Demystifying the Robot The Role of Robotic Surgery

Demystifying the Robot: The Role of Robotic Surgery in Gynecologic Oncology Shazia Bashir MD, MPH Gynecologic Oncologist

Disclosure Ø I have no disclosures

Epidemiology • Most common gynecologic cancer diagnosed in women – Estimated new cases in 2015 – Estimated deaths in 2015 – Lifetime risk 54, 870 10, 170 1 in 37 Siegel et al. Cancer Statistics, 2015. CA Cancer J Clin 2015; 65: 5 -29

Endometrial Cancer

Best Practices • Gynecologic oncologists should be involved in the initial care of every woman diagnosed with endometrial cancer.

Steps in Complete Surgical Staging Peritoneal lavage for cytology Inspection of all peritoneal surfaces Total hysterectomy Bilateral salpingo-oophorectomy Pelvic/para-aortic node sampling Omental biopsy ( unfavorable histology)
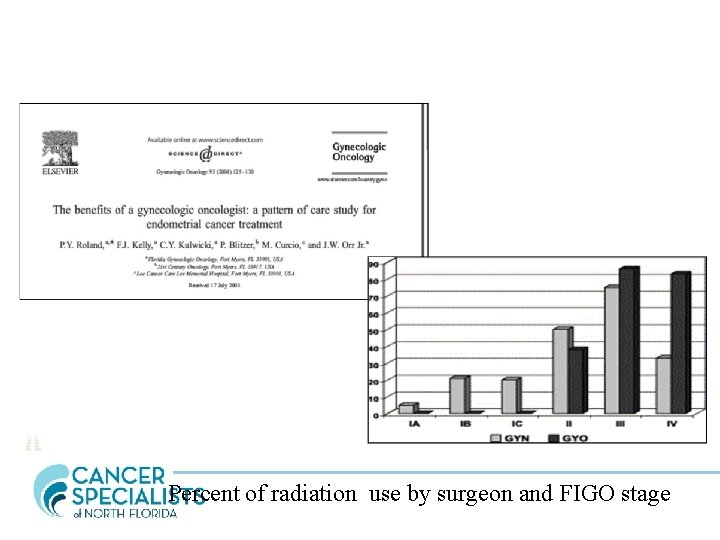
Percent of radiation use by surgeon and FIGO stage
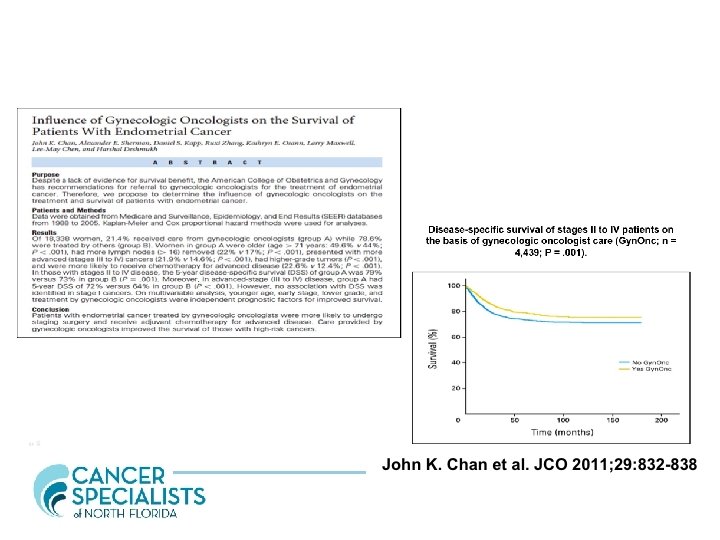
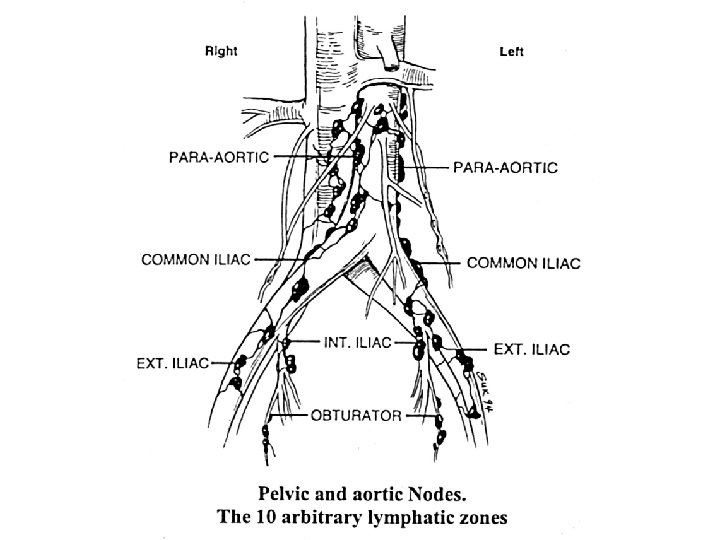

