DEGENERATIVE OSTEOARTHRITIS Treatment and Rehabilitation Assoc Prof Ece

DEGENERATIVE OSTEOARTHRITIS Treatment and Rehabilitation Assoc. Prof. Ece AYDOĞ Physical Medicine and Rehabilitation
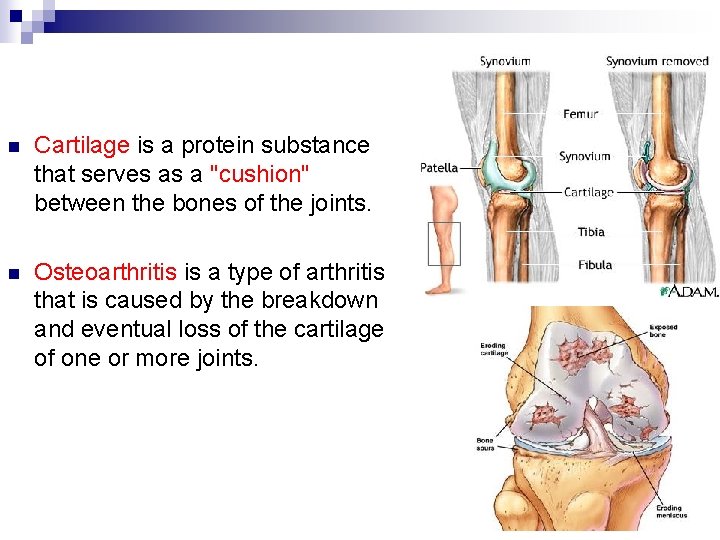
n Cartilage is a protein substance that serves as a "cushion" between the bones of the joints. n Osteoarthritis is a type of arthritis that is caused by the breakdown and eventual loss of the cartilage of one or more joints.

