Delivery of Maternal and Newborn Care Services in

Delivery of Maternal and Newborn Care Services in Africa: What are the facilities telling us? Koye Oyerinde MD, MPH, FAAP Symposium on Maternal Mortality, Dakar

The Averting Maternal Death and Disability Program - AMDD • Mailman School of Public Health, Columbia University, New York City. • Help to strengthen heath systems to provide emergency care for all women experiencing life-threatening obstetric complications. • Conduct research and policy analysis, provide technical expertise, and advocate for solutions • Collaborate with global, regional, and local institutions – including NGOs & academic centers

The Alliance • Memorandum of Understanding signed June 2008 between UNICEF, UNFPA, AMDD • Alliance supports country plans for the strengthening of Em. ONC service delivery as a strategy for attaining MDGs 4 and 5. • WHO collaborates on alliance activities at country and regional level.

Needs Assessment Overview • The Em. ONC Needs Assessments are facility based crosssectional studies of the capacity of a health system to provide health services to mothers and newborns • Main focus – health system. ▫ ▫ ▫ Accessibility/Coverage/Equity 24 hour services Human Resources Equipment and Supplies Infrastructure Aspects of quality of care
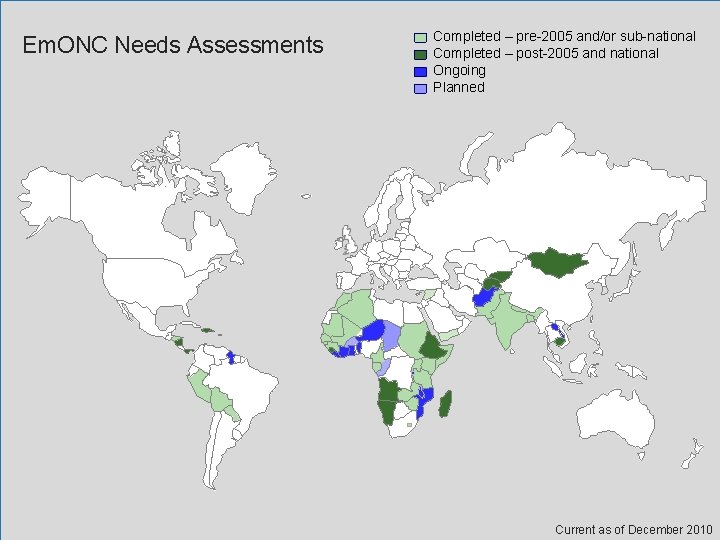
Em. ONC Needs Assessments Completed – pre-2005 and/or sub-national Completed – post-2005 and national Ongoing Planned Current as of December 2010
The Needs Assessment Process The AMDD team: Phase III: From Data to Action • Conducting the Needs Assessment • provides customized technical support and training through these phases Phase II: Conducting the • works remotely and in. Needs Assessment country to support the MOH to conduct the assessments. Phase I: Advocacy and Planning

