DEMENTIA CAPABLE CARE TRANSITIONS BETTER CARE AND BETTER

DEMENTIA CAPABLE CARE TRANSITIONS: BETTER CARE AND BETTER OUTCOMES JANUARY 16, 2018 Stakeholder Planning Summit
Jeffrey B. Klein, FACHE, President & CEO Welcome NEVADA SENIOR SERVICES MISSIO N STRATEG Y NO WRONG DOOR ACCESS Clinical Nevada Senior Services , Inc. CPI Communit y PROGRAMS

Facilitator Mike Splaine, Splaine Associates Conference Agenda MORNING SESSION 10: 20 to 10: 25 Conference Overview 10: 25 to 10: 40 The Need, Jane Gruner, Special Projects, Nevada Senior Services 10: 40 to 10: 50 Q&A 10: 50 to 11: 10 Understanding the Dementia Care Transitions Program, Marissa Shoop, Care Partner Institute, Nevada Senior Services 11: 10 to 11: 30 Target Populations, Jeffrey Klein, President & CEO, Nevada Senior Services
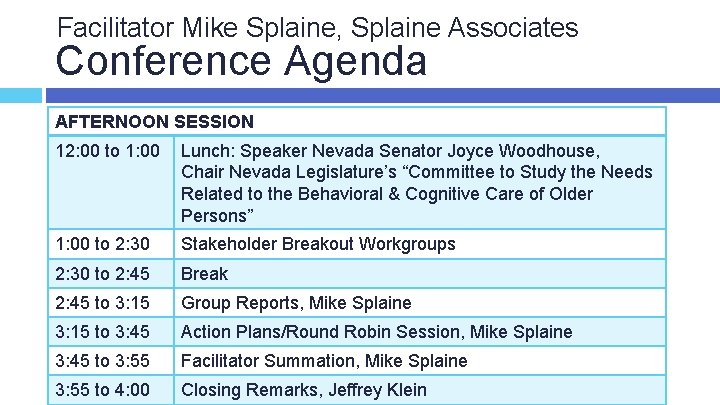
Facilitator Mike Splaine, Splaine Associates Conference Agenda AFTERNOON SESSION 12: 00 to 1: 00 Lunch: Speaker Nevada Senator Joyce Woodhouse, Chair Nevada Legislature’s “Committee to Study the Needs Related to the Behavioral & Cognitive Care of Older Persons” 1: 00 to 2: 30 Stakeholder Breakout Workgroups 2: 30 to 2: 45 Break 2: 45 to 3: 15 Group Reports, Mike Splaine 3: 15 to 3: 45 Action Plans/Round Robin Session, Mike Splaine 3: 45 to 3: 55 Facilitator Summation, Mike Splaine 3: 55 to 4: 00 Closing Remarks, Jeffrey Klein

THE NEED Improving Health Outcomes for Persons with Alzheimer’s Disease and Related Conditions and Their Care Partners Jane Gruner, Special Projects, Nevada Senior Services

Start with big picture… …what we do today creates the system of tomorrow.

Nevada Population 65+

Fastest Population Growth States with fastest population growth in U. S. (2017) 1. 2. 3. 4. 5. 6. Idaho – 2. 2% Nevada – 2. 0% Utah – 1. 9% Washington – 1. 7% Florida – 1. 6% Arizona – 1. 6%
Increase in Adults 65+ Largest increase in adults 65+ (ACL 2005 to 2015) 1. 2. 3. 4. 5. Nevada – 55. 3% Colorado – 53. 8% Georgia – 50. 2% So. Carolina – 48. 9% Arizona – 48%

Dementia

Nevada Population by the Numbers # of people: 2. 9 million # age 65+: approx. 435, 000 # age 65+ with dementia: 43, 000

Nevada Caregivers by the Numbers # of Caregivers: 145, 000 # of hours of unpaid care: 165 million hours of care annually Value of unpaid care: $2 billion

Increases in Diagnoses and Deaths Increase in # of individuals diagnosed with dementia 130% SINCE 2000 Deaths from Alzheimer’s dementia Nationwide increase of 89% from 2000 -2014 Nevada has increased 211%
Nevada Medicaid Cost of caring for people with dementia (2017) $158 million

Clark County by the Numbers

Clark County by the Numbers # of people: 2. 2 million # age 65+: 339, 390 # age 65+ with dementia: 33, 500 # of Caregivers: 113, 000

Service Gaps

Unmet Needs in Nevada Funding Support for family caregivers Health care system Education

Time for Change!

