Device related pressure Ulcer in Cardio thoracic intensive





- Slides: 12

Device related pressure Ulcer in Cardio thoracic intensive care unit Heart Hospital

CTICU Pressure Ulcer Project Team Leader Dr. Alejandro Kohn Tuli Physician Dr. Hesham Ahmed Safety Facilitator Dr. Poonam Gupta Quality Management Ms. Kakoli Roy Mr. Othman Otoum Nursing Staff Ms. Shiny Shiju Ms. Manal Hassan Dietician Ms. Aisha Pookunju Wound Care Nurses Ms. Sunitha Mathew Ms. Marife Quinto Physiotherapist Mr. Prasobh Jacob Mr. Syed Ansari Respiratory Therapist Mr. Ruzzel Galvez

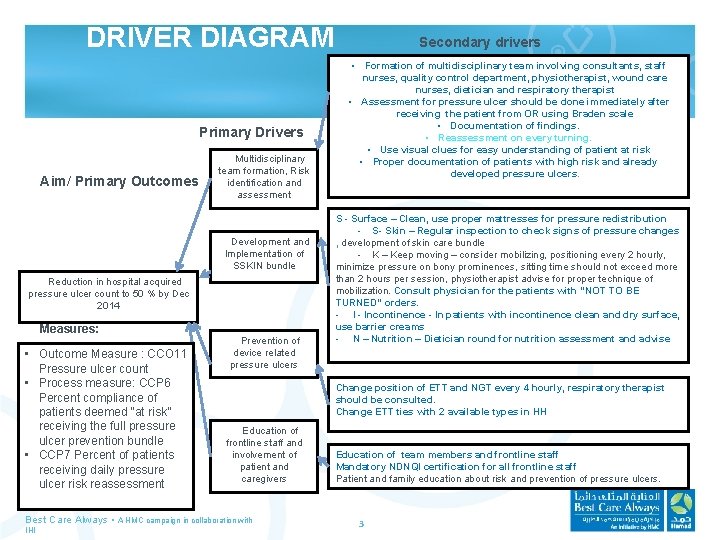
DRIVER DIAGRAM Primary Drivers Aim/ Primary Outcomes Multidisciplinary team formation, Risk identification and assessment Development and Implementation of SSKIN bundle Reduction in hospital acquired pressure ulcer count to 50 % by Dec 2014 Measures: • Outcome Measure : CCO 11 Pressure ulcer count • Process measure: CCP 6 Percent compliance of patients deemed “at risk” receiving the full pressure ulcer prevention bundle • CCP 7 Percent of patients receiving daily pressure ulcer risk reassessment Prevention of device related pressure ulcers • Formation of multidisciplinary team involving consultants, staff nurses, quality control department, physiotherapist, wound care nurses, dietician and respiratory therapist • Assessment for pressure ulcer should be done immediately after receiving the patient from OR using Braden scale • Documentation of findings. • Reassessment on every turning. • Use visual clues for easy understanding of patient at risk • Proper documentation of patients with high risk and already developed pressure ulcers. S - Surface – Clean, use proper mattresses for pressure redistribution - S- Skin – Regular inspection to check signs of pressure changes , development of skin care bundle - K – Keep moving – consider mobilizing, positioning every 2 hourly, minimize pressure on bony prominences, sitting time should not exceed more than 2 hours per session, physiotherapist advise for proper technique of mobilization. Consult physician for the patients with “NOT TO BE TURNED” orders. - Incontinence - In patients with incontinence clean and dry surface, use barrier creams - N – Nutrition – Dietician round for nutrition assessment and advise Change position of ETT and NGT every 4 hourly, respiratory therapist should be consulted. Change ETT ties with 2 available types in HH Education of frontline staff and involvement of patient and caregivers Best Care Always • A HMC campaign in collaboration with IHI Secondary drivers Education of team members and frontline staff Mandatory NDNQI certification for all frontline staff Patient and family education about risk and prevention of pressure ulcers. 3

