Developing Evidencebased Integrative Medicine Teaching Cases for Family

Developing Evidence-based Integrative Medicine Teaching Cases for Family Medicine Residency Curricula Rob Saper MD MPH, Ben Kligler MD MPH, Paula Gardiner MD, Andrea Gordon MD Robert Bonakdar MD STFM Annual Meeting January 17, 2006

Workshop Goals § Explore the potential for integrative medicine teaching cases in family medicine residency training § Generate creative constructive input for creating a set of 12 integrative medicine teaching cases for national dissemination to family medicine residencies

Workshop Flow • Reflective Exercise • Background of Project • Sample Case Discussion • Small Group Work – content, format, competencies & evaluation • Small Group Reports, Wrap and Next Steps

Workshop Flow • Reflective Exercise • Background of Project • Sample Case Discussion • Small Group Work – content, format, competencies & evaluation • Small Group Reports, Wrap and Next Steps

Workshop Flow • Reflective Exercise • Background of Project • Sample Case Discussion • Small Group Work – content, format, competencies & evaluation • Small Group Reports, Wrap and Next Steps

What is Integrative Medicine? § Combines evidence-based conventional medicine with evidence-based complementary alternative medicine (CAM)

NIH CAM Definition “A group of diverse medical and healthcare systems, practices, and products that are not presently considered to be part of conventional medicine. ”

What is Integrative Medicine? § Combines evidence-based conventional medicine with evidence-based complementary alternative medicine (CAM) § Patient-centered § Relationship-centered

What is Integrative Medicine? § Combines evidence-based conventional medicine with evidence-based complementary alternative medicine (CAM) § Patient-centered § Relationship-centered

A Brief History of Integrative Medicine: 1960 s – 1980 s

A Brief History of Integrative Medicine: 1990 -Present § Eisenberg 1990 NEJM survey § NIH Office Alternative Medicine § 1998 JAMA theme issue § NIH NCCAM established § 2002 NHIS survey § Emergence of integrative medicine § Growth of clinical, research, educational initiatives

Why Educate Family Medicine Residents about Integrative Medicine? • Large overlap with family medicine philosophy • Acknowledge diverse preferences for treatment • High CAM use in our pts • Potential for help and harm

Alternative Medicine Instruction In Medical Schools & FP Residency Programs • STFM 16 -question survey to all US medical school fp dept chairs & non-university-based residency directors about existing, planned, under consideration instruction in alternative medicine • Overall response rate 77. 9% (364/467) • 29. 7% (108/364) currently teaching • 6. 0% (22/364) starting to teach • 6. 3% (23/364) considering teaching • Most common in NE & Rocky Mountain regions • Predominantly elective (72. 2%) Carlston M, Stuart MR, Jonas W. Family Medicine. 29(8): 559 -62, 1997

Suggested Curriculum Guidelines on CAM: Recommendations of the STFM Group on Alternative Medicine • Widespread use of CAM provides new challenge to medical education • No standardized curriculum available for medical educators • STFM Group on Alternative Medicine over 2 years met at conferences and communicated via email • Consensus guidelines of recommended knowledge, skills, and attitudes in CAM for incorporation into the family practice residency training curriculum was developed Kligler B, Gordon A, Stuart M, Sierpina V. Family Medicine 1999; 31: 30 -3

BETH ISRAEL CAM MONTH: GOALS AND OBJECTIVES • Basic skills in nutrition, herbal medicine, mind-body medicine, acupressure • Referral skills for acupuncture, osteopathy, chiropractic, homeopathy • Self-care/reflection • Information mastery
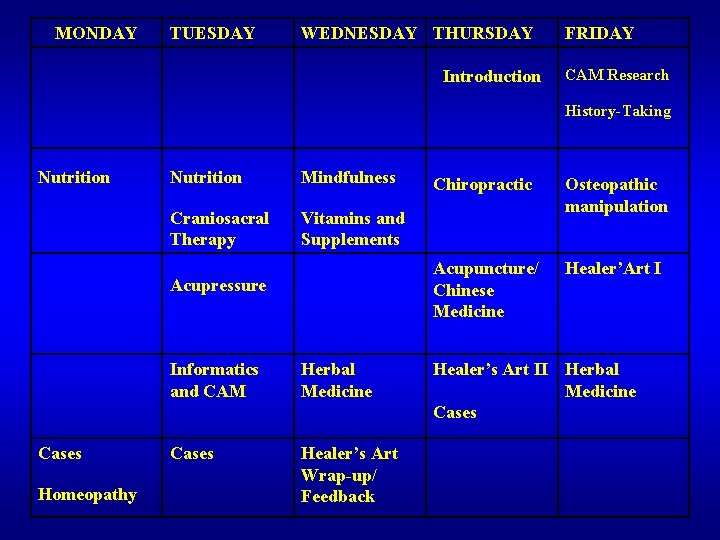
MONDAY TUESDAY WEDNESDAY THURSDAY Introduction FRIDAY CAM Research History-Taking Nutrition Mindfulness Craniosacral Therapy Vitamins and Supplements Acupressure Cases Homeopathy Informatics and CAM Herbal Medicine Cases Healer’s Art Wrap-up/ Feedback Chiropractic Osteopathic manipulation Acupuncture/ Chinese Medicine Healer’Art I Healer’s Art II Herbal Medicine Cases