Surgical staging in endometrial cancer. “Clinical estimation of depth of invasion, with or without frozen section, is inaccurate and may lead to underestimation of disease status when surgical staging is not performed. The practice of resecting only clinically suspicious nodes should be discouraged as it is no substitute for comprehensive surgical staging. Comprehensive surgical staging provides proper guidance for postoperative adjuvant therapy, avoiding needless radiation in 85% of clinical stage I/II patients” Kirby TO, Leath CA 3 rd, Kilgore LC. Oncology 2006


What is “Adequate” Staging? n 352 women surgically staged for endometrial cancer n Lymph node count did not impact rate of node positivity n Number of nodal stations sampled was an accurate predictor of node status


What is “Adequate” Staging? • Ability to assess full extent of disease – Chan JK et al. , “Lymphadnectomy in endometrioid uterine cancer staging: how many lymph nodes are enough? A study of 11, 443 patients. ” Cancer 2007 109(12): 2454 -60 • Increasing number of lymph nodes removed associated with higher likelihood of identifying those with lymph node metastases • Largest increase in probability of detection was when 21 -25 lymph nodes were removed. >25 lymph nodes did not significantly improve detection rate

Is Laparoscopic Hysterectomy and staging equivalent to Laparotomy?

Laparoscopy vs. Laparotomy in the Management of Endometrial Cancer • Retrospective review of 510 endometrial cancer patients • Surgical intent TLH in 226 and TAH in 284 • 11 conversions to laparotomy in the TLH group • Median f/u 29 months. No difference in recurrence pattern, DFS or OS between groups Obermair A. et al. Gynecol Oncol 2004

Laparoscopy vs. Laparotomy in the Management of Endometrial Cancer n Prospective, randomized study of 122 endometrial cancer patients n Surgical intent laparoscopy in 63 and laparotomy in 59 n Median f/u 44 months. n 12. 6% recurrence in laparoscopic group vs. 8. 5% with laparotomy (P>. 05) Tozzi et al. J Minim Invasive Gynecol 2005

Laparoscopy vs. Laparotomy in the Management of Endometrial Cancer • DFS 87. 4% vs 91. 6% in laparoscopy vs laparotomy (P>. 05) • OS 82. 7% vs 86. 5% (P>. 05) • Stage I pts: DFS 91. 2% vs 93. 8% (P>. 05) Tozzi et al. J Minim Invasive Gynecol 2005
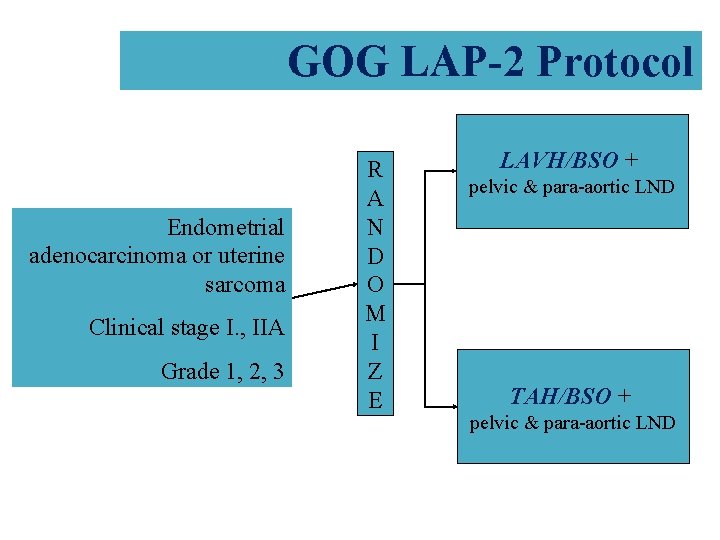
GOG LAP-2 Protocol Endometrial adenocarcinoma or uterine sarcoma Clinical stage I. , IIA Grade 1, 2, 3 R A N D O M I Z E LAVH/BSO + pelvic & para-aortic LND TAH/BSO + pelvic & para-aortic LND