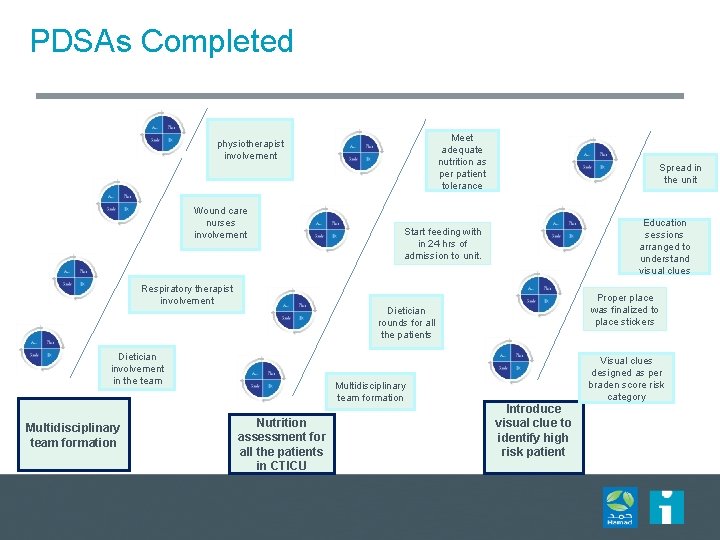
PDSAs Completed Meet adequate nutrition as per patient tolerance physiotherapist involvement Wound care nurses involvement Respiratory therapist involvement Education sessions arranged to understand visual clues Start feeding with in 24 hrs of admission to unit. Proper place was finalized to place stickers Dietician rounds for all the patients Dietician involvement in the team Multidisciplinary team formation Spread in the unit Multidisciplinary team formation Nutrition assessment for all the patients in CTICU Visual clues designed as per braden score risk category Introduce visual clue to identify high risk patient

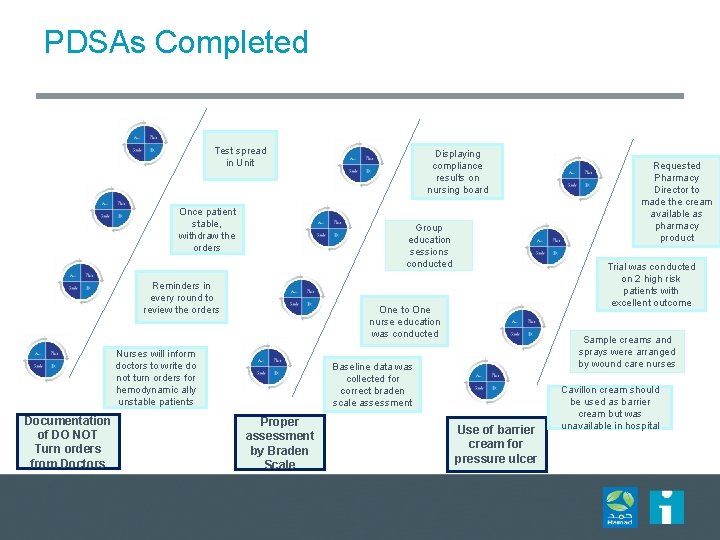
PDSAs Completed Test spread in Unit Once patient stable, withdraw the orders Group education sessions conducted Reminders in every round to review the orders Sample creams and sprays were arranged by wound care nurses Baseline data was collected for correct braden scale assessment Proper assessment by Braden Scale Requested Pharmacy Director to made the cream available as pharmacy product Trial was conducted on 2 high risk patients with excellent outcome One to One nurse education was conducted Nurses will inform doctors to write do not turn orders for hemodynamic ally unstable patients Documentation of DO NOT Turn orders from Doctors Displaying compliance results on nursing board Use of barrier cream for pressure ulcer Cavillon cream should be used as barrier cream but was unavailable in hospital

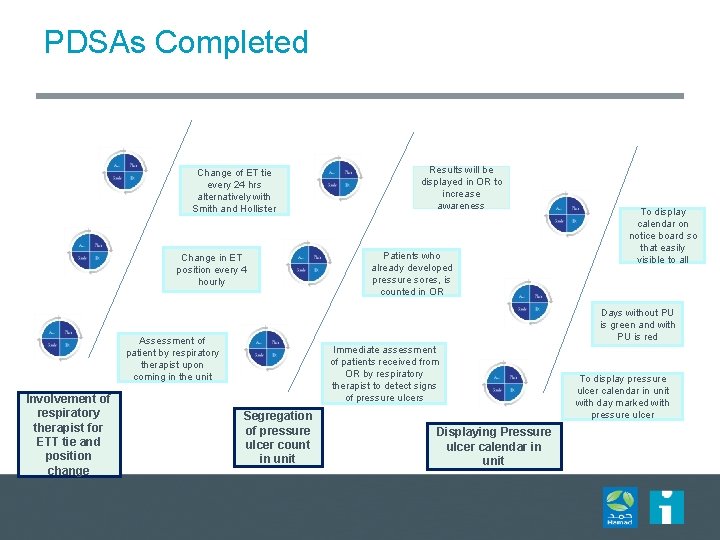
PDSAs Completed Change of ET tie every 24 hrs alternatively with Smith and Hollister Change in ET position every 4 hourly Patients who already developed pressure sores, is counted in OR To display calendar on notice board so that easily visible to all Days without PU is green and with PU is red Assessment of patient by respiratory therapist upon coming in the unit Involvement of respiratory therapist for ETT tie and position change Results will be displayed in OR to increase awareness Immediate assessment of patients received from OR by respiratory therapist to detect signs of pressure ulcers Segregation of pressure ulcer count in unit Displaying Pressure ulcer calendar in unit To display pressure ulcer calendar in unit with day marked with pressure ulcer

