Definitions Digestion Breakdown of ingested nutrients into forms

Definitions Digestion: Breakdown of ingested nutrients into forms which can be absorbed Absorption: Transport of small molecules from the GI tract into the blood Motility: Patterns of GI contraction and relaxation; tone of sphincters Secretion: Control of secretion of digestive enzymes & regulatory hormones 1
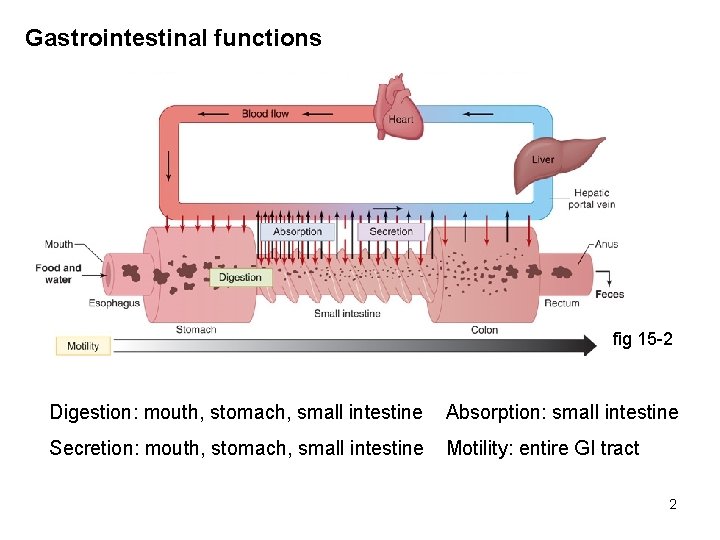
Gastrointestinal functions fig 15 -2 Digestion: mouth, stomach, small intestine Absorption: small intestine Secretion: mouth, stomach, small intestine Motility: entire GI tract 2
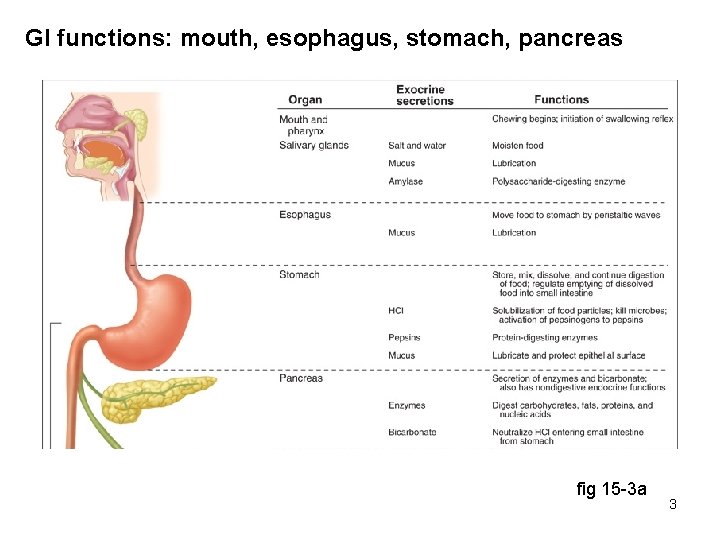
GI functions: mouth, esophagus, stomach, pancreas fig 15 -3 a 3
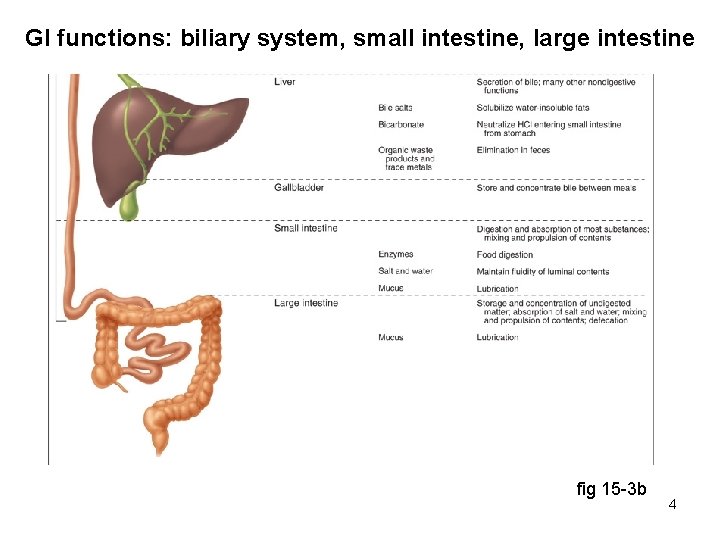
GI functions: biliary system, small intestine, large intestine fig 15 -3 b 4
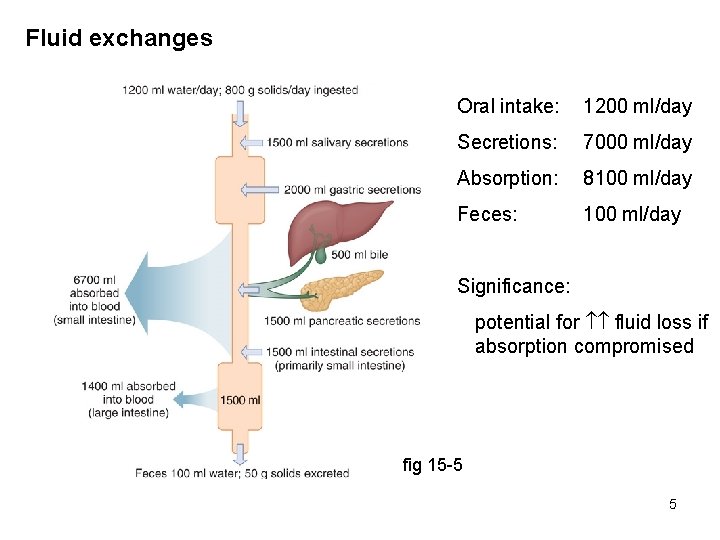
Fluid exchanges Oral intake: 1200 ml/day Secretions: 7000 ml/day Absorption: 8100 ml/day Feces: 100 ml/day Significance: potential for fluid loss if absorption compromised fig 15 -5 5
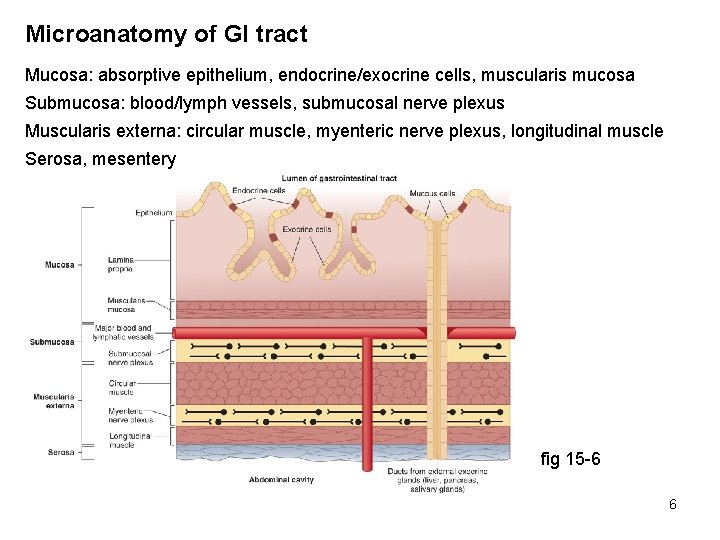