GOG LAP-2 • • N = 2616 enrolled, 2213 evaluable 23. 7% required conversion to laparotomy LOS shorter in scope group (3 v 4 days) Operative time longer in scope group QOL same after 30 days Scope arm less likely to sample PA nodes No difference in stage, node positivity, cytology No difference in progression-free or overall survival
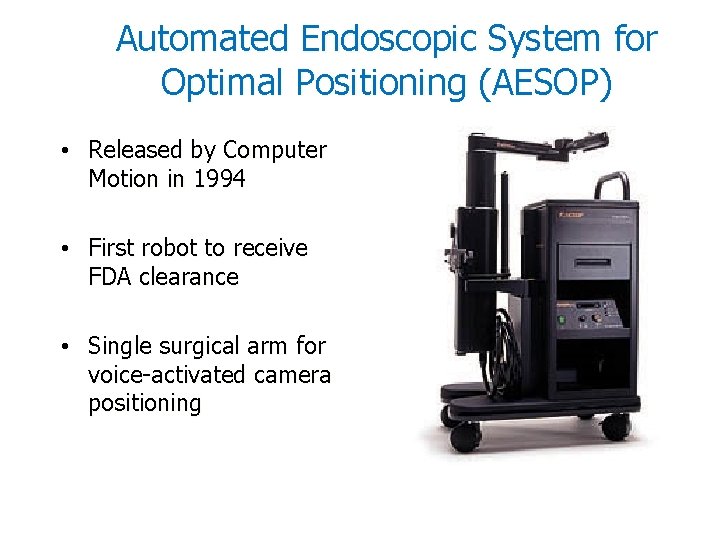
Automated Endoscopic System for Optimal Positioning (AESOP) • Released by Computer Motion in 1994 • First robot to receive FDA clearance • Single surgical arm for voice-activated camera positioning

ZEUS Surgical Robotic System • Released by Computer Motion in 1998 • Uses AESOP technology for camera movement • 2 surgical arms and 2 D optics available on console
Da Vinci Robotic System

Da. Vinci Robot • First approved in 2000 (2005 for gynecological laparoscopic procedures) • 1, 571 systems worldwide • Compared to open: • Minimally invasive • Improved visualization • Reduction of tremors

Appeal of Robotics • Compared to laparoscopic: – 3 -dimensional view – Lack of fulcrum effect – Improved range of motion (7 degrees of freedom) – exceeds natural range of motion – Reduction of tremors – Seated position for the surgeon

Appeal of Robotics

Concern of Robotics • • • Cost Positioning Lack of haptic feedback Setup time Learning curve

Robotic Versus Laparoscopic Staging of Endometrial Cancer • Boggess et al. , 2008 AJOG: open (n=138) vs. lap (n=81) vs. robot (n=103) • Robot-assisted • • Most LN: 32. 9 (vs. 23. 1 lap and 14. 9 open) Shortest LOS: 1. 0 (vs. 1. 2 lap and 4. 4 open) Least EBL: 74. 5 (vs. 145. 8 lap and 266 open) Less complications: 5. 8% (vs. 29. 7% open) • Laparoscopic: longest OR time (213 min, vs. 191 robot and 146 open)