Constituents of hyaline cartilage n n Cellular material: Chondrocytes: 5% Extracellular material: Matrix: 95% ( Water comprises approximately 70%) – Collagen fibres – Proteoglycan molecules
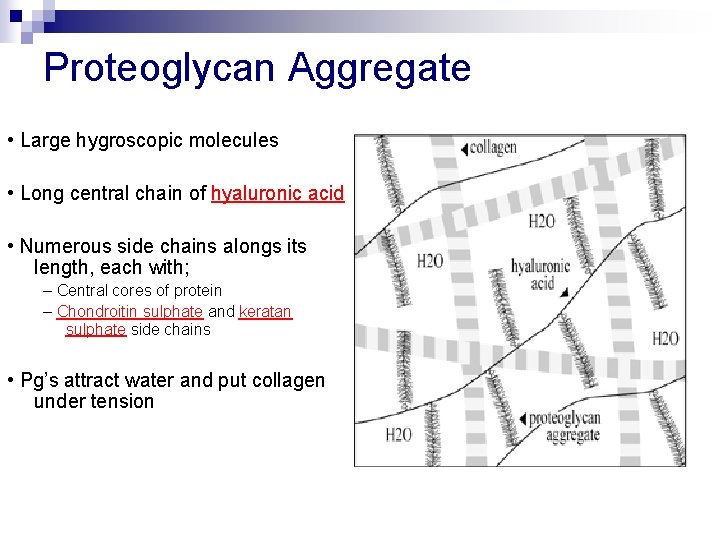
Proteoglycan Aggregate • Large hygroscopic molecules • Long central chain of hyaluronic acid • Numerous side chains alongs its length, each with; – Central cores of protein – Chondroitin sulphate and keratan sulphate side chains • Pg’s attract water and put collagen under tension
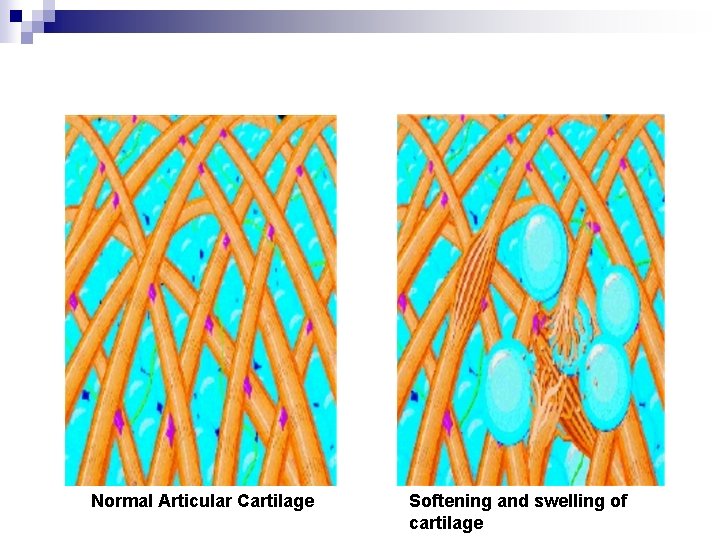
Normal Articular Cartilage Softening and swelling of cartilage
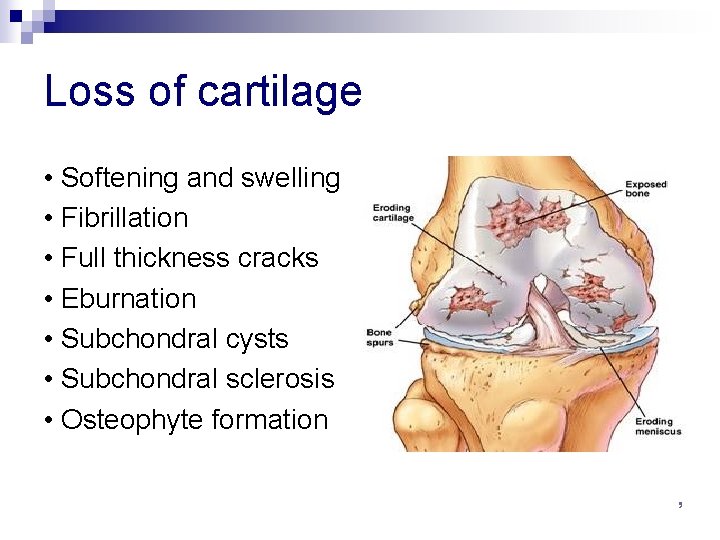
Loss of cartilage • Softening and swelling • Fibrillation • Full thickness cracks • Eburnation • Subchondral cysts • Subchondral sclerosis • Osteophyte formation ‘
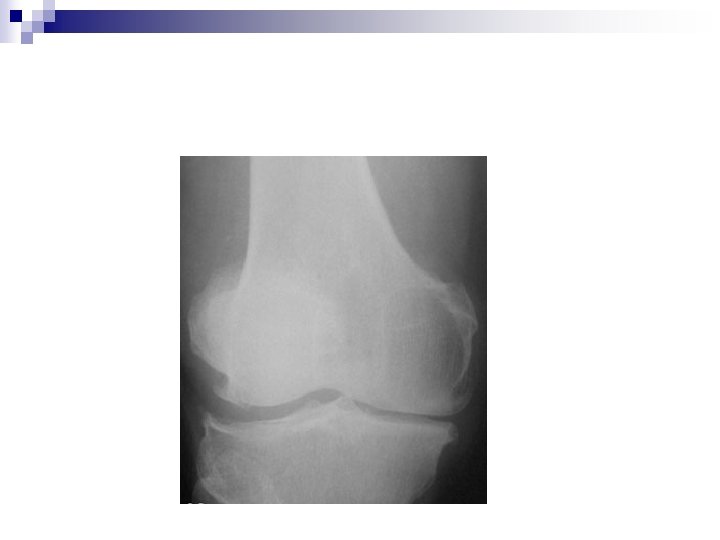


Individual risk factors for development of OA • Obesity: knee > Hip • Family history (genetic): polyarticular esp hands • Trauma • Hypermobility • Dysplasia: Hip and knee • Occupation and sport: excessive and repeated loading of a joint

Clinical features Pain and tenderness n Originates in joint /periarticular soft tissue n Diffuse/ sharp and stabbing local pain n Initially, symptomatic patients incur pain during activity, which can be relieved by rest and may respond to simple analgesics n Joints may become unstable as the OA progresses; therefore, the pain may become more prominent (even during rest) and may not respond to medications