Microanatomy of GI tract Mucosa: absorptive epithelium, endocrine/exocrine cells, muscularis mucosa Submucosa: blood/lymph vessels, submucosal nerve plexus Muscularis externa: circular muscle, myenteric nerve plexus, longitudinal muscle Serosa, mesentery fig 15 -6 6
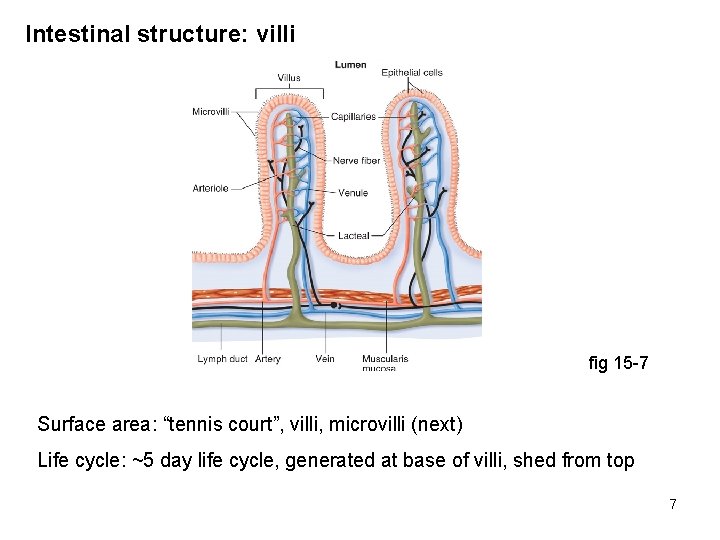
Intestinal structure: villi fig 15 -7 Surface area: “tennis court”, villi, microvilli (next) Life cycle: ~5 day life cycle, generated at base of villi, shed from top 7
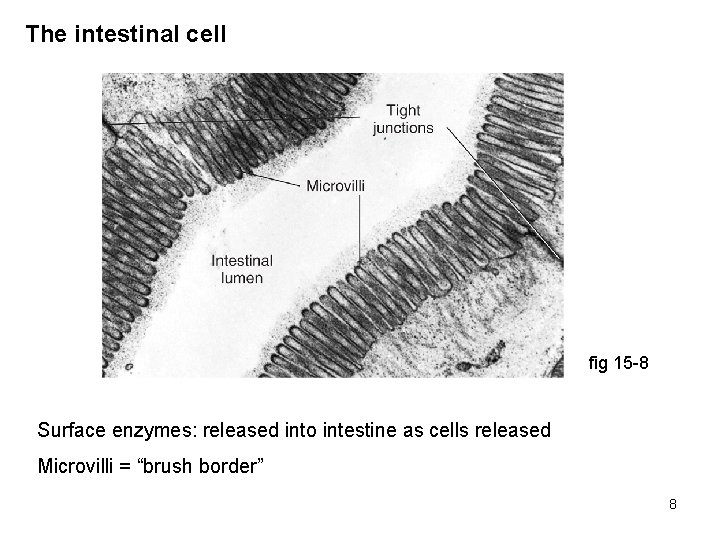
The intestinal cell fig 15 -8 Surface enzymes: released into intestine as cells released Microvilli = “brush border” 8

Carbohydrate digestion & absorption Source: ~ half of daily caloric intake ~ 70% as starch (potatoes, pasta, rice, bread), ~ 30% as sucrose, lactose cellulose: glucose links not digestible, forms “bulk” of diet Starch: 1 4, 1 6 links hydrolyzed by salivary & pancreatic amylase maltose, maltotriose Intestinal disaccharidases: maltase: hydrolyses maltose, maltotriose glucose sucrase: hydrolyses sucrose glucose + fructose lactase: hydrolyses lactose glucose + galactose Absorption: from small intestine into blood capillaries Glucose, galactose by Na+ linked cotransport at luminal border Fructose by facilitated diffusion at luminal border Glucose, galactose, fructose by facilitated diffusion at basolateral surface 9