Building Dementia Capability in Southern Nevada Task Force on Alzheimer’s Disease Initiatives focused on building dementia-friendly communities. Development of programs designed to support family care givers. Collection of statewide data related to dementia, caregivers and cost. Seeking grant funding to develop innovative solutions to the needs of NV citizens.

Nevada Senior Services Collaborating with partners to provide innovative service solutions. Adopting dementia capable evidence-based programs. Creation of the Care Partner Institute Designation as the Aging and Disability Resource Center for Southern Nevada.

Nevada Senior Services Geriatric Assessment Center Wellness initiatives Home Modification Program

The Big Idea

Care Transitions Deliver the evidence-based Bridge Transition of Care Model Provided by a licensed social worker Collaboration with hospital to ensure seamless continuum of health and community care across settings. Evidence informed dementia education and innovative practices offered to the individual and care partner.
Post-care Transition Plan Person-centered focused on the values and desires of the individual. Includes internal and external referrals for on-going supports

Short-term Respite Coaching Short-term respite following acute hospitalization Provided by dementia trained respite professionals Assist in managing challenges relate to care transitions

Education and Training Dementia capable education to support hospital staff caring for individual with Alzheimer’s Disease and Related Dementias. Deliver information and best practice education to individuals and their care partners as they transition from hospital to home.

Expected Outcomes

Expected Outcomes Reduced readmission rates Reduced emergency department visits Increased health indicators Decreased caregiver burden Increased caregiver coping Decreased depression Enhanced patient and caregiver activation

Expected Outcomes

Together we make a better Nevada

UNDERSTANDIN G THE DEMENTIA CARE TRANSITIONS PROJECT The Bridge Model, A Rush University Medical Center Product Marissa Shoop, MPA, Care Partner Institute Manager, Nevada Senior Services

Grants Awarded Nevada Aging and Disability Services Division Primary Goal: Improve health outcomes & quality of life for people with dementia. Secondary Goal: Reduce 30 day hospital readmission rates Objective: Implement an evidence based model that can be sustained and replicated throughout Nevada.

Grants Awarded Administration on Community Living Primary Goal: Improving health outcomes & quality of life with individuals living with dementia Objective 1: Deliver evidenced-based care transitions model and post care transitions services within a community based dementia capable framework Objective 2: Offer short-term intensive respite (respite coaching) to care partners for up to 30 days following hospital discharge Objective 3: Provide dementia capable education and training to hospital staff to better service patients with ADRD and their care partners.

Selection of a Model Identified and reviewed possible evidence-based interventions Researched care transitions interventions specific to individuals living with ADRD Community-based model Ability to integrate within a dementia capable system

The Bridge Model Person-centered, social work-led model Emphasizes collaboration Ability to incorporate enhancements of evidence based dementia education tools Integration of dementia specific enhancements approved
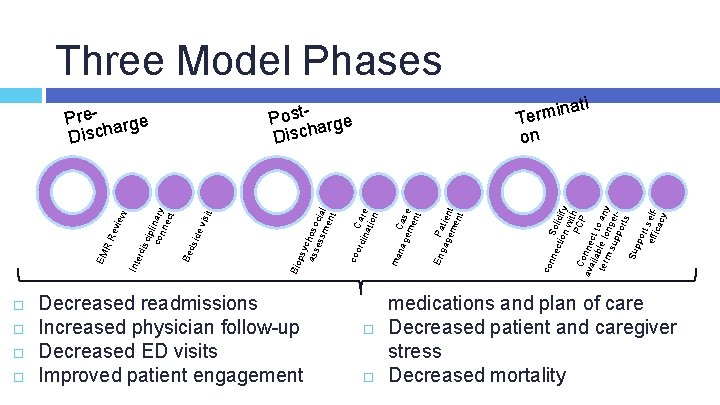
Three Model Phases Decreased readmissions Increased physician follow-up Decreased ED visits Improved patient engagement nec Soli tion dify wi PC th Co P ava nne ilab ct to term le lo any sup nger por ts Su ppo rt effi selfcac y con gag Patie em nt ent En ma nag Cas em e ent rdin Care atio n coo Bio psy ass choso ess cia me l nt vis it de Be dsi cip l con inary nec t rdis w Inte evi e RR EM ati in Term on Post- arge Disch Pre- arge Disch medications and plan of care Decreased patient and caregiver stress Decreased mortality

