Definition IMPLANTS An implant is a biological or
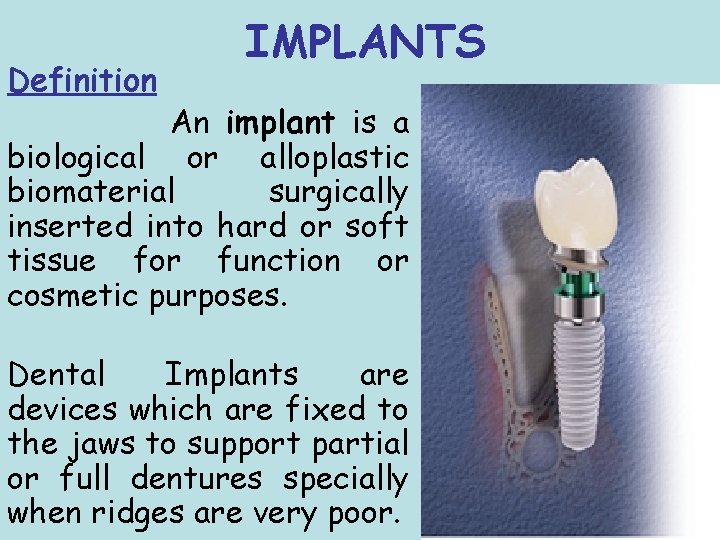
Definition IMPLANTS An implant is a biological or alloplastic biomaterial surgically inserted into hard or soft tissue for function or cosmetic purposes. Dental Implants are devices which are fixed to the jaws to support partial or full dentures specially when ridges are very poor.

It can be accomplished by 2 ways 1. Fibro osseous integration 2. Osteointegration 1. Fibro osseous integration is tissue to implant contact with healthy dense collagenous tissue between the implant and the bone. These collagenous fibers act similar to periodontal ligament.

2. Osteointegration is direct connection between living bone and load bearing endosseous implant at a light microscopic level. Four factors are necessary to achieve this they are 1. Bio compatible material: Titanium and certain calcium phosphate ceramics are biologically inert.

2. An implant precisely adapted to prepared bony site: Gap size between the bone and implant, immediately after implant placement is critical for achievement of osteointegration. Hence gap size is controlled by precise surgical bed into which the implant is placed. Cylindrical preparation are the most predictable one, if made in an accurate shape.

3. Atraumatic surgery to minimize tissue damage: Atraumatic surgery is required to allow minimal mechanical and thermal injury. Sharp, high quality burs which run at low Speed is necessary

4. Immobile or undisturbed healing phase: Areas of jaws that have high percentage of cortical bone such as the anterior mandible are more likely to anchor the implant successfully. Areas of jaws that have high percentage of cancellous bone makes stability for implant more difficult. Hence it is advantageous for initial implant stability if both superior and inferior cortical plates can be used to stabilize the implant.

• The potential problems with the tooth and implant supported fixed partial dentures are – Breakdown of osteointegration – Cement failure on natural abutment – Screw or abutment loosing – Failure of implant prosthetic component.

Classification: Based on their location: Implants are classified into three basic categories : Endosseous Implants (in bone) Subperiosteal Implants (through bone) Transosseous Implants (on bone)

• • According to their body geometry: Threaded or Non threaded (smooth) Porous or non porous Based on Design Screw Cylindrical Hollow Blade

• Based on Material • 3 categories : • Biotolerant (stainless steel, chromium cobalt alloys) • Bioinert (titanium, carbon) • Bioactive (hydroxyl apatite, ceramic oxidized aluminum)

• • • Based on Osseointegration Osseointegrated implant Non Osseointegrated implant Based on Loading Delayed immediate

Subperiosteal implant • It is a framework specifically fabricated to fit on top of supporting areas in mandible or maxilla under the mucoperiostum with perimucosal extension for support and attachment of a prosthesis. • Are implants, which typically lie on top of the jawbone, but underneath gum tissues.

– The Technique involves an initial surgery in which flaps are reflected to expose the edentulous ridge. – Impression of the bone is made at the site of surgery. – Cast is made from the impression and is used to fabricate the implant frame work.

– The Second stage surgery involves the placement of subperiosteal implant on the bony ridge and the reflected periosterum is replaced and sutured over the framework. – An implant supported denture is fabricated and is fixed to the intraoral projections and is retained by prosthetic clips.




Transosseous implants These are inserted through an extraoral incision below the chin with a series of projections that penetrates the mandible from inferior border and are connected by a bone plate that rests on inferior border of the mandible.




Endosteal implant • These are surgically placed within alveolar or basal bone. • They are further divided into – Root form – Blade Form

Root Form • They are cylindrical in shape and may have an external thread. – They are 3 -5 mm in diameter and 7 -20 mm in length – They are made of Titanium or Titanium. Aluminum – Vandium alloy system with or without hydroaxyapatite coatings. – They have the best bio-compatibility character functionally.

Blade Form • These are wedge shaped or rectangular in cross section. – They are 2. 5 mm in width. – 8 -15 mm in depth – 15 -30 mm in length.

Contra indication to implant placement – Acute illness – Pregnancy – Uncontrolled metabolic disease – Improper motivation. – Tumorocidal radiation to implant site – Lack of operating experience – Unable to prosthodontically restore

Surgical Phase • Treatment Plan: Clinical Examination: • Visual • palpation – to find out the following – Flabby tissue – Sharp underlying ridges – Undercuts

Radiographic Evaluation: – Panoramic radiographs: Routine – Lateral Cephalometric film: To find out the bone width in anterior maxilla and mandible – C. T. Scan ( Computerized Tomograms) – used to determine the location of inferior alveolar canal and maxillary sinus.

SURGICAL PROCEEDURES • STAGE I SURGERY- IMPLANT PLACEMENT: – Incision- Crestal incision – Bone is exposed surgical splint is positioned and periodontal probe is used to make a preliminary assessment of potential sites. – Implants that are threaded requires final thread preparation in the bone at a very low speed with the help of a bur.

– The implant recipient site is prepared by a series of gradually larger burs. – After desired depth and diameter of recipient site is prepared the implant is placed – Non threaded implants are positioned into the recipient site and gently tapped with mallet to seat the instrument whereas threaded ones are screwed into place. – Wound is closed with tension free closure. – Radiograph is taken to see the position of implant post operatively.




COMPLICATIONS OF STAGE I SURGERY – Improper angulation's or position of implants – Perforation into the maxillary sinus – Perforation into the inferior alveolar canal – Dehiscence of buccal and lingual cortical plate – Dehiscence of soft tissue. – Fracture of the mandible.

STAGE II SURGERY – This is done after 6 -9 months – At this stage the mucosa is reflected from superior portion of the implant either with a punch or making a crestal incisor. – After the implant is exposed, the implant abutment is placed. – There are 2 approaches to place the implant abutment • To place the abutment that the restorative dentist will use in restoration • To place a temporary healing cap that remains until the tissue heals and will then be discarded And replaced by an abutment.















- Slides: 49