Cost of Robotic Surgery • Barnett et al. , 2010 Obstet Gynecol: decision model – Laparoscopy $10, 128 vs. robot $11, 476 vs. open $12847

Cornell Experience: Robotic versus Laparoscopic Staging in Endometrial Cancer • • • Design: retrospective review Study Group: 118 subjects Assignment: surgeon/patient choice Dates: 5/2006 – 10/2010 Data obtained from: chart review of operative and pathology reports

Methods • Data analysis performed using SPSS® 16. 0 – Pearson c 2, Fisher’s exact tests used for categorical data – Mann-Whitney U test used for comparison of non-normally distributed continuous data (LOS, EBL) – Student’s t-test used for comparison of normally distributed continuous data • Graphs generated using Microsoft Excel®

Results • 118 patients who underwent surgical treatment for endometrial cancer via MIS – 39 laparoscopic/79 robotic assisted • No difference in mean age between laparoscopic and robotic patients (60. 8 vs 60. 9 years) • No difference in BMI between laparoscopic and robotic (28. 3 vs. 29. 6, p=. 38)

Results • Trend towards longer operating time with robotic assistance (204. 3 vs. 226. 9 minutes, p=0. 05) • No difference in EBL (100 m. L vs. 100 m. L, p=0. 633)
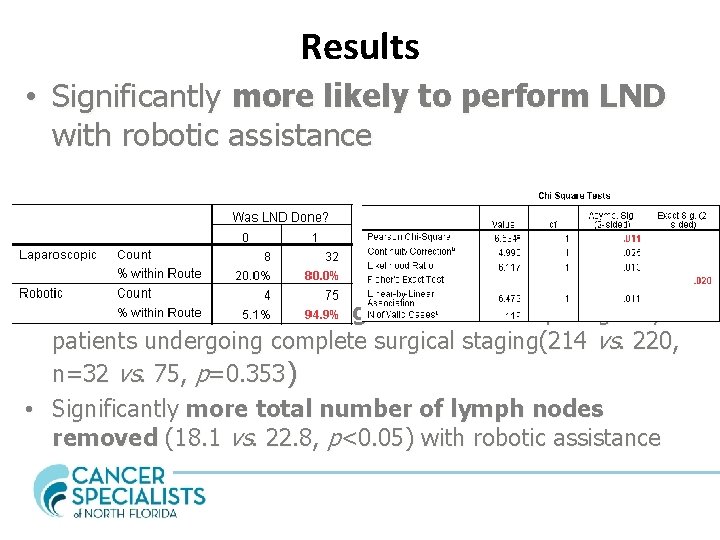

Results • Significantly more likely to perform LND with robotic assistance • No difference in operating time when comparing only patients undergoing complete surgical staging(214 vs. 220, n=32 vs. 75, p=0. 353) • Significantly more total number of lymph nodes removed (18. 1 vs. 22. 8, p<0. 05) with robotic assistance
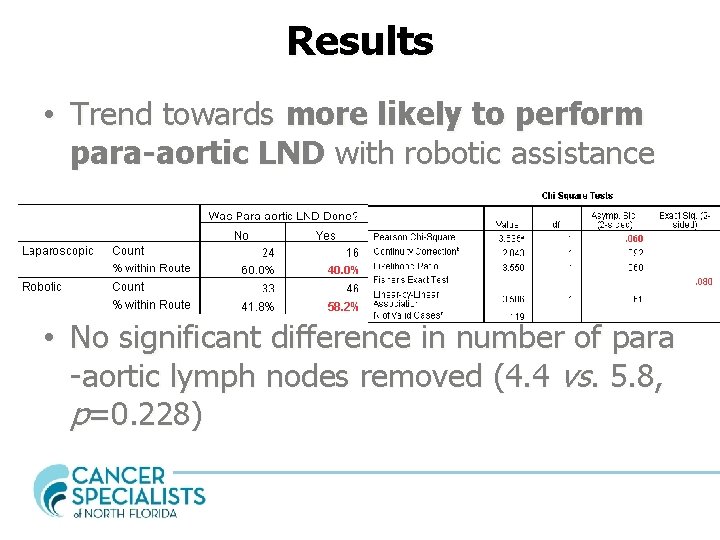
Results • Trend towards more likely to perform para-aortic LND with robotic assistance • No significant difference in number of para -aortic lymph nodes removed (4. 4 vs. 5. 8, p=0. 228)

