Defnition Recurrent abortions is traditionally defined as three


Defnition Recurrent abortions is traditionally defined as three or more consecutive miscarriages occurring before 20 weeks. May affect as many as 1% to 2% of women of reproductive age

Some guidelines use the definition of two or more miscarriages for offering an evaluation of etiologic causes. (ASRM) An earlier evaluation( investigation) may be indicated Ø fetal cardiac activity was identified prior to a loss, Ø Woman older than 35 years, Ø Couple had difficulty in conceiving. (infertility)


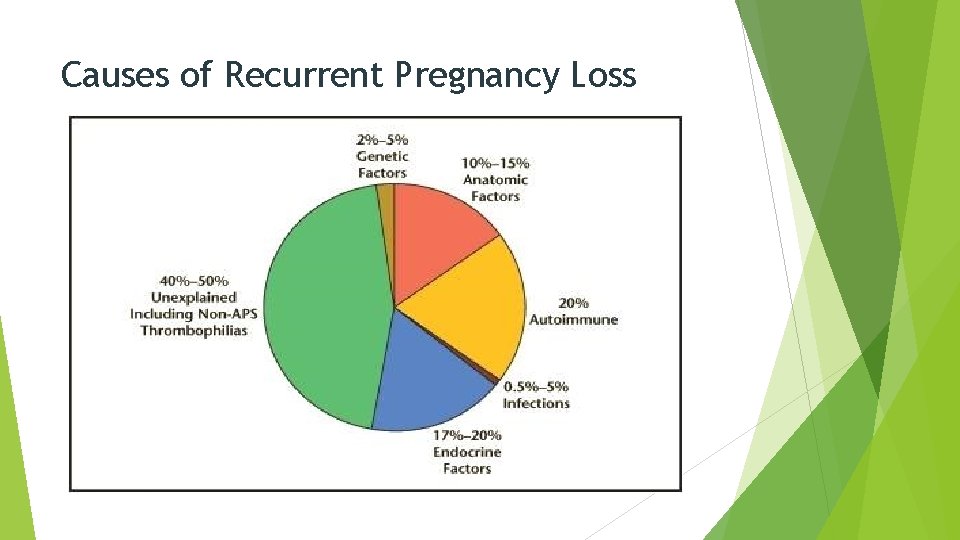
Causes of Recurrent Pregnancy Loss





Congenital Septate uterus 65 % • Unicornuate uterus 50% loss Uterus didelphys 40% loss Bicornuate uterus 30 % loss DES exposure - many have abnormal uterine structure (T shaped uterus+/-cervical changes)-24 % Acquired Uterine Leiomyomas Intrauterine Adhesions(Asherman’s Syndrome) Incompetent cervix

ANATOMIC FACTORSUTERINE FACTORS Acquired or congenital anomalies Congenital uterine anomalies: 6 - 7 % in women with RPL vs. 2 % in all women. Pathogenesis uncertain but attributed to : Reduced intrauterine volume Poor vascular supply




GENETIC FACTORS Repetitive first trimester losses Anembryonic pregnancies History of malformations or mental retardation Advanced maternal age Genetic etiology less likely with late first trimester or second trimester losses

Genetic factors Parental Chromosomal abnormalities • One of the partner carries a balanced structural • chromosomal anomaly Most common is balanced reciprocal and Robertsonian translocation which causes unbalanced translocation in the fetus Embryonic Chromosomal abnormalities- • Due to abnormalities in the egg, sperm or both. Most common- Monosomy or trisomy Mainly responsible for sporadic miscarriage

Risk factors for recurrent abortions Maternal age- associated with a decline in both the number and quality of the remaining oocyte Previous miscarriages- risk increases with each successive pregnancy loss, 40% after 3 consecutive pregnancy losses Obesity-increases risk of both sporadic and recurrent miscarriage Environmental factors-Cigarette smoking, caffeine and alcohol consumption,