Movement abnormalities n Gelling ¨ ¨ n Coarse crepitus ¨ n stiffness after periods of inactivity passes over within minutes of using joint again palpate/hear Reduced ROM ¨ capsular thickening and bony changes in joint
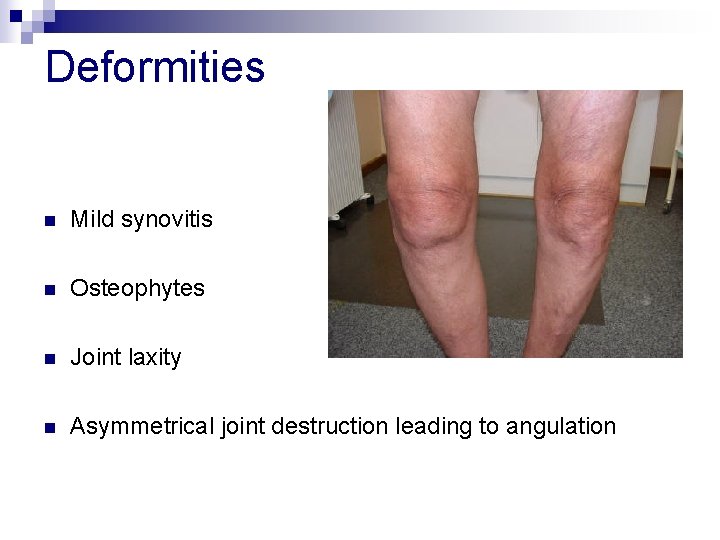
Deformities n Mild synovitis n Osteophytes n Joint laxity n Asymmetrical joint destruction leading to angulation

Treatment Principles • Education • Physiotherapy – Exercise program – Pain relief modalities • Aids and appliances • Medical Treatment • Surgical Treatment

• Prevent overloading of joint; Obesity!! • Appropriate use of treatment modalities • Importance of exercise program


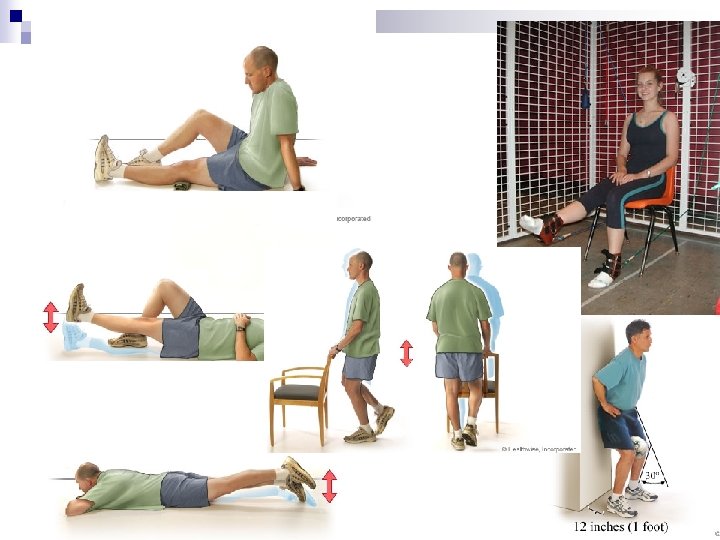
Exercises n Flexibility exercises — daily stretching and range-of-movement exercises. n Strengthening exercises — (a) Isometric exercises (static muscle contraction that does not move a joint or alter muscle length) up to twice daily during acute inflammatory periods; and (b) Isotonic exercises (resistance training exercises, often with weights), maximum two days per week. n Endurance/fitness exercises — such as walking, swimming, dancing, aquarobics, cycling, 3– 4 times per week. ¨ The intensity, duration, and frequency of exercise should graded to allow for progression. be specified and

Physical Agents ¨Heat ¨Cold ¨Water ¨Pressure ¨Sound ¨Electrical Current

Physical Agents n n n Cryotherapy: Ice packs, commercial cold packs, iced towels, ice massage, cold baths (immersion), vapocoalant spray, contrast baths. Radiant heat: Infrared Conductive heat -Hot packs -Paraffin bath Superficial heat Hydrotherapy -Whirlpool -Hubbard tank Shortwave diathermy Deep heat Ultrasound

General Indications n Purported Uses ¨ Modulate pain ¨ Reduce or eliminate inflammation ¨ Increase rate of healing ¨ Modify muscle tone ¨ Increase connective tissue extensibility
Ice n Contraindications ¨ Cold hypersensitivity ¨ Raynaud’s disease ¨ Regenerating peripheral nerves n Precautions ¨ Over superficial main branches of nerve n Peroneal nerve ¨ Open ¨ Poor wounds sensation

