Delirium The Confusion Conundrum February 4 2011 Mitchell

Delirium: The Confusion Conundrum February 4, 2011 Mitchell T. Heflin, MD Barbara Kamholz MD Juliessa Pavon, MD Yvette West, RN, MSN, CNS Duke GEC www. interprofessionalgeriatrics. duke. edu

Case Presentation Mr. A – 82 year old white male post-op day #18 from AAA repair – Consult for agitation and altered mental status HPI: – Pulsatile mass found by PCP on routine exam – Confirmed as 8. 2 cm infrarenal AAA on CT – Referred for elective surgical repair Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: History • Past Medical History: – Hypertension – Hyperlipidemia – Smoked 1 ppd until quit 1995 – s/p finger amputation on left hand from work accident • Home Medications: – Simvastatin 40 mg daily – Bisoprolol 5 mg bid – ASA 81 mg daily • ROS: – Denied abd pain, back pain, chest pain, sob, claudication Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: History • Family History: – Alzheimer’s disease in both parents • Social History: – – Lives at home alone, widower for 5 years Independent in ADLs and IADLs Physically active, playing golf daily Son and daughter do not live locally Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: Hospital Course • Elective AAA repair on 12/15/10 • POD #0 returned to OR for bleeding from aneurysm • Following surgery: – Mental status did not return to baseline despite weaning off sedation – Failed trial of extubation due to AMS • POD #3: atrial fibrillation and tachycardia – Amiodarone started • POD #7: Trach and PEG Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: Hospital Course • POD #7 -14: Restless and agitated – Pulling at trach and PEG – Attempts to treat with haldol, risperidone and ativan • POD # 16: Adynamic ileus and aspiration – Vancomycin and ciprofloxacin • POD # 18: Geriatrics consulted – Assist with management of agitation and altered mental status Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: Medications • • • Aspirin Amiodarone Metoprolol Vancomycin Ciprofloxacin Ativan 1 mg IV q 6 hrs Risperidone 0. 5 mg VT qhs Haldol 0. 5 – 1. 5 mg IV PRN (5 mg in last 24 hrs) Dilaudid 0. 5 mg IV q 6 hrs PRN (0 mg in last 24 hrs) Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: Exam T 36. 4 HR 100 s BP 90 s/60 s Pulse ox 97% on 40 % Fi. O 2 • Ext: Restraints on hands, edema in LE • Gen: – Somnolent but easily arousable and anxious – Grimacing and tachypneic – Trach in place on ventilation • Neuro: – Opens eyes to loud voice and tracks but does not follow simple commands – moves all extremities – no Babinski or clonus Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: Diagnostic Testing • • Head CT: No focal lesions CXR: Small bilateral effusions KUB: Mildly distended loops of small bowel WBC 12 K, Hct 28% Creatinine 1. 0, Albumin 2. 3, LFT’s and TSH normal UA: + hematuria EKG: Afib 100, Cardiac enzymes: normal Duke GEC www. interprofessionalgeriatrics. duke. edu

Case: Daughter’s input • Very physically and socially active • Had problems with forgetfulness, repeating and perseverations in the prior year • Very hard of hearing and wears glasses for distance vision • Drank at least two-three glasses of wine each week Duke GEC www. interprofessionalgeriatrics. duke. edu

Delirium: Definitions • Acute disorder of attention and global cognitive function • DSM IV: – Acute and fluctuating – Change in consciousness and cognition – Evidence of causation • Synonyms: organic brain syndrome, acute confusional state • Not dementia Duke GEC www. interprofessionalgeriatrics. duke. edu

So what’s the conundrum? • Highly prevalent • Associated with much suffering and poor outcomes • Complex and often multifactorial • Preventable but…. Better care requires a shift in paradigm Duke GEC www. interprofessionalgeriatrics. duke. edu

