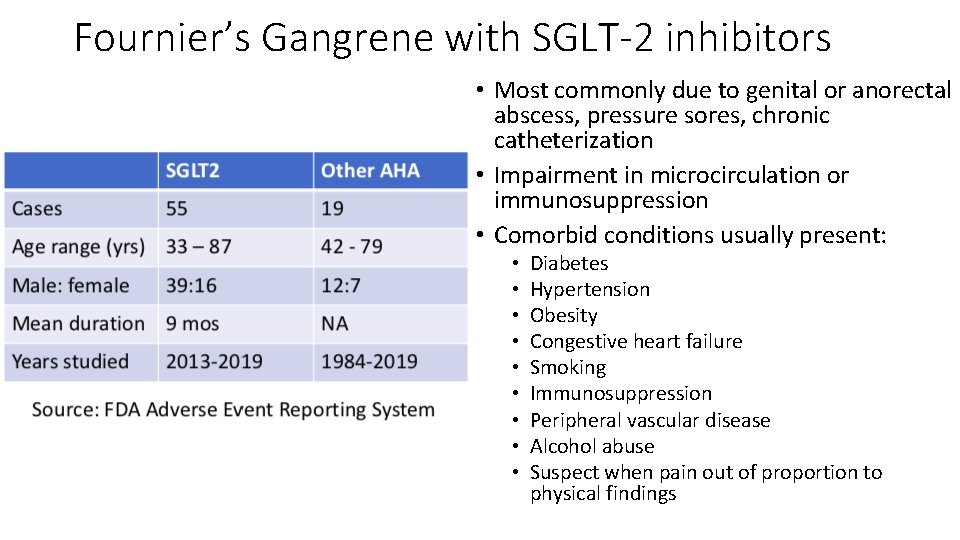

Fournier’s Gangrene with SGLT-2 inhibitors • Most commonly due to genital or anorectal abscess, pressure sores, chronic catheterization • Impairment in microcirculation or immunosuppression • Comorbid conditions usually present: • • • Diabetes Hypertension Obesity Congestive heart failure Smoking Immunosuppression Peripheral vascular disease Alcohol abuse Suspect when pain out of proportion to physical findings

How to Handle DKA Associated with Use of SGLT 2 Inhibitors • If a diabetic individual develops DKA during SGLT 2 inhibitor therapy, do not restart it, as there have been several reports of recurrent of DKA with continuous SGLT 2 inhibitor therapy • SGLT 2 inhibitor therapy should be also stopped during acute illness and at least 48 h before any planned procedure, so that a catabolic state is not aggravated and the risk of DKA is minimized. • Carefully consider alternative antihyperglycemic therapies
Minimizing Amputation Risks with SGLT-2 Inhibitors • Canagliflozin (SGLT-2 inhibitors) should be used with caution in individuals at risk for amputations, such as those with advanced PVD, severe peripheral neuropathy or prior history of lower-limb amputation or foot ulceration. • Minimize risk for volume depletion • Discontinue SGLT-2 inhibitors in the presence of active foot ulcer, infection.

Tips and Tricks: SGLT 2 inhibitors • Choose the right patient who can afford it • With heart disease • With heart failure • With CKD • Circumcised men without urinary hesitancy/frequency • Women without serious tinea • Educate • Hold for fasting • Hold for procedures

WHAT ABOUT OLDER MEDS? • Define the effects of metformin, sulfonylureas and thiazolidinedione on cardiovascular risk.

Metformin • Metformin available since 1995. • Mechanism: reduce hepatic glucose output. May also increase • insulin sensitivity. • Dosing: slow titration, with meals, 2000 mg/day maximal effective dose. • A 1 c lowering: 1 -2% • Pros: weight loss, no hypoglycemia, efficacy, metabolic improvements, outcome measurements, history of use. Possible cancer prevention effect • Cons: GI side-effects, renal insufficiency and lactic acidosis.

What should come after metformin? What is your practice?