Application n 10 minutes is sufficient n Re-applied regularly, every 2 -3 hours n Following approximately the first 3 -5 days of an acute injury
Red/Infra-Red Phototherapy

Conductive Heat Hot Packs Moist heat n Canvas filled wityh silica gel n Immersed in water of about 77 C n

Paraffin Bath Tank containing a mixture of paraffin and mineral oil n 52 -53 C n Areas that are diffucult to heat n Helps to soften the skin n

Contraindications (heat) n n n n n Pregnancy Acute inflammotory conditions Active Cancer Active bleeding Patients with cardiac insufficiency Extremly old adults and children less than 4 years old Patients with peripheral vascular disease Tissues that are devitalized by x-ray theraphy Already existing fever

Precautions Already existing edeme n Patients with sensory loss n Patients who are confused n
Low Level Laser Therapy Cold Laser Therapy Primary Effects – Similar to effects of Infrared therapy Secondary Effects – Cell proliferation, protein synthesis, growth factor secretion, neurotransmitter modification Tertiary Effects – System effects; Increase immune response, stimulate bone healing

Ultrasound n Therapeutic Ultrasound sends high frequency sound waves through tissue and has a thermal effect. n Therapeutic ultrasound frequency used is 0. 7 to 3. 3. MHz n Maximum energy absorption in soft tissue is 2 to 5 cm. n Intensity decreases as the waves penetrate deeper. n They are absorbed primarily by connective tissue: ligaments, tendons, and fascia (and also by scar tissue)

Ultrasound n Typical applications of Ultrasound ¨ Pain control (Munting 1978) ¨ Increase tissue extensibility (Knight 2001) ¨ Accelerate healing wounds (Dyson 1978), bone fractures (Duarte 1983) ¨ et al Pharm Res 1992)

Ultrasound Two types of benefit: n Thermal effects n Non thermal effects n Indications: n Soft tissue shortening (Joint contractures, scarring) n Subacute and chronic inflammation n
Electrical Stimulation n Common uses: ¨ Pain control (TENS, interferential) ¨ Iontophoresis (Direct Current) ¨ Muscle stimulation (NMES) ¨ Tissue healing (wound care)

TENS (Transcutaneous Electrical Nerve Stimulation) Pain control 2 theories of how TENS may control pain Gate control theory – high frequency TENS n Opiate-mediated control – low frequency TENS (Acupuncture- like TENS) n

TENS n Contraindications ¨ Patients with cardiac pacemakers ¨ Pregnancy ¨ Sites over the carotid sinus, laryngeal or pharyngeal muscles, sensitive eye areas, or mucosal membranes ¨ Do not use while operating hazardous machinery

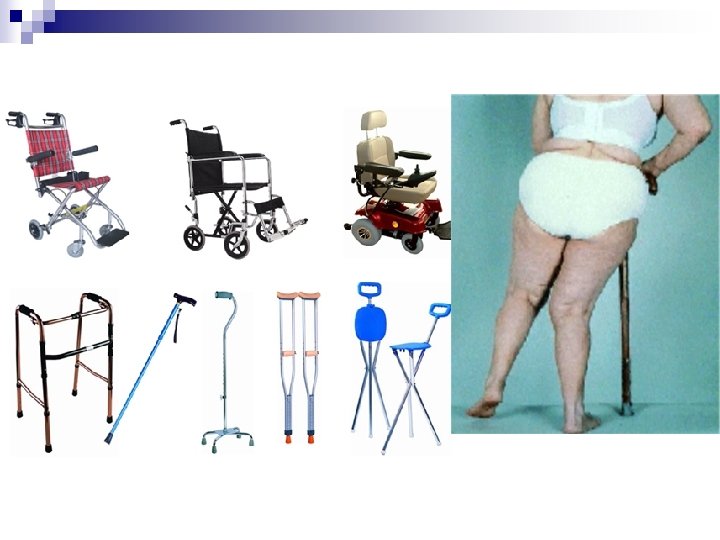
Aids and appliances n Braces / splints n Special shoes/insoles n Mobility aids n Aids: dressing, reaching, tap openers, kitchen aids n Taping of patella in patello femoral OA
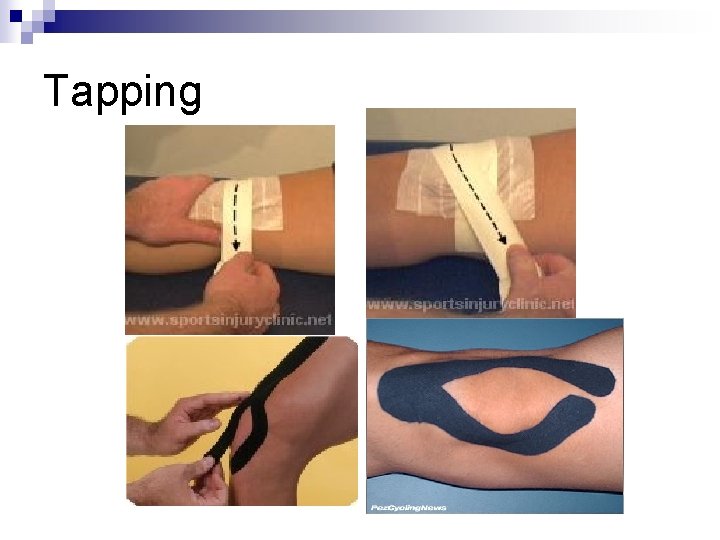
Tapping

