Definition of flu Definition might be different according




Definition of flu • Definition might be different according to Flu alert status • Classic definition: 1)Fever 2)Cough or sore throat 3) One of the following items: • malaise( ill appearance? ) • Neck pain (calf tenderness? ) (muscle pain) • Shivering • Mucosal irritation • Hx of contact to suspicious flu case • Definition during pandemic: Illness with both of the following: 1)T>38 c 2)cough, sore throat, or dyspnea

Transmission • Human influenza is transmitted by inhalation of infectious droplets and droplet nuclei, by direct contact, and perhaps, by indirect (fomite) contact, with self-inoculation onto the upper respiratory tract or conjunctival mucosa • Evidence is consistent with bird-to-human, possibly environment-to-human, and limited, nonsustained human-to-human transmission

• No significant risk related to eating or preparing poultry products or exposure to persons with influenza A (H 5 N 1) disease • Exposure to ill poultry and butchering of birds were associated with seropositivity for influenza A (H 5 N 1). • Most patients have had a history of direct contact with poultry, although not those who were involved in mass culling of poultry

Potential Modes: • Oral ingestion of contaminated water during swimming and direct intranasal or conjunctival inoculation during exposure to water • Contamination of hands from infected fomites and subsequent self-inoculation

How do humans get “bird flu” ? l l l Through close contact with infected birds e. g. breathing in particles from their droppings Rare for bird flu to infect humans Limited evidence of human-tohuman transmission to date according to WHO


پﺎﻧﺪﻣیﻬﺎی ﺟﻬﺎﻧی آﻨﻔﻠﻮآﻨﺰﺍ ﺩﺭ ﻗﺮﻥ ﺑیﺴﺘﻢ Credit: US National Museum of Health and Medicine 1918: 1957: 1968: “Spanish Flu” “Asian Flu” “Hong Kong Flu” 20 - 40 million deaths A(H 1 N 1) 1 - 4 million deaths A(H 2 N 2) 1 - 4 million deaths A(H 3 N 2)
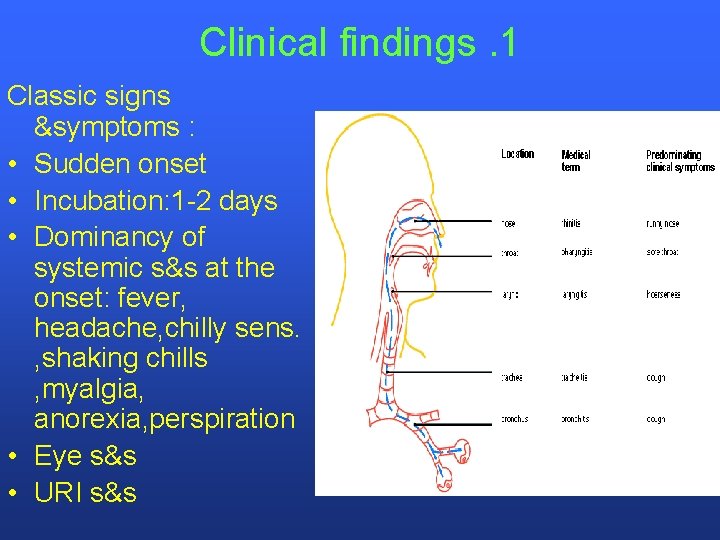
Clinical findings. 1 Classic signs &symptoms : • Sudden onset • Incubation: 1 -2 days • Dominancy of systemic s&s at the onset: fever, headache, chilly sens. , shaking chills , myalgia, anorexia, perspiration • Eye s&s • URI s&s

Clinical findings. 2 Uncomplicated course: • Persistence of systemic s&S FOR 3 DAYS • Cough become more prominent & can continue for a few days after stopping the fever • A few wks convalescence

