DEVELOPMENT OF DIGESTIVE SYSTEM MIDGUT HINDGUT By Dr

DEVELOPMENT OF DIGESTIVE SYSTEM, MIDGUT & HINDGUT By: Dr. Mujahid Khan

Midgut The derivatives of the midgut are: Ø The small intestine including most of the duodenum Ø The cecum, appendix, ascending colon and the right half to two-thirds of the transverse colon

Midgut Ø Midgut derivatives are supplied by the superior mesenteric artery Ø The midgut loop is suspended from the dorsal abdominal wall by an elongated mesentery Ø As the midgut elongates, it forms a ventral Ushaped loop of gut, the midgut loop Ø It projects into the remains of the extraembryonic coelom in the proximal part of the umbilical cord
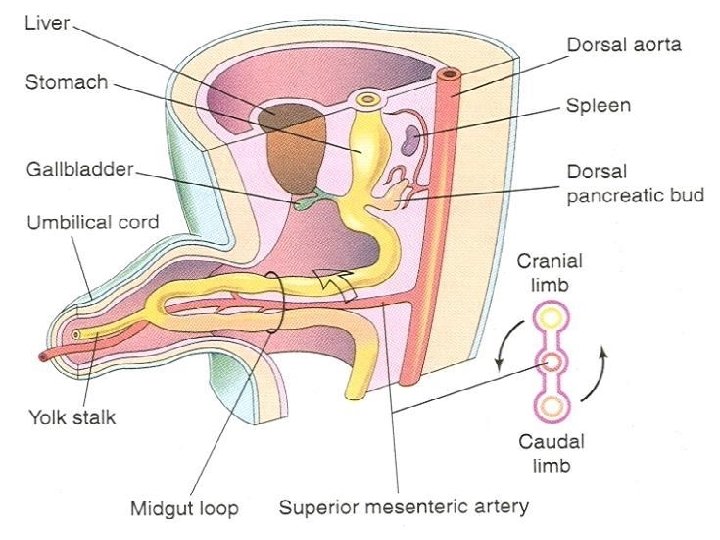

Midgut Ø At this stage the intraembryonic coelom communicates with extraembryonic coelom at the umbilicus Ø This movement of the intestine is a physiological umbilical herniation Ø It occurs at the beginning of the 6 th week Ø The midgut loop communicates with the yolk sac through the narrow yolk stalk or vitelline duct until the 10 th week
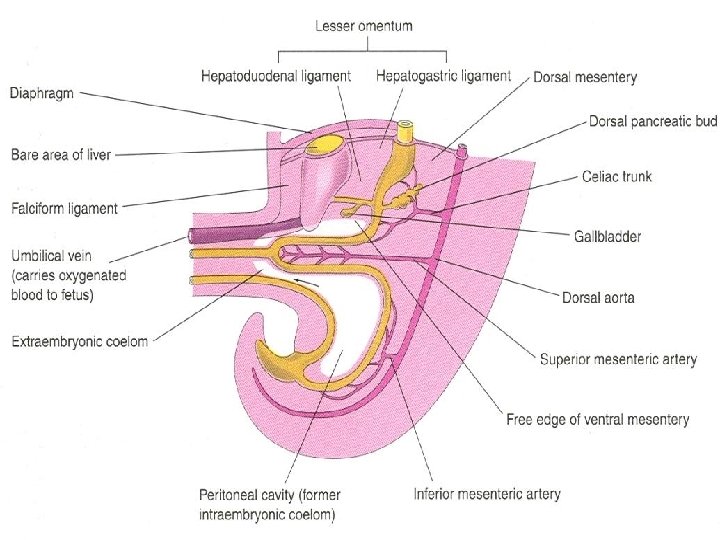