Sulfonylureas • Available since 1954. • Names: Glipizide, Glyburide, Glimeperide • Mechanism: bind to SU receptor, stimulates insulin secretion = the insulin squeeze • Dosing: prior to meals, glucose-lowering effect plateaus around 1⁄2 max dose. • A 1 c lowering: 1 -2% • Pros: long history of use, cost, efficacy, daily dosing, outcomes measurements. • Cons: weight gain, hypoglycemia, (CV effects, beta- cell decline? ), caution with renal and liver dysfunction.

Do Sus increase CV mortality? • Recent meta-regression analysis of 19 RCTs with SUs as comparator • Sulfonylureas were associated with an increased risk of cardiovascular events and mortality in 5 of the 6 studies found to have low design bias (relative risks 1. 16– 1. 55) • In patients with ASCVD, it is wise to avoid agents that are known to act on the myocardial ATP sensitive potassium channel • Glyburide should be avoided • 3 rd generation glimepiride has not been found to have myocardial activity and do not appear to impair “ischemic preconditioning” • Glipizide – no human studies showing specific potential harm • • More reassurance from glimepiride? • A recent large CVOT comparing DPP 4 inhibitor linagliptin to glimepiride did not show a difference (CAROLINA) in MACE; linagliptin vs. placebo also did not show a difference (CARMELINA)

Tips and Tricks: Sulfonylurea • Do not use glyburide • Long acting; cardiovascular concerns • Start with glimepiride • Consider using premeal shorter acting (glipizide) as a “next step” after failure, may have more potency • Don’t titrate beyond the max effective dose • If control is poor after 10 years, not working, replace!

Thiazolidinediones • Available since 1997 • Pioglitazone is the TZD mostly available New Data • Lowers progression to cirrhosis in Nonalcoholic Steatohepatitis (Cusi, 2016) • Lowers risk of stroke (Kernan, 2016) • Prevents progression from prediabetes to diabetes (Kernan, 2016)

TZDs are affordable and effective but should I use them? Rosiglitazone Pioglitazone • Meta-analysis 1 of all available • Meta-analysis 3 of 19 trials randomized trials • MI risk increased 43% (p=0. 03) - CV • The primary outcome (death, nondeath risk increased 64% fatal MI, non-fatal stroke) was 18% LESS common with pioglitazone • (p=0. 06) (p=0. 005) • Risk of CV death was double the comparator (p=0. 02) • Pioglitazone: 4. 4% - Control: 5. 7% • MI risk confirmed with longer- term meta-analysis 2

Thiazolidinediones IRIS study The TZD, pioglitazone, ’d fatal/non-fatal stroke & MI by 24% (and 52% progression to DM) in 3895 insulin resistant patients with stroke or TIA. (Supports MACE results from PROactive study. )
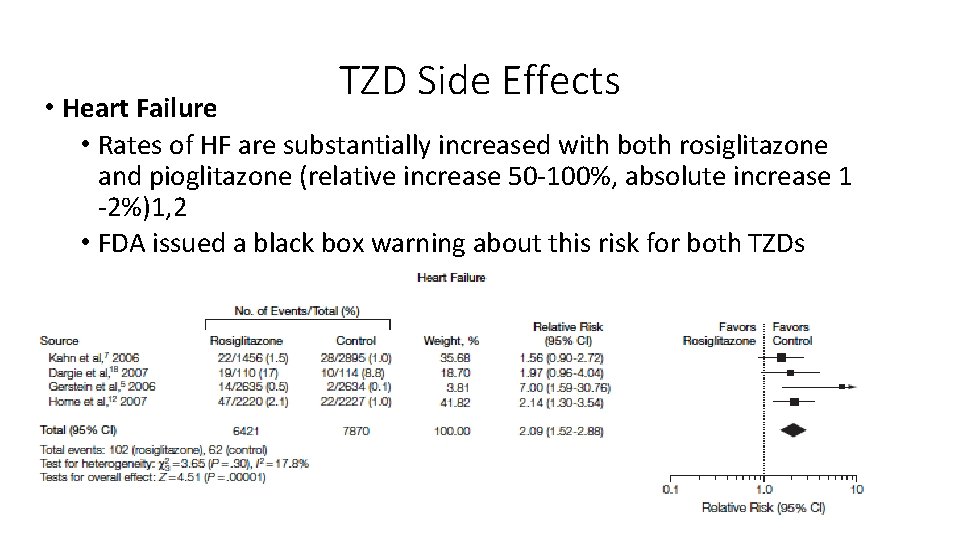
TZD Side Effects • Heart Failure • Rates of HF are substantially increased with both rosiglitazone and pioglitazone (relative increase 50 -100%, absolute increase 1 -2%)1, 2 • FDA issued a black box warning about this risk for both TZDs