Results • No significant difference in frequency of complications (2. 5% vs. 6. 3%, p=0. 662) • No difference in length of hospital stay (2 days vs. 2 days, p=0. 986)
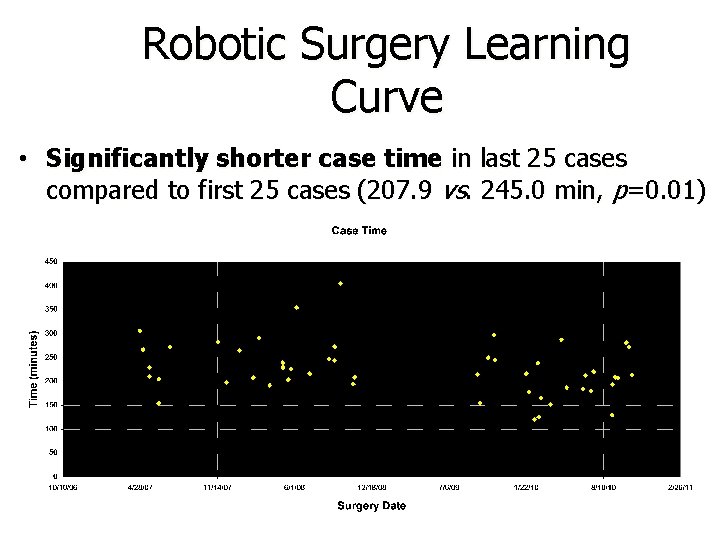
Robotic Surgery Learning Curve • Significantly shorter case time in last 25 cases compared to first 25 cases (207. 9 vs. 245. 0 min, p=0. 01)
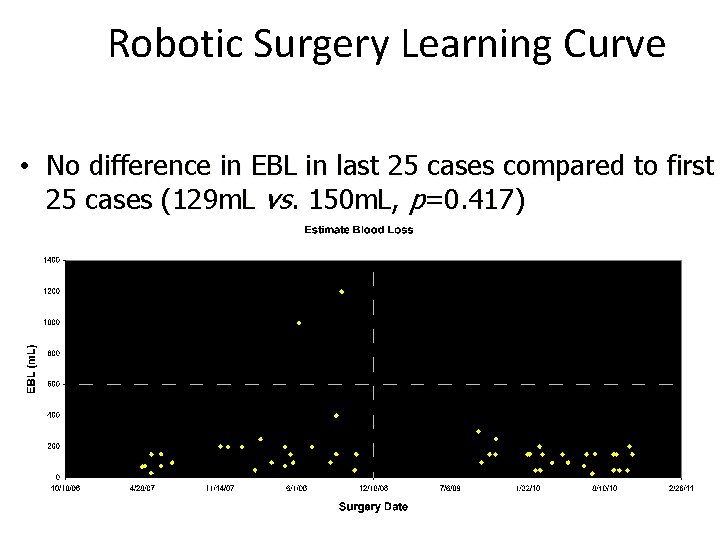
Robotic Surgery Learning Curve • No difference in EBL in last 25 cases compared to first 25 cases (129 m. L vs. 150 m. L, p=0. 417)
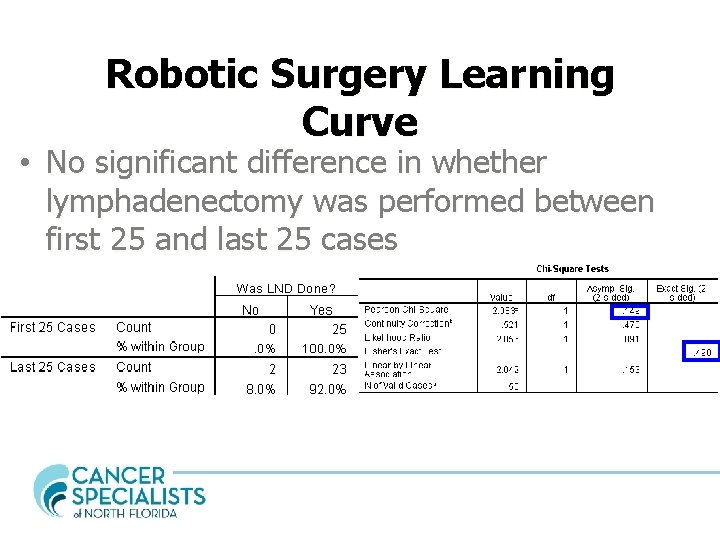

