DEFINITION A cancer of bloodforming tissues hindering the
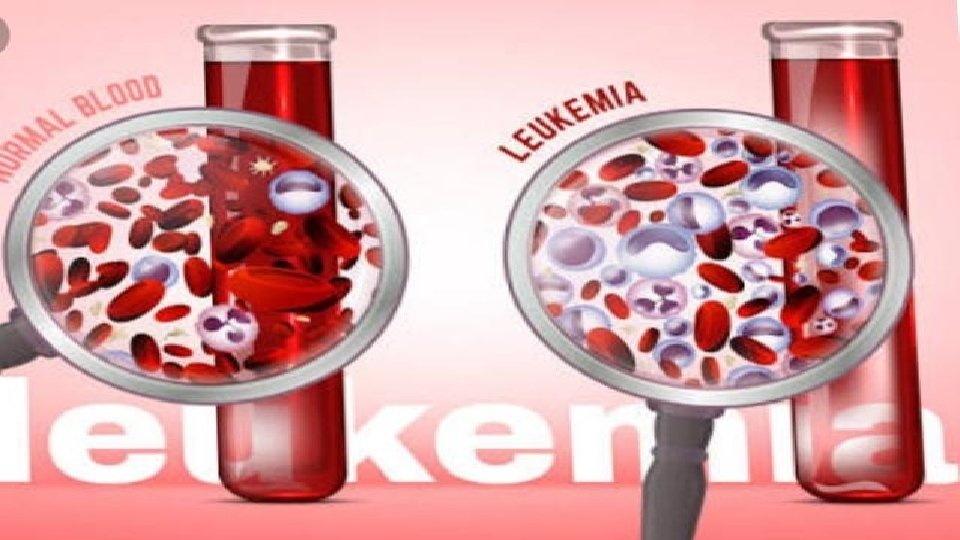

DEFINITION • A cancer of blood-forming tissues, hindering the body's ability to fight infection. • a malignant progressive disease in which the bone marrow and other blood-forming organs produce increased numbers of immature or abnormal leucocytes. These suppress the production of normal blood cells, leading to anaemia and other symptoms.

CAUSES • Causes are unknown for leukemia : studies have found some risk factors for leukemia

RISK FACTORS 1. Working with certain chemicals Example : —Exposure to high levels of benzene in the workplace can cause leukemia. 2. Very high levels of radiation — People exposed to very high levels of radiation are much more likely than others to develop leukemia 3. Chemotherapy — Cancer patients treated with certain cancerfighting drugs sometimes later develop leukemia. 4. Smoking 5. Down syndrome 6. Genetic diseases

SYMPTOMS • Fever, chills, and other flu-like symptoms • Weakness and fatigue • Frequent infections • Loss of appetite and/or weight • Swollen or tender lymph nodes, liver, or spleen

• Easy bleeding or bruising • Tiny red spots (called petechiae) under the skin • Swollen or bleeding gums; • Sweating, especially at night • Bone or joint pain.

LEUKEMIA CLASSIFICATION BASED ON HOW FAST IT DEVELOPS 1. Acute leukemia happens when most of the abnormal blood cells don’t mature and can’t carry out normal functions. It can get bad very fast. 2. Chronic leukemia happens when there are some immature cells, but others are normal and can work the way they should. It gets bad more slowly than acute forms do.

LEUKEMIA CLASSIFICATION BASED ON WHICH TYPE OF CELL IS INVOLVED 1. Lymphocytic (or lymphoblastic) leukemia involves bone marrow cells that become lymphocytes, a kind of white blood cell. 2. Myelogenous (or myeloid) leukemia involves the marrow cells that create red blood cells, platelets, and other kinds of white blood cells.

TYPES OF LEUKEMIA • These broad categories are combined and classified into the four main types of leukemia, which are: 1. Acute lymphocytic leukemia – The most common form of leukemia in children

2. Acute myelogenous leukemia – The most common form of leukemia overall, affecting both adults and children 3. Chronic lymphocytic leukemia – The most prevalent form of chronic leukemia in adults 4. Chronic myelogenous leukemia – Mainly affects adults and may produce few or no symptoms for months or even years

DIAGNOSIS 1. Physical exam. Your doctor will look for physical signs of leukemia, such as pale skin from anemia, swelling of your lymph nodes, and enlargement of your liver and spleen. 2. Blood tests. By looking at a sample of your blood, your doctor can determine if you have abnormal levels of red or white blood cells or platelets — which may suggest leukemia.

