Dermatology in Family Medicine 1 Clerkship Briefing Dr

Dermatology in Family Medicine 1 Clerkship Briefing Dr. Clayton Dyck

Dermatology in Family Medicine 1 (Or, How To Suck Less in Derm) Clerkship Briefing Dr. Clayton Dyck

Objectives 1. 2. 3. 4. Use appropriate terminology to describe common skin presentations seen in family medicine Apply a systematic approach to their diagnosis Know the modalities used in their treatment Understand basic principles of topical therapy

A call from Victoria Beach…

Dermatologic Diagnosis Approach is same as for any other medical condition: n n History Examination Formulate differential diagnosis Apply investigations to confirm/rule out

Dermatologic Diagnosis Use whatever algorithm you like: n n n TTIINNMAP VITTAMIN DD CITTIN VD

Tools Used in Dermatologic Assessment n n n Our ears Our eyes Our hands Our noses (thankfully infrequently!) Lab tests n n n Biopsies Scrapings/clippings Blood and urine samples

Questions to ask n n n Onset Pattern Skin symptoms Systemic symptoms Related factors n n n Environmental Occupational Other medical conditions Drugs Others affected? To name a few…

An overview of terms…

macule
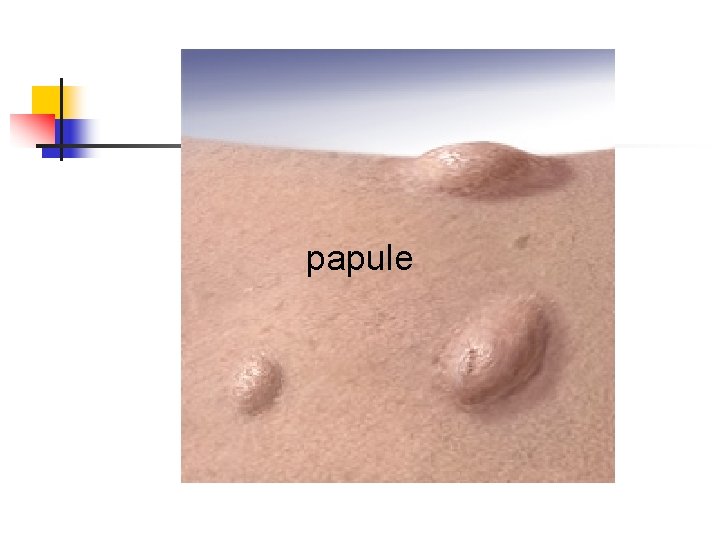
papule
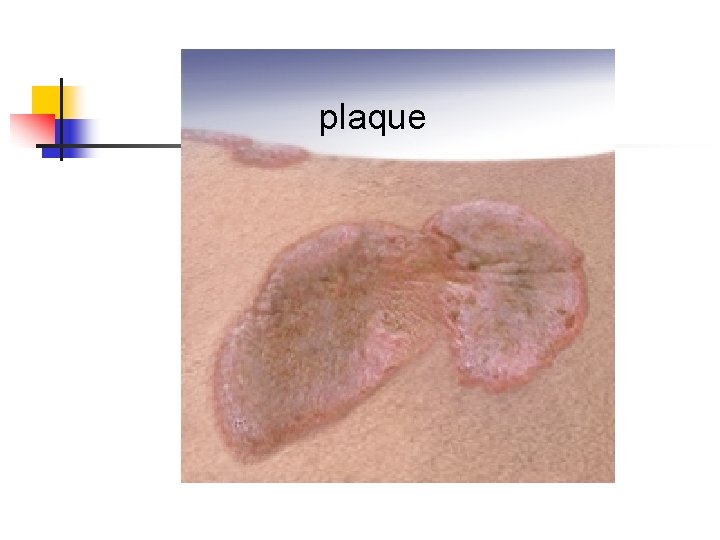
plaque
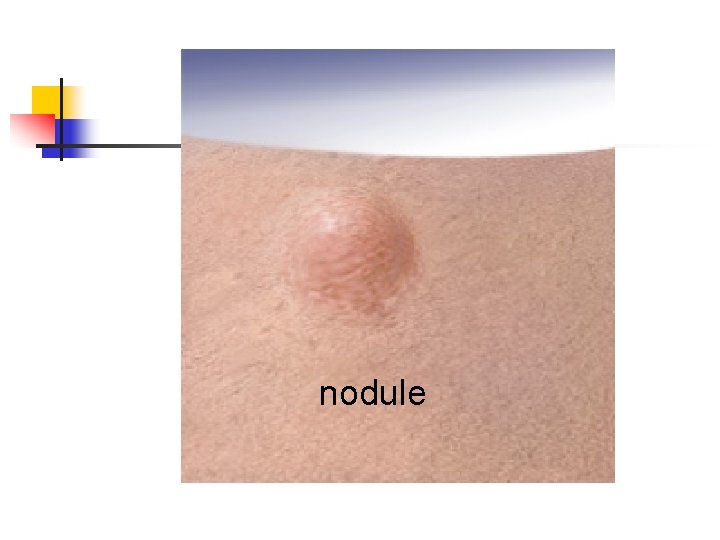
nodule
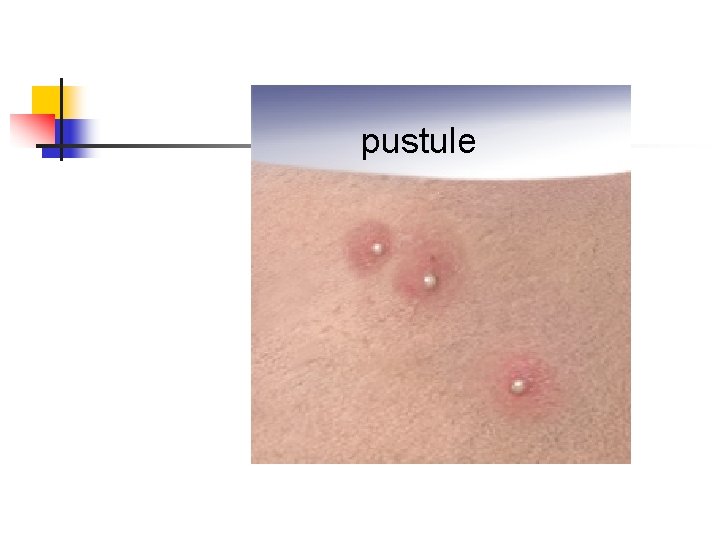
pustule
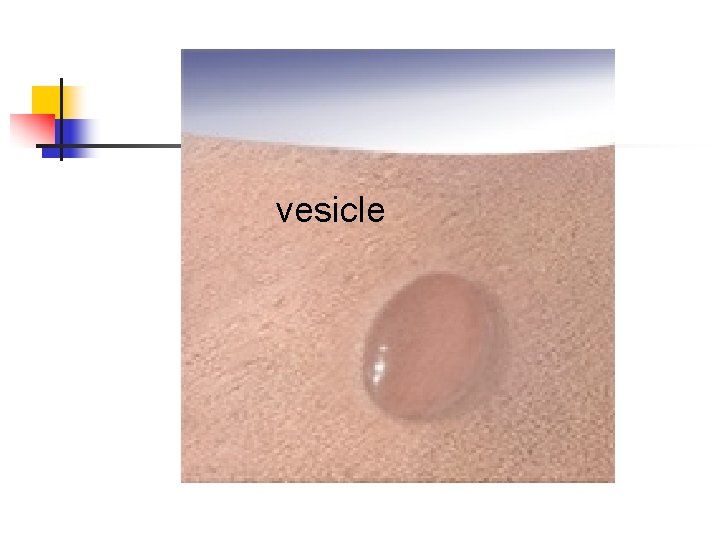
vesicle
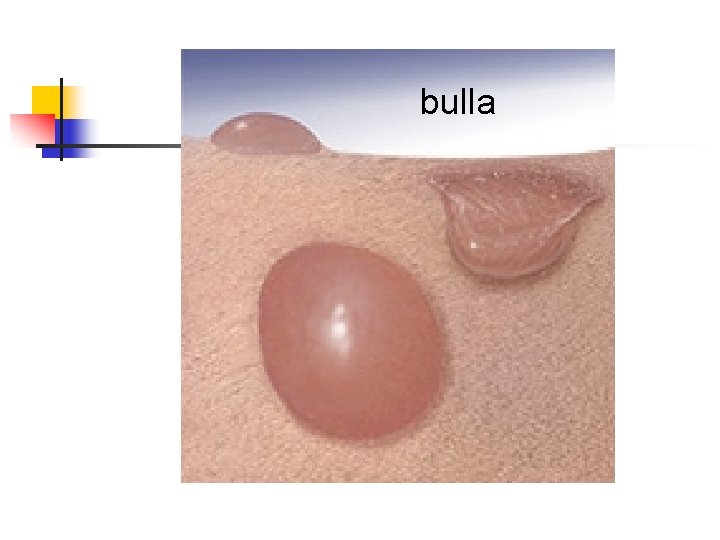
bulla
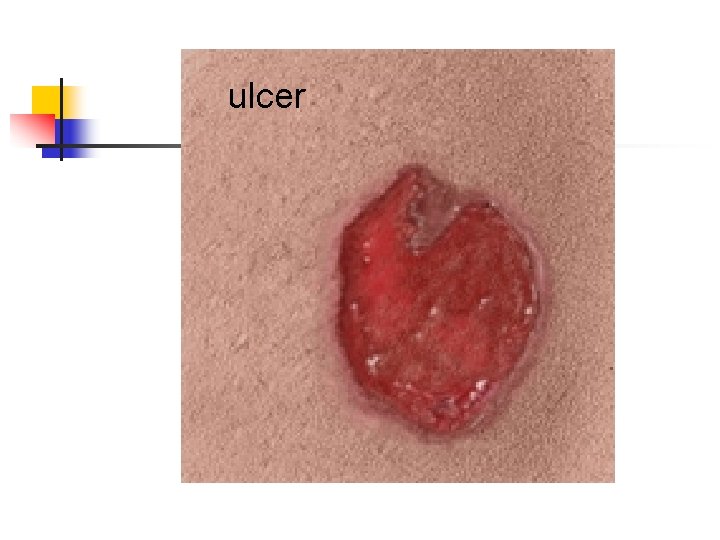
ulcer
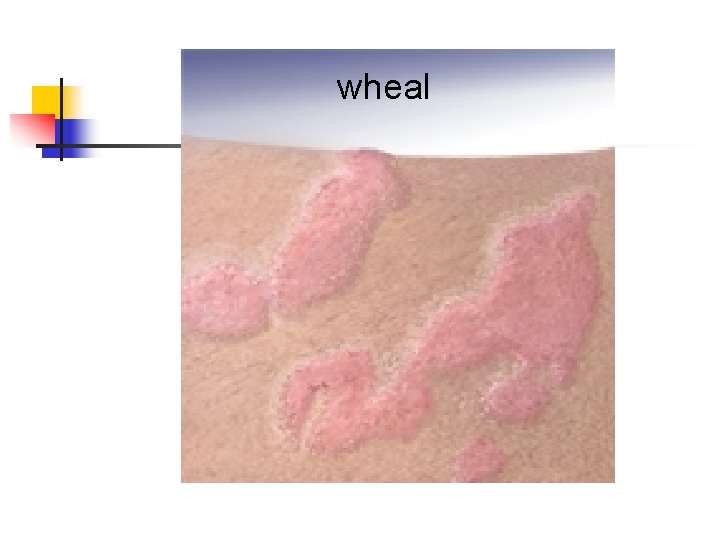
wheal
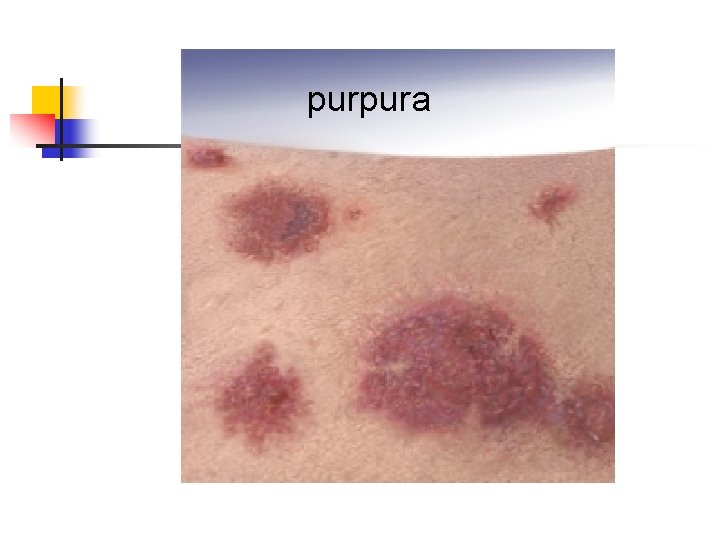
purpura
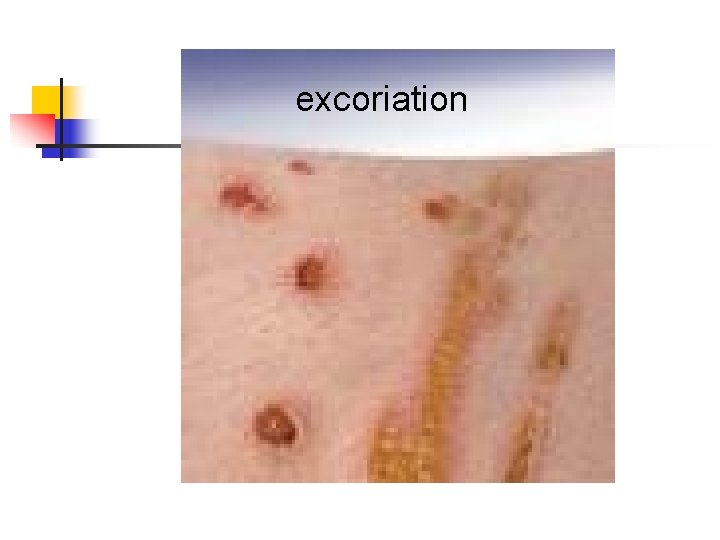
excoriation
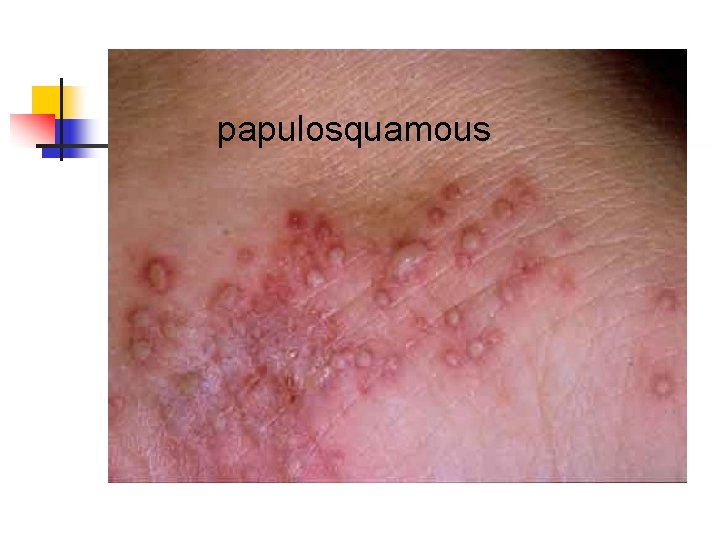
papulosquamous