Glitazones side effects • Fractures • Glitazones cause an increased risk of fracture in women • PROactive: 5. 1% (pio) v. 2. 5% (placebo) • ADOPT: 9. 3% (rosi) v. 3. 5% (glyburide) v. 5. 1% (metformin) • Hypoglycemia • Glitazones do not appear to increase risk of hypoglycemia; more limited data for other agents although risk theoretically low • Bladder cancer • debate about whether pioglitazone promotes or causes bladder cancer • dose response • FDA withdrew warnings about the use of pioglitazone being associated with an increased risk of bladder cancer.

Tips and Tricks: TZDs • Select the right patient: • Fatty liver • TIA, stroke history • MI history, normal EF, unable to take SGLT 2 i
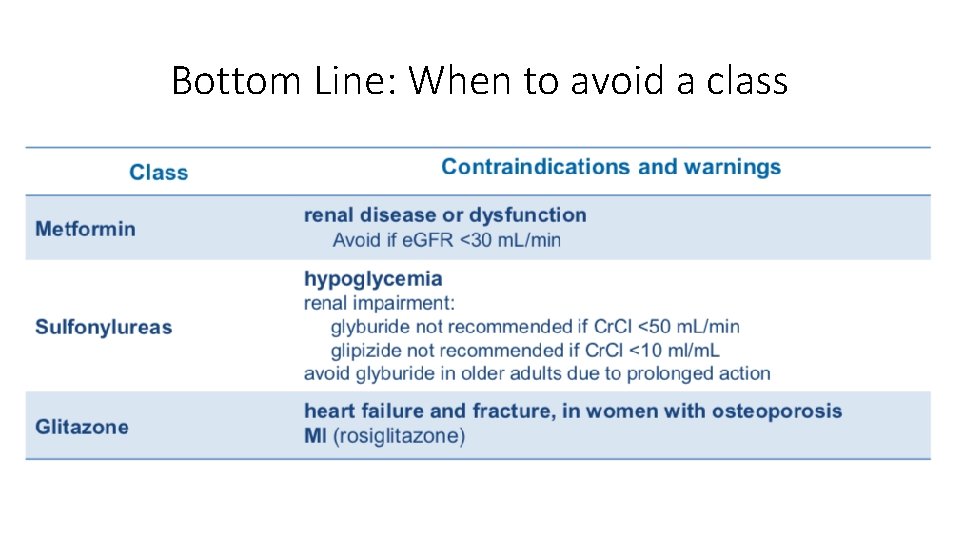

Bottom Line: When to avoid a class

Approach to Hyperglycemia • Endocrine Society: Patients ≥ 65 years old with diabetes should have their outpatient regimen “designed specifically to minimize hypoglycemia” • Relaxing glycemic targets for older patients with high burden of comorbidities and limited life expectancy may be appropriate, yet goals that minimize hyperglycemia are indicated for all patients

Is hypoglycemia risk reduction worth the price tag? Answer: Sometimes, mostly in older adults and those with ASCVD

