DEFICIENCY OF PROTEINS Presented By Mr Ajith K

DEFICIENCY OF PROTEINS Presented By: Mr. Ajith K K Asst. Professor College of Nursing, Kishtwar

PROTEIN ENERGY MALNUTRITION (PEM) Protein Energy Malnutrition (PEM) or Protein Caloric Malnutrition (PCM) has been identified as not only an important cause of children morbidity and mortality but also leads to permanent impairment of physical and mental growth.

CLINICAL FORMS OF PEM � Kwashiorkor is caused by the deficiency of proteins in diet. The main features are growth failure, edema, diarrhoea, anaemia, and changes in skin and hair. � Marasmus is caused by severe deficiency of both proteins and calories in the diet. This is characterized by growth failure, loss of fat, signs of dehydration, and mental changes.

CAUSES OF PEM � An inadequate intake of food in quantity and quality. � Infections like diarrhoea, measles, respiratory infections and intestinal worms. � Poor environmental sanitation. � Large family size. � Poor maternal health. � Failure of lactation. � Premature termination of breast feeding. � Adverse cultural practices related to breast feeding and weaning.
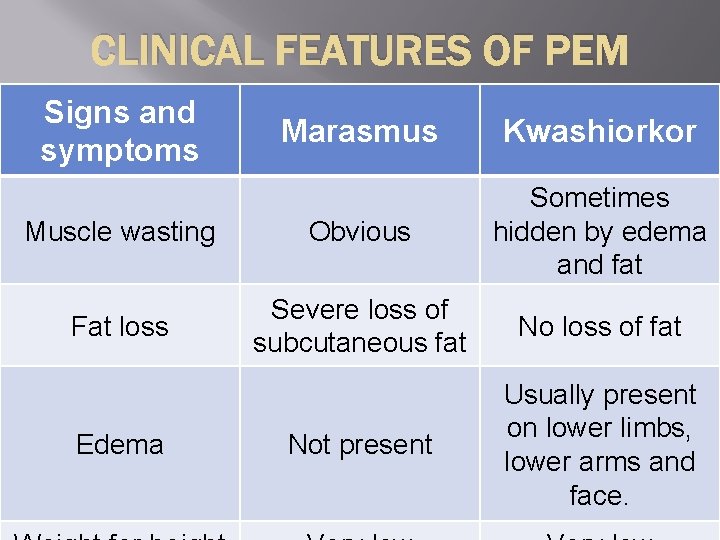

CLINICAL FEATURES OF PEM Signs and symptoms Marasmus Kwashiorkor Muscle wasting Obvious Sometimes hidden by edema and fat Fat loss Severe loss of subcutaneous fat No loss of fat Not present Usually present on lower limbs, lower arms and face. Edema
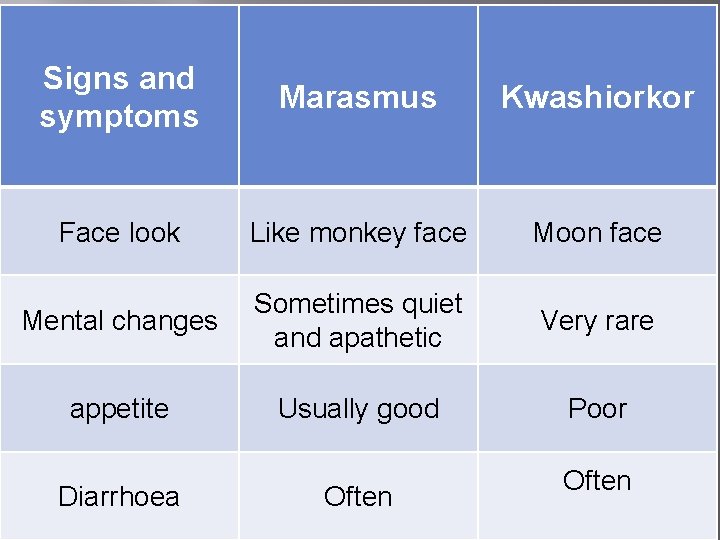
Signs and symptoms Marasmus Kwashiorkor Face look Like monkey face Moon face Mental changes Sometimes quiet and apathetic Very rare appetite Usually good Poor Diarrhoea Often
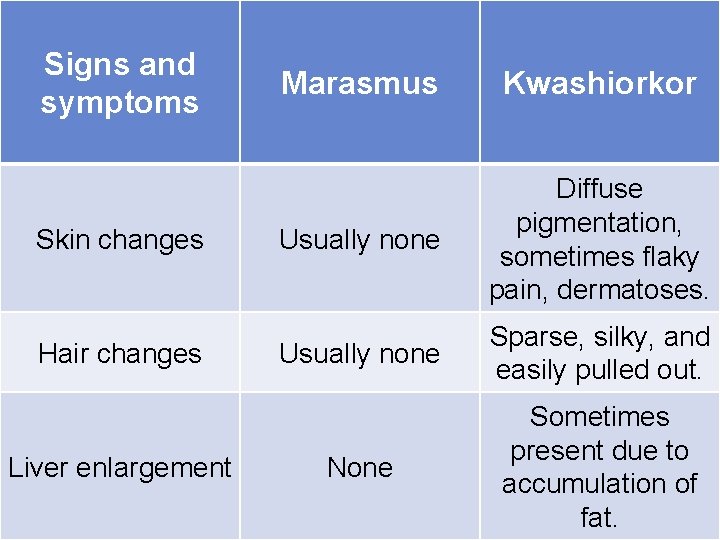
Signs and symptoms Skin changes Hair changes Liver enlargement Marasmus Kwashiorkor Usually none Diffuse pigmentation, sometimes flaky pain, dermatoses. Usually none Sparse, silky, and easily pulled out. None Sometimes present due to accumulation of fat.

DETECTION OF PEM � Underweight for age. � Road – to – health growth chart.

CLASSIFICATION OF PEM a) Gomez’s classification � Degree of PEM is classified as: Ø Weight between 90 – 110% = Normal nutritional status Ø Weight between 75 – 89% = 1 st degree malnutrition (mild) Ø Weight between 60 – 74% = 2 nd degree malnutrition (moderate) Ø Weight below 60% = 3 rd degree malnutrition (severe)

b) Waterflow’s classification Weight ∕ height Height ∕ age ˃ m – 2 SD ˂ m – 2 SD ˃ m – 2 SD Normal Wasted Stunted Wasted and stunted ˂ m – 2 SD