MANAGEMENT Genetic counselling Assisted reproductive technologies, including PGD (preimplantation genetic diagnosis) Use of either donor oocyte or donor sperm depending on the affected partner

UTERINE ASSESSMENT Sonohysterography (SIS) More accurate than HSG Differentiate septate & bicornuate uterus Hysterosalpingogram Does not evaluate outer contour Not ideal for the cavity (HSG) Hysteroscopy Gold standard for Dx + Rx intrauterine lesions

Ultrasound Presence and location of uterine myomas Associated renal abnormalities MRI Differentiate septate from bicornuate


Treatment for uterine abnormalities in RPL l Whether hysteroscopic septum resection has beneficial effects (improving live birth rates, and decreasing miscarriage rates, without doing harm), should be evaluated in the context of surgical trials in women with RPL and septate uterus. l Metroplasty is not recommended for bicorporeal uterus with normal cervix (former AFS bicornuate uterus) and RPL.

UNICORNUATE UTERUS • No surgical procedure can enlarge unicornuate uterus • Available evidence suggests most pregnancies best managed expectantly with cervical cerclage reserved for those with previous second trimester pregnancy losses or evidence of progressive cervical shortening
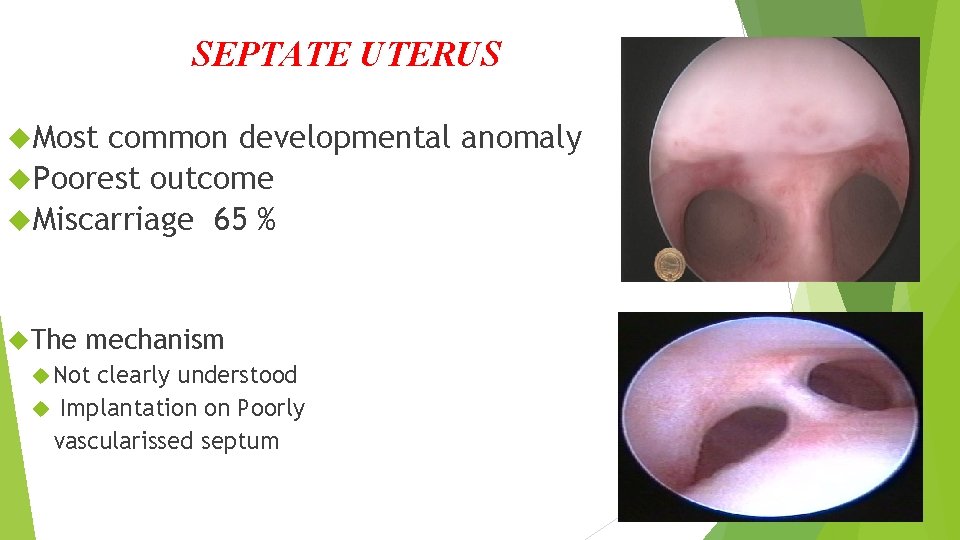
SEPTATE UTERUS Most common developmental anomaly Poorest outcome Miscarriage 65 % The mechanism Not clearly understood Implantation on Poorly vascularissed septum

Uterine septa not always associated with a poor pregnancy outcome but their presence in a woman with RPL is an indication for surgical correction (Hysteroscopic septoplasty, usually only incision required)

UTERUS DIDELPHYS Only surgery indicated is removal of an obstructing longitudinal vaginal septum Unification procedures can benefit some women with numerous miscarriages or previable births The recommended technique unifies the two fundi and leaves the two cervices intact

BICORNUATE UTERUS Surgery generally considered unnecessary and best reserved for those with a well established history of otherwise unexplained recurrent pregnancy loss or previable births Strassman abdominal metroplasty surgical procedure of choice

Uterine leiomyoma Unclear relationship between uterine leiomyomata and RPL • Pregnancy outcomes adversely affected by submucous myoma, not by subserosal or intramural myomas under 5 -7 cm in size • Large submucosal fibroids distort the cavity or occupy a large subendometial area

Surgery not indicated when myomas do not distort the uterine cavity or when specific symptoms are not attributable to them Treatment options: Hysteroscopic/Abdominal myomectomy, subtotal hysteroscopic myomectomy

• There is insufficient evidence supporting hysteroscopic removal of submucosal fibroids or endometrial polyps in women with RPL. • Surgical removal of intramural fibroids is not recommended in women with RPL. There is insufficient evidence to recommend removing fibroids that distort the uterine cavity.