3. Flow cytometry: This test may provide valuable insight into whether the tumor cells contain a normal or abnormal amount of DNA, and the relative rate at which the tumor is growing. 4. Imaging tests: These procedures may provide information about the extent of leukemia in the body, and the presence of infections or other problems. The following imaging tests may be used to help formulate a leukemia diagnosis: - X-RAY

• CT scan • PET/CT scan • MRI • Ultrasound • 2 D echocardiogram • Pulmonary function test 5. Lumbar puncture: Also known as a spinal tap, this test may be required to determine the extent of leukemia. Lumbar punctures may also be used to inject medications, such as chemotherapy drugs, to treat the disease.

MEDICAL MANAGEMENT 1. Chemotherapy is the major form of treatment for leukemia. This drug treatment uses chemicals to kill leukemia cells. Depending on the type of leukemia you have, you may receive a single drug or a combination of drugs.

2. Biological therapy works by using treatments that help your immune system recognize and attack leukemia cells. 3. Targeted therapy uses drugs that attack specific vulnerabilities within your cancer cells. For example, the drug imatinib (Gleevec) stops the action of a protein within the leukemia cells of people with chronic myelogenous leukemia. This can help control the disease.

4. Radiation therapy uses X-rays or other high-energy beams to damage leukemia cells and stop their growth. During radiation therapy, you lie on a table while a large machine moves around you, directing the radiation to precise points on your body. You may receive radiation in one specific area of your body where there is a collection of leukemia cells, or you may receive radiation over your whole body. Radiation therapy may be used to prepare for a stem cell transplant.

5. Stem cell transplant. A stem cell transplant is a procedure to replace your diseased bone marrow with healthy bone marrow. Before a stem cell transplant, you receive high doses of chemotherapy or radiation therapy to destroy your diseased bone marrow. Then you receive an infusion of blood-forming stem cells that help to rebuild your bone marrow. You may receive stem cells from a donor, or in some cases you may be able to use your own stem cells. A stem cell transplant is very similar to a bone marrow transplant

SURGICAL MANAGEMENT • BONE MARROW TRANSPLANT bone marrow transplant is a process to replace unhealthy bone marrow with healthy bone marrow.

NURSING MANAGEMENT

PATIENT EDUCATION AND HEALTH MAINTENANCE: • Teach signs and symptoms of infection and advise whom to notify. • Encourage adequate nutrition to prevent emaciation from chemotherapy.

• Teach avoidance of constipation with increased fluid and fiber, and good perineal care. • Teach bleeding precautions. • Encourage regular dental visits to detect and treat dental infections and disease.

PREVENTING INFECTION: • Frequently monitor the client for pneumonia, pharyngitis, esophagitis, perianal cellulitis, urinary tract infection, and cellulitis, which are common in leukemia and which carry significant morbidity and mortality. • Monitor fever, flushed appearance, chills, tachycardia; appearance of white patches in the mouth; redness, swelling, heat or pain in the eyes, ears, throat, skin, joints, abdomen, rectal and perineal areas; cough, changes in sputum; skin rash

• Check results of granulocyte counts. Concentrations less than 500/mm 3 put the patient at serious risk for infection. • Avoid invasive procedures and trauma to skin or mucous membrane to prevent entry of microorganisms. • Use the following rectal precautions to prevent infections: Avoid diarrhea and constipation, which can irritate the rectal mucosa, avoid the use of rectal thermometers, and keep perineal are clean.

• Care for the patient in private room with strict handwashing practice. • Encourage and assist patient with personal hygiene, bathing, and oral care. • Obtain cultures and administer antimicrobials promptly as directed.

PREVENTING AND MANAGING BLEEDING: • Watch for signs of minor bleeding, such as petechiae, ecchymosis, conjunctival hemorrhage, epistaxis, bleeding gums, bleeding at puncture sites, vaginal spotting, heavy menses. • Be alert for signs of serious bleeding, such as headache with change in responsiveness, blurred vision, hemoptysis, hematemesis, melena, hypotension, tachycardia, dizziness.

• Test all urine, stool, emesis for gross and occult blood. • Monitor platelet counts daily. • Administer blood components as directed. • Keep patient on bed rest during bleeding episodes.

NURSING DIAGNOSIS ? ? ?

THANK YOU
- Slides: 29