Midgut Ø Umbilical herniation occurs because there is not enough room in the abdomen for the rapidly growing midgut Ø The shortage of space is caused mainly by the relatively massive liver and two sets of kidneys during this stage of development Ø The midgut loop has a cranial limb and a caudal limb Ø Yolk stalk is attached to the apex of the midgut loop where the two limbs join
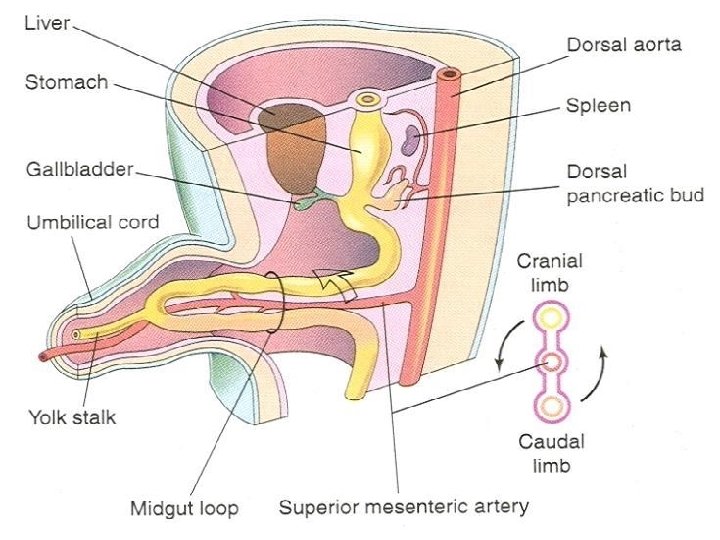

Midgut Ø The cranial limb grows rapidly and forms small intestinal loops Ø The caudal limb undergoes very little change except for development of cecal diverticulum which is a primordium of the cecum and appendix
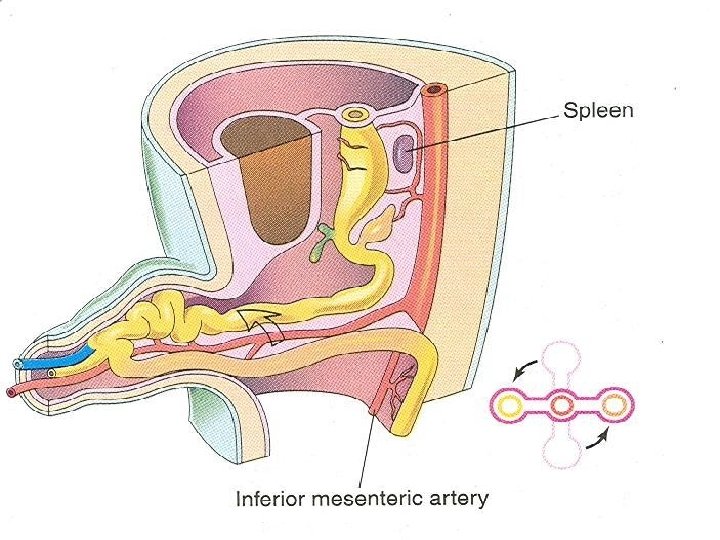

Rotation of Midgut Loop Ø While it is in the umbilical cord the midgut loop rotates 90º counterclockwise around the axis of superior mesenteric artery Ø This brings cranial limb to the right and the caudal limb to the left Ø During rotation the midgut elongates and forms intestinal loops e. g. Jejunum and ileum
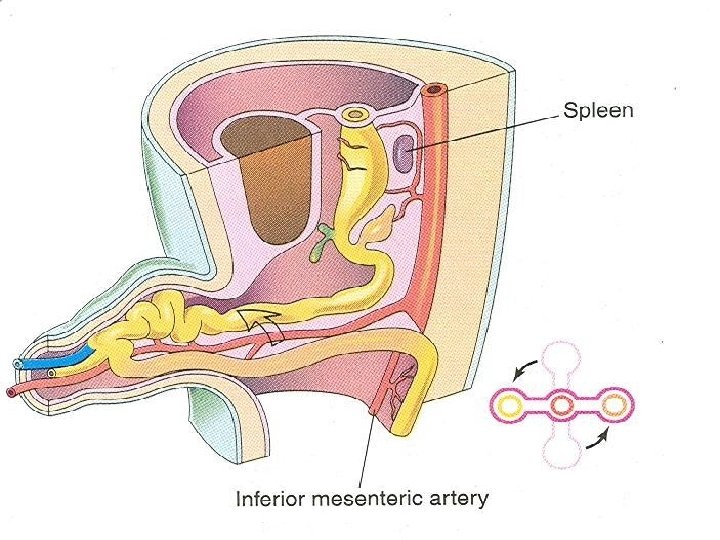