Differences of findings in pediatric age group More common features in pediatric patients: • More sudden onset • Anorexia • Abd. Pain & GI s&s • Very high fever • Cervical LNP • Specially in younger kids: non obvious respiratory s&s • Newborn period: like sepsis • Febrile convulsion
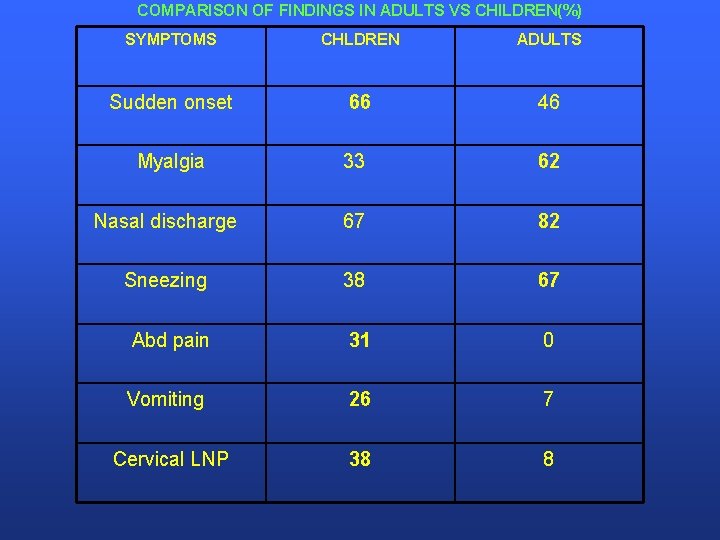
COMPARISON OF FINDINGS IN ADULTS VS CHILDREN(%) SYMPTOMS CHLDREN ADULTS Sudden onset 66 46 Myalgia 33 62 Nasal discharge 67 82 Sneezing 38 67 Abd pain 31 0 Vomiting 26 7 Cervical LNP 38 8

Animals and Highly Pathogenic Avian Influenza

Clinical Signs • • Incubation period: 3 -14 days Birds found dead Drop in egg production Neurological signs Depression, anorexia, ruffled feathers Combs swollen, cyanotic Conjunctivitis and respiratory signs

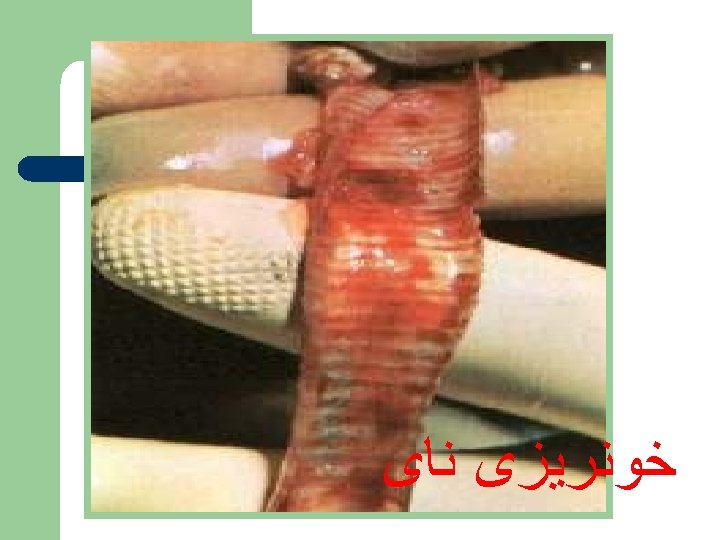
Post Mortem Lesions may be absent with sudden death • Severe congestion of the musculature • Dehydration • Subcutaneous edema of head and neck area •
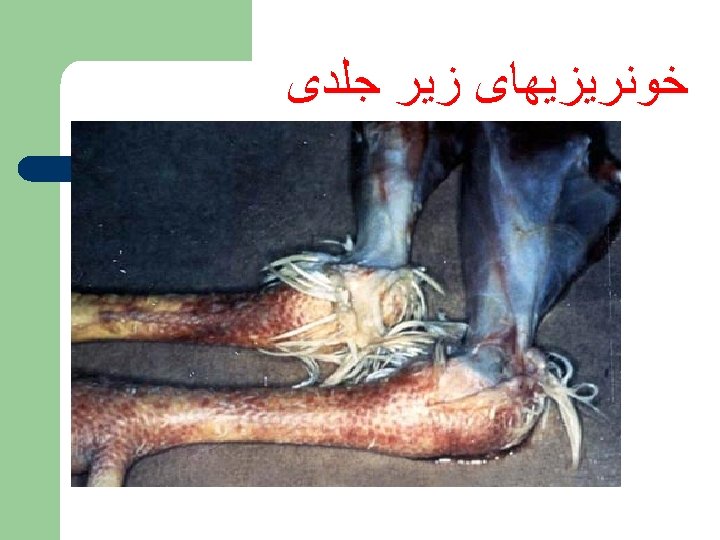
Post Mortem Lesions Nasal and oral cavity discharge • Petechiae on serosal surfaces • Kidneys severely congested • Severe congestion of the conjunctivae •