• Mild symptomatic hypoglycemia is not associated with serious clinical effects. • Severe hypoglycemia is serious, particularly in the elderly • People > 80 years old, 25% of hospital admissions related to diabetes were due to severe hypoglycemia. Falls increase with lower A 1 c in those on insulin • Almost 50% presented with loss of consciousness. • Approximately 5% were associated with stroke, myocardial infarction, TIAs, or death • Severe hypoglycemia is associated with increase mortality, and the more frequent the events, the higher the risk of death • Observed in both Inpatient and outpatient settings • Increased risk of death is 10 x higher in the year after a severe event than in subsequent years (VADT) • Hypoglycemia limits the ability achieve and maintain glycemic control
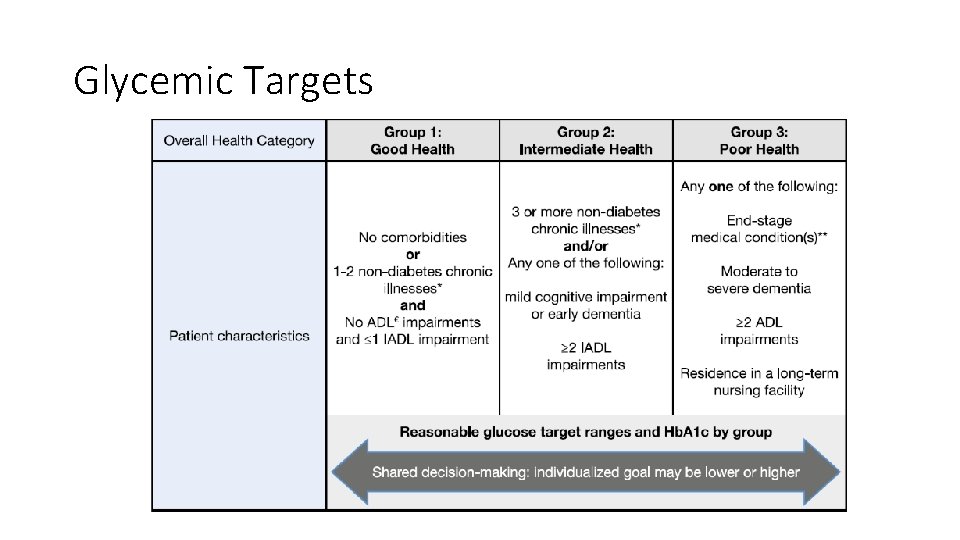
Glycemic Targets
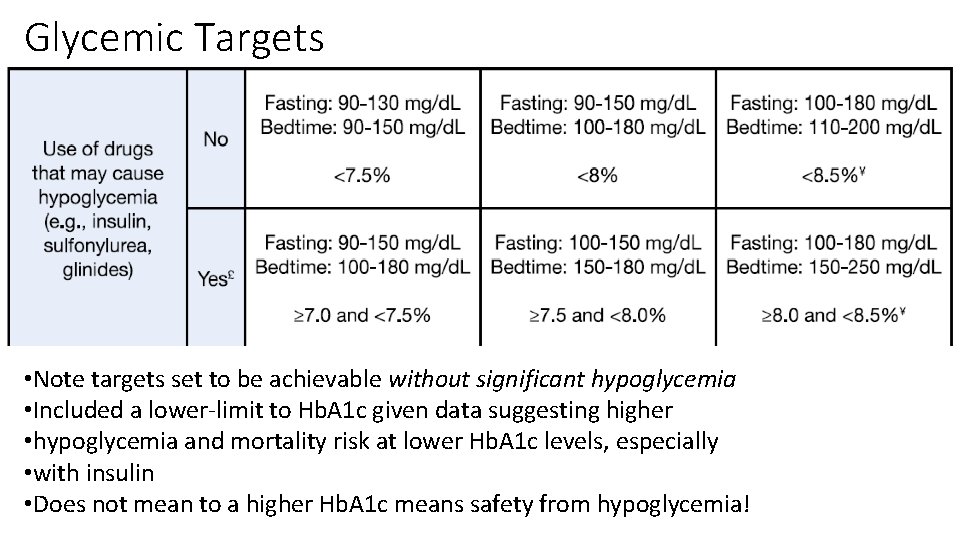