Protein digestion & absorption Source: ~ 20% of daily caloric intake Digestion: gastric *pepsin (endopeptidase, acid p. H optimum) pancreatic *trypsin & *chymotrypsin (endopeptidase, alkaline p. H optimum) pancreatic carboxypeptidase (exopeptidase) intestinal aminopeptidase (exopeptidase) Absorption: small intestine, into blood capillaries aminoacids by Na+ linked cotransport, di- & tri-peptides by H+ linked cotransport at luminal border peptides hydrolyzed in intestinal cell aminoacids by facilitated diffusion at basolateral membrane * secreted as inactive precursor (next slide) 10
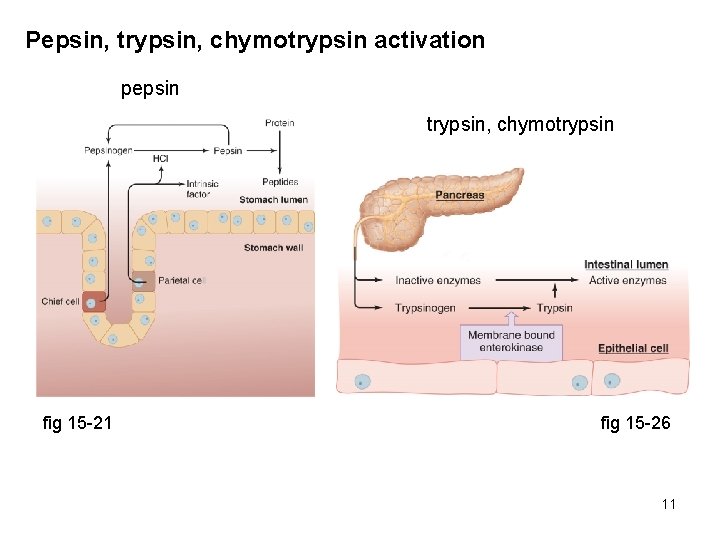
Pepsin, trypsin, chymotrypsin activation pepsin trypsin, chymotrypsin fig 15 -21 fig 15 -26 11

Lipid digestion & absorption Source: Triglyceride, ~30% of daily caloric intake Digestion: pancreatic lipase (triglyceride 2 -monoglyceride + 2 fatty acids) lipases act at fat water interfaces & depend on fat surface area Emulsification: mechanical disruption (chewing, motility of stomach & small intestine amphipathic emulsifiers (bile salts, bile phospholipid) 12