Some Common Conditions



Herpes Zoster n n n VZV reactivation Pain may precede rash Usually dermatomal Crusts usually fall off in 2 -3 weeks Worse in immunocomprimised, elderly

Herpes Zoster - Treatment n n Wet dressings Antivirals n n n May reduce post herpetic neuralgia Within 48 -72 hours of vesicle appearance Eg famcyclovir 500 mg tid x 7 days

Ophthalmic Zoster - Treatment n n n Hutchinson’s sign Refer to ophthalmologist urgently 50% complications if antivirals not given



Tinea infections n n Dermatophytes, candida Topical antifungals Keep dry! If resistant/severe consider n n n Scraping DM, immunocomprimised PO antifungals


Onychomycosis n n Trichophyton sp. , Candida Do KOH prep, culture first Topical treatment only in simple cases Usually needs oral treatment n n Eg Lamisil 250 mg od x 12 weeks Watch for toxicity


Dyshydrotic Eczema n n Common if hands frequently moist/wet Consider other irritants, allergens, fungi Watch for superinfection Treatment: n n n Moisturize x 3 Topical steroids (usually moderate to high potency) Topical immune modulators



Psoriasis n n Peaks in 20 s and 50 s Multifactorial Exacerbated by trauma, infections, drugs, winter 5 -8% have psoriatic arthritis

Psoriasis - Treatment n n n Topical tar (ick!) High - ultrahigh potency steroids Vitamin D analogues Phototherapy Immunosuppressive agents

Topical Therapy n Choice of vehicle important: n n n n Powder Paste Solutions (water or alcohol based) Gels Lotions Creams Ointments

Topical Therapy n n n Usually only a thin layer needed 1 gram = 10 cm x 10 cm area OD to BID usually sufficient


Topical Steroids n n Consider thickness of skin, thickness of lesion, moistness of area Choose one drug of each potency Consider occlusion with lower potency steroids Avoid extended periods of treatment

Topical Steroids - Examples (by potency) Low Hydrocortisone 1 % Medium Betamethasone 0. 1% High Mometasone Ultrahigh Augmented betamethasone