Return of Midgut Loop to Abdomen Ø During the 10 th week the intestines return to the abdomen Ø What causes the return of the intestine is not known Ø The decrease in the size of the liver and kidneys and the enlargement of the abdominal cavity are important factors Ø This process is called reduction of the physiological midgut hernia
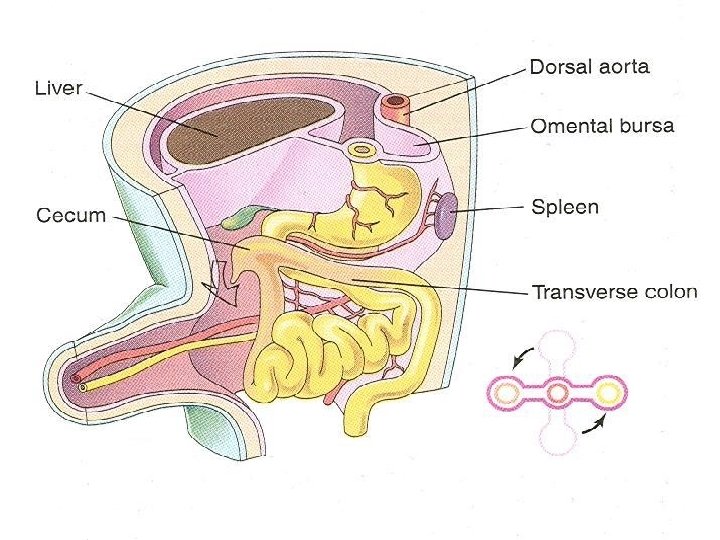

Return of Midgut Loop to Abdomen Ø The small intestine formed from cranial limb returns first Ø It passes posterior to the superior mesenteric artery and occupies the central part of the abdomen Ø As the large intestine returns, it undergoes further 180º counterclockwise rotation Ø Later it comes to occupy the right side of the abdomen

Cecum and Appendix Ø The primordium of cecum and appendix, the cecal diverticulum appears in the 6 th week as a swelling on the antimesenteric border of the caudal limb of the midgut Ø The apex of the cecal diverticulum does not grow as rapidly as the rest of it Ø The appendix is initially a small diverticulum of cecum
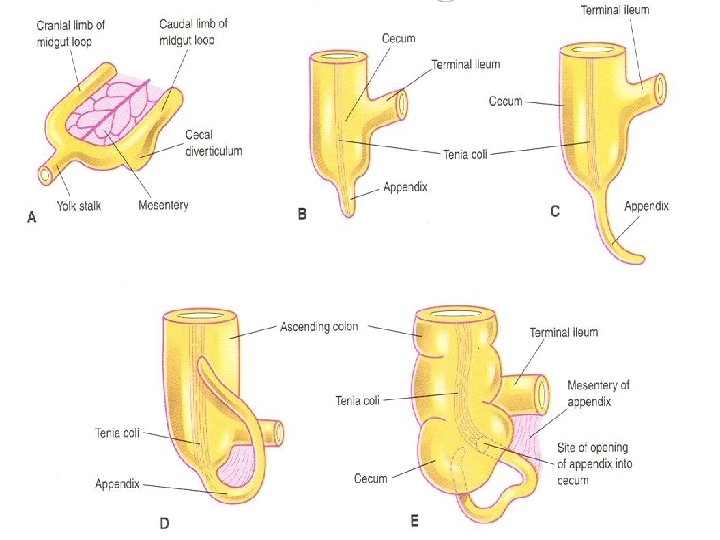

Cecum and Appendix Ø The appendix increases rapidly in length so that at birth it is a relatively long tube arising from the distal end of the cecum Ø After birth the wall of the cecum grows unequally with the result that appendix comes to enter the medial side Ø Appendix is considerably variant in position, retrocecal, retrocolic and pelvic appendix