IFM Program Goals • Develop/implement accredited model for a 4 yr FP residency integrating Integrative Medicine with conventional fp training • Graduates will manifest the philosophy and practice of Integrative Medicine – healing-oriented medicine – takes account of whole person (body, mind, spirit) including all aspects of lifestyle – Emphasizes therapeutic relationship

IFM Participating Programs & Faculty • Albert Einstein College of Medicine • Maine Medical Center • Middlesex Hospital Family Practice Residency Program • Oregon Health & Science University • University of Arizona College of Medicine • University of Wisconsin – Madison
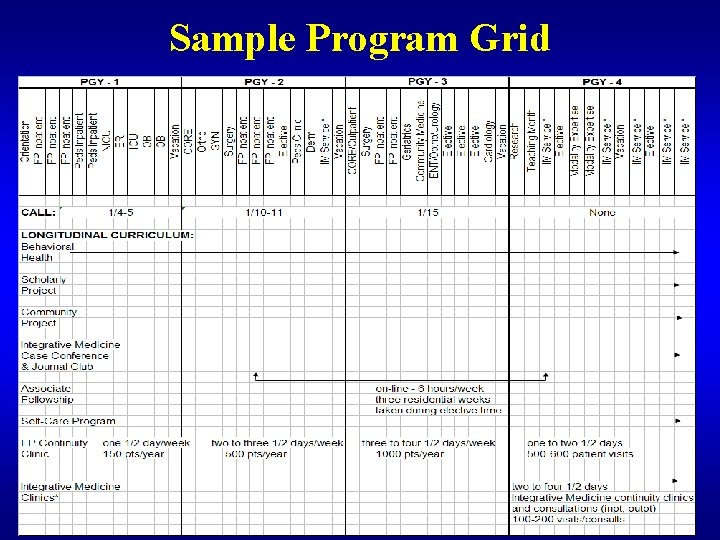
Sample Program Grid

Why Teaching Cases? • Educational theory/research learning aided by case-based problem solving • Learners can: – articulate their knowledge – identify info needed to answer ? s raised by case – collaborate with small group of learners – use experience & knowledge to resolve case – stimulate self-directed learning • Large growth at predoctoral level

Goal of Integrative Medicine Teaching Cases Project • Develop, pilot, evaluate, & disseminate a national integrative medicine competency -based curriculum of 12 teaching cases for family medicine residencies • Funded by NCCAM Career Development Award

Methods • Assemble Working Group • Assemble Advisory Group • Develop Competencies, Topics, & Formats • Case Development • Iterative Review & Revision • Dissemination & Evaluation

General Parameters of Cases • Illustrate 3 principles integrative medicine • Efficient • Interactive • Flexible

Workshop Flow • Reflective Exercise • Background of Project • Sample Case Discussion • Small Group Work – content, format, competencies & evaluation • Small Group Reports, Wrap and Next Steps

The Case Of Mrs. T: An Integrative Medicine Approach To Dyspnea “I get short of breath when I climb stairs and carry things. I love to walk, hike, be active. I like to be busy. It’s really impacted my life and my ability to do what I want to do. Our laundry is in the basement. I would get to the bottom of the stairs with a load of laundry. I wasn’t sure I wanted to climb up, due to my breathing getting labored. I remember coming home one day carrying bundles from the grocery store and then sitting on the couch. I felt very short of breath and it struck me how much more I

• What are 6 possible diagnoses for Mrs. T?