Objectives • Describe the prevalence of delirium and its impact on the health of older patients • Identify pathophysiology, risk factors and key presenting features • Describe strategies for prevention and management • Find opportunities to improve current practice Duke GEC www. interprofessionalgeriatrics. duke. edu
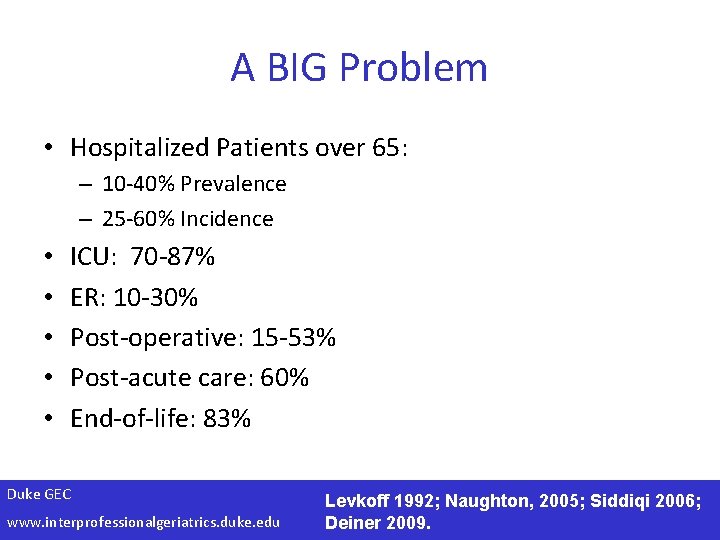
A BIG Problem • Hospitalized Patients over 65: – 10 -40% Prevalence – 25 -60% Incidence • • • ICU: 70 -87% ER: 10 -30% Post-operative: 15 -53% Post-acute care: 60% End-of-life: 83% Duke GEC www. interprofessionalgeriatrics. duke. edu Levkoff 1992; Naughton, 2005; Siddiqi 2006; Deiner 2009.

Costs of Delirium • In-hospital complications 1, 3 – UTI, falls, incontinence, LOS – Death • Persistent delirium– Discharge and 6 mos. 2 1/3 • Long term mortality (22. 7 mo)4 HR=1. 95 • Institutionalization (14. 6 mo)4 OR=2. 41 – Long term loss of function • Incident dementia (4. 1 yrs)4 • Excess of $2500 per hospitalization Duke GEC OR=12. 52 1 -O’Keeffe 1997; 2 -Mc. Cusker 2003; 3 Siddiqi 2006; 4 -Witlox 2010 www. interprofessionalgeriatrics. duke. edu

The experience… Duke GEC www. interprofessionalgeriatrics. duke. edu

Grade for Recognition: D • 33 -95% of in hospital cases are missed or misdiagnosed as depression, psychosis or dementia • ER: 15 -40% discharge rate of delirious patients – 90% of delirium missed in ED is then also missed in hospital! Duke GEC www. interprofessionalgeriatrics. duke. edu Inouye 1998 ; Bair 1998.

Clinical Features of Delirium • • • Acute or subacute onset Fluctuating intensity of symptoms Inattention – aka “human hard drive crash” Disorganized thinking Altered level of consciousness – Hypoactive v. Hyperactive • Sleep disturbance • Emotional and behavioral problems Duke GEC www. interprofessionalgeriatrics. duke. edu

In-attention • Cognitive state DOES NOT meet environmental demands • Result= global disconnect – Inability to fix, focus, or sustain attention to most salient concern • Hypoattentiveness or hyperattentiveness • Bedside tests – Days of week backward – Immediate recall Duke GEC www. interprofessionalgeriatrics. duke. edu

This Can Look Very Much Like… …. depression • • 60% dysphoric 52% thoughts of death or suicide 68% feel “worthless” Up to 42% of cases referred for psychiatry consult services for depression are delirious Duke GEC www. interprofessionalgeriatrics. duke. edu Farrell 1995

Improving The Odds of Recognition • Clinical examination – CAM • Team observations – Nursing notes • Prediction by risk – Predisposing and precipitating factors Duke GEC www. interprofessionalgeriatrics. duke. edu

Confusion Assessment Method (CAM) 1. 2. 3. 4. Acute onset and fluctuating course Inattention Disorganized thinking Altered level of consciousness Duke GEC www. interprofessionalgeriatrics. duke. edu Or Inouye 1994

CAM • Geropsychiatry assessment standard • Recent systematic review 2 – – Sensitivity 86% (74 -93) Specificity 93% (87 -96) LR + 9. 4 (5. 8 -16) LR – 0. 16 (0. 09 -0. 29) • Other tools: – CAM-ICU – Delirium Rating Scale Duke GEC www. interprofessionalgeriatrics. duke. edu 1 Inouye 1996; 2 Wong 2010.

