DESIGNER INSULINS IN GESTATIONAL DIABETES DR T RAMANI

DESIGNER INSULINS IN GESTATIONAL DIABETES DR. T. RAMANI DEVI MD DGO FICS FICOG RAMAKRISHNA NURSING HOME TRICHY
Maternal Diabetes Two lives. . Twice as special An oppurtunity for primary prevention -Maternal health -Child health

Definition GDM is defined as carbohydrate in tolerance of variable severity with onset or first recognition during pregnancy. The definition is applicable regardless of whether insulin is used to treat the disease or if the condition persists after pregnancy. It does not exclude the possibility that unrecognized glucose intolerance may have antedated the pregnancy

Introduction • Incidence of GDM is variable from 17% to 29% of all pregnancies • Associated with maternal and perinatal complications. • 90% of all Diabetics are GDM and 10% are due to pregestational diabetes. • 4 million pregnancies in India are complicated by GDM • This may contribute a part of MMR in India



GDM prevalence linked to background IGT rates GDM 2% 1980 s 1990 s 2000 s Agarwal S, Gupta AN. Gestational Diabetes. J Assoc Physicians India 1982; 30: 203 7. 6% Narendra J, Munichoodappa C, et al, Prevalence of glucose intolerance during pregnancy. Int J Diab Dev Countries 1991; 11: 24 16. 6% V Seshiah, V Balaji, Madhuri S Balaji, CB Sanjeevi, A. Green. Gestational Diabetes Mellitus in India. J Assoc Physicians India 2004; 52: 707 IGT 2% Ramachandran A, et. al. , High prevalence of diabetes in an urban population in south India. BMJ 1988; 3; 297(6648): 587 -90 8. 2% Ramachandran A, Snehalatha c, Dharmaraj D, Viswanathan M. Prevalence of glucose intolerance in Asian Indians. Diabetes Care 1992; 15: 1348 -55 14. 5% Ramachandran A, Snehalatha C, Kapur A, Vijay V, Mohan V, Das AK, Rao PV, Yajnik CS, Prasanna Kumar KM, Nair JD. For the Diabetes Epidemiology Study Group in India (DESI). Diabetologia 2001; 44: 1094 -1101.

Significance of Diabetes and Pregnancy • Malformation rate in 94/1000 Vs 9. 7/1000 in general population • Still birth is 15 times higher 25/1000 Vs 5/1000 • PNM is 3 times higher 19. 9/1000 Vs 6. 8/1000 • Recent concept of adult diseases having their origin inutero insults has been established. • 1989 WHO/IDF discussed the problem of hyperglycemia in pregnant women. They wanted to achieve pregnancy outcome in diabetic women same as in non diabetic women.
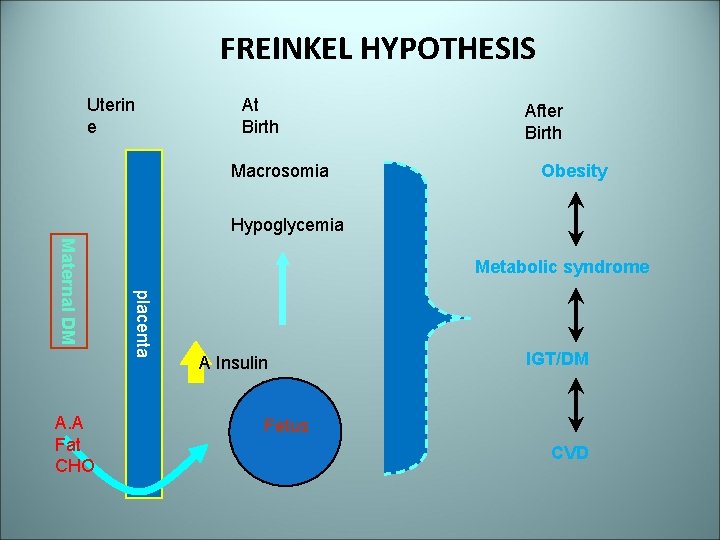
FREINKEL HYPOTHESIS Uterin e At Birth Macrosomia After Birth Obesity Hypoglycemia placenta Maternal DM A. A Fat CHO Metabolic syndrome A Insulin IGT/DM Fetus CVD