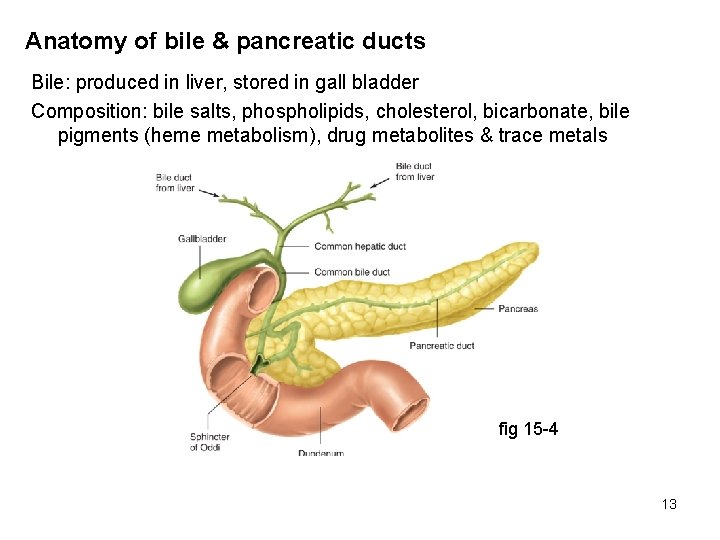
Anatomy of bile & pancreatic ducts Bile: produced in liver, stored in gall bladder Composition: bile salts, phospholipids, cholesterol, bicarbonate, bile pigments (heme metabolism), drug metabolites & trace metals fig 15 -4 13
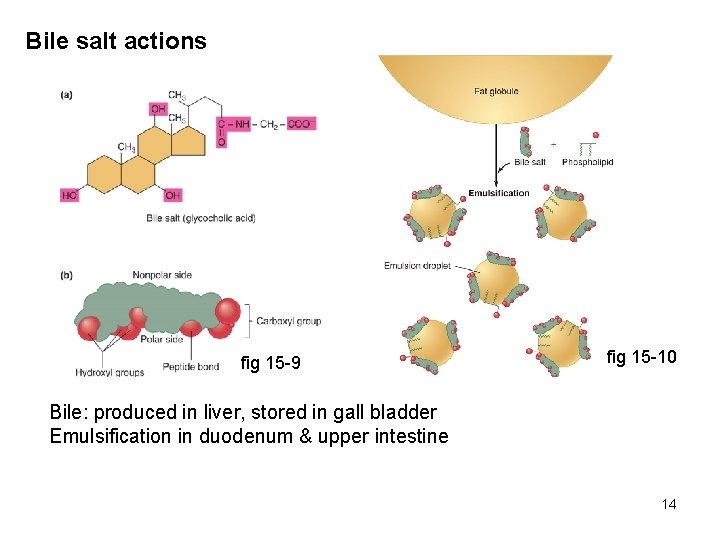
Bile salt actions fig 15 -9 fig 15 -10 Bile: produced in liver, stored in gall bladder Emulsification in duodenum & upper intestine 14
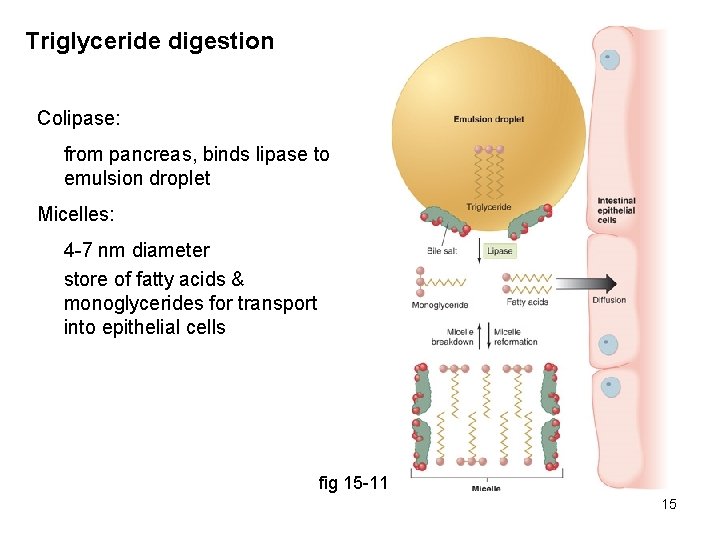
Triglyceride digestion Colipase: from pancreas, binds lipase to emulsion droplet Micelles: 4 -7 nm diameter store of fatty acids & monoglycerides for transport into epithelial cells fig 15 -11 15
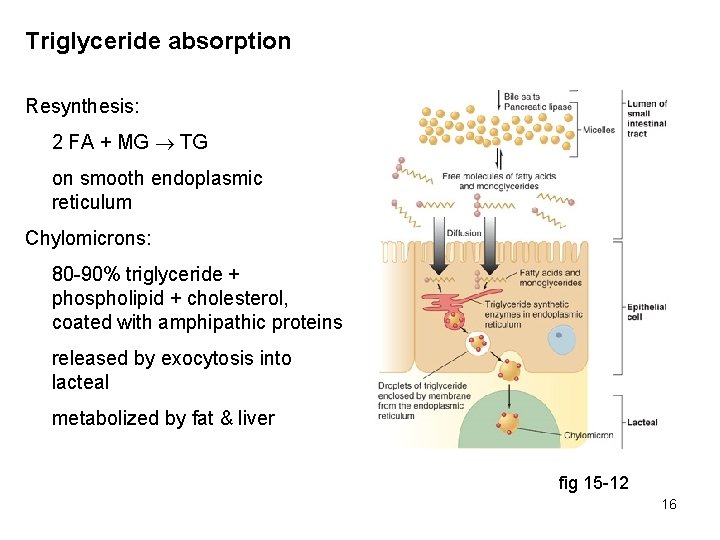
Triglyceride absorption Resynthesis: 2 FA + MG TG on smooth endoplasmic reticulum Chylomicrons: 80 -90% triglyceride + phospholipid + cholesterol, coated with amphipathic proteins released by exocytosis into lacteal metabolized by fat & liver fig 15 -12 16

Vitamins, water absorption Water: passively absorbed down osmotic gradient GI wall permeable, therefore GI contents isosmotic mostly from small intestine Vitamins: lipid soluble (vit