Nursing Input • Chart Screening Checklist • Nurses’ commonly charted behavioral signs (Sensitivity= 93. 33%, Specificity =90. 82% vs CAM) • Pulling at tubes, verbal abuse, odd behavior, “confusion”, etc • 97. 3% of diagnoses of delirium can be made by nurses’ notes alone using CSC • 42. 1% of diagnoses made by physicians’ notes alone using CSC Duke GEC www. interprofessionalgeriatrics. duke. edu Kamholz, AAGP 1999
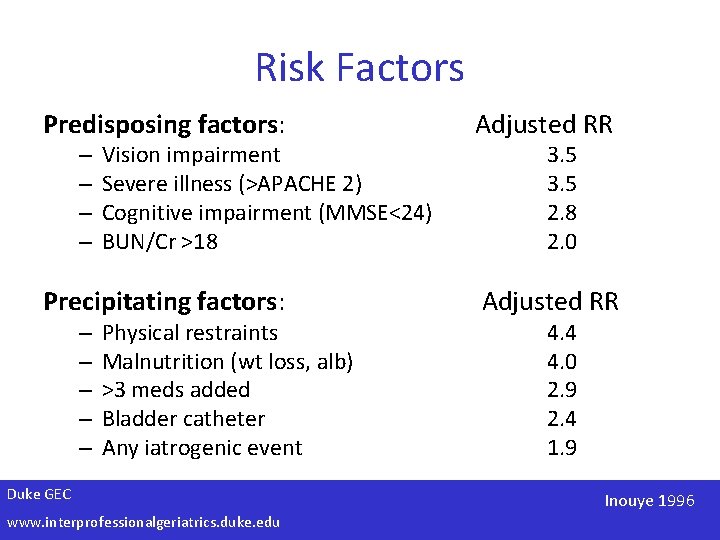
Risk Factors Predisposing factors: Adjusted RR Precipitating factors: Adjusted RR – – – – – Vision impairment Severe illness (>APACHE 2) Cognitive impairment (MMSE<24) BUN/Cr >18 Physical restraints Malnutrition (wt loss, alb) >3 meds added Bladder catheter Any iatrogenic event Duke GEC www. interprofessionalgeriatrics. duke. edu 3. 5 2. 8 2. 0 4. 4 4. 0 2. 9 2. 4 1. 9 Inouye 1996

Putting it all together. . . Predisposing Factors Precipitating Factors Duke GEC www. interprofessionalgeriatrics. duke. edu Inouye 1996

Oxidative Stress Model: ARDS • ANY source of ischemia – Low cardiac output – Impaired pulmonary function/oxygenation – Low Hgb/Hct • Mechanisms: – Ca++ influx, imbalance of neurotransmitters – Neuronal damage, including decreased synaptic transmission & cell death Duke GEC www. interprofessionalgeriatrics. duke. edu
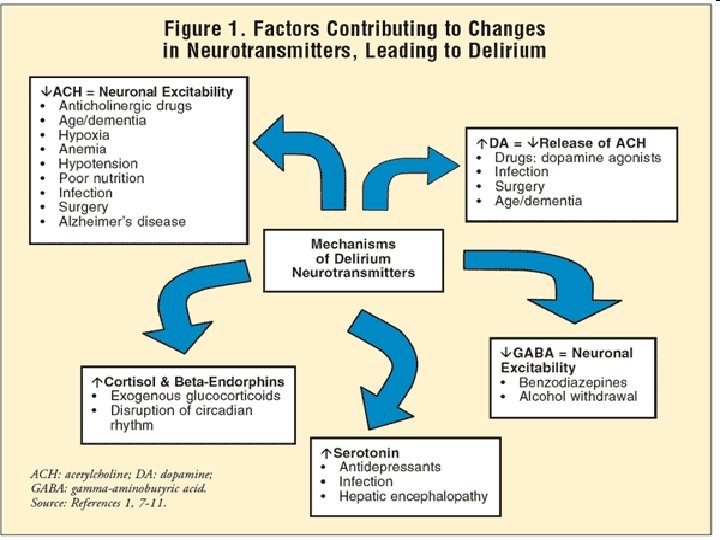
Duke GEC www. interprofessionalgeriatrics. duke. edu