INTRAUTERINE ADHESION /ASHERMAN’SYNDROME/AMENORRHOEA TRAUMATICA Excessive curettage for pregnancy complications Traumatize basalis layer granulation tissue Insufficient endometrium to support fetoplacenta growth Menstrual irregularities (hypomenorrhea, amenorrhea), cyclic pelvic pain, infertility.

Diagnosis primarily on high index of suspicion, based on history Scanty or no withdrawl bleeding after sequential treatment with exogenous estrogen and progestin Operative Most hysteroscopy primary method of treatment advocate insertion of an intrauterine balloon catheter (left in place for approx 7 -10 days) after adhesiolysis

Treatment with broad spectrum antibiotic and a non-steroidal anti inflammatory drug minimize the risk of infection and uterine cramping while catheter is in place High dose exogenous estrogen for approx 4 weeks after surgery encourage rapid endometrial re-epithelialization and proliferation with a progestin in the final week Recurrence rates 20 -60%

Cerclage l In women with a singleton pregnancy and a history of recurrent second-trimester PL attributable to cervical weakness, a cerclage could be considered. l There is no evidence that this treatment increases perinatal survival.

SURGICAL TREATMENT Shirodkar operation Mc. Donald operation Abdominal pessary cerclage

Circlage Operation Principle A non absorbable encircling suture is placed around the cervix at the level of internal os Operates by interfering with the uterine polarity and the adjacent lower segment from being taken up. Timing of operation Elective cerclage-In proven cases around 14 weeks or at least 2 weeks earlier than the lowest period of previous wastage as early as 10 th week. Emergency cerclage- when the cervix is dilated and the membranes are bulging.

Contraindications for cerclage Intrauterine Ruptured infections membranes History of vaginal bleeding Severe uterine irritability Cervical dilatation >4 cm

Cerclage operation Shirodkar operation- opening the anterior fornix and dissecting away the adjacent bladder before placing the suture submucosaly, tied interiorly and the knot buried by suturing the anterior fornix mucosal opening Mac Donald technique- requires no bladder dissection and the cervix is closed by purse string sutures around the cervix

Complications Slipping or cutting through the suture Chorioamniotis Rupture of the membrane Abortion /Preterm labour

Post operative advice Bed rest Tocolysis To avoid intercourse Report in case of leaking, bleeding, and pain Stitch should be removed at 38 weeks or earlier when the labour starts

Endometrial polyps • Endometrial polyps are found in women with RPL, but there is no clear evidence of an association with pregnancy loss. • Although there are no adequate studies showing benefit for polypectomy in RPL, hysteroscopic removal can be considered for larger polyps (>1 cm) in women with RPL without any other known cause.

Hypothyroidism Associated with isolated as well as RPL l Patients with hypothyroidism even subclinical have an increased rate of spontaneous miscarriage l Subjects have concomitant reproductive abnormalities including ovulatory dysfunction and luteal phase defect l Association between antithyroid antibody positivity and RPL unclear

Hypothyroidism • Overt hypothyroidism arising before conception or during early gestation should be treated with levothyroxine in women with RPL.