A, D, E, K) with lipids (micelles, diffusion, chylomicrons) water soluble (vit B, vit C) diffusion, mediated transport vit B 12 with intrinsic factor (from stomach parietal cells), endocytosis 17

Regulation of secretion: general Luminal stimuli: 1. distension of wall (volume stimulates mechanoreceptors) 2. osmolality of chyme (osmoreceptors) 3. acidity of chyme (chemoreceptors) 4. chyme concentration of digestive products: monosaccharides, fatty acids, peptides, aminoacids (chemoreceptors) 18
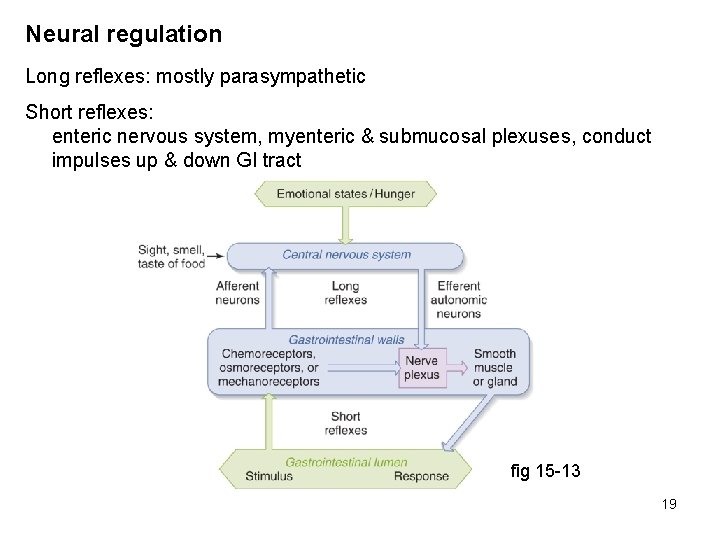
Neural regulation Long reflexes: mostly parasympathetic Short reflexes: enteric nervous system, myenteric & submucosal plexuses, conduct impulses up & down GI tract fig 15 -13 19
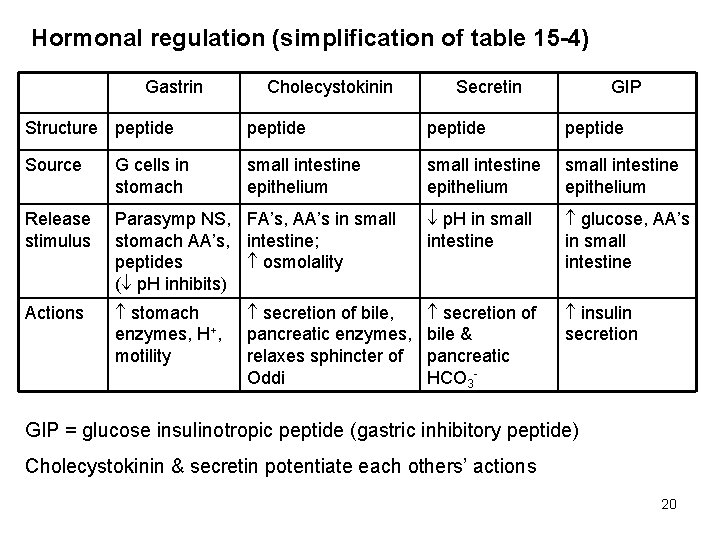
Hormonal regulation (simplification of table 15 -4) Gastrin Cholecystokinin Secretin GIP Structure peptide Source G cells in stomach small intestine epithelium Release stimulus Parasymp NS, FA’s, AA’s in small stomach AA’s, intestine; peptides osmolality ( p. H inhibits) p. H in small intestine glucose, AA’s in small intestine Actions stomach enzymes, H+, motility secretion of bile & pancreatic HCO 3 - insulin