DELIRIUM IN ELDERLY CAN BE DIAGNOSED BY BIOMARKERS

DELIRIUM IN ELDERLY CAN BE DIAGNOSED BY BIOMARKERS? Magdy Dahab, MD Professor of Neurology, Azhar University, United Doctors Hospital, Jeddah, KSA March 28 th, 2019

DEFINITION • Delirium is a common and serious and acute neuropsychiatric syndrome characterized by inattention and global cognitive dysfunction • The etiologies are diverse, multifactorial and often reflects the pathophysiologic consequences of an acute medical illness, medical complications or drug intoxications • At present, the diagnosis of delirium depends on the presence of certain clinical features • Recently we identify biomarkers for delirium to predict its onset, severity, recovery rate or prognosis • Six approaches are examined to identify biomarkers of delirium: serum chemistry, genes, neurotransmitters, inflammatory factors, serum cortisol levels and end products of delirium

CHARACTERISTICS OF DELIRIUM • Disturbance of consciousness • Abnormal attention • Abnormal cognition • • • Orientation Memory Thought processing Executive function Perception • Acute in onset and fluctuating in course • Precipitated by acute medical illness, post-operative status, medications, or substance intoxication 3

BEHAVIOURS • Just “more confused” • Poor attention- can’t give a history • Looks around the room • Agitated, plucking at bed clothes • Hallucinating • Very quiet or drowsy • Reduced ability to care for self • Loss of mobility 4

DELIRIUM: EPIDEMIOLOGY • Prevalence in community 0. 5 - 2% • General hospital admissions ~20% • On admission 10 – 15% elders • During hospitalization up to 40% • At end of life up to 80% 5
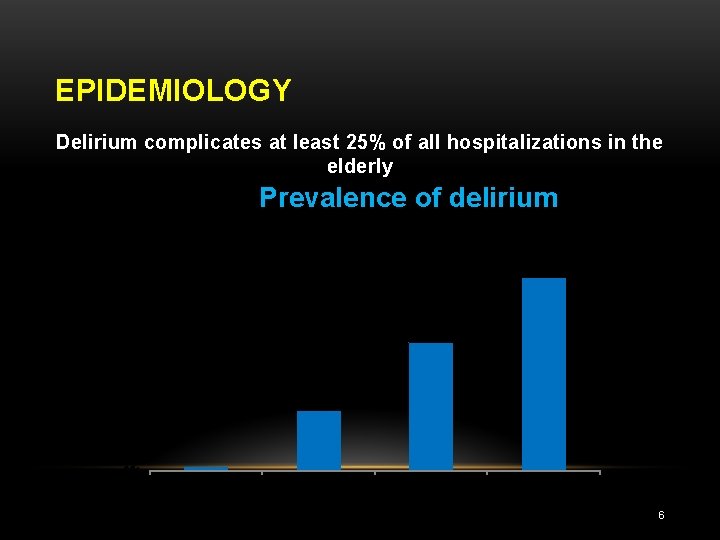
EPIDEMIOLOGY Delirium complicates at least 25% of all hospitalizations in the elderly Prevalence of delirium 100% 75% 50% 25% 0% Community Hospital admission Post-op ICU 6

INCIDENCE • 60%-80% of mechanically ventilated patients • 50%-70% of non-ventilated patients • Hypoactive delirium = 43. 5% • Hyperactive delirium = 1. 6% • Mixed delirium = 54. 1% 7

DELIRIUM: PRESENTATION • Hyperactive • Better recognized • More attention to treatment • Associated with improved outcome • Hypoactive • Little recognized • Depression is primary differential • Associated with poor outcomes • Mixed 8

CAUSES OF DELIRIUM? • Anything that hurts the brain or impairs its proper functioning can provoke a delirium! • Brain’s way of demonstrating “acute organ dysfunction” 9

FIGURE OUT THE TRIGGER Drug use (hypnotics, anticholinergic) (30%) Electrolyte abnormalities (40%) Lack of drugs (withdrawal) Infection (40%) Reduced sensory input (24%) Intracranial problems (stroke) Urinary retention and fecal impaction Myocardial or metabolic problems (14 - 26%) 10

ETIOLOGIES OF DELIRIUM Iatrogenic and polypharmacy • Anticholinergic medications • Opioids • Benzodiazepines • Steroids • Antihistamines • Antibiotics 11

DELIRIUM: NEUROBIOLOGY • Direct injury to the neurons • Metabolic • Ischemic • Alters synthesis/release of neurotransmitters • Stress response • Trauma, surgery, infection release of proinflammatory cytokines, elevated cortisol • Direct neurotoxic effects • Alters neurotransmitter levels 12