Diabetes and Pregnancy – Why it is relevant?
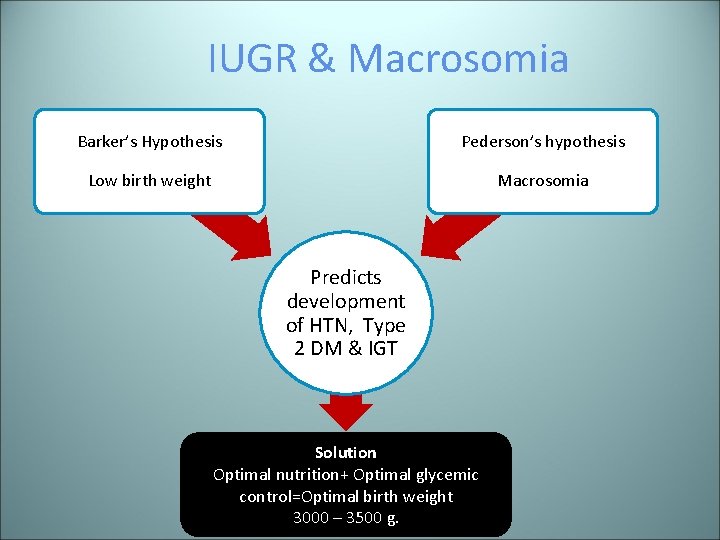
IUGR & Macrosomia Barker’s Hypothesis Pederson’s hypothesis Low birth weight Macrosomia Predicts development of HTN, Type 2 DM & IGT Solution Optimal nutrition+ Optimal glycemic control=Optimal birth weight 3000 – 3500 g.


SCREENING FOR DIABETES
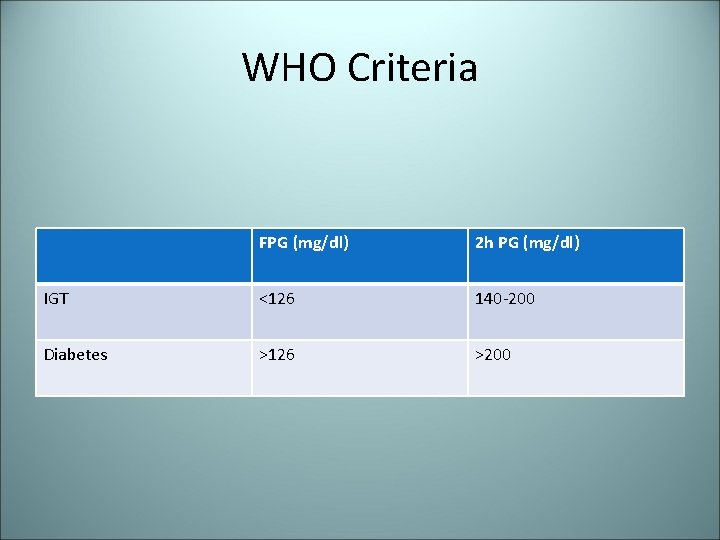
WHO Criteria FPG (mg/dl) 2 h PG (mg/dl) IGT <126 140 -200 Diabetes >126 >200
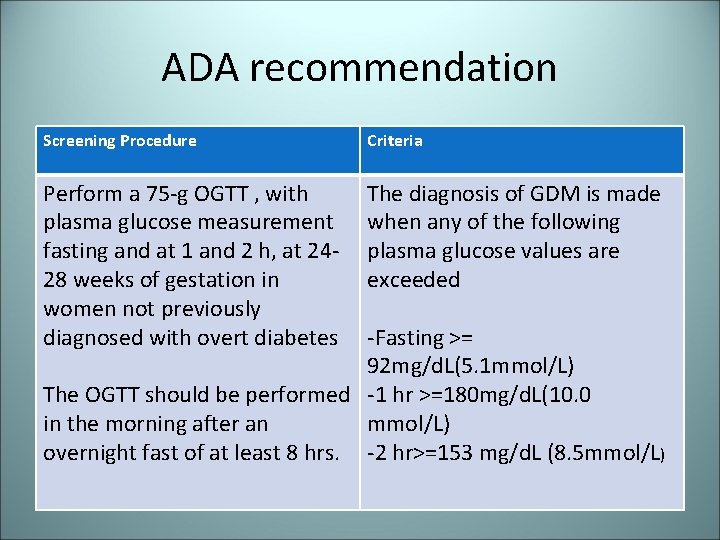