Robotic Surgery Learning Curve • No significant difference in whether lymphadenectomy was performed between first 25 and last 25 cases
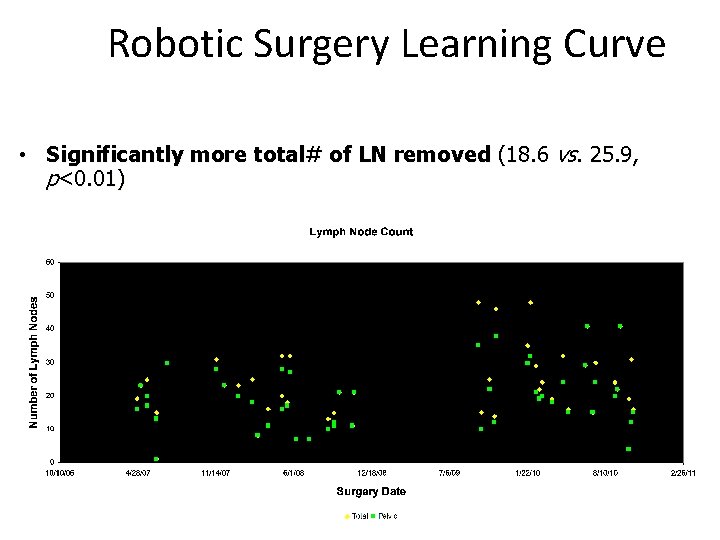
Robotic Surgery Learning Curve • Significantly more total# of LN removed (18. 6 vs. 25. 9, p<0. 01)
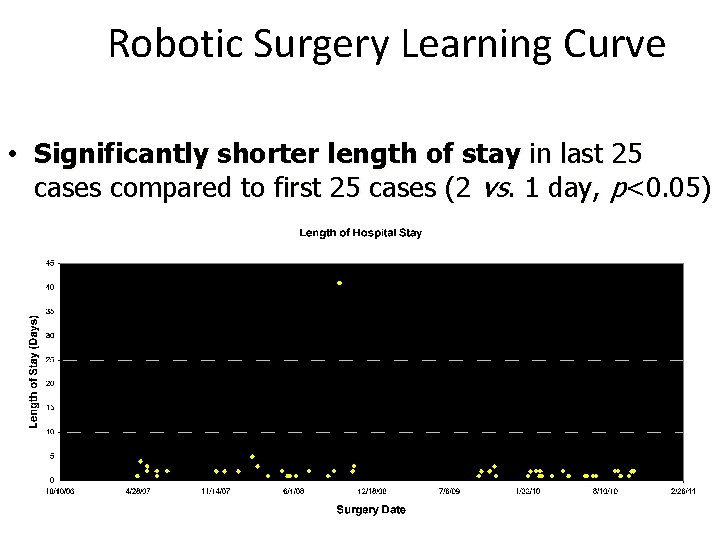
Robotic Surgery Learning Curve • Significantly shorter length of stay in last 25 cases compared to first 25 cases (2 vs. 1 day, p<0. 05)