Differential Diagnosis • • Virulent Newcastle disease Avian pneumovirus Infectious laryngotracheitis Infectious bronchitis Chlamydia Mycoplasma Acute bacterial diseases − Fowl cholera, E. coli infection

Diagnosis Clinically indistinguishable from virulent Newcastle Disease • Suspect with: • − Sudden death − Drop in egg production − Facial edema, cyanotic combs and wattles − Petechial hemorrhages • Virology and serology necessary for definitive diagnoses

Diagnosis • Laboratory Tests − HP AI is usually diagnosed by virus isolation • Presence of virus confirmed by − AGID − ELISA − RT-PCR • Serology may be helpful

Avian Influenza in Humans

Avian Flu 1)Fever & 2)at least one of the following items: n Sore throat n Headache n Conjunctivitis n Dyspnea & 3)At least one of the following epidemiologic clues: n Hx of contact to dead bird during preceding 10 days n Hx of contact to confirmed human case of avian flu, during preceding 10 days n Hx of contact to suspicious environmental area during preceding 10 days n Hx of occupational contact in the lab during preceding 10 days n Positive inf A virus detection without knowing it’s subtype

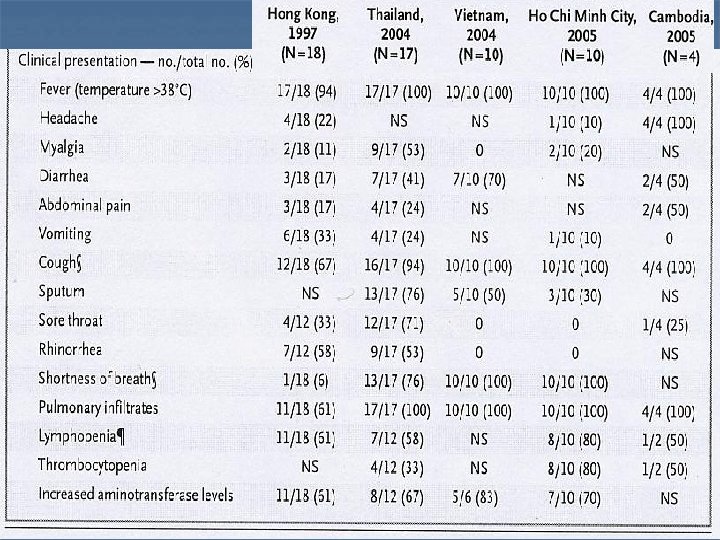
Initial symptoms v n n n n High fever >38. c Headache Myalgia Watery diarrhea Abdominal pain Vomiting Cough Sputum Sore throat Bleeding nose and gums Rhinorrhea Shortness of breath Conjunctivitis(Rarely)
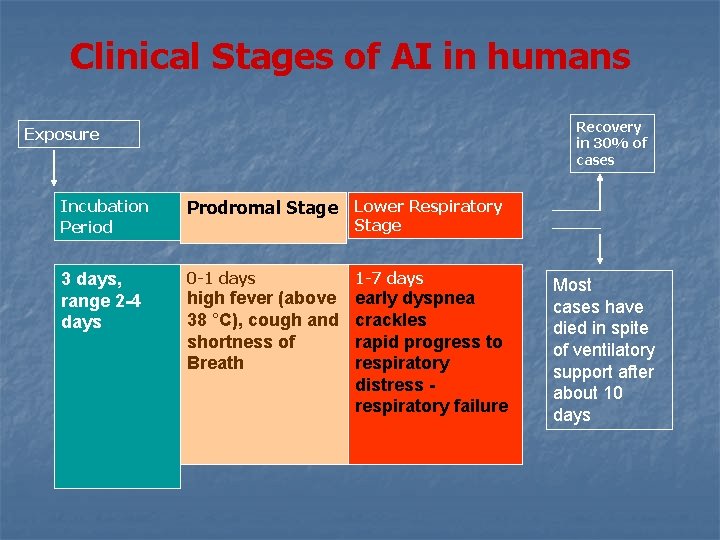
Clinical Stages of AI in humans Recovery in 30% of cases Exposure Incubation Period Prodromal Stage Lower Respiratory 3 days, range 2 -4 days 0 -1 days 1 -7 days high fever (above 38 °C), cough and shortness of Breath early dyspnea crackles rapid progress to respiratory distress respiratory failure Stage Most cases have died in spite of ventilatory support after about 10 days