Inflammatory Process Model: Sepsis • Peripheral interleukins (IL 6, TNFa, IL 1 B) induce symptoms of delirium – Increase permeability of BBB – Alter neurotransmission • TNFa can persist for months in CNS • May share inflammatory mechanisms with dementia Duke GEC www. interprofessionalgeriatrics. duke. edu

Pathophysiology of delirium • Delirium in frail patients often associated with disturbances of most basic substrates and cellular functions: – Impaired oxygenation (blood loss, pulmonary disease) – Metabolic disturbances (Na, Calcium) – Infection/inflammation (UTI, Pneumonia) – Medications • Primary CNS causes are in the distinct minority Duke GEC www. interprofessionalgeriatrics. duke. edu

Multicomponent Intervention to Prevent Delirium • 852 patients over 70 on Gen Med – IM risk (1 -2 RF’s) or High risk (3 -4 RF’s) • • Randomized by units with prospective matching Standardized protocols for 6 risk factors ID Team: Nurse specialist, PT, RT, MD and volunteers Outcomes assessed daily by CAM Duke GEC www. interprofessionalgeriatrics. duke. edu Inouye 1999.
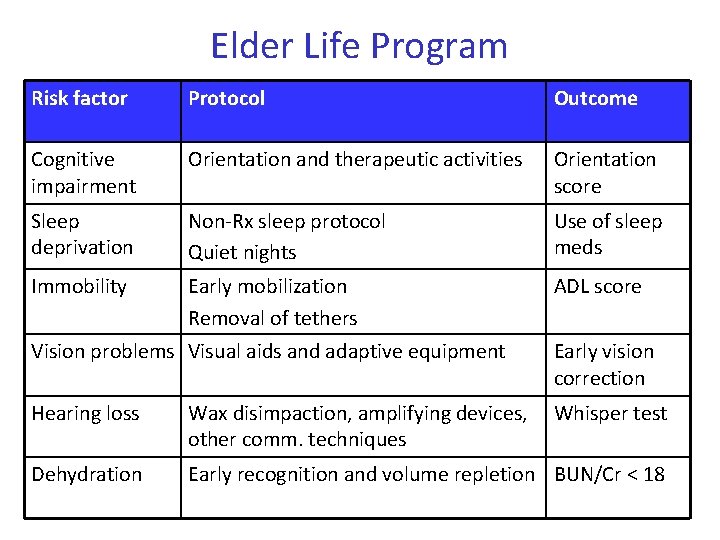
Elder Life Program Risk factor Protocol Outcome Cognitive impairment Orientation and therapeutic activities Orientation score Sleep deprivation Non-Rx sleep protocol Quiet nights Use of sleep meds Immobility Early mobilization Removal of tethers ADL score Vision problems Visual aids and adaptive equipment Early vision correction Hearing loss Wax disimpaction, amplifying devices, other comm. techniques Whisper test Dehydration Early recognition and volume repletion BUN/Cr < 18
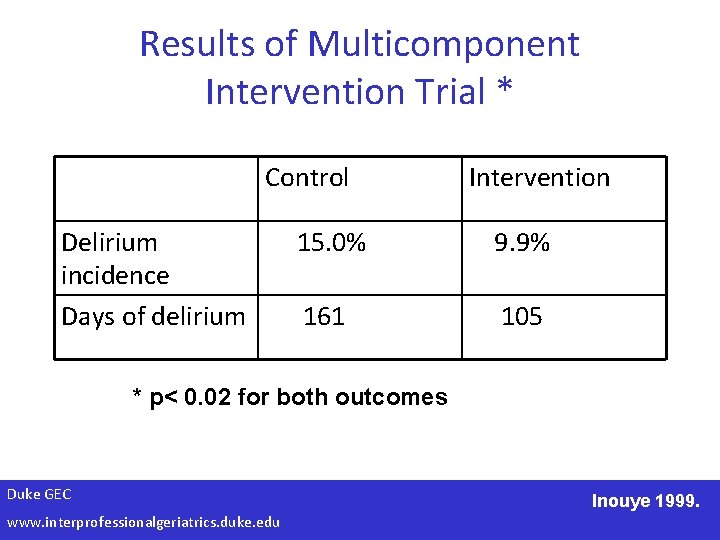

