DELIRIUM Treatment 122022 1 Objectives At the end

DELIRIUM: Treatment 1/2/2022 1

Objectives At the end of the presentation, you will be able to: • Implement patient-centered treatment plans • Adjust treatment plan for delirium with underlying dementia 1/2/2022 2

Treatment 1. 2. 3. 4. 5. 6. Prepare environment to promote mobility and orientation 7. Review Events Prior to Admission 8. Review Supportive Care-Delirium Protocol 9. Interventions Promote care with nursing initiated protocols Develop plans for returning to previous level of care Review medical care to promote optimal prescribing for older patients Delirium-what is organic pathology? Review Labs 10. Medication Review– De-prescribe – BEERs – Manage hyperactivity or hypoactivity
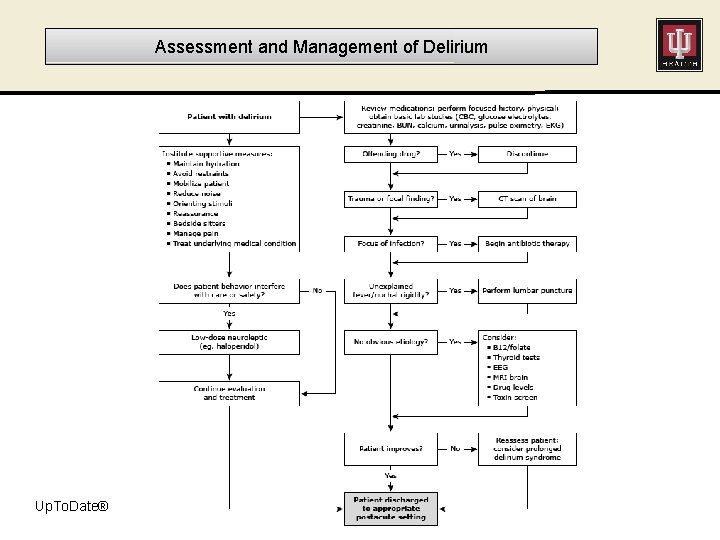
Assessment and Management of Delirium Up. To. Date®

Treatment • NO pharmacological intervention to treat delirium – Look for organic pathways: what is the cause? – De-prescribe: BEERs Criteria – Reduce dosing or hold certain home medications based on presentation: hypo vs. hyper

Trazadone • Insomnia; Other antidepressant • Mechanism of Action-exact unknown; antagonizes serotonin receptors; inhibits serotonin reuptake • Common reaction—somnolence • At a low dose 12. 5 -25 mg this will aid sleep, insomnia with associated agitation is often a symptom of delirium (ideally schedule 5 -6 pm)

Antipsychotic Medications **Use only when non-pharm has failed** Assess for side effects: arrhythmias, EPS, Anticholinergic effects The principle here is to "start low and go slow. " Sometimes will actually have to discontinue the medication at the low dose due to adverse effects and/or paradoxical reaction to medication. Ø Typical Antipsychotic § Halopreidol – Tab, IM inj, IV inj (Black box warning for dementia-related psychosis) Ø Atypical Antipsychotics § Quetiapine (Seroquel) – Tab, suspension (Use with caution, can impact balance, increase risk of falling) § Risperidone (Riperdal) – Tab, ODT, Solution § Olanzapine (Zyprexa) – Tab, ODT, IM inj

Journal of American Geriatrics Society • Systematic Review & Meta-Analysis April 2016 • Suggests antipsychotics do not improve outcomes when used as prevention or treatment

Lorazepam • Sedation, Hypnosis • Amnesia with normal doses • Onset 5 -20 minutes, half-life 8 -15 hrs • Delayed emergence from sedation – Hepatic dysfunction (Exacerbates HE) • Not for use in elderly • Increased risk for development of delirium

Delirium with Underlying Dementia • Most vulnerable population for delirium • Non-pharm interventions • Identify organic pathology • Limit/reduce contributing factors • Hold medication until delirium symptoms improve

Cholinesterase Inhibitors • Donepezil (Aricept) • Rivastigmine (Exelon) • Action: inhibits the acetylcholinesterase enzyme from breaking down acetylcholine – Acetylcholine is a neuromodulator-alters the way brain structures process information – plays a role in arousal, attention and motivation Uses in Alzheimer’s: apathy, cognitive symptoms

NMDA Antagonist • Memantine (Namenda) • Action: Binds N-methyl D-aspartate receptors. – May slow Calcium ion influx and nerve damage

Antidepressants • SSRI (Selective Serotonin Reuptake Inhibitor) • Escitalopram (Lexapro) • Sertraline (Zoloft) • SNRI (Serotonin Norepinephrine Reuptake Inhibitor) • Duloxetine (Cymbalta)

Compassion • This is a person, not a patient • Support the family • Recognize the vulnerability of these people. • Realize they are not responsible for their actions. • Understand that you can make a difference in these people’s lives.