Hypothyroidism l There is conflicting evidence regarding treatment effect of levothyroxine for women with subclinical hypothyroidism and RPL. l Treatment of women with SCH may reduce the risk of miscarriage, but the potential benefit of treatment should be balanced against the risks.

l If women with subclinical hypothyroidism and RPL are pregnant again, TSH level should be checked in early gestation (7 -9 weeks AD), and hypothyroidism should be treated with levothyroxine. l If women with thyroid autoimmunity and RPL are pregnant again, TSH level should be checked in early gestation (79 weeks AD), and hypothyroidism should be treated with levothyroxine.

levothyroxine in euthyroid women • There is insufficient evidence to support treatment with levothyroxine in euthyroid women with thyroid antibodies and RPL outside a clinical trial.

Polycystic Ovarian Syndrome Characterized by excessive production of androgens by the ovaries which interferes with the reproductive, endocrine, and metabolic functions. Woman presents with oligo/anovulation, Hyperandrogenism, and polycystic ovaries on ultrasound Increaaased risk of miscarriage in PCOS is due to insulin resistance, hyperinsulinaemia, and hyperandrogenemia Metformin treatment can reduce the risk of miscarriage in PCOS woman

Metformin There is insufficient evidence to recommend metformin supplementation in pregnancy to prevent PL in women with RPL and glucose metabolism defects.

Role of progesterone in recurrent abortions There is insufficient evidence to evaluate the effect of progesterone supplementation in pregnancy to prevent a miscarriage Progesterone is responsbile for the immune cascade of pregnancy and is called immunomodulater Therefore in the absence of any factor , progesterone is given till the placenta takes over the luteal functional Type of progesterone- natural micronized progesterone/dyhydrogesterone Route-oral/vaginal/intramuscular Dose-600 -800 mg per day vaginally or orally

Autoimmune Systemic lupus erythematosus - Risk for loss is 20%, mostly in 2 nd and 3 rd trimester of pregnancy and associated with antiphospholipid antibodies Antiphospholipid syndrome (APA) -5%of women with RPL may have APA induces microthrombi at placentation site. Altered vascularity affects developing embryo and induces abortion

APLA/APS-Treatment 1. Unfractionated Heparin 5000 -10000 IU subcutaneous twice a day Or Low molecular weight Heparin is better option + 2. Low dose Aspirin (75 -85 mg/day)

When to start treatment Heparin with low dose aspirin is preferred regime. Aspirin is started when pregnancy is being attempted or documented. Heparin TVS. is started as soon as cardiac activity is documented on

Sperm selection is not recommended as a treatment in couples with RPL

Antioxidants for men have not been shown to improve the chance of a live birth.

Treatment for unexplained RPL Lymphocyte immunization therapy should not be used as treatment for unexplained RPL as it has no significant effect and there may be serious adverse effects. Intravenous immunoglobulin (Iv. Ig) is not recommended as a treatment of RPL. Glucocorticoids are not recommended as a treatment of unexplained RPL or RPL with selected immunological biomarkers. Heparin or low dose aspirin are not recommended, as there is evidence that they do not improve live birth rate in women with unexplained RPL. Vaginal progesterone does not improve live birth rates in women with unexplained RPL

Low dose folic acid is routinely started preconceptionally to prevent neural tube defects, but it has not been shown to prevent pregnancy loss in women with unexplained RPL.

There is no evidence to recommended endometrial scratching in women with unexplained RPL If women with RPL ask about using multivitamin supplements, they should be advised on multivitamin supplements that are safe in pregnancy.

Management of Patient with Idiopathic Recurrent abortions Preconception. Counselling of the couple -after 3 consecutive miscarriages chance of a successful pregnancy is high(70%) 1. Folic acid 2. Correct 3. Empiric 4. Luteal 5. nutritional deficiencies antibiotics support Natural progesterone

Management of Patient with Idiopathic Recurrent abortions Post conception : 1. 2. 3. 4. 5. 6. Reassurance and Tender loving Care (TLC) Prophylactic aspirin Prophylactic cervical circlage If history of repeated D & E Anticardiolipin antibodies [ Ig. M ] Steroids for pulmonary maturity Monitor closely near term [ NST, USG ]

Any Question? Thanks

Thank you
- Slides: 63