secretion of bile, pancreatic enzymes, relaxes sphincter of Oddi GIP = glucose insulinotropic peptide (gastric inhibitory peptide) Cholecystokinin & secretin potentiate each others’ actions 20

Saliva Composition: fluid, mucus, amylase Functions: moistening food, preventing tooth decay (lysozyme, Ig. A), starting starch digestion Regulation of release: parasympathetic NS (responding to sight, smell, thought of food) sympathetic NS (transient); ( saliva flow, blood flow) acidic fruit juices, mechanical contact 21
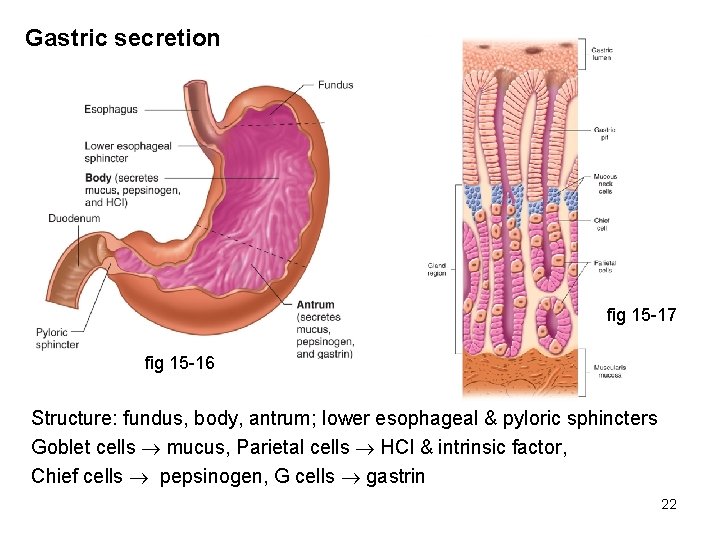
Gastric secretion fig 15 -17 fig 15 -16 Structure: fundus, body, antrum; lower esophageal & pyloric sphincters Goblet cells mucus, Parietal cells HCl & intrinsic factor, Chief cells pepsinogen, G cells gastrin 22
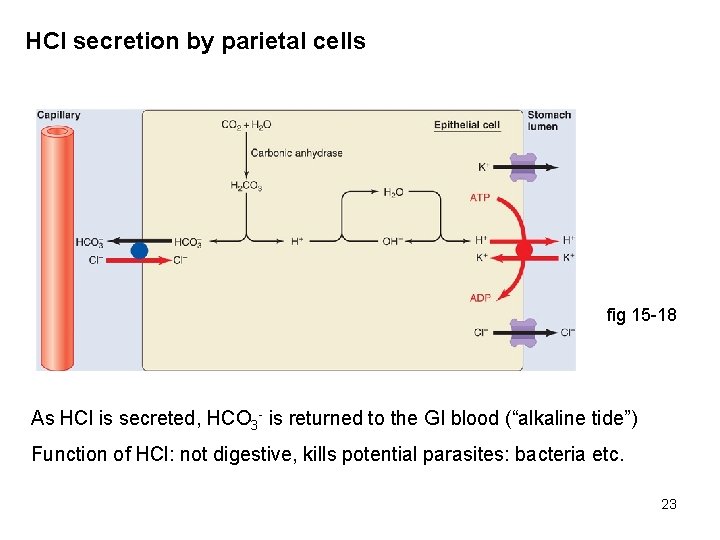
HCl secretion by parietal cells fig 15 -18 As HCl is secreted, HCO 3 - is returned to the GI blood (“alkaline tide”) Function of HCl: not digestive, kills potential parasites: bacteria etc. 23
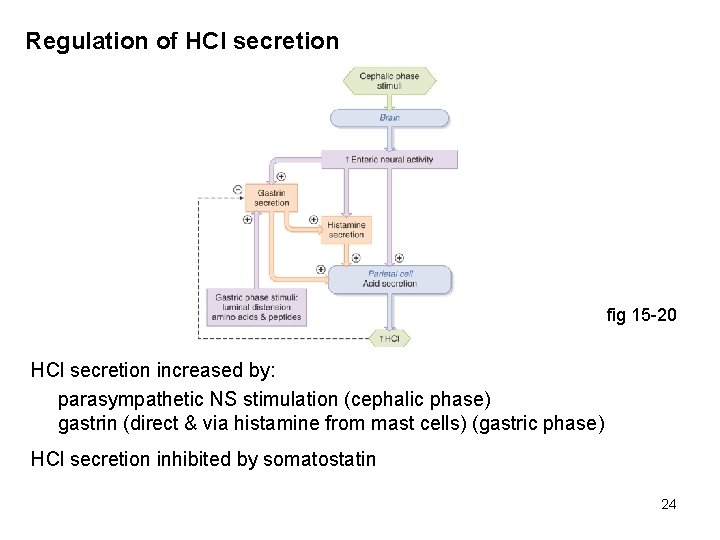
Regulation of HCl secretion fig 15 -20 HCl secretion increased by: parasympathetic NS stimulation (cephalic phase) gastrin (direct & via histamine from mast cells) (gastric phase) HCl secretion inhibited by somatostatin 24