T-A-DA Approach • Tolerate – Tolerate as much as possible-the behavior or agitation • Anticipate – Anticipate what typically agitates the person • Don’t Agitate – If you notice certain things tend to agitate the person, then avoid those things if possible

References 1 of 2 American Psychiatric Association. (1994). The diagnostic and statistical manual of mental disorders, 4 th ed. Washington, DC: American Psychiatric Association. Arend, E. & Christensen, M. (2009). Delirium in the intensive care unit: a review. British Association of Critical Care Nurses, 14(3). Baztan et al (2009) Effectiveness of acute care geriatric units on functional decline, living at home and case fatality among older patients admitted to hospital for acute medical disorders: meta-analysis. Br Med J. 338: b 50. Balas, M. , Vasilevskis, E. , Burke, W. , Boehm, L. , Pun, B. , Olsen, K. , Peitz, G. , & Ely, E. W. (2012). Critical care nurses’ role in implementing the “ABCDE bundle” into practice. Critical Care Nurse, 32, (2), 35 -47. Brown, S. et al (2007). Delirium dichotomy: a review of recent literature. Contemporary Nurse 26(238 -247). Delirium Assessment and Management. (November 2011). Retrieved from http: //www. aacn. org/WD/practice/docs/practicealerts/delirium-practice-alert 2011. pdf Gusmao-Flores D. , Salluh J. I. , Chalhub R. A. , & Quarantini L. C. (2012) The Confusion Assessment Method for the Intensive Care Unit (CAM-ICU) and Intensive Care Delirium Screening Checklist (ICDSC) for the diagnosis of delirium: a systematic review and meta-analysis of clinical studies. Critical Care, Jul 3; 16(4): R 115 Fox MT, et al (2012). Effectiveness of acute geriatric unit care using acute care for elders components: a systematic review and meta-analysis. J Am Geriatrics Society. 60(12): 2237 -45. ICU Delirium and Cognitive Impairment Study Group. (2013). Retrieved from http: //www. mc. vanderbilt. edu/icudelirium/assessment. html Indiana University Center for Aging Research. Anticholinergic Cognitive Burden Scale. Retrieved from http: //americandeliriumsociety. org/ on June 25, 2013. Inouye, S. , Bogardus, S. , Charpentier, P. , Leo-Summers, L. , Acampora, D. , Holford, T. , & Cooney, L. (1999). A multicomponent intervention to prevent delirium in hospitalized older patients. The New England Journal of Medicine, 340, (9), 669 -676. Inouye, S. , Bogardus, S. , Baker, D. , Leo-Summers, L. , Cooney, L. (2000). The hospital elder life program: a model of care to prevent cognitive and functional decline in older hospitalized patients. Journal of American Geriatrics Society, 40, (12), 1697 -1706. 1/2/2022 16

References 2 of 2 Maldonado JR. Pathoetiological model of delirium: a comprehensive understanding of the neurobiology of delirium and an evidence-based approach to prevention and treatment. Crit Care Clin 2008; 24: 789 -856. Milisen, K. et al (2005). Multicomponent intervention strategies for managing delirium in hospitalized older people: systematic review. Journal of Advanced Nursing 52(1), 79 -90. National Institute for Health and Clinical Excellence. (2010). Delirium: diagnosis, prevention, and management. NICE Clinical Guidline 103. London, England. O’Mahoney, R. , Murthy, L. , Akunne, A. , & Young, J. (2011). Synopsis of the national institute of health and clinical excellence guideline for prevention of delirium. Annals of Internal Medicine, 154, (11), 746 -752. The American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. Journal of the American Geriatrics Society 2015 The Confusion Assessment Method (CAM). (2012). Retrieved from http: //consultgerirn. org/uploads/File/trythis/try_this_13. pdf Truman, B. , Ely, E. W. (2003). Monitoring Delirium in Critically Ill Patients, Using the Confusion Assessment Method for the Intensive Care Unit. Critical Care Nurse, 23(2), 25 -35. Tullman, D. , Fletcher, K. , & Foreman, M. (2012). Delirium. In Boltz, M. , Capezuti, E. , Fulmer, T. , & Zwicker, D. (Eds. ) Evidence-based geriatric nursing protocols for best practice (4 th Ed), (pp. 186 -228). New York, NY: Springer Publishing Wei, L. A. , Fearing, M. A. , Sternberg, E. J. , Inouye, S. K. (2008). The Confusion Assessment Method (CAM): A Systematic Review of Current Usage. Journal of the American Geriatrics Society, 56(5). 823 -830. Wei, L. et al (2008). The confusion assessment method: a systematic review of current usage. Journal of American Geriatric Society, 56: 823 -830. Wong RY et al (2006). Discharge outcomes of older medical inpatients in a specialized acute care for elders unit compared with non-specialized units. Can J Geriatrics. 9(3): 96 -101. Wong RY et al (2008). Adverse outcomes following hospitalization in acutely ill older patients. BMC Geriatrics. 8: 10. 1/2/2022 17
- Slides: 17