Delirium Recognition Assessment Prevention Management WRHA Surgical Program

































- Slides: 37

Delirium: Recognition Assessment Prevention Management WRHA Surgical Program Delirium Guidelines

Delirium Definition: A disturbance of consciousness with inattention that develops over a short time & fluctuates

What is Delirium? • An acute confusional state • Usually has a reversible cause • Characterized by: – Inattention – Sudden onset – ………………. .

Why Should We Use Delirium Guidelines ? • Delirium can result in: – morbidity and mortality – length of stay – rates of admission to long term care facilities – 20% of patients discharged post hip # still had evidence of delirium (Journal of American Geriatric Society 2001 May; 49(5): 678 -9).

Outcomes of Delirium (even with complete recovery, 30% dementia within 3 years = decreased brain reserve)

Recognition of Delirium • Previous studies 32%-66% of cases are unrecognized by Medical Staff Yale- New Haven study (Inouye S. Ann Intern Med 1993: 119 -474) – 65% unrecognized by Physicians – 43% unrecognized by Nurses

Top 4 Independent Risk Factors for Delirium Vision impairment: Any severe illness: Cognitive impairment: High Urea/Creatinine ratio: Inouye S. Ann Intern Med 1993: 119 -474

4 Independent Risk Factors for Nurse Under-Recognition • Hypoactive Delirium • Age 80 yrs and over • Visual Impairment • Dementia

Types of Delirium • Hyperactive • Hypoactive • Mixed

Causes of Delirium? • Anything that hurts the brain or impairs its proper functioning can provoke a delirium! • Brain’s way of demonstrating “acute organ dysfunction”

Causes of Delirium: 1. 2. 3. 4. 5. 6. Drugs Infection System failure/events Metabolic Imbalance Dehydration/Poor Nutrition Surgery or general anaesthetic within the last 5 days

Causes of Delirium: 7. Pain 12. Sleep disruption 8. Uncorrected sensory 13. No factors can be or language impairment 9. Fecal Impaction 10. Urinary Retention/Catheter 11. Restraints identified 20% of the time 14. Recent severe illness or event involving hypoxia

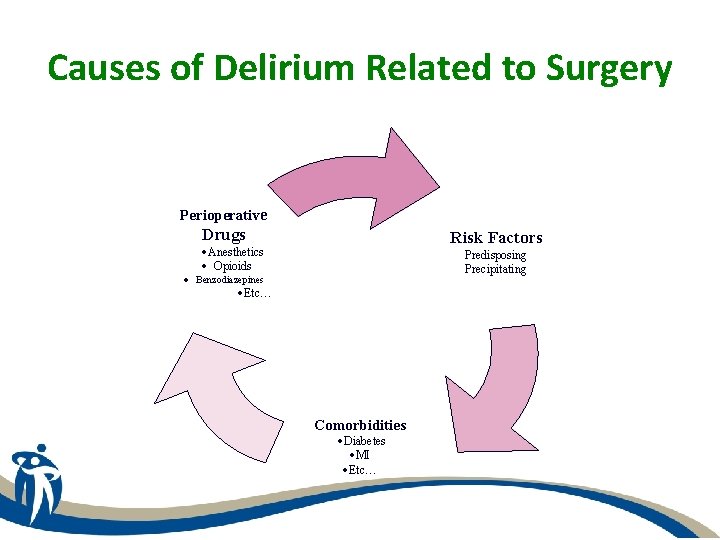
Causes of Delirium Related to Surgery Perioperative Drugs Risk Factors ·Anesthetics · Opioids Predisposing Precipitating · Benzodiazepines ·Etc… Comorbidities ·Diabetes ·MI ·Etc…

Theories for Post Op Delirium • Acetylcholine interaction with medications used during surgery • Increase of neurotransmitters, serotonin and dopamine during surgery • Previous abnormality levels of melatonin • Damage to neurons by oxidative stress or inflammation caused by a surgical procedure • Post op abnormal brain waves

Medications Associated with Delirium • Any drug can potentially cause confusion • Take a careful history of any new drug STARTED or any old drug STOPPED recently