Topical Steroids - Adverse Fx n n n n Irritation Hypopigmentation Skin breakdown Rebound phenomenon Atrophy Striae Systemic adsorbsion And many more!
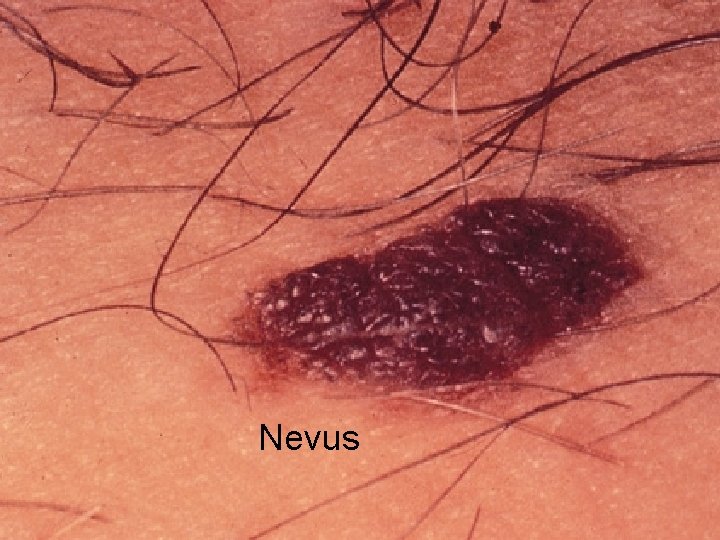
Nevus
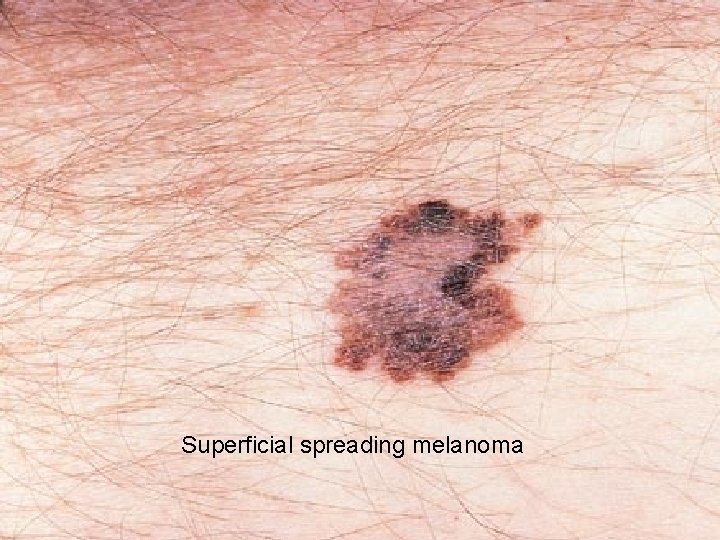
Superficial spreading melanoma
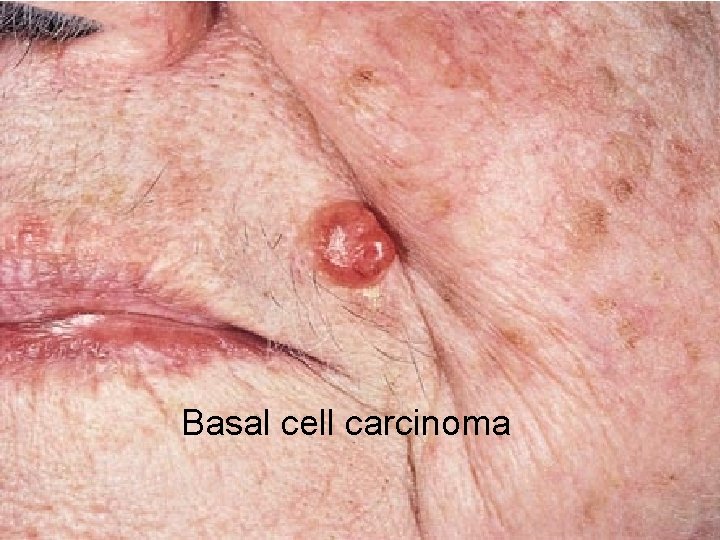
Basal cell carcinoma
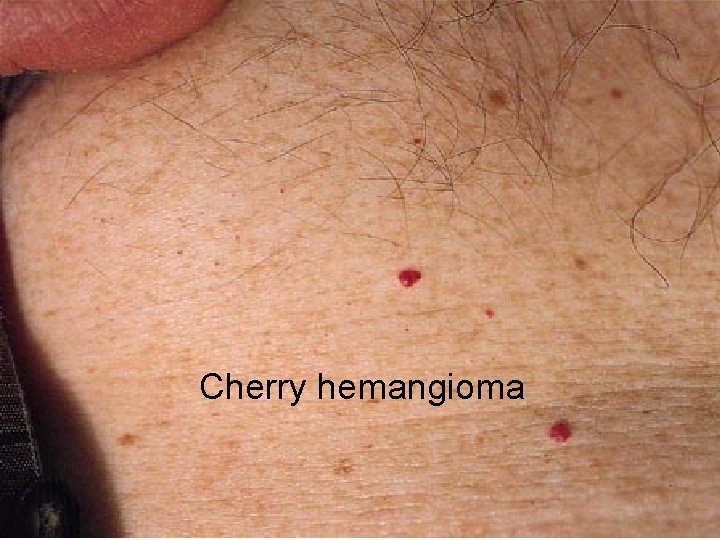
Cherry hemangioma
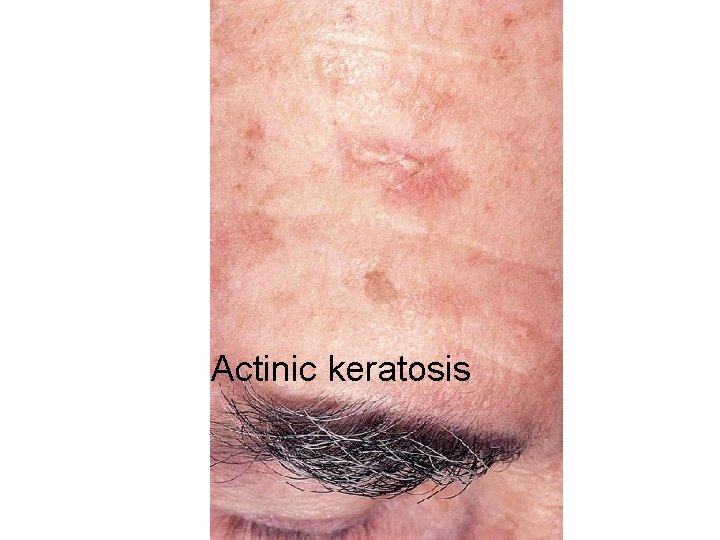
Actinic keratosis