At-a-glance Delivery: in-person and/or telephonic First contact: 1 to 2 days post-discharge Duration: 30 days

At-a-glance Intensity: 20 -25 telephonic and/or in-person contacts � Patient, caregiver, family members � Medical providers � Community providers � Resources Caseloads: 40 -45 per month per social worker Peak activity: 3 to 5 days post-discharge

Service Population Criteria Defined by grant requirements and stakeholder input Currently Serving individuals with ADRD (diagnosed or selfidentified) of all ages Currently hospitalized for any medical condition Lives at home OR Care Partner and Person with ADRD reside together CP provides +4 hours per week with ADL and IADL Discharge from hospital to home Medicare fee-for-service
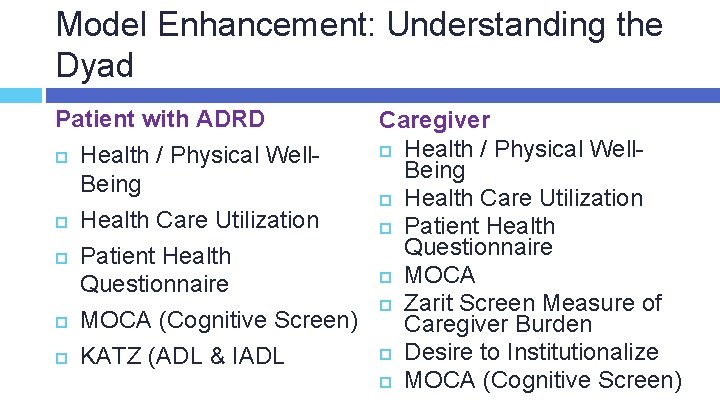
Model Enhancement: Understanding the Dyad Patient with ADRD Caregiver Health / Physical Well. Being Health Care Utilization Patient Health Questionnaire Patient Health MOCA Questionnaire Zarit Screen Measure of MOCA (Cognitive Screen) Caregiver Burden Desire to Institutionalize KATZ (ADL & IADL MOCA (Cognitive Screen)

Model Enhancement: Post Care Transitions Service Delivery 30 -day post assessment Personalized Care Plans � Internal and external information and referrals � Assistance to manager behavioral and psychological symptoms of dementia (BPSD) � Goal: Supporting patient and caregiver to continue to engage in other services for continued support

Model Enhancement: Post Care Transitions Service Delivery Internal Caregiver evidencedbased programs: 1. 2. 3. 4. RCI REACH Skills 2 Care BRI Care Consultation Caring For You, Caring For Me Other supportive programs: 1. 2. 3. 4. Respite Support Groups Home modifications Wellness programs

Model Enhancement: Post Care Transitions Service Delivery External Referrals to community public and private resources Long term supportive resources Basic need programs Caregiver education and support services

Respite Coaching Post hospitalization increases stress and caregiver burden Provides a short-term intensive respite services post hospitalization Dementia trained respite professional Part of Care Transitions Team � � Identify and support the changing needs of individuals with ADRD Assist in reducing caregiver burden

Dementia Education and Training For healthcare partners and caregiver Providing support to hospital staff and caregivers by offering education to address challenges and reduce barriers to care. Sample topics: 1. 2. Communication strategies and techniques Non-pharmacological modalities to decrease and manage behavioral and psychological symptoms of dementia (BPSD) 3. Increasing care partner engagement 4. Care partner support 5. General dementia education

Why Hospitalized as Our Target Population Jeffrey Klein, President & CEO, Nevada Senior Services

The Problem Persons with dementia and their care partners experience challenges receiving dementia capable health care and related communitybased care transitions services, during and after a hospital stay.