ADA recommendation Screening Procedure Criteria Perform a 75 -g OGTT , with plasma glucose measurement fasting and at 1 and 2 h, at 2428 weeks of gestation in women not previously diagnosed with overt diabetes The diagnosis of GDM is made when any of the following plasma glucose values are exceeded -Fasting >= 92 mg/d. L(5. 1 mmol/L) The OGTT should be performed -1 hr >=180 mg/d. L(10. 0 in the morning after an mmol/L) overnight fast of at least 8 hrs. -2 hr>=153 mg/d. L (8. 5 mmol/L)
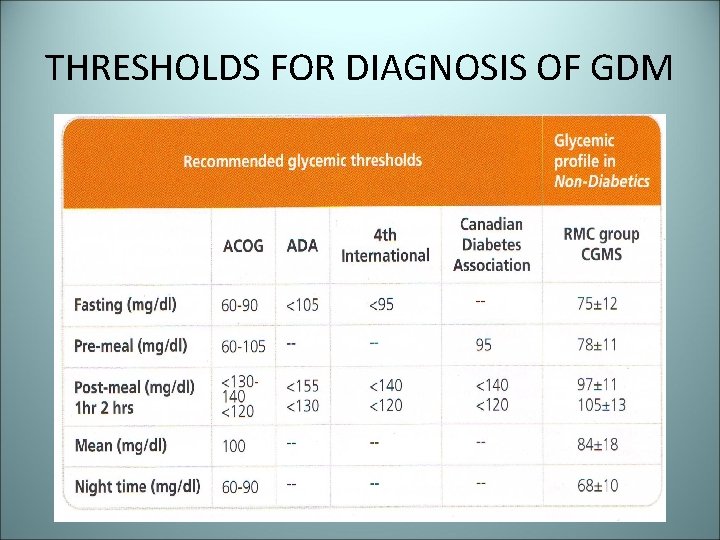
THRESHOLDS FOR DIAGNOSIS OF GDM

GLYCEMIC THRESHOLDS FOR PREVENTION OF DIABETIC COMPLICATION
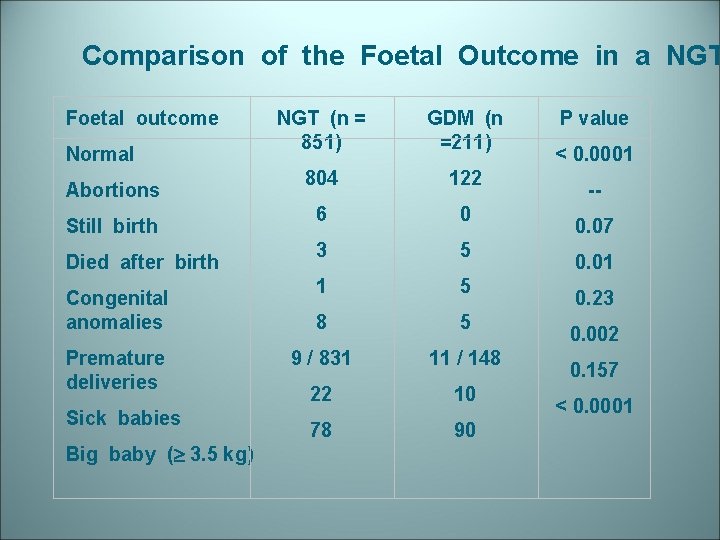
Comparison of the Foetal Outcome in a NGT Foetal outcome Normal Abortions Still birth Died after birth Congenital anomalies Premature deliveries Sick babies Big baby ( 3. 5 kg) NGT (n = 851) GDM (n =211) 804 122 6 0 3 5 1 5 8 5 9 / 831 11 / 148 22 10 78 90 P value < 0. 0001 -0. 07 0. 01 0. 23 0. 002 0. 157 < 0. 0001
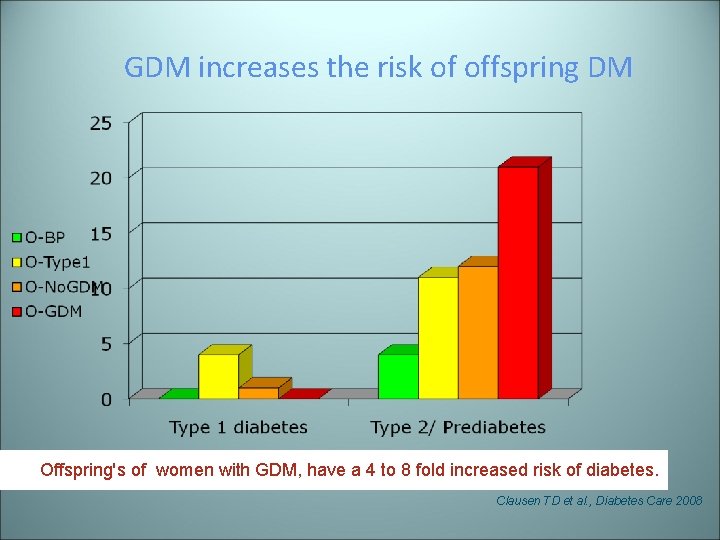
GDM increases the risk of offspring DM Offspring's of women with GDM, have a 4 to 8 fold increased risk of diabetes. Clausen TD et al. , Diabetes Care 2008