DELIRIUM: NEUROBIOLOGY • Best established neurotransmitter dysfunction: reduced cholinergic activity • Increased dopamine may also play a role • Low and excessive serotonin • Low and excessive GABA 13

DIAGNOSIS OF DELIRIUM • Delirium is a clinical diagnosis • History and physical examination • Meni Mental Status Examination • Rating Scales-consider on admission • Confusion Assessment Method • Delirium Rating Scale • Clock 14
DIAGNOSIS OF DELIRIUM • Lab tests cannot diagnose definite delirium but may support diagnosis e. g. CBC, ESR, Urine toxins, TSH, ammonia • CXR, EKG, LP if indicated • Neuroimaging • EEG • Generalized slowing in delirium, nonspecific • Triphasic waves in hepatic encephalopathy • Low voltage fast activity in BZD withdrawal 15

DELIRIUM WORKUP: LAB TESTING • Basic labs most helpful! • CBC, electrolytes, BUN/Cr, glucose, Ca+, Mg, • TSH, B-12, LFTs & albumin • Infection workup (Urinalysis, CXR) +/- blood cultures • O 2 sat/ABG Cause can not be identified in 15 to 25% 16

DELIRIUM: DIFFERENTIAL DIAGNOSIS • Dementia with Behavioral Disturbance • Psychotic Disorder (Schizophrenia) • Mood Disorder (Depression, Mania) • Catatonia 17
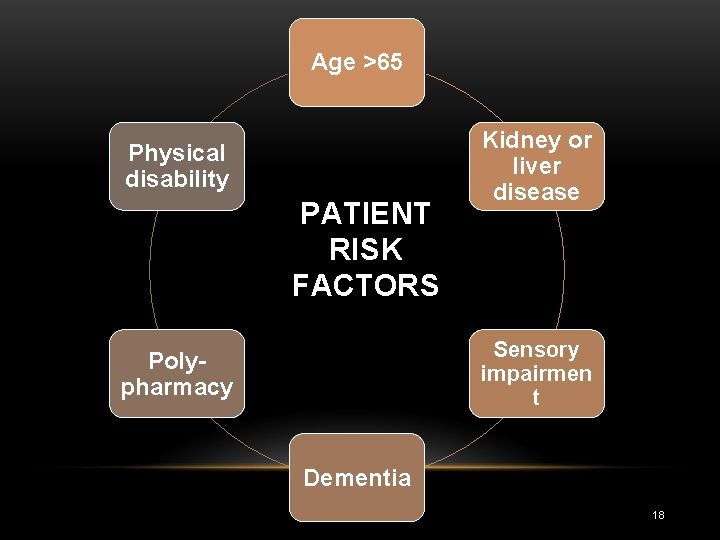
Age >65 Physical disability PATIENT RISK FACTORS Kidney or liver disease Sensory impairmen t Polypharmacy Dementia 18
TOP 4 INDEPENDENT RISK FACTORS Vision impairment: impairment Any severe illness: illness Cognitive impairment: impairment High Urea/Creatinine ratio: 19

BIOMARKERS • Definition: Biochemical or molecular parameters associated with presence and/or severity of specific disease state. They are measurable with physical examination laboratory assay or imaging • Three pattern of biomarker: 1. It may serve as a risk marker for disease i. e. present before disease onset e. g. apolipo-protein E 4 allele represents risk marker for Alzheimer disease 2. It may be a disease marker that is rising with disease onset and falls in recovery e. g. CA-125 for ovarian cancer 3. It may be end product of disease indicating damage e. g. creatine kinase in myocardial infarction
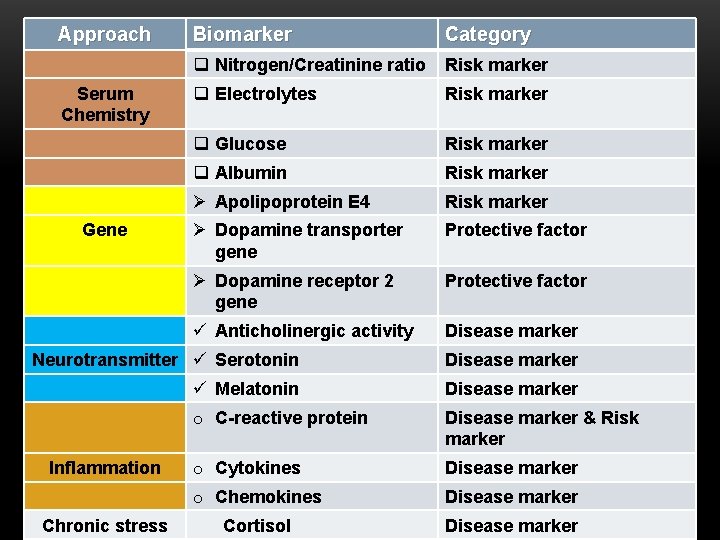
Approach Biomarker Category q Nitrogen/Creatinine ratio Risk marker q Glucose Risk marker q Albumin Risk marker Ø Apolipoprotein E 4 Risk marker Ø Dopamine transporter gene Protective factor Ø Dopamine receptor 2 gene Protective factor ü Anticholinergic activity Disease marker Serum q Electrolytes Risk marker BIOMARKERS FOR DELIRIUM Chemistry Gene Neurotransmitter ü Serotonin Disease marker ü Melatonin Disease marker o C-reactive protein Disease marker & Risk marker o Cytokines Disease marker o Chemokines Disease marker Cortisol Disease marker Inflammation Chronic stress