The Problem 25% Hospitalized elderly may have a dementia (with or without diagnosis) Hospitalization rate persons with dementia 2 X cognitively healthy ED visits & hospitalizations often triggered by � � � Challenging Behaviors Chronic or Acute Illnesses Falls Admission rate for Urinary Tract infections (UTI) & Pneumonia 80% higher in dementia population
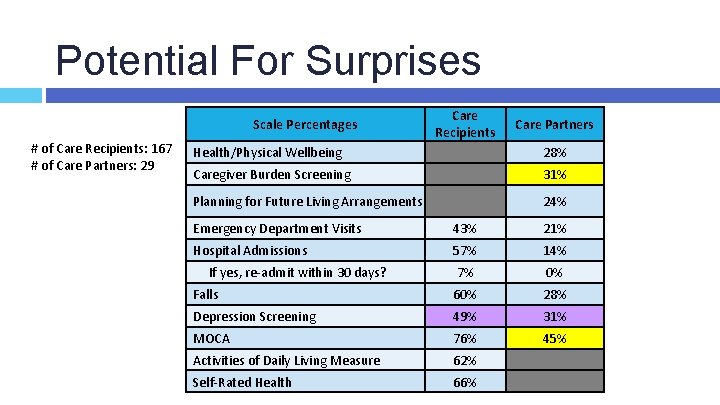

Potential For Surprises Scale Percentages # of Care Recipients: 167 # of Care Partners: 29 Care Recipients Care Partners Health/Physical Wellbeing 28% Caregiver Burden Screening 31% Planning for Future Living Arrangements 24% Emergency Department Visits 43% 21% Hospital Admissions 57% 14% 7% 0% Falls 60% 28% Depression Screening 49% 31% MOCA 76% 45% Activities of Daily Living Measure 62% Self-Rated Health 66% If yes, re-admit within 30 days?

Persons with Cognitive Issues Unreliable reporters of symptoms, medical history May fail to follow instructions

Persons with Cognitive Issues During A Hospital Stay More likely to: Wander Exhibit Agitation/Aggressive Behaviors Need for Physically Restraint Experience Functional Decline Post-Discharge

Dementia Challenges Dementia increases burden on acute care systems Creates excessive resource consumption Higher Complication Rates Poor outcomes increased

Additional Challenges: Target Gap Populations Persons Living Alone With Dementia Persons with Moderate to Severe Dementia Persons Aging with IDD

Persons Living Alone with Dementia May Be: Isolated Unaware of services and resources Lack financial resources Possess limited insight into their changing cognitive capacity

Persons Living Alone with Dementia: May present discharge challenges May present potential unsafe situations Require intensive community supports

Persons with Moderate to Severe Dementia: Higher Percentage of Hospital Stays Increased Co-morbidities � Coronary Artery Disease � Stroke � Diabetes � Cancer Behaviors precipitating Emergency Department visits

Caregivers of Persons with Moderate to Severe Dementia: Experience high stress levels during & after hospitalizations Stress levels intensified by repeated hospital stays

Persons Aging with IDD May experience ADRD onset at earlier age Diagnosis can be difficult, particularly in hospital setting Over 25% live with aging parents who may be in poor health

The Dementia Capable System Mike Splaine, Mike Splaine Associates

Public Policy/Systems Intervention Development & Implementation Intellectual Disabilities and Dementia Overview of Breakout Workgroups 1: 00 – 2: 30 pm Adjacent Ballrooms / Call-ins welcome

Public Policy/Systems Level Work Facilitator: Mike Splaine Chart likely care/support trajectory: hospitalized person with dementia living alone Scenario: person with dementia caring for a person with dementia identified through transitions in care Create decision tree style flow chart to: Call in for Coworkers � Identify stakeholders Local 702 -359 -0270 � System gaps Toll-Free 1 -800 -201� Knowledge gaps 6394 Code 696607

Intervention Implementation Facilitator: Marissa Shoop Discuss implementation strategies Development and implementation timing for same. Managed care organizations Community education : Call in for Coworkers � Delirium � Preventable hospitalizations Local 702 -359 -0270 of Persons with Dementia. Toll-Free 1 -800 -2016394 Code 508219

Intellectual Disabilities and Dementia Facilitator: Kathleen Bishop Introduction to Terms Population Estimates Map Clark County assets targeted to persons with IDD or IDD with dementia Discuss strategies to engage resources, Call in for Coworkers stakeholders, & participants Local 702 -359 -0270 Checklist of key elements for Toll-Free 1 -800 -201 successful work with this subpopulation 6394 Code 236049

Lunch Speaker: Nevada Senator Joyce Woodhouse Chair Nevada Legislature’s “Committee to Study the Needs Related to the Behavioral & Cognitive Care of Older Persons”

Group Reports

Action Plans/Round Robin Session

Planning Committee: Jeffrey Klein Mike Splaine Jane Gruner Marissa Shoop Ellen Grossman Shari Schwartz Thank You for Participating! http: //www. nevadaseniorservices. org/summit. cfm
- Slides: 68