When to biopsy n Change in: n n n Colour Size (<6 mm) Shape Especially if weeks to months, rather than months to years Bleeding Any doubt


Impetigo n n n S. aureus, S. pyogenes, or both Common in schools, daycares Treatment n n Bactroban tid x 10 days Cloxacillin 250 qid x 5 -10 days Keflex 250 qid x 5 -10 days Resistance common, may need swab n Consider Bactroban in nares bid x 5 days


Fifth’s Disease n n n Parvovirus B 19 Peaks in school age children Mild flu-like symptoms Arthritis in 10% Teratogenic, especially before 20 weeks


Erysipelas n n n Group A Streptococci Sudden onset, can be painful Fever, sick Penicillin V po/iv for 2 weeks Macrolide if penicillin allergic



Hand Foot and Mouth Disease n n Coxsackie A 16 virus Mild flu Sx, fever Usually children < 5 years Self limited, resolve within 10 days



Scabies n n n Itchy - worse at night Usually more than one family member A great mimic - consider if: n n n Impetigo Eczema Idonomata

Scabies - Treatment n n n Treat family concurrently Wash all clothes/bedding/towels Permethrin cream n n n Everywhere but hair, mouth, eyes Rinse after 12 hours Infants - precipitated sulfur Consider 2 nd treatment Itchiness persists days to weeks later