SERUM CHEMISTRY • Blood urine nitrogen (BUN)/creatinine ratio over 18 is one of 4 risk markers of delirium in hospitalized elderly • Abnormal serum levels of sodium, potassium and glucose are independent risk factors for delirium • Low albumin and hypermagnesemia are biochemistry imbalances associated with increased risk of delirium

GENETIC MARKERS APOLIPOPROTEIN E 4 ALLELE • Increasing evidence points to relationship between delirium and dementia because Genetic risk markers for dementia may also be risk markers for delirium • Presence of the Apo E 4 allele increased the risk of post-operative delirium after non-cardiac surgery so this Apo E 4 allele serve as a predictive factor for recovery from delirium

GENETIC MARKERS DOPAMINE-RELATED GENES • Polymorphisms in dopamine receptor and transporter genes were found to be associated with alcohol withdrawal delirium • Polymorphisms in the dopamine receptor gene was associated to reduced risk of delirium • Homogenous AA genotype in SLC 6 A 3 gene reduced risk of delirium by lower cerebral basal dopamine concentration

NEUROTRANSMITTERS ACETYLCHOLINE & SERUM ANTICHOLINERGIC ACTIVITY • Postulated mechanism for delirium is cholinergic failure. Clinically, delirium is one manifestation of anticholinergic toxicity • Cumulative serum anticholinergic activity in peripheral blood is measured by utilizing a radio receptor assay • Anticholinergic activity acts as a biomarker for delirium

NEUROTRANSMITTERS SEROTONIN, MELATONIN & OTHER SERUM AMINO ACIDS Serotonin: • Synthesis & release in human brain is dependent on availability of its precursor tryptophan from blood. Tryptophan competes with other large neural amino acids (LNAA) like tyrosine & phenylalanine for transport across blood brain barrier • Plasma ratio of tryptophan/LNAA & plasma levels of tryptophan and serotonin is used as indirect peripheral measures of central serotonergic functioning • Both increased & decreased serotonergic activity are associated with delirium. Elevated CNS serotonin activity can be found in hepatic encephalopathy. Serotonin syndrome is a main symptom of delirious patients.

NEUROTRANSMITTERS SEROTONIN, MELATONIN & OTHER SERUM AMINO ACIDS Melatonin: • It is hormone affecting pattern of sleep, its duration & quality. Sleep pattern of delirious patients are usually disturbed • Lower post/preoperative melatonin concentration is observed when delirium developed in elderly. While higher level of melatonin was detected in hypoactive type of delirium while low level was in hyperactive type • This is measured by urinary chief metabolite of melatonin called 6 -sulphatoxymelatonin

NEUROTRANSMITTERS SEROTONIN, MELATONIN & OTHER SERUM AMINO ACIDS Other serum amino acids: • Although dopamine & norepinephrine may be related in delirium pathogenesis, no research within last 15 years has investigated them as a biomarker for delirium • Serum amino acids fluctuate widely depending on protein content of diet • Analyzing these amino acids require specialized processing of serum

INFLAMMATORY FACTORS C-REACTIVE PROTEIN • Delirium is common in inflammatory states e. g. infections, cancer & postoperative recovery. CRP is a widespread used as traditional marker of infection, inflammation & tissue injury in activation of vascular endothelial cells leading to organic brain disease • It is associated • Higher levels of CRP were seen in postoperative elderly with complications. So CRP levels are highly predictive of incident delirium.