Results of Multicomponent Intervention Trial * Control Delirium incidence Days of delirium Intervention 15. 0% 9. 9% 161 105 * p< 0. 02 for both outcomes Duke GEC www. interprofessionalgeriatrics. duke. edu Inouye 1999.

Results • Most effective for IM risk group • No change in severity of delirium • Cost – $327/pt – $6341/case prevented • No lasting beneficial effect on functional status or resource utilization • Benefit replicated Duke GEC www. interprofessionalgeriatrics. duke. edu Inouye 1999; Rizzo 2001; Bogardus 2003

Reducing Delirium After Hip Fracture Geriatrics Consultation CNS oxygen delivery Fluid and electrolytes Treatment of pain Unnecessary medications • Bowel/bladder • Early mobilization • • Duke GEC www. interprofessionalgeriatrics. duke. edu • Prevention, early detection and treatment of complications • Nutrition • Environmental stimuli • Agitated delirium Marcantonio 2001.
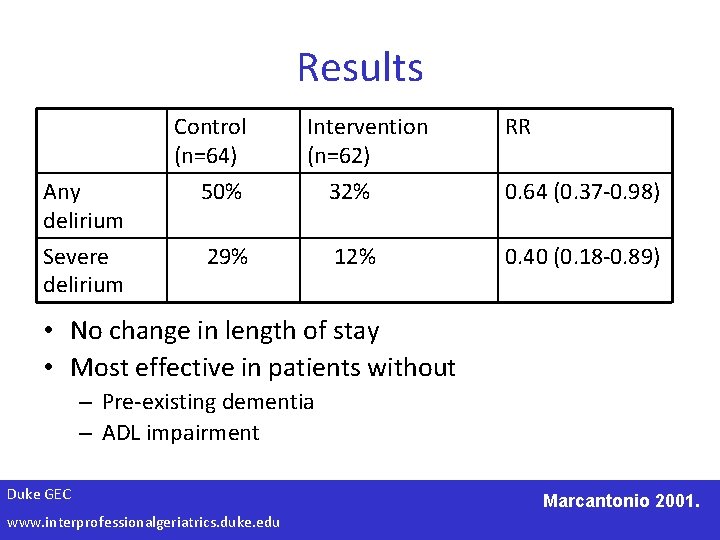
Results Any delirium Severe delirium Control (n=64) 50% Intervention (n=62) 32% 29% 12% RR 0. 64 (0. 37 -0. 98) 0. 40 (0. 18 -0. 89) • No change in length of stay • Most effective in patients without – Pre-existing dementia – ADL impairment Duke GEC www. interprofessionalgeriatrics. duke. edu Marcantonio 2001.

Pharmacotherapy • Dopamine blockade 1 – Haldol (1. 5 mg daily) prophylaxis in high risk hip fracture patients – No change in incidence – Decrease in severity and duration • Acetylcholinesterase inhibitor 2 – Donepezil did not decrease incidence or severity of delirium Duke GEC www. interprofessionalgeriatrics. duke. edu 1 Kalisvaart 2005, 2 Liptzin 2005.

Treating pain • Prospective cohort study >500 hip fracture patients with and without delirium • Patients receiving <10 mg IV Morphine/day were 5 x more likely to become delirious • Patients reporting severe pain 10 x more likely to develop delirium Duke GEC www. interprofessionalgeriatrics. duke. edu Morrison 2003.