Avian flu characteristics. 1 n n Lower respiratory tract manifestations n dyspnea n Respiratory distress, tachypnea, and inspiratory crackles are common. Radiographic changes include diffuse, multifocal, or patchy infiltrates; interstitial infiltrates; and segmental or lobular consolidation with air bronchograms. Radiographic abnormalities were present a median of 7 days after the onset of fever in one study Pleural effusions are uncommon. primary viral pneumonia, usually without bacterial super infection

Avian flu characteristics: 2 n n Progression to respiratory failure Manifestations of the acute respiratory distress syndrome (ARDS) Multiorgan failure with signs of renal dysfunction Ventilator-associated pneumonia, pulmonary hemorrhage, pneumothorax, pancytopenia, Reye's syndrome, and sepsis syndrome without documented bacteremia.

Mortality in avian flu n n n The fatality rate among hospitalized patients has been high The overall rate is probably much lower in patients older than 13 years of age The case fatality rate was 89 percent among those younger than 15 years of age in Thailand. Death has occurred an average of 9 or 10 days after the onset of illness. Most patients have died of progressive respiratory failure

Laboratory findings 1. leukopenia particulary lymphopenia 2. mild –to-moderate thrombocytopenia 3. mild-to-moderate elevated Aminotransferase levels

Some laboratory Findings in avian flu n n n Marked hyperglycemia Elevated creatinine levels Death was associated with decreased leukocyte, platelet, and particularly, lymphocyte counts at the time of admission.

Radiographic changes : n Diffuse , multifocal , or patchy infiltrates interstitial infiltrates and segmental or lobular consolidation with air bronchograms n Pleural effusions are uncommon
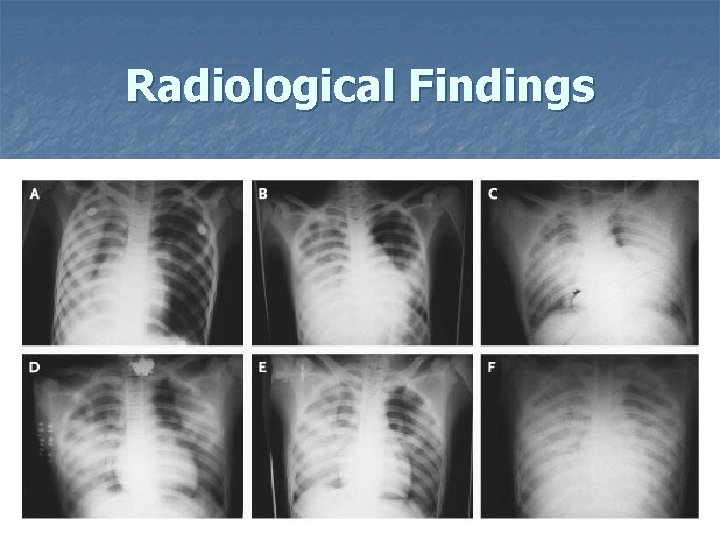
Radiological Findings

Virologic diagnosis 1. Viral isolation(pharyngeal>nasal) 2. RT – PCR 3. Rapid antigen test

When do you suspect to flu in a case? Very important key findings: n Characteristics of fever n Toxic appearance at presentation+/n Body pain+/n Avian flu has many clinical similarities but the key point is the epidemiologic evidences