Hindgut The derivatives of the hindgut are: Ø The left one-half of the transverse colon Ø Descending and sigmoid colons Ø Rectum and the superior part of the anal canal Ø The epithelium of the urinary bladder and most of the urethra

Hindgut Ø All hindgut derivatives are supplied by the inferior mesenteric artery Ø The junction between the segment of transverse colon derived from the midgut and that originated from the hindgut is indicated by the change in blood supply Ø Superior mesenteric artery is the midgut artery Ø Inferior mesenteric artery is the hindgut artery

Hindgut Ø The descending colon becomes retroperitoneal as its mesentery fuses with the peritoneum on the left posterior abdominal wall and then disappears Ø The mesentery of the sigmoid colon is retained but it is shorter than in the embryo

Cloaca Ø This terminal part of the hindgut is an endoderm-lined chamber that is in contact with the surface ectoderm at the cloacal membrane Ø This membrane is composed of endoderm of the cloaca and ectoderm of the proctodeum or anal pit Ø The cloaca, the expanded terminal part of the hindgut receives the allantois
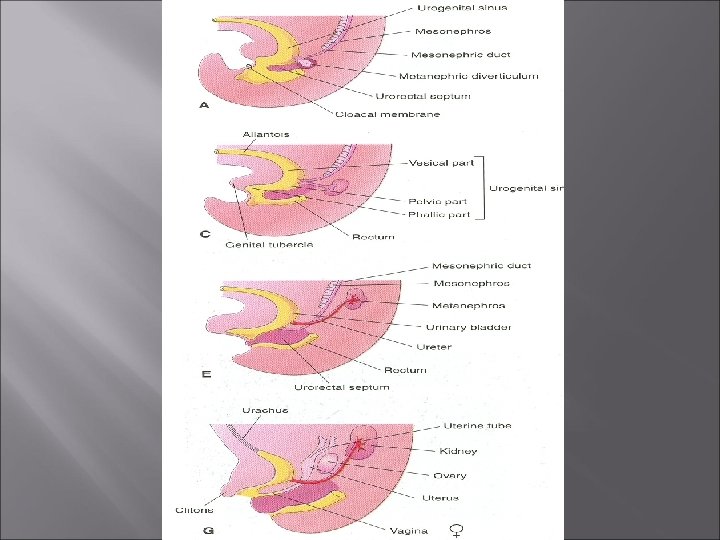

Partitioning of Cloaca Ø The cloaca is divided into dorsal and ventral parts by a wedge of mesenchyme, the urorectal septum Ø It develops in the angle between the allantois and hindgut Ø As the septum grows toward the cloacal membrane , it develops forklike extensions that produce infoldings of the lateral walls of the cloaca

Partitioning of Cloaca Ø These folds grow toward each other and fuse to form a partition that divides the cloaca into two parts Ø The rectum and cranial part of the anal canal dorsally Ø The urogenital sinus ventrally
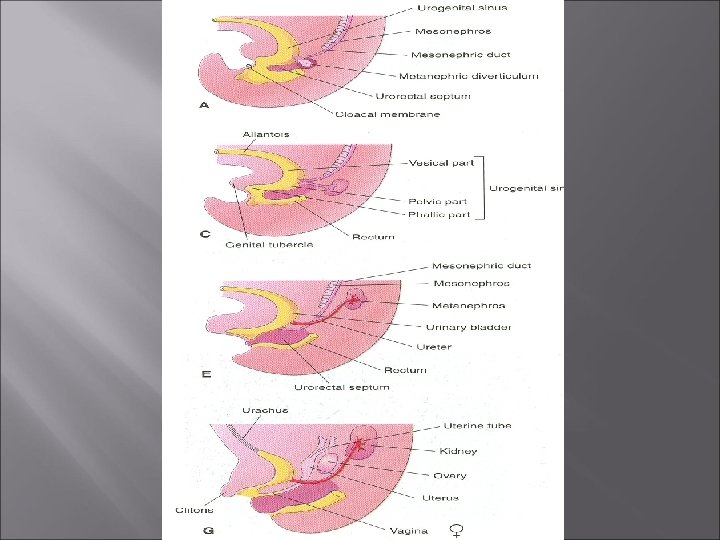