What additional information do you want and how do you ask for it? • • • HPI PMHx Medications Psychosocial History Habits History Family History ROS PE Testing

History of Present Illness Mrs. T is a lovely 77 year old widow who for approximately 9 months has been experiencing a mild amount of dyspnea on exertion, such as when she walks up one flight of stairs carrying a load of laundry, walking several blocks, and hiking. She complains of an associated chest tightness without nausea, vomiting, diaphoresis, or cough. Resting provides relief. In the past wheezing has been noted, and albuterol gives some relief. She quit smoking 30 years ago. Her cardiac risk factors include hypertension,

Past Medical History Remarkable for hypertension, CVA due to a ruptured right posterior cerebral artery aneurysm over 20 years ago with no significant residual disability, mitral valve prolapse, osteoporosis, kyphosis, chronic neck pain, seborrhea, glaucoma, and allergic rhinitis. She denies a history of depression or anxiety. Past Surgical History includes a craniotomy for the ruptured aneurysm, bilateral cataract surgeries, and excision of a basal cell

Medications, Supplements, And Complementary Therapy History • • • Dyazide 75/50 mg qd Axopt 1 qtt ou bid Chlortrimaton 4 mg 2 tid prn allergies Multivitamin Calcium-Magnesium 1000 -500 combination qd • Ibuprofen 800 tid prn • Massage therapy for neck pain

Psychosocial history • Mrs. T is originally from Ohio. She moved to the Boston area 10 years ago to live with her daughter, who is a free-lance journalist. They live together in an apartment in Cambridge. She is a retired nurse. Her husband died in a sudden accident in the 1980 s. She lost one child due to prematurity. She also lost an older sister due to ovarian cancer. She never remarried nor has an intimate partner. Although she has many close friends, she considers her daughter her best friend. Her greatest fear is what will happen to her daughter after she dies. Her Catholicism is a source of strength to her. She enjoys reading, doing crossword puzzles, house chores, and the outdoors.

Habits History • Mrs. T has a 23 pack year smoking history in the distant past. • She usually drinks 2 glasses of wine with dinner. She does not use recreational drugs. She drinks 2 cups coffee per day. A typical daily eating pattern is for breakfast, she has orange juice, cereal and milk; for lunch, 2 rice crackers with peanut butter; and for dinner, chicken or fish, vegetables, and salad. • She loves to walk, hike, and canoe but these have been limited due to her dyspnea. Her sleep is fine, without insomnia or frequent awakening.

Family History • Rremarkable for her father dying of CHF; her deceased mother had hypertension, diabetes, and osteoarthritis. She is the youngest and only surviving sibling of 5 children.

Review Of Systems • Neck pain, chronic. • Otherwise negative.

Physical Examination • Mrs. T is an alert thin elderly extremely pleasant woman in no respiratory distress. Her height is 5 feet, 4 inches, weight 121 lbs, temperature 97 degrees, blood pressure 175/100, heart rate 92, and respirations 16. Skin is normal turgor and color. She has a well-healed craniotomy scar. Her neck has mild decreased range of motion with tender hypertonic paracervical muscles. She has a mild kyphosis of the upper back. Her chest has bibasilar rales without wheezing. Cardiac exam is regular rate and rhythm without murmurs or S 3. Her abdomen is benign. Her extremities show no clubbing, cyanosis, or edema. Her neuro exam is nonfocal.

What Tests Would You Order?

Work-Up • • • CBC no anemia K= 2. 7 Echocardiogram normal, except for a patent foramen ovale with left to right shunt, trace to mild MR and TR. No evidence of LVH or systolic dysfunction. Pulmonary artery pressures are estimated to be 30 -35 mm Hg. • Exercise stress test with myoview Fair exercise tolerance (4. 6 mets). No
Work-Up • Spirometry Moderate obstruction w/o change after bronchodilator, nl lung volumes, normal diffusion capacity. • Chest Xray ill-defined patchy infiltrates, ? scarring • Chest CT scan no tumor, infiltrate
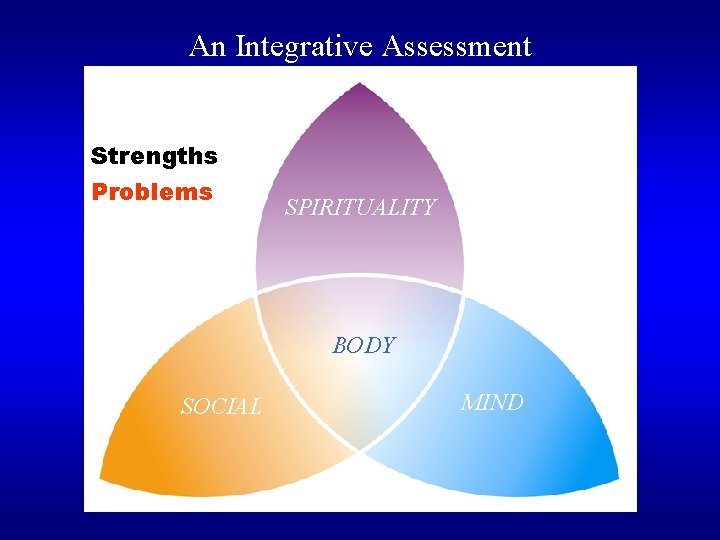
An Integrative Assessment Strengths Problems SPIRITUALITY BODY SOCIAL MIND