Some trends from the recent Em. ONC Needs Assessments in Africa
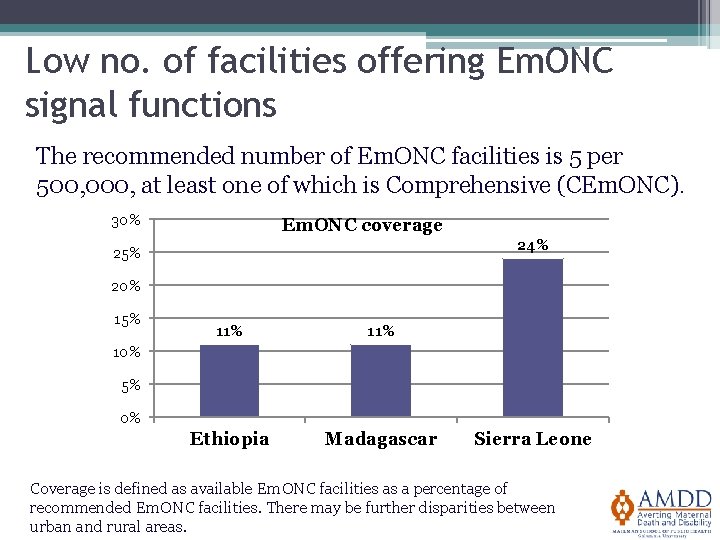
Low no. of facilities offering Em. ONC signal functions The recommended number of Em. ONC facilities is 5 per 500, 000, at least one of which is Comprehensive (CEm. ONC). 30% Em. ONC coverage 24% 25% 20% 15% 11% Ethiopia Madagascar 10% 5% 0% Sierra Leone Coverage is defined as available Em. ONC facilities as a percentage of recommended Em. ONC facilities. There may be further disparities between urban and rural areas.
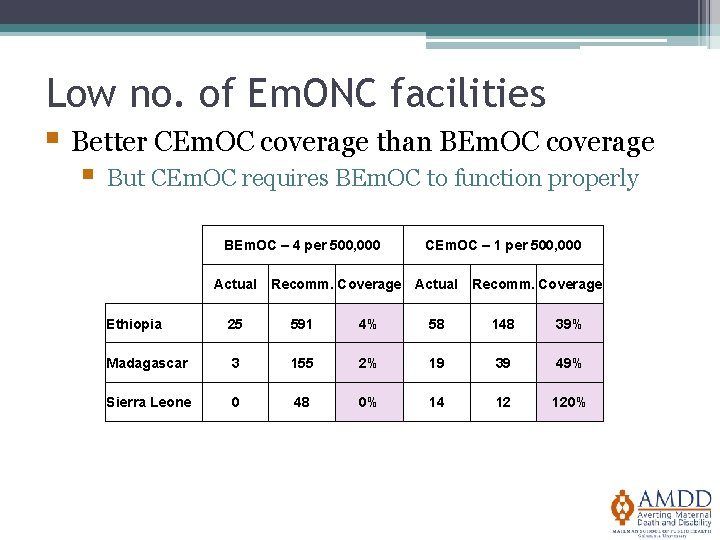