INFLAMMATORY FACTORS CYTOKINES & CHEMOKINES • Cytokines are produced by activated immune cells whereas chemokines are locally acting cytokines that rapidly mediate leukocytes to site of inflammation • Therapeutic use of cytokines (interferons) can induce symptoms of delirium. Interleukin-1 increases acetyl cholinesterase activity & inhibits acetylcholine release from hippocampal neurons • Association between interlukin-6 & delirium was evident. Chemokines are measured using new method of dual-channel microsphere flow cytometry

CHRONIC STRESS CORTISOL • Chronic stress is well known to activate sympathetic nervous system leading to activation of hypothalamicpituitary axis and elevates serum cortisol • Delirium is associated with stress leading to disturbance of hypothalamic-pituitary-adrenal system. Studies showed link hypo- or hyper cortisolemia with delirium • There is a strong relationship between delirium and dexamethasone suppression, irrespective of age & severity of trauma

END PRODUCTS OF DELIRIUM S 100 B PROTEIN (S 100 B) • S 100 B belongs to the family of calcium-binding proteins is expressed mainly by astrocytes & is found in both intra- and extracellular brain tissue • Elevated in blood & CSF after disturbance of integrity astrocytes & Schwann cells membrane increasing permeability of BBB. Elevation is associated with delirium after abdominal & cardiac surgeries • Comparing S 100 B, cortisol and IL-6, It was found that S 100 B is the strongest independent marker of post hip fracture surgery delirium

END PRODUCTS OF DELIRIUM NEURON SPECIFIC ENOLASE • NSE is intracytoplasmic glycolytic enzyme enolase found in neurons and neuroendocrine tissue which is elevated in circulating blood when more of these cells have died • Some patients develop sequelae of persistent cognitive deficit, which may progress to dementia. This reflect irreversible brain damage caused by pathophysiological mechanism of dementia • Serum biomarkers of neuronal injury or death may indicate delirium persistence

PHARMACOLOGICAL INTERVENTIONS • Only use medication if: • Non-pharmacological interventions are not successful • Patients are danger to themselves or others • Physicians and pharmacists suggest the following medications: • • Low dose Haloperidol or Low dose Risperidone or Low dose Olanzapine ** Avoid the use of benzodiazepines 34

MEDICATION HIERARCHY Level One - Neuroleptics Level Two – Analgesics; Sedatives-Hypnotics; Dopamine agonists Level Three – Antihistamine; anti-inflammatory; anticholinergic; antidepressants Level Four – H 2 Antagonist, Dihydropyridine; Tricyclic antidepressants; anti-Parkinson 35

PHARMACOLOGICAL INTERVENTIONS • It is important to remember that: • Dosing is best given pm when agitation becomes a concern or becomes a safety issue • Medications must be discontinued once the agitation from the delirium is resolved 36

PREVENTION • Limit use of medications known to cause delirium • Ensure good nutrition and hydration • Correct sensory deprivation • Encourage normal sleep patterns • Promote cognitive stimulation 37

PROGNOSIS • Delirium is usually reversible. • Take several weeks for mental function to return to normal levels • The longer the delirium goes untreated – there is worsening global cognition and executive function worsening. • Pathophysiological evidence – inflammation – neuronal apoptosis – brain atrophy 38
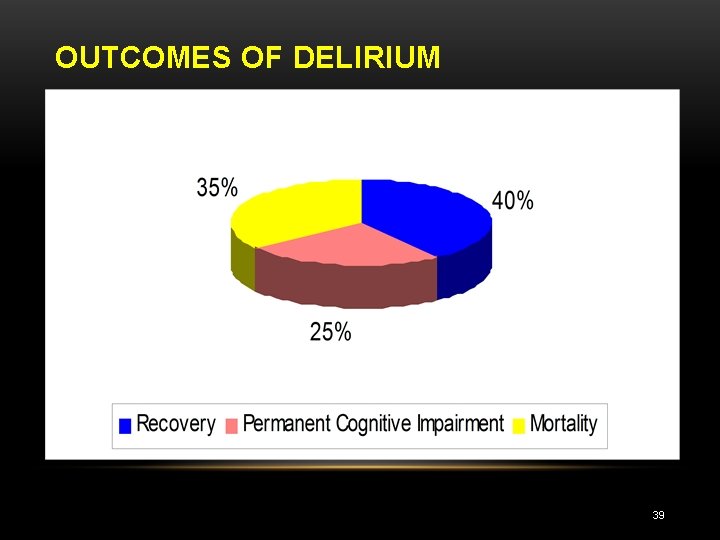
OUTCOMES OF DELIRIUM 39

CONCLUSION • Dementia is a risk factor for delirium which is common in the geriatric population • Recognizing delirium, and distinguishing this syndrome from primary psychiatric conditions is critical • Delirium can present in a variety of ways and can be a result of a number of etiologies • biomarkers of delirium are serum chemistry, genes, neurotransmitters, inflammatory factors, serum cortisol levels and end products of delirium • Antipsychotic medications are useful in management of symptoms of delirium 40

Thank you www. magdydahab. com
- Slides: 41