Glycemic Targets • Note targets set to be achievable without significant hypoglycemia • Included a lower-limit to Hb. A 1 c given data suggesting higher • hypoglycemia and mortality risk at lower Hb. A 1 c levels, especially • with insulin • Does not mean to a higher Hb. A 1 c means safety from hypoglycemia!
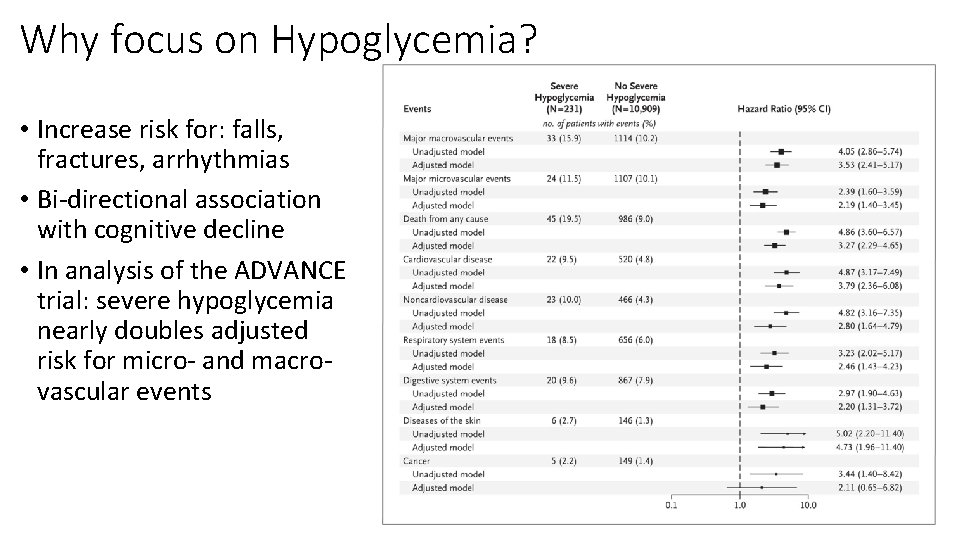
Why focus on Hypoglycemia? • Increase risk for: falls, fractures, arrhythmias • Bi-directional association with cognitive decline • In analysis of the ADVANCE trial: severe hypoglycemia nearly doubles adjusted risk for micro- and macrovascular events

GLP-1 Receptor Agonists • Low risk of hypoglycemia • +CV benefit (recent CVOT ~50% over age 65) • Careful with weight loss and appetite suppression in elderly population • Weekly dosing may be easier for care givers, help adhere to the treatment plan • Increased risk of pancreatitis has not been clearly established • GLP-1 agonists may be beneficial for cognition?

Reducing Risk for Adverse Reactions with GLP-1 Receptor Agonists • Avoid Volume Depletion/Nausea and Vomiting • Start low and go slow – consider even slower titration than recommended or use medication with lowest risk for nausea (Exenatide QW) • Advise about risk for nausea and vomiting, with recommendation to seek early medical attention if severe • Advise to serve smaller serving sizes and to eat more slowly – stop when no longer hungry

SGLT 2 inhibitors • Low risk for hypoglycemia, can promote weight loss • Likely class effect on reducing CV events, CHF and CKD progression • Risks include polyuria/dizziness, dehydration, genital mycotic infections, DKA • Canagliflozin: lower bone density at total hip (but not other sites), increased risk of limb fracture (but not spine); amputations? • No signal that side effects are worse in elderly compared to phase 3 studies

Reducing Risk for Adverse Reactions with SGLT-2 Inhibitors • Volume Depletion • Assess BP – if at goal, consider reducing doses of other antihypertensives, especially diuretics • Advise consumption of additional 500 ml of water daily • Genital Mycotic Infections • Consider risk-benefit in those with history of recurrent GMI or incontinence • Advise on careful genital hygiene • Consider use of barrier creams/ointments • DKA • • Avoid in patients with Type 1 diabetes Advise patients about symptoms Discontinue prior to planned procedures Early intervention with fluid, carbs and insulin in symptomatic patients • Amputations • Avoid volume depletion • Delay using in presence of ulcer or extremity infection, until healed • Advise patient to discontinue in presence of ulcer, lower extremity infection

Summary • The long-term benefits of SGLT-2 inhibitors and GLP-1 receptor agonists (over and beyond glycemic control and weight) outweigh the serious risks that have been described in clinical trials • Reduction in 3 -point MACE • Reduction in hospitalization for heart failure (SGLT-2 inhibitors) • Reduction in risk for progression of diabetic kidney disease • Counselling patients of the relative risks of and how to minimize serious adverse events is important to help patients make informed decisions.
- Slides: 47