Low no. of Em. ONC facilities § Better CEm. OC coverage than BEm. OC coverage § But CEm. OC requires BEm. OC to function properly BEm. OC – 4 per 500, 000 CEm. OC – 1 per 500, 000 Actual Recomm. Coverage Ethiopia 25 591 4% 58 148 39% Madagascar 3 155 2% 19 39 49% Sierra Leone 0 48 0% 14 12 120%
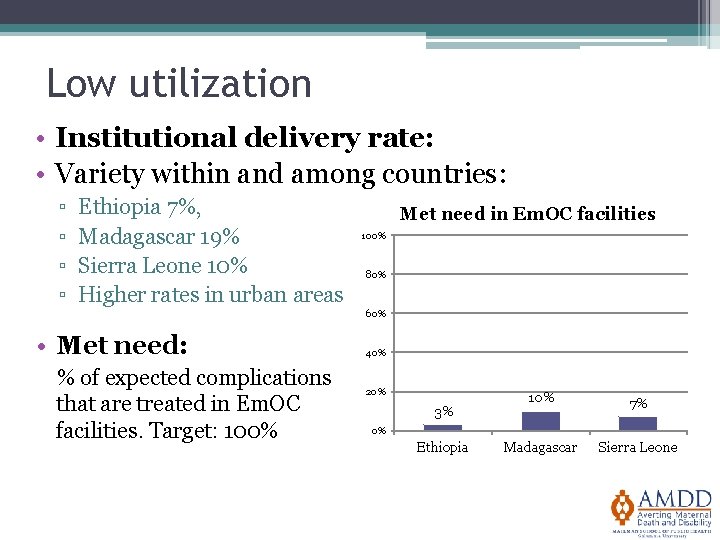
Low utilization • Institutional delivery rate: • Variety within and among countries: ▫ ▫ Ethiopia 7%, Madagascar 19% Sierra Leone 10% Higher rates in urban areas Met need in Em. OC facilities 100% 80% 60% • Met need: % of expected complications that are treated in Em. OC facilities. Target: 100% 40% 20% 3% 10% 7% Madagascar Sierra Leone 0% Ethiopia
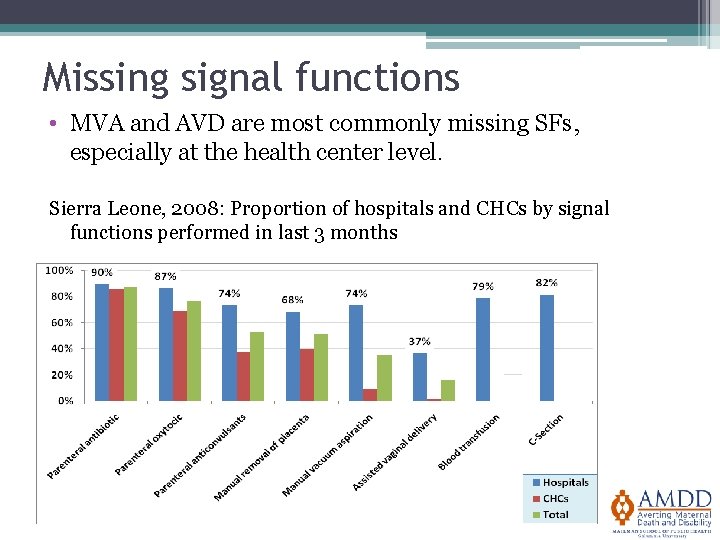
Missing signal functions • MVA and AVD are most commonly missing SFs, especially at the health center level. Sierra Leone, 2008: Proportion of hospitals and CHCs by signal functions performed in last 3 months
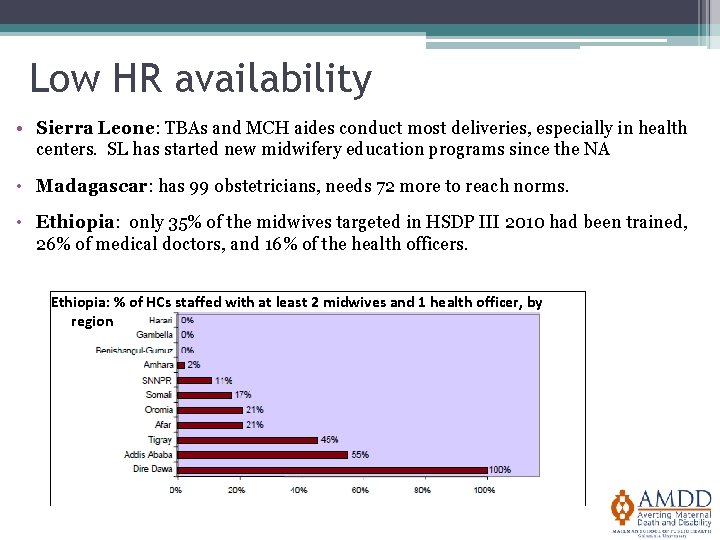
Low HR availability • Sierra Leone: TBAs and MCH aides conduct most deliveries, especially in health centers. SL has started new midwifery education programs since the NA • Madagascar: has 99 obstetricians, needs 72 more to reach norms. • Ethiopia: only 35% of the midwives targeted in HSDP III 2010 had been trained, 26% of medical doctors, and 16% of the health officers. Ethiopia: % of HCs staffed with at least 2 midwives and 1 health officer, by region
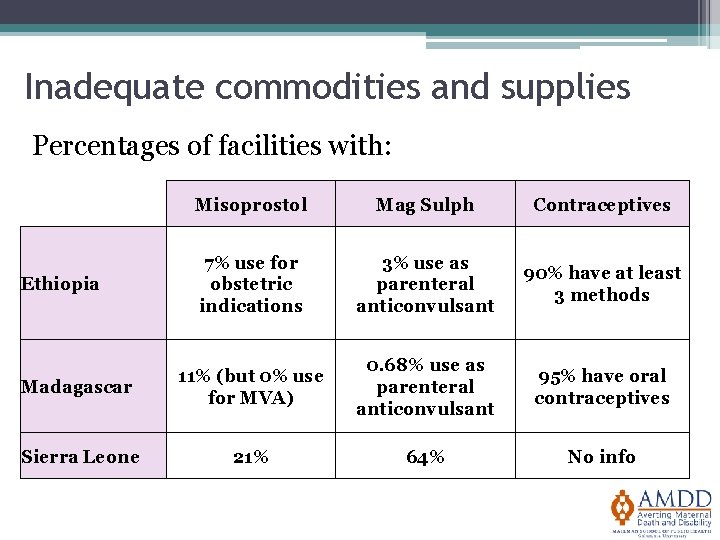