How to reduce this • • Early screening for GDM Monitoring frequently Proper uses of diet plan , exercise and insulin. Future concepts of CSII, CGMS, telemedicine, e-health, will revolutionize the management of GDM

How to treat? • • MNT Exercise Insulin Glyburide Metformin Acarbose? Insulin pump

Calorie allotment • 30 kcal per kg current weight per day in pregnant women who are BMI 22 to 25. • 24 kcal per kg current weight per day in overweight pregnant women (BMI 26 to 29). • 12 to 15 kcal per kg current weight per day for severely obese pregnant women (BMI >30). • 40 kcal per kg current weight per day in pregnant women who are less than BMI 22. • Jovanovic-Peterson L, Peterson, CM. Nutritional management of the obese gestational diabetic woman. J Am Coll Nutr 1992; 11: 246.

How long MNT? • Consensus and hard data are lacking regarding how long diet therapy should be maintained before initiating pharmacologic treatment. • 70% of the subjects with initial fasting plasma glucose less than 95 mg/d. L achieved targeted levels of glycemia within 2 weeks of dietary management, but no significant improvement occurred thereafter • Mc. Farland et al obstet gynecol 1999

Exercise Prescription Can continue prepregnancy activity Keeping physically active is essential for good glycemic control Upperbody ergometric exercise useful Do not start new vigorous exercise for glucose control Uterine contractions, fetal tachy, maternal heart rate to be monitored

ORAL AGENTS IN PREGNANCY Glyburide study: ›Randomized trial glyburide vs insulin › 404 GDMs FPG >95 but <140 mg/dl or 2 hr pp >120 on diet ›Similar success of glucose control in both groups Langer et al: NEJM 200: 343: 1134


Animal insulin Insulin Analogues • 1920 - Introduction of insulin revolutionized Diabetes Management • 1920 - Introduced insulin had impurities and batch to batch variation • 1980 - higher quality insulin from bovine and porcine sources. Then came recombinant Insulin

IDEAL AGENT SHOULD FULFILL • Mimic physiological control • No adverse effect upon maternal and fetal outcome. • Should not interfere with antenatal , perinatal and post natal care • Insulin Analogues fulfills all the criteria when given in right doses in right manner.

ADVANTAGES Batch to Batch consistency No allergy, antibody formation No immune mediated lipoatrophy Glucose control is similar in endogenous insulin production • Preprandial hypoglycemia and postprandial hyperglycemia are well controlled. • Mealtime flexibility is possible with analogues. • •