Medications Associated with Delirium • Over the counter drugs – Cimetidine – Cough/Cold Remedies – Gravol/Maxeran – Sleeping medications – Herbal meds

Reference List of Drugs with Anticholinergic Effects • Antidepressants • Antipsychotics • Antihistamines/ Antipruritics • Antiparkinsonian • Antispasmotics • Antiemetics • • • Opioids Anticonvulsants Antibiotics Corticosteroids Anticholinergics

Studies In studies, drugs with anticholinergic side effects have been shown to: • Lower cognitive scores in elderly subjects • Cause/worsen severity of delirium • Associated with more ADL decline in patients with dementia • Associated with faster MMSE decline in patients with dementia • If drugs reduced, be associated with improvements in dementia and delirium.

Full List of Safe Medications for the Older Adult Please see attachment at the end of this presentation

Assessing for Delirium

Pre-Admission Assessment • Decision Tree

CAM – Confusion Assessment Method – Sensitivity (94 to 100%), specificity (90 to 95%) Requirement for delirium = 1, 2 AND either 3 OR 4 1. Abrupt change? 2. Inattention, can’t focus? 3. Disorganized thinking? Incoherent, rambling, illogical? 4. 4. Altered level of consciousness? (Hyper-alert to stupor? ) AND

Trigger Questions 1. Acute change in behaviour? 2. Changes in function? 3. Changes in cognition? MMSE 4. Changes in medications? 5. Physiologically stable?

How Do We Assess for Inattention • Recite the months backwards or days backwards • Have the patient count backwards from 20 to 1. • Use the CAM

Once You Identify Delirium, Now What? • Identify the acute medical problems that could be either triggering the delirium, or prolonging it! • Clarify pre-morbid functional status, sequence of events and previous admission cognitive baseline • Identify all predisposing and precipitating factors, and consider the differential

Physical Exam – Vitals: normal range of BP, HR, Temp and pain – Good physical exam: particular emphasis on Cardiac, pulmonary and neurologic systems – Hydration status – Also rule out • fecal impaction • urinary retention • Infected pressure ulcer, UTI or pneumonia

Delirium workup: Lab testing • Basic labs most helpful! – CBC, lytes, BUN/Cr, glucose, CO 2, Ca+, Mg, PO 4 – TSH, B-12, LFTs & albumin • Infection workup (Urinalysis, CXR) +/blood cultures • EKG • O 2 sat/ABG

What About Prevention?

Yale Delirium Prevention Trial Risk Factors Intervention Cognitive Impairment. Reality orientation / therapeutic activities program Vision/Hearing impairment Vision / hearing aids / adaptive equipment Immobilization Early mobilization / Reduce immobilizing equipment Psychoactive medication Non pharmacologic approaches to sleep / anxiety / Restricted use of sleeping medication Dehydration Early recognition / Volume expansion Sleep deprivation Noise reduction strategies/sleep enhancement program Ref: Inouye SK, NEJM. 1999; 340: 669 -676

Prevention and Pre-Op Assessment • Pre-op Clinic Form • Pre- op- Questionnaire

What about Management?

Non Pharmacological Interventions • Always apply non-pharmacological interventions in your Care Plan. Examples – Initiate toileting routines – Mobilize ASAP – Quiet room, soothing music

Pharmacological Interventions • Only use medication if: – Non-pharmacological interventions are not successful – The patient is a danger to themselves or others • You may see the physician order or a pharmacist suggest the following medications: – Low dose Haloperidol or – Low dose Risperidone or – Low dose Olanzapine – ** Avoid the use of benzodiazepines

Pharmacological Interventions • It is important to remember that: – Dosing is best given prn when agitation becomes a concern or becomes a safety issue – Medications must be discontinued once the agitation from the delirium is resolved

Delirium Pamphlet • This is to be given to Families so that they may better understand what their family member is going through. • It is also recommended that it be displayed in any Pamphlet Holders for Patient and Family Education. • A copy of the pamphlet is found at the back of the presentation

Pre-Admission Clinic Forms

Questions ? ? ?