Inadequate commodities and supplies Percentages of facilities with: Misoprostol Mag Sulph Contraceptives 7% use for obstetric indications 3% use as parenteral anticonvulsant 90% have at least 3 methods Madagascar 11% (but 0% use for MVA) 0. 68% use as parenteral anticonvulsant 95% have oral contraceptives Sierra Leone 21% 64% No info Ethiopia
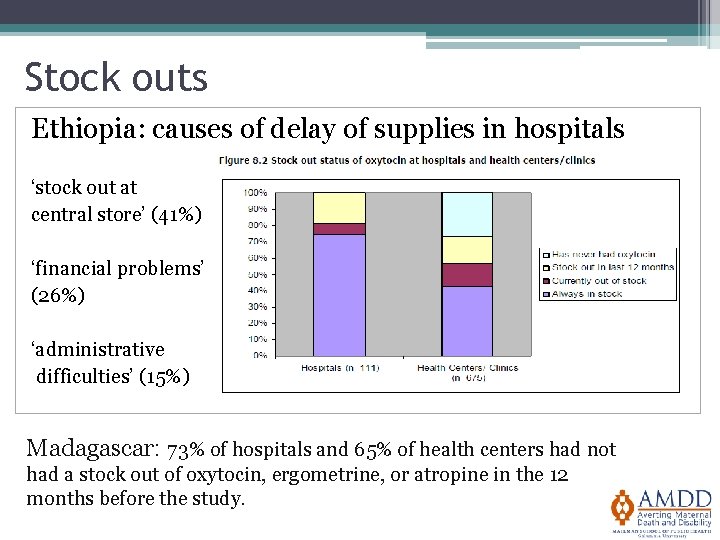
Stock outs Ethiopia: causes of delay of supplies in hospitals ‘stock out at central store’ (41%) ‘financial problems’ (26%) ‘administrative difficulties’ (15%) Madagascar: 73% of hospitals and 65% of health centers had not had a stock out of oxytocin, ergometrine, or atropine in the 12 months before the study.

Limited data collection • HMIS indicators ▫ Often important indicators are not collected ▫ When collected the data are unused for planning ▫ HMIS data often considered unreliable A common outcome of the Needs Assessment is HMIS revision. • Data collection at front-lines ▫ Facility registers often unclear and incomplete ▫ 51% of health centers in Ethiopia had drug and inventory registers

Fee for Service • Fees are often considered a barrier, especially for the poorest. • “Some women when told to go to the hospital would not because they do not have money; so they have problems during delivery” - Sierra Leone Needs Assessment, qualitative data: • Sierra Leone made health services for pregnant and lactating mothers and children under 5 free in spring 2010 ▫ Initial reports suggest a phenomenal increase in utilization; thus raising concerns for potential fall in quality of care

Socio-cultural barriers • NA results are made more meaningful when combined with social science research • Socio-cultural barriers – including abusive / disrespectful care - have been shown to delay utilization and limit benefits derived from the health system
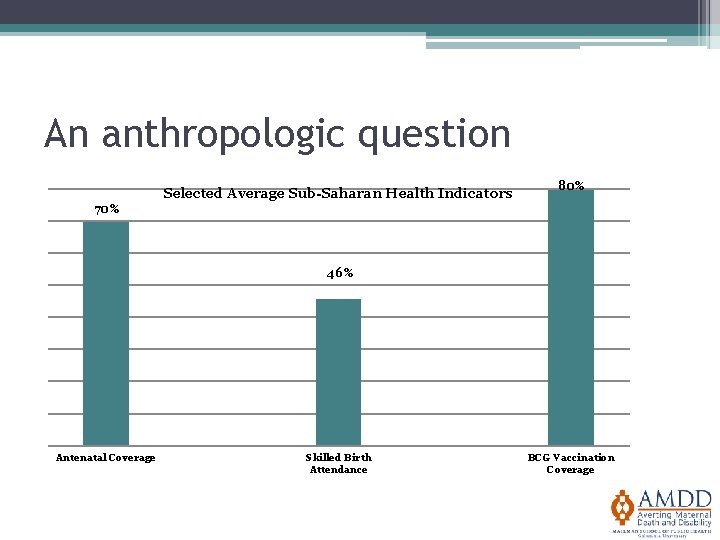
An anthropologic question Selected Average Sub-Saharan Health Indicators 80% 70% 46% Antenatal Coverage Skilled Birth Attendance BCG Vaccination Coverage

Conclusion • Needs Assessments have potential to surface gaps and indicate ways forward • A systems science/health systems perspective is critical – we need strong health systems to support women during labor.

Conclusion • Health facilities in Africa are saying: ▫ Not enough, not the right type and not in the right place ▫ Not adequately staffed, not with the right skills ▫ Not adequately stocked, not with the right tools, drugs, and supplies
Many thanks! Merci beaucoup! Further resources available from the AMDD website: www. amddprogram. org
- Slides: 21