Safety issues with Insulin Analogues • - Ideal insulin Mimic physiological insulin secretion Does not cross placenta No mitogenic potential Since Ig. G bound insulin can cross placenta, therapeutic agent should not induce antibody generation
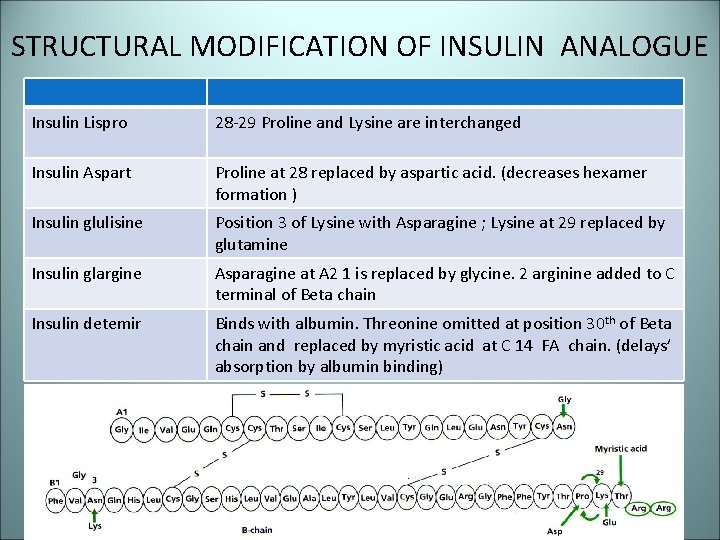
STRUCTURAL MODIFICATION OF INSULIN ANALOGUE Insulin Lispro 28 -29 Proline and Lysine are interchanged Insulin Aspart Proline at 28 replaced by aspartic acid. (decreases hexamer formation ) Insulin glulisine Position 3 of Lysine with Asparagine ; Lysine at 29 replaced by glutamine Insulin glargine Asparagine at A 2 1 is replaced by glycine. 2 arginine added to C terminal of Beta chain Insulin detemir Binds with albumin. Threonine omitted at position 30 th of Beta chain and replaced by myristic acid at C 14 FA chain. (delays’ absorption by albumin binding)
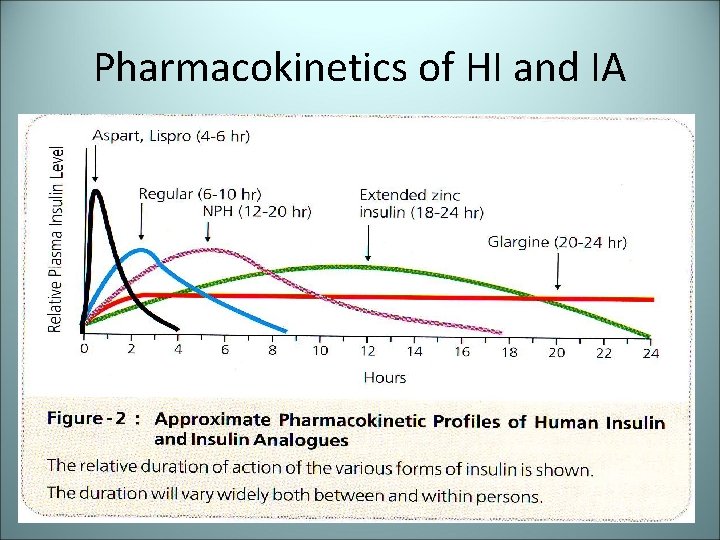
Pharmacokinetics of HI and IA
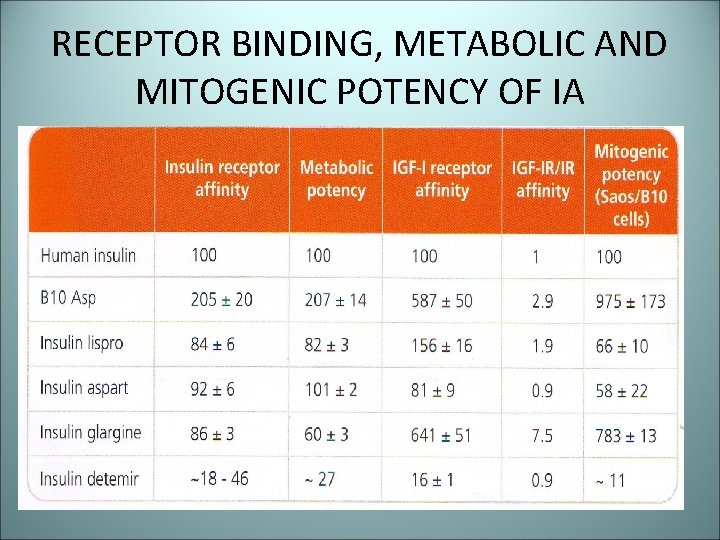
RECEPTOR BINDING, METABOLIC AND MITOGENIC POTENCY OF IA

HAPO: Hyperglycemia And Adverse Pregnancy Outcome • 9 countries, 25 centers, 23, 325 patients • 7 year study • Women were screened between 24 -32 weeks with fasting glucose, 1 hour and 2 hour post 75 gm glucose. • Medical caregivers were blinded to results except that exceeded pre defined cut offs[ 5. 8 fasting, 11. 1 post 75 gm glucose] and were then removed from the study. • Birth weight, maternal complications, operative delivery, insulin levels in newborn were studied. Int J, Gynecology & Obstetrics. 2002, 78, (1); 69 -77


GLYCEMIC STATUS IN GDM FASTING HYPOGLYCEMIA POSTPRANDIAL HYPERGLYCEMIA Normalisation of this is possible by Insulin Analogues.