Delirium Management: Key Points • Early recognition of high risk patients and situations is key to effective management • Prevention is more effective than treatment • Address: – – Physiologic Environmental Pharmacologic Psychosocial • Enlist a team Duke GEC www. interprofessionalgeriatrics. duke. edu Sendelbach and Guthrie, 2009.
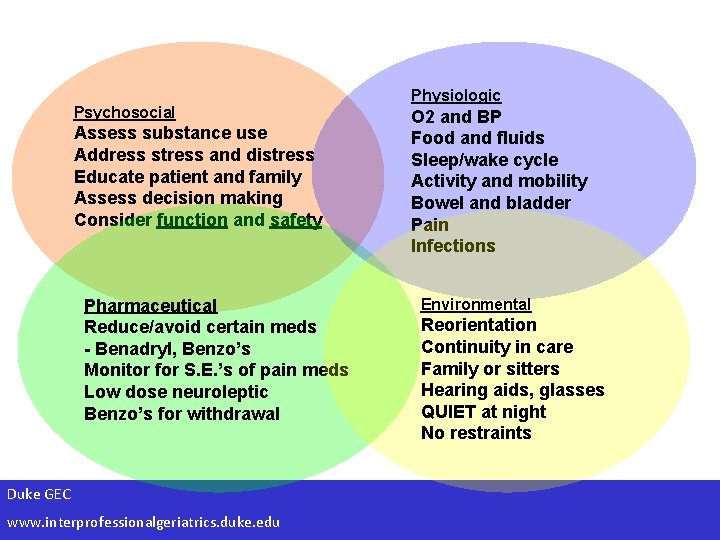
Psychosocial Assess substance use Address stress and distress Educate patient and family Assess decision making Consider function and safety Pharmaceutical Reduce/avoid certain meds - Benadryl, Benzo’s Monitor for S. E. ’s of pain meds Low dose neuroleptic Benzo’s for withdrawal Duke GEC www. interprofessionalgeriatrics. duke. edu Physiologic O 2 and BP Food and fluids Sleep/wake cycle Activity and mobility Bowel and bladder Pain Infections Environmental Reorientation Continuity in care Family or sitters Hearing aids, glasses QUIET at night No restraints
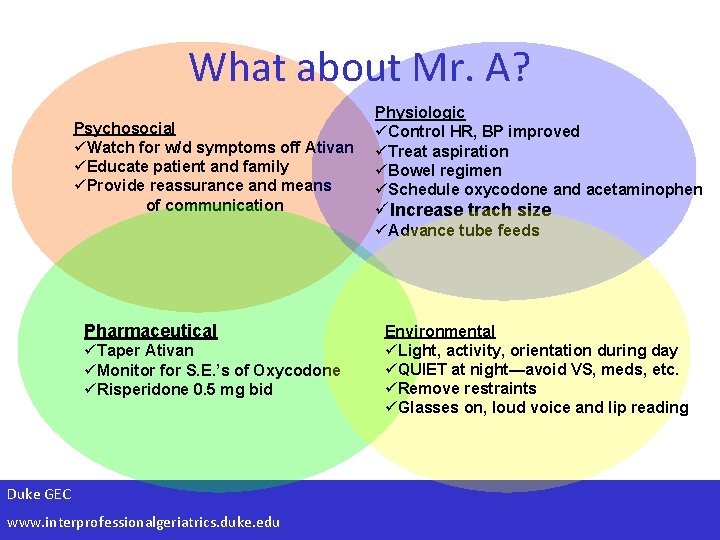
What about Mr. A? Psychosocial üWatch for w/d symptoms off Ativan üEducate patient and family üProvide reassurance and means of communication Physiologic üControl HR, BP improved üTreat aspiration üBowel regimen üSchedule oxycodone and acetaminophen üIncrease trach size üAdvance tube feeds Pharmaceutical üTaper Ativan üMonitor for S. E. ’s of Oxycodone üRisperidone 0. 5 mg bid Duke GEC www. interprofessionalgeriatrics. duke. edu Environmental üLight, activity, orientation during day üQUIET at night—avoid VS, meds, etc. üRemove restraints üGlasses on, loud voice and lip reading