What Therapeutic Interventions Can You Try?

Therapeutic Interventions • Azmacort no subjective change in DOE or change in home peak flows • Serevent no change in DOE or peak flows • Singulair no effect • Discontinued dyazide due to hypokalemia. Started cozaar improved hypertension, no impact on DOE

What Next? • Pulmonary Referral – Unclear if asthma is cause – No evidence of interstitial lung disease, pulmonary vascular disease, or emphysema on CT. – Doubt patent foramen ovale is playing a role – Mild pulmonary hypertension. – Ordered cardiopulmonary stress test DOE felt to be from rapid shallow breathing & not using her full lung capacity, possibly in part due to kyphosis,

Primary Care F/u • Mrs. T was instructed in how to do deep breathing exercises (a. k. a. diaphragmatic breathing, 3 part breath, pranayama) in the office and with a handout. She was asked to practice 15 minutes daily, both at rest and during exertion, and to monitor her subjective dyspnea sensation and objective incentive

Evidence-based Rationale for Use of Deep Breathing Exercises in this setting • Yoga breathing decreases sensitivity and the ventilatory response to hypoxia and hypercapnea in healthy volunteers (Spicuzza L et al, Lancet 2000) • Deep breathing/meditation can lower anxiety (Waelde LC, J Clin Psychol 2004) • Deep breathing exercises in CHF patients lower dyspnea and improve exercise tolerance (Bernardi L et al, Lancet 1998) • Yoga breathing exercises in asthma improve symptoms of dyspnea without change in lung function parameters (Cooper S et al, Thorax 2003)

Mrs. T’s Response “I was tremendously relieved to have all the tests done and to know it wasn’t anything serious. It felt good to be taken seriously, which my previous doctor didn’t do. I’m not at all anxious about it now. My breathing now is very good. When I think I’m short of breath, I use the deep breathing exercises. Last Saturday I snowshoed up a 500 foot ascent with heavy boots, snowshoes, and poles. It was snowy and windy but I did it with no problem. The other day I climbed up the stairs with a big box of photo albums with no trouble. I can now do about 1950 on the spirometer, compared to 1700 before. I’ll occasionally forget to do the exercises, but when I get short of breath, I remember to breathe way I should, then I do, and it really helps. ”

Diaphragmatic Breathing Instruction • Focus on breath • 3 parts to the breath: lower, middle, and upper lungs • Always start with exhalation • Exhale through pursed lips slowly • Imagine a balloon in your belly and chest slowly inflating and deflating • Rest hands on abdomen initially until you get the hang of it

BREAK!

ACGME Competencies • • • Patient Care Medical Knowledge Practice Based Learning & Improvement Interpersonal and Communication Skills Professionalism Systems based Practice

Patient Care • • Effective respectful communication w/ pts Gather hx, develop assessment, formulate plan Use IT resources at point of care Competently perform procedures

Medical Knowledge • • Know about established and evolving medical scientific knowledge and how to apply to pt care Analytic approach to clinical situations

Practice Based Learning and Improvement • Locate, assess, and assimilate scientific evidence about your patient’s problems • Use IT to manage information, access on-line medical information; and support their own education

Interpersonal & Communication Skills • • • Create and sustain therapeutic ethical patient relationships Effective listening skills Work effectively with others as a member or leader of a health care team

Professionalism • • • Demonstrate respect, compassion, integrity Commitment to ethical principles Sensitive and responsive to patients’ culture, age, gender, and disabilities

Systems based Practice • • Understand interrelationships of patient care, other health care providers, health care organizations, and society Advocate for quality patient care and assist patients in dealing with system complexities
- Slides: 54