Phases of gastric secretion of pepsinogen & HCl Cephalic phase: stimulus: sight, smell, thought of food, chewing mechanism: parasympathetic NS secretion & motility Gastric phase: stimulus: aminoacids, peptides in stomach, distension, p. H as food enters mechanism: short/long loop reflexes, gastrin secretion & motility Intestinal phase: stimulus: intestinal distension, p. H, osmolality, digestive products mechanism: short/long loop reflexes, secretin, CCK, GIP 25
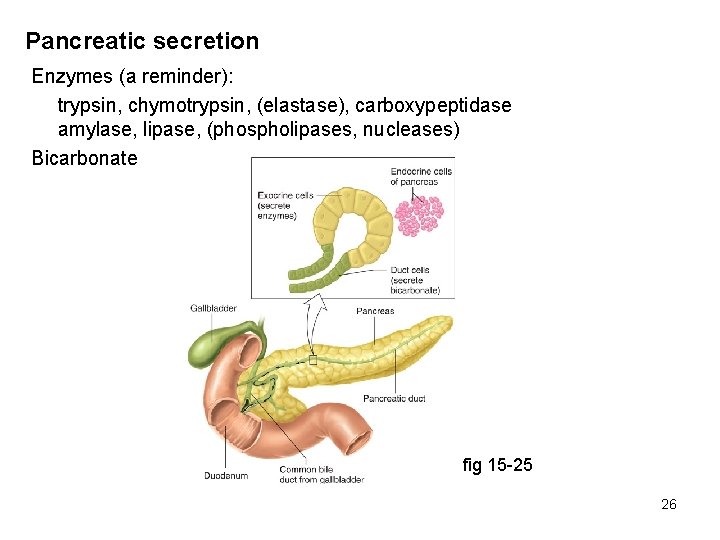
Pancreatic secretion Enzymes (a reminder): trypsin, chymotrypsin, (elastase), carboxypeptidase amylase, lipase, (phospholipases, nucleases) Bicarbonate fig 15 -25 26

Regulation of pancreatic secretion Stimulus: fatty acids, glucose, osmolality, distension in small intestine Mediator: cholecystokinin Response: relaxation of sphincter of Oddi, contraction of gall bladder secretion of pancreatic enzymes, potentiation of secretin actions Stimulus: p. H in small intestine Mediator: secretin Response: secretion of bicarbonate in pancreatic juice & bile Stimulus: glucose in small intestine Mediator: glucose insulinotropic peptide (GIP) Response: secretion of insulin, inhibition of gastric secretion 27