Insulin aspart qualifies for use in GDM • Insulin analogues does not cross the placenta but placental concentration is higher than in maternal blood.

Insulin Aspart in pregnancy status compared with Human Insulin Moshe Hod et al. , Studied insulin aspart in Type I diabetic patient Randomized parallel group open label Multinational study - Decreased hypoglycemic spells - Increased fetal outcome

Insulin Aspart in pregnancy status compared with Human Insulin Primary objective – Hypoglycemic attacks Secondary objective – Analyze maternal/fetal outcome - Hb. A 1 c - 8 point glucose profile - Number of mild hypoglycemia - cord blood insulin AB





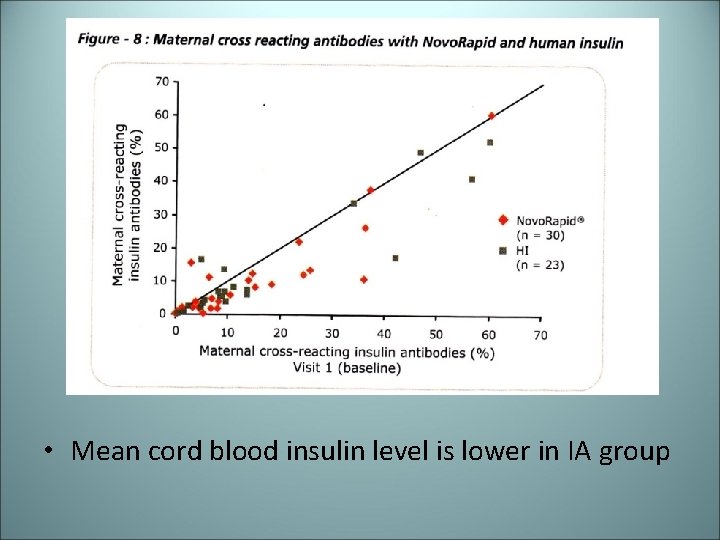
• Mean cord blood insulin level is lower in IA group




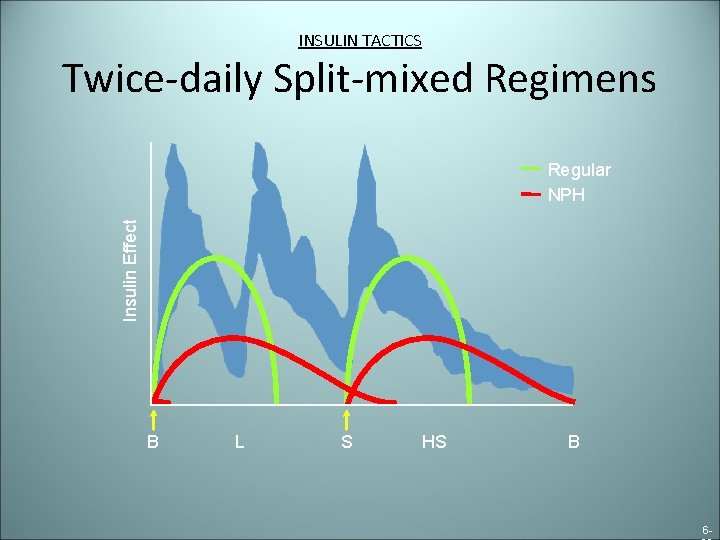
INSULIN TACTICS Twice-daily Split-mixed Regimens Insulin Effect Regular NPH B L S HS B 6 -
C


FUTURE CONCEPTS IN INSULIN THERAPY

Continuous Subcutaneous Insulin Infusion (CSII) • Blood glucose levels monitored continuously • Pre specified insulin dose is subcutaneously delivered by pump • This minimized timing and dosing errors.

Continuous Glucose Monitoring System (CGMS) • Blood glucose is assessed periodically • Insulin dose is calculated • CGMS integrated monitoring system with a delivery device • Hence round the clock blood glucose is controlled.

e-health system • Patient has her data in USB device which can be analyzed and seek guidance from internet.

CSII & CGMS • Paradigm device connects CGMS and delivery device through bluetooth. This early trial is about to be started in USA.


THANK YOU
- Slides: 59