Medical Treatment n n n n Simple analgesics: paracetamol Topical treatment; NSAI, capsaicin creams Glucoseamine; oral, topical NSAID’s Tramadol or opioidis Intra-articular corticosteroids Intra-articular viscosupplementation PRP
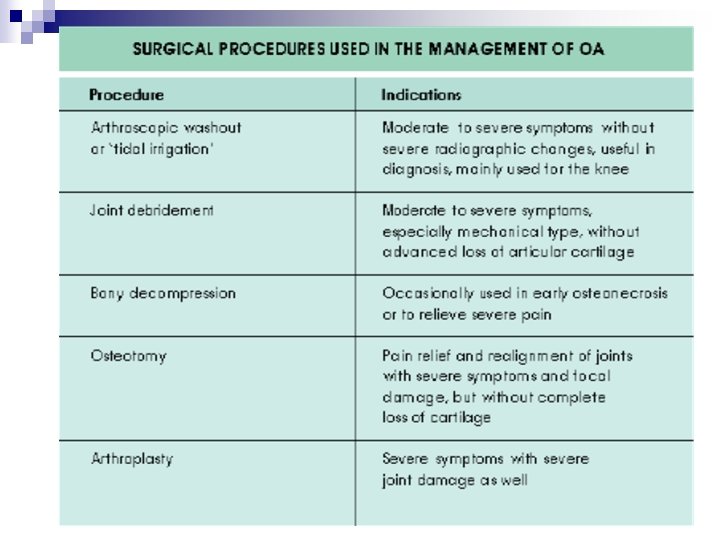
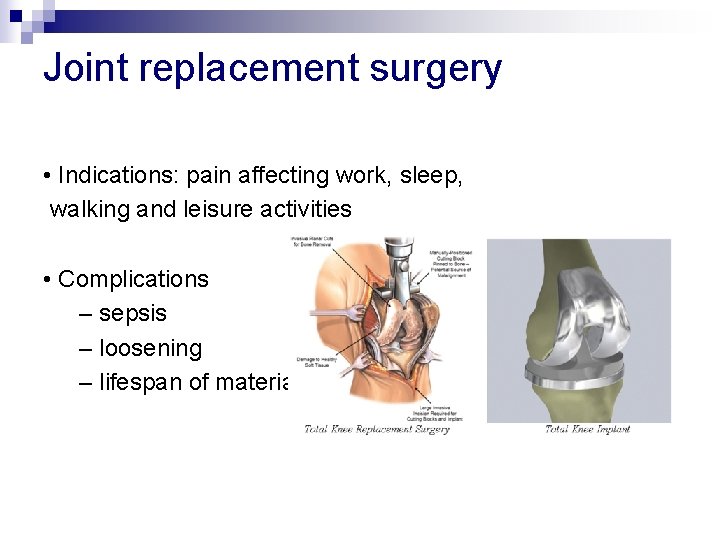
Joint replacement surgery • Indications: pain affecting work, sleep, walking and leisure activities • Complications – sepsis – loosening – lifespan of materials (mechanical failure)
- Slides: 41