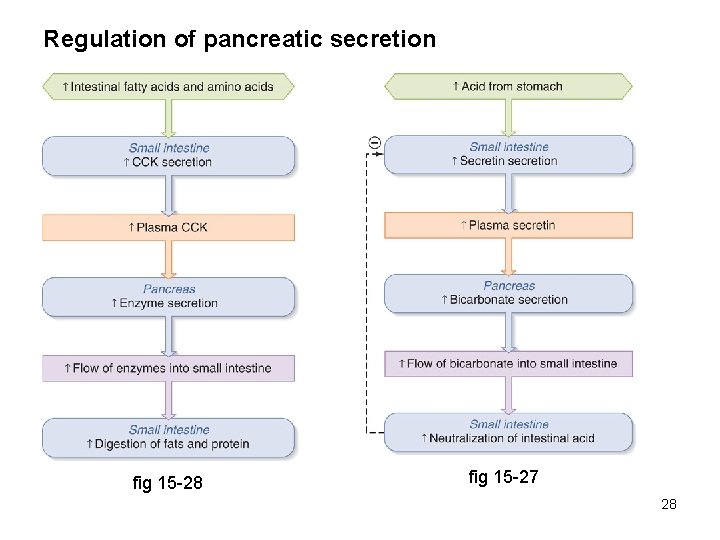
Regulation of pancreatic secretion fig 15 -28 fig 15 -27 28

Bile Source: produced in liver, stored & concentrated in the gall bladder Composition: bile salts, phospholipids, cholesterol (emulsify fats) bicarbonate (neutralizes HCl) bile pigments (heme metabolism), drug metabolites & trace metals Regulation of secretion: intestinal fatty acids cholecystokinin gall bladder contraction Enterohepatic circulation: next screen 29
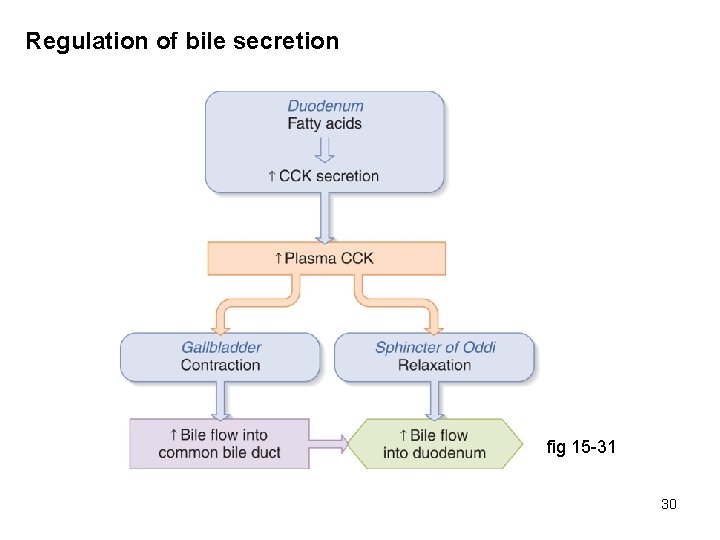
Regulation of bile secretion fig 15 -31 30
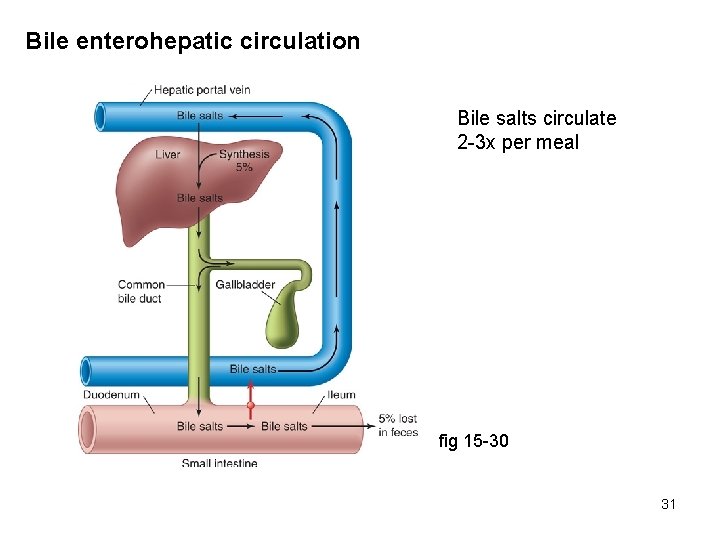
Bile enterohepatic circulation Bile salts circulate 2 -3 x per meal fig 15 -30 31

Gastrointestinal motility omitted Omit objectives 16 -20 32

Liver functions 1. exocrine function: bile salts, bicarbonate 2. plasma proteins: albumin, binding proteins, angiotensinogen 3. metabolism: gluconeogenesis, urea, ketoacids, lipoproteins 4. cholesterol synthesis, secretion in bile 5. excretion: bile pigments, trace metals, drug metabolites 33
- Slides: 33