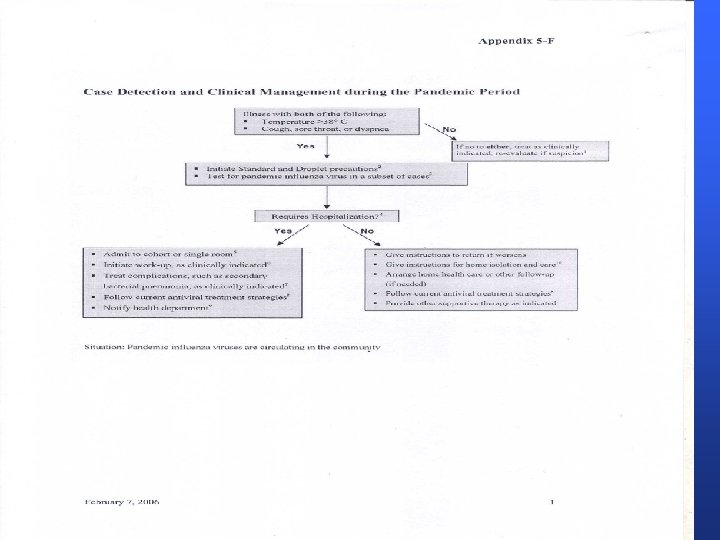
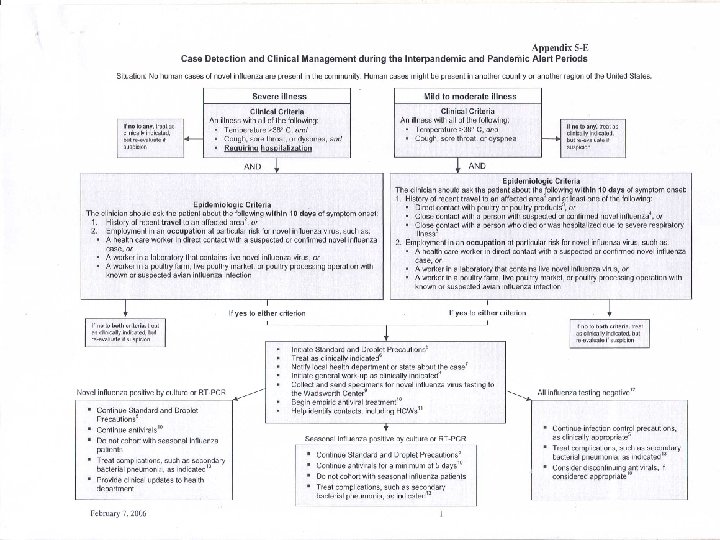
CASE DEFINITIONS n Person under investigation A person whom public health authorities have decided to investigate for possible H 5 N 1 infection. n Suspected H 5 N 1 case A person presenting with unexplained acute lower respiratory illness with fever (>38 ºC ) and cough, shortness of breath or difficulty breathing. AND One or more of the following exposures in the 7 days prior to symptom onset: a. Close contact (within 1 meter) with a person (e. g. caring for, speaking with, or touching) who is a suspected, probable, or confirmed H 5 N 1 case; b. Exposure (e. g. handling, slaughtering, defeathering, butchering, preparation for consumption) to poultry or wild birds or their remains or to environments contaminated by their faeces in an area where H 5 N 1 infections in animals or humans have been suspected or confirmed in the last month; c. Consumption of raw or undercooked poultry products in an area where H 5 N 1 infections in animals or humans have been suspected or confirmed in the last month; d. Close contact with a confirmed H 5 N 1 infected animal other than poultry or wild birds (e. g. cat or pig); e. Handling samples (animal or human) suspected of containing H 5 N 1 virus in a laboratory or other setting.

CASE DEFINITIONS n n Probable H 5 N 1 case (notify WHO) Probable definition 1 : A person meeting the criteria for a suspected case AND One of the following additional criteria: a. infiltrates or evidence of an acute pneumonia on chest radiograph plus evidence of respiratory failure (hypoxemia, severe tachypnea) OR n b. positive laboratory confirmation of an influenza A infection but insufficient laboratory evidence for H 5 N 1 infection. Probable definition 2 : A person dying of an unexplained acute respiratory illness who is considered to be epidemiologically linked by time, place, and exposure to a probable or confirmed H 5 N 1 case.

CASE DEFINITIONS n Confirmed H 5 N 1 case (notify WHO) A person meeting the criteria for a suspected or probable case AND One of the following positive results conducted in a national, regional or international influenza laboratory whose H 5 N 1 test results are accepted by WHO as confirmatory: a. Isolation of an H 5 N 1 virus; b. Positive H 5 PCR results from tests using two different PCR targets, e. g. primers specific for influenza A and H 5 HA; c. A fourfold or greater rise in neutralization antibody titer for H 5 N 1 based on testing of an acute serum specimen (collected 7 days or less after symptom onset) and a convalescent serum specimen. The convalescent neutralizing antibody titer must also be 1: 80 or higher; d. A microneutralization antibody titer for H 5 N 1 of 1: 80 or greater in a single serum specimen collected at day 14 or later after symptom onset and a positive result using a different serological assay, for example, a horse red blood cell haemagglutination inhibition titer of 1: 160 or greater or an H 5 specific western blot positive result.


- Slides: 46