Some short snappers
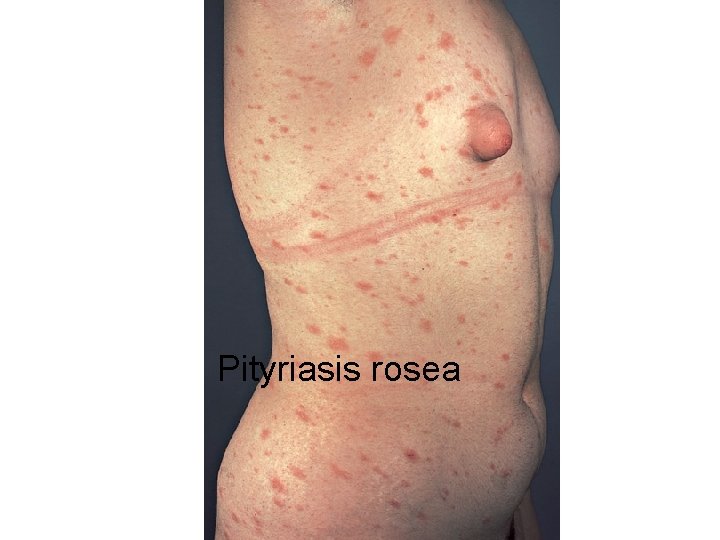
Pityriasis rosea
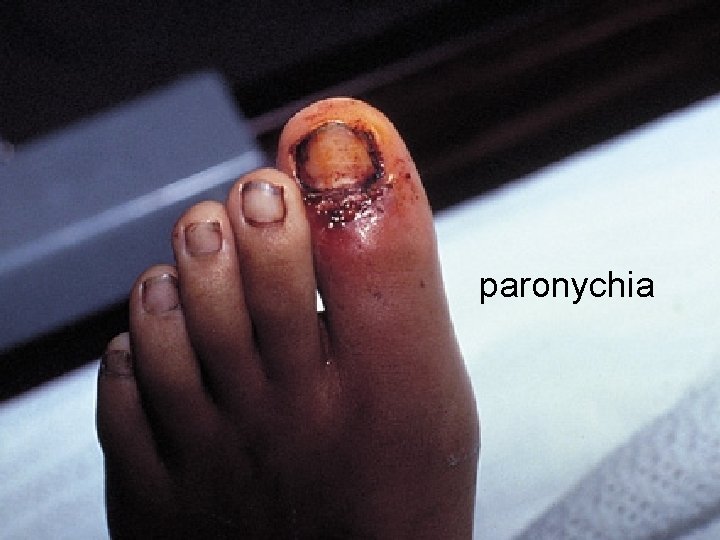
paronychia
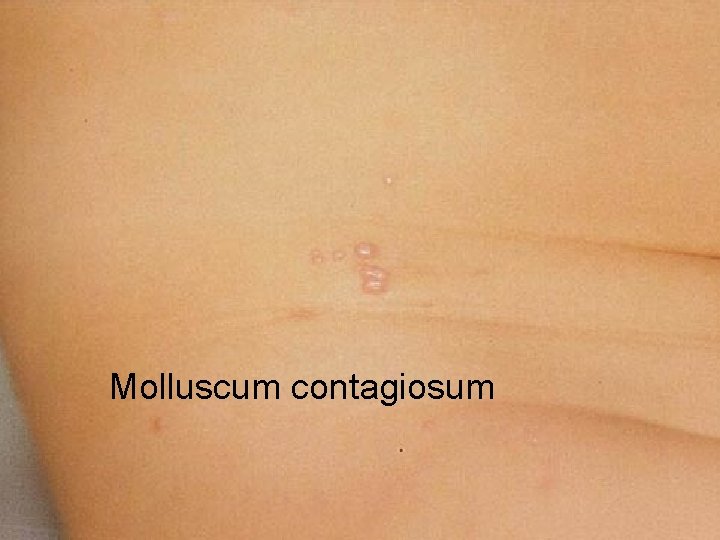
Molluscum contagiosum
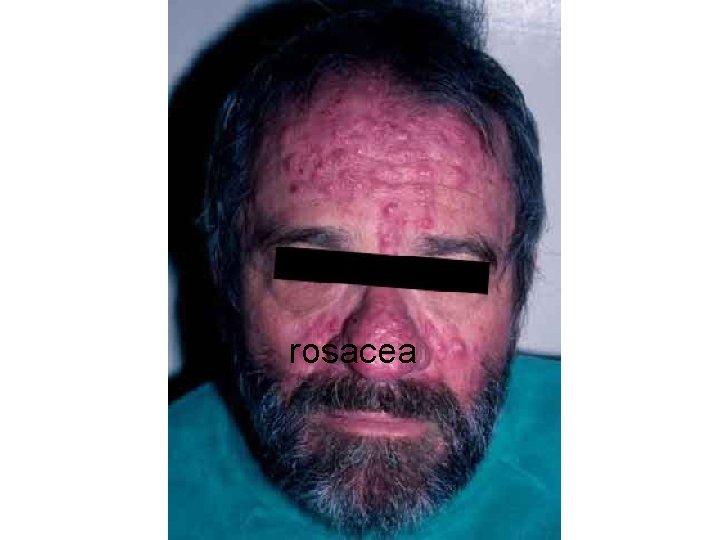
rosacea
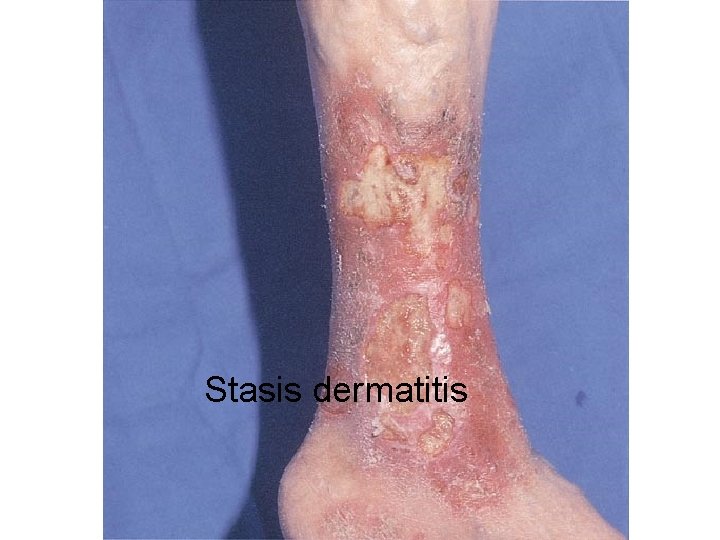
Stasis dermatitis
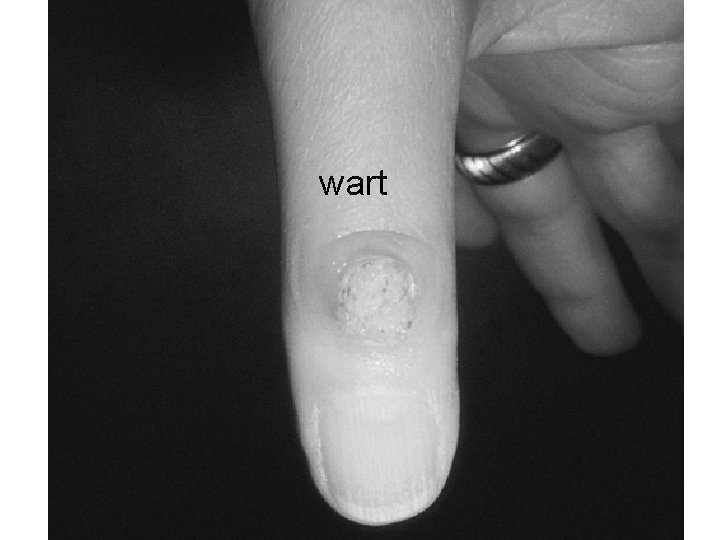
wart
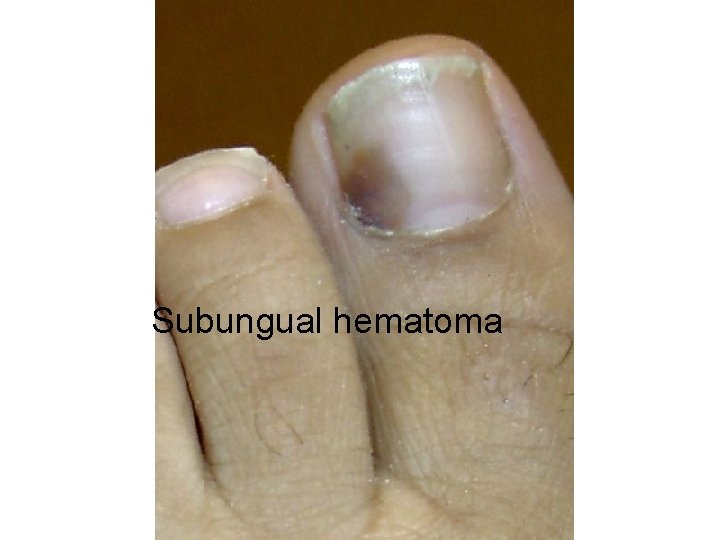
Subungual hematoma

Take home “berries” n n n Know your terminology When in doubt - back to first principles Always keep a differential diagnosis Use the right topical for the job Don’t be afraid to overbiopsy


Objectives 1. 2. 3. 4. Describe common skin presentations seen in family medicine Apply a systematic approach to their diagnosis Know the modalities used in their treatment Understand basic principles of topical therapy

References Skin Diseases: Diagnosis and Treatment, T P Habif et al, Elsevier 2005 Color Atlas and Synopsis of Clinical Dermatology, T B Fitzpatrick, Mc. Graw-Hill, 1997 Images. MD (NJM Library Database) http: //missinglink. ucsf. edu/lm/Dermotology. Gloss ary
Questions? Or itching to leave?
- Slides: 76