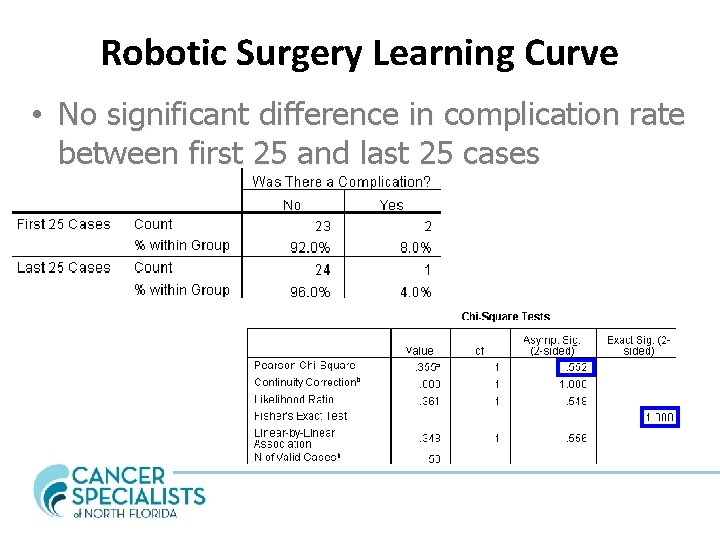
Robotic Surgery Learning Curve • No significant difference in complication rate between first 25 and last 25 cases
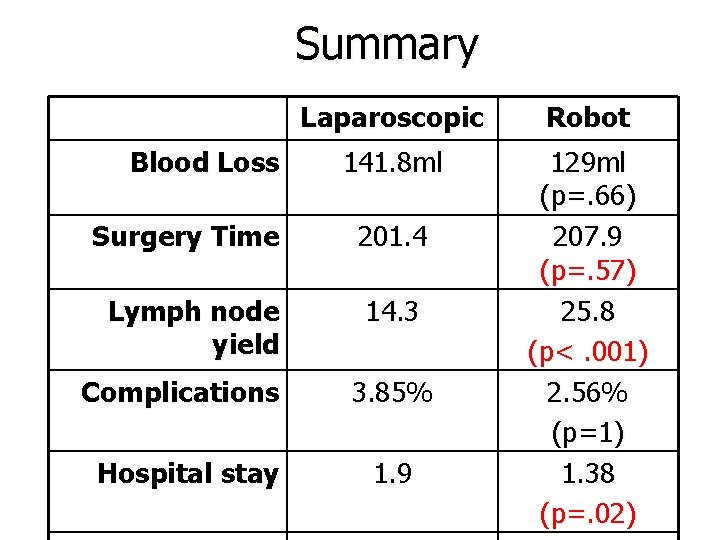
Summary Blood Loss Laparoscopic Robot 141. 8 ml 129 ml (p=. 66) 207. 9 (p=. 57) 25. 8 (p<. 001) 2. 56% (p=1) 1. 38 (p=. 02) Surgery Time 201. 4 Lymph node yield 14. 3 Complications 3. 85% Hospital stay 1. 9