Geriatrics • Inpatient consult service • Assistance with older adults with: – Delirium and other cognitive disorders – Multiple, complex medical problems – Medications, medications – Goals of care • Pager 970 -0370 Duke GEC www. interprofessionalgeriatrics. duke. edu

Old way…. D = Dehydration E = Electrolytes (including glucose, Ca) L= Low oxygen I = Infection R = Retention of urine/stool I = In pain U = Under-diagnosed withdrawal M = Medications Duke GEC www. interprofessionalgeriatrics. duke. edu

A better way…. NP’s PA’s Medicine Social work Psychosocial Physiologic Nursing Patients and Caregivers Environmental Pharmacologic Pharmacy Nutrition Administrators Duke GEC www. interprofessionalgeriatrics. duke. edu PT/OT

• 5 year, $1. 2 million project funded by HRSA • Goal: Create Geriatrics Education Hub - Staffed by interprofessional faculty - Focused on improving the care of older adults with or at risk for delirium - Learning resources, clinical experiences and practice improvement projects - Part of six school consortium addressing this issue Duke GEC www. interprofessionalgeriatrics. duke. edu

Delirium: Nursing Strategies Duke NICHE Geriatric Resource Nurse Initiative Kristin Nomides RN Grace Kwon RN Samantha Badgley RN Duke Hospital 2100 Duke GEC www. interprofessionalgeriatrics. duke. edu

Supporting Literature: Nursing Interventions Yale Delirium Prevention Program : multi-component interventions § § § Cognitive impairment with Reality Orientation Sleep enhancement protocol Sensory impairment with therapeutic activities protocol Sensory deprivation Dehydration § Reduction in delirium 9. 95% (c) vs. 15% (i); LOS & # episodes Inouye, s. 2004 Delirium education for team (MD and RN) § Provided post program support and learning reinforcement § 250 acute admit patients > 70 recruited on 2 units § Delirium 12/122 intervention unit vs. 25/128 control unit Tabet N, , et al, 2005 Post op multi-factorial intervention educational program § Teamwork and care planning on prevention and treatment of delirium § Targeted delirium risk factors § Post op delirium compared to controls (56/102 and 73/97) Lundrtrom, et al. 2007 Duke GEC www. interprofessionalgeriatrics. duke. edu

Nursing Interventions: • Delirium & Risk Factors Staff Education • Activity Cart / Busy Apron – Stimulate cognitive and motor skills • All About Me Poster – Orientation Information • Me File – Orientation information provided by patient / family for high risk patients • Question Mark – Identification of patients with AMS Duke GEC www. interprofessionalgeriatrics. duke. edu ? Altered Mental Status

Summary • RESPECT delirium. Its common and caustic. • PREDICT delirium. Assess for common predisposing and precipitating factors. • RECOGNIZE delirium. It can be diagnosed with simple tools (e. g. CAM). • PREVENT delirium. It can be averted with multicomponent strategies. • RECRUIT team members to improve care. Duke GEC www. interprofessionalgeriatrics. duke. edu

GEC crew Eleanor Mc. Connell, RN, MSN, Ph. D Anthony Galanos, MD Jason Moss, Pharm. D Julie Pruitt, RD Cornelia Poer, MSW Gwendolen Buhr, MD Mamata Yanamadala, MD S. Nicole Hastings, MD Jennie De Gagné, Ph. D, MSN, MS, RN-BC • Katja Elbert-Avila, MD • • • Duke GEC www. interprofessionalgeriatrics. duke. edu Sandro Pinheiro, Ph. D Robert Konrad, Ph. D Emily Egerton, Ph. D Heidi White, MD Kathy Shipp, PT, Ph. D Deirdre Thornlow, RN, Ph. D Lisa Shock, MHS, PA-C Michelle Mitchell, LMBT Michele Burgess, MCRP Joan Pelletier, MPH Sujaya Devarayasamudram, RN, MSN • Loretta Matters, RN, MSN • • •
- Slides: 50