Partitioning of Cloaca Ø By the seventh week, the urorectal septum has fused with the cloacal membrane Ø Dividing it into a dorsal anal membrane and a larger ventral urogenital membrane Ø The area of fusion of the urorectal septum with the cloacal membrane is represented in the adult by the perineal body

Partitioning of Cloaca Ø The perineal body is a fibromuscular node and a landmark of perineum where several muscles converge and attach Ø The urorectal septum also divides the cloacal sphincter into anterior and posterior parts Ø The posterior part becomes the external anal sphincter Ø The anterior part develops into the superficial transverse perineal, bulbospongiosus and ischiocavernosus muscles

Partitioning of Cloaca Ø This developmental fact explains why one nerve, the pudendal nerve supplies all these muscles Ø The anal membrane usually ruptures at the end of the eighth week Ø This brings the distal part of the digestive tract into communication with the amniotic cavity

Anal Canal Ø The superior two-thirds of the adult anal canal is derived from the hindgut Ø The inferior one-third develops from the proctodeum Ø The junction between the epithelia of the two parts is indicated by the irregular pectinate line Ø This line is located at the inferior limit of the anal valves Ø It indicates the former site of anal membrane
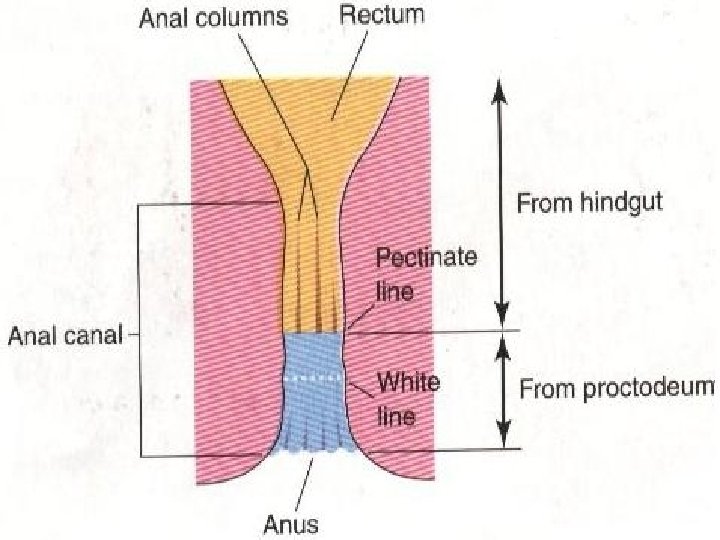

Anal Canal Ø About 2 cm superior to the anus is an anocutaneous line or white line Ø This demarcates where the anal epithelium changes from columnar to stratified squamous Ø At the anus, the epithelium is keratinized and continuous with the skin around the anus Ø Because of its hindgut origin the superior two-thirds of the anal canal are mainly supplied by the superior rectal artery
Anal Canal Ø Because of its origin from the proctodeum, the inferior one-third of the anal canal is supplied mainly by the inferior rectal arteries Ø The differences in blood supply, nerve supply, venous and lymphatic drainage of anal canal are important clinically, when considering the metastasis of cancer cells

Anal Canal Ø The characteristics of carcinomas in the two parts are different Ø Tumors in the superior part are painless and arise from columnar epithelium Ø Tumors in the inferior part are painful and arise from stratified squamous epithelium
Congenital Omphalocele Ø This anomaly is a persistence of the herniation of abdominal contents into the proximal part of the umbilical cord Ø Herniation of intestines into the cord occurs in about 1 in 5000 births Ø Herniation of liver and intestines in 1 of 10, 000 births Ø Size of the hernia depends on its contents

Congenital Omphalocele Ø The abdominal cavity is proportionately small when there is an omphalocele Ø Immediate surgical repair is required Ø Omphalocele results from failure of the intestines to return to the abdominal cavity Ø The covering of the hernial sac is the epithelium of the umbilical cord which is a derivative of the amnion