Summary • Robot-assisted laparoscopic staging: more likely to perform pelvic lymphadenectomy, higher lymph node yield. – Trend towards more likely to perform paraaortic lymphadnectomy • No difference in operative time • No difference in EBL or complications • Shorter hospital stay for robotic assisted staging • There is a learning curve associated with roboticassisted laparoscopic staging

Discussion • Strengths • Single surgeon • Weaknesses • Not random assignment • Did not assess long-term follow-up • Did not assess costs
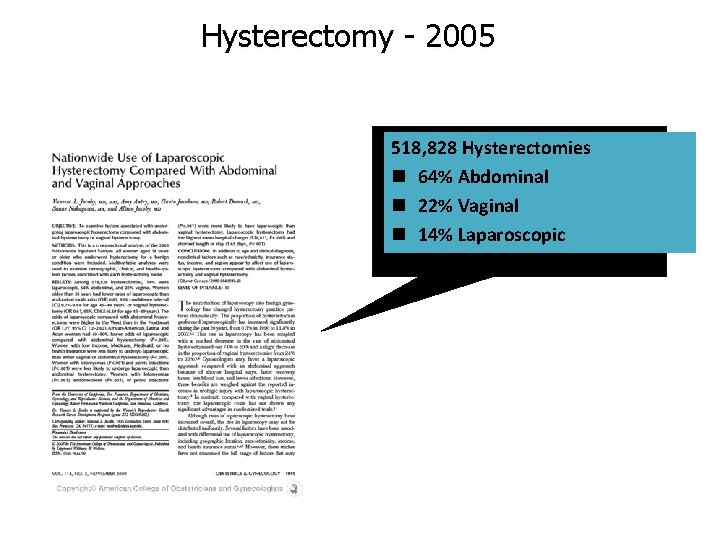
Hysterectomy - 2005 518, 828 Hysterectomies n 64% Abdominal n 22% Vaginal n 14% Laparoscopic
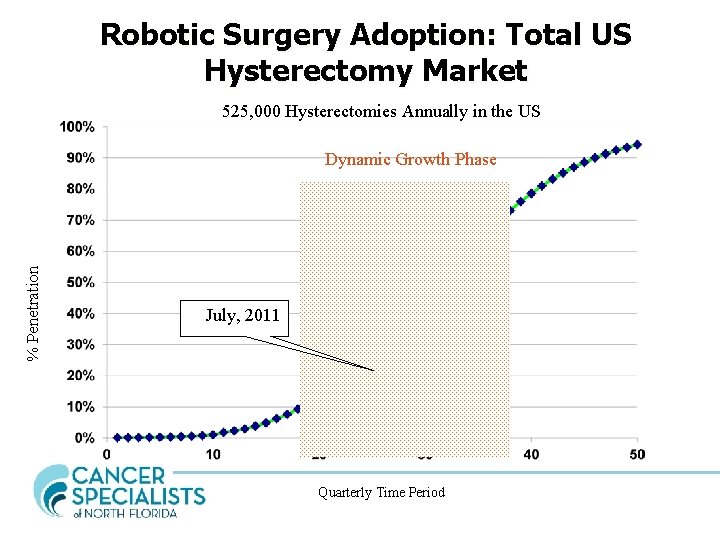
Robotic Surgery Adoption: Total US Hysterectomy Market 525, 000 Hysterectomies Annually in the US % Penetration Dynamic Growth Phase July, 2011 Quarterly Time Period
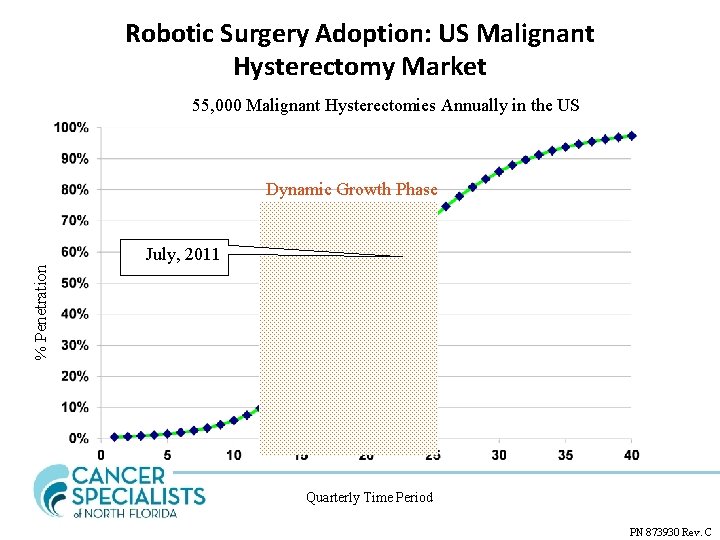
Robotic Surgery Adoption: US Malignant Hysterectomy Market 55, 000 Malignant Hysterectomies Annually in the US Dynamic Growth Phase % Penetration July, 2011 Quarterly Time Period PN 873930 Rev. C

What do you think is the most likely explanation for the increased acceptance of robotic surgery?

1. Faster learning curve compared to traditional laparoscopy 2. Improved patient outcomes compared to traditional laparoscopy 3. Marketing tool to attract patients and increase surgical volume

Acknowledgements Thank you to Kevin Holcomb MD and Billy Burke MD Cornell and Columbia University Questions?
- Slides: 52