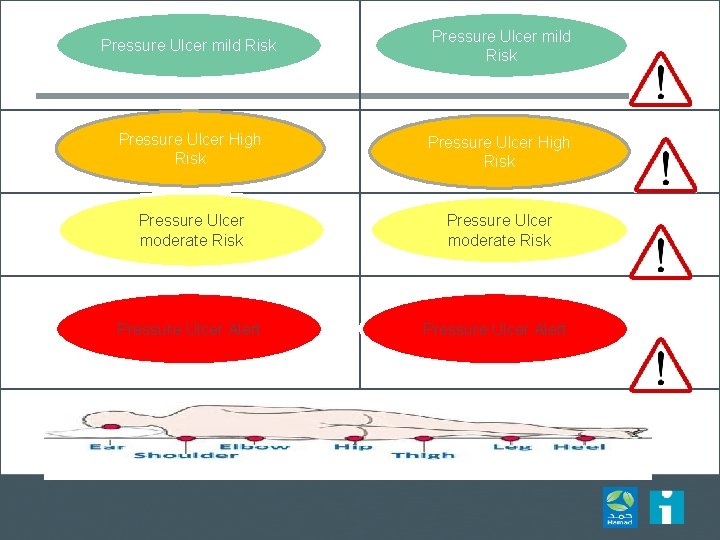
Pressure Ulcer mild Risk Pressure Ulcer High Risk Pressure Ulcer moderate Risk Pressure Ulcer Alert

Number of stage 2 pressure ulcers in the unit Number of stage 2 pressure ulcers 10 Number of pressure ulcers 9 8 7 6 5 4 3 2 1 0 April May June July August September October November April – Out of 9, 5 were device related Pressure ulcers May – Out of 4, 2 were device related pressure ulcers June – 2 device related pressure ulcers noted 150 days of no stage II pressure ulcer in this microsystem

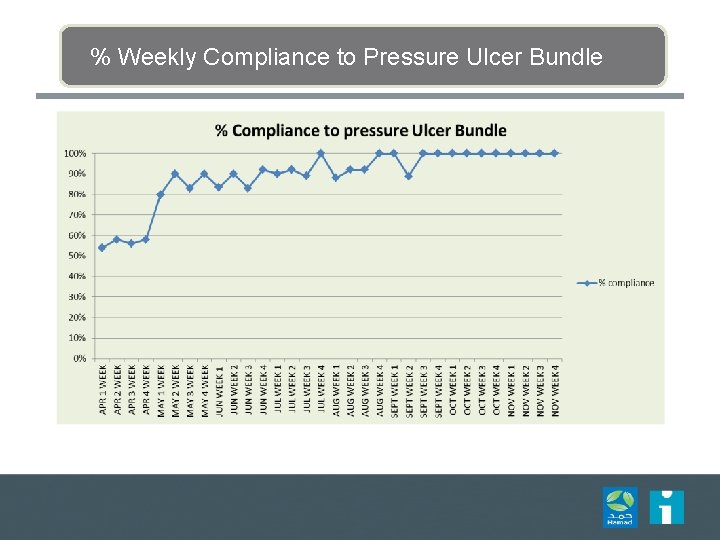
% Weekly Compliance to Pressure Ulcer Bundle

Pressure Ulcer Calendar in CTICU November 2014 Stage 2 and More 1 4 5 No HAPU 11 6 No HAPU 12 19 No HAPU 25 No HAPU 15 21 No HAPU 28 No HAPU 17 23 29 No HAPU 24 No HAPU 30 No HAPU No HAPU 10 16 22 3 No HAPU 9 No HAPU 27 No HAPU 8 14 20 26 No HAPU 13 No HAPU 18 7 No HAPU 2 No HAPU

Key Learnings 1 - There may be unconventional pressure ulcers in the unit, we have to do detailed study before planning interventions. 2 - Multidisciplinary team approach for pressure ulcer is key of success of this project as many healthcare professional are involved in patient care apart from doctors and nurses 3 - Introduction of visual cues is important part of the project which helped in identifying patients at risk without seeing the patient files. 4 - Barrier creams were not available in the unit. We managed to get 2 samples from wound care and tested it on 2 patients. After getting promising results, now its available in the stock. 5 - To share the data with the staff act as motivator for the team. 11

Recommendations and Next Steps We are planning to extend our project to OR as after data analysis, patients are transferred from OR with oral sores. 12