Umbilical Hernia Ø When the intestines return back to the abdominal cavity during the 10 th week and then herniate through an imperfectly closed umbilicus, an umbilical hernia forms Ø This is different from the omphalocele Ø In umbilical hernia the protruding mass is covered by subcutaneous tissue and skin Ø Hernia reaches its maximum size at the end of the first month after birth

Umbilical Hernia Ø It usually ranges from 1 to 5 cm Ø The defect through which the hernia occurs is the linea alba Ø Hernia protrudes during crying, straining, or coughing Ø It can easily be reduced through the fibrous ring at the umbilicus Ø Surgery is not usually performed until it persists to the age of 3 to 5 years

Meckel Diverticulum Ø This outpouching is one of the most common anomalies of the digestive tract Ø This congenital ileal diverticulum occurs in 2 to 4% of people Ø 3 to 5 times more prevalent in males than females Ø It sometimes becomes inflamed and causes symptoms that mimic appendicitis
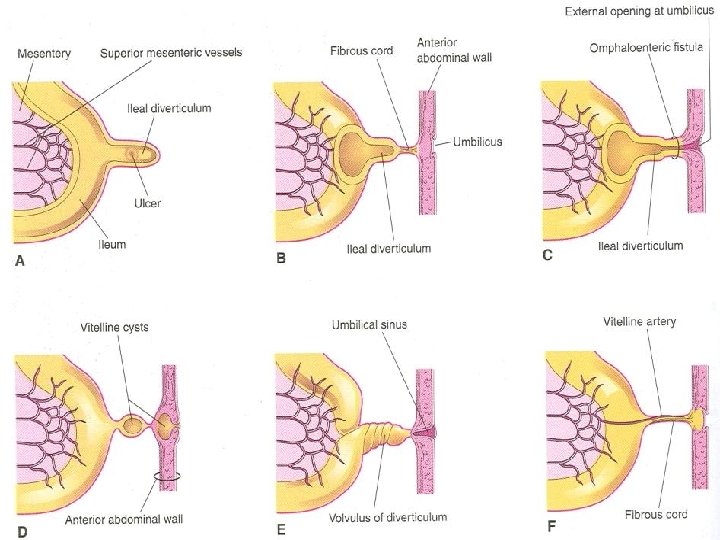

Meckel Diverticulum Ø The wall of the diverticulum contains all layers of the ileum and may contain small patches of gastric and pancreatic tissues Ø The gastric mucosa often secretes acid, producing ulceration and bleeding Ø It is the remnant of the proximal part of the yolk stalk Ø It typically appears as a fingerlike pouch about 3 to 6 cm long

Meckel Diverticulum Ø It arises from the antimesenteric border of the ileum 40 to 50 cm from the ileocecal junction Ø It may be connected to the umbilicus by a fibrous cord or an omphaloenteric fistula

Congenital Megacolon Ø A part of the colon is dilated because of the absence of autonomic ganglion cells in the myenteric plexus distal to the dilated segment of colon Ø The enlarged colon has the normal number of ganglion cells Ø The dilation results from failure of peristalsis in the aganglionic segment Ø In most cases only rectum and sigmoid colon are involved

Congenital Megacolon Ø It is the most common cause of neonatal obstruction of the colon Ø Accounts for 33% of all neonatal obstruction Ø Males are affected more often than females Ø It results from failure of neural crest cells to migrate into the wall of the colon during the 5 th and 6 th weeks Ø This results in failure of parasympathetic ganglion cells to develop in Auerbach plexuses

Imperforate Anus Ø It occurs about once in every 5000 newborn infants Ø More common in males Ø Most anorectal anomalies result from abnormal development of the urorectal septum Ø Results due to incomplete separation of the cloaca into urogenital and anorectal portions

Imperforate Anus Ø There is normally a temporary communication between rectum and anal canal dorsally, from the bladder and urethra ventrally Ø It closes when the urorectal septum fuses with the cloacal membrane Ø Lesions are classified as low or high depending on whether the rectum ends superior or inferior to the puborectalis muscle

Imperforate Anus Following are the low anomalies : Ø Anal agenesis with or without a fistula Ø Anal stenosis Ø Membranous atresia of anus Ø Anorectal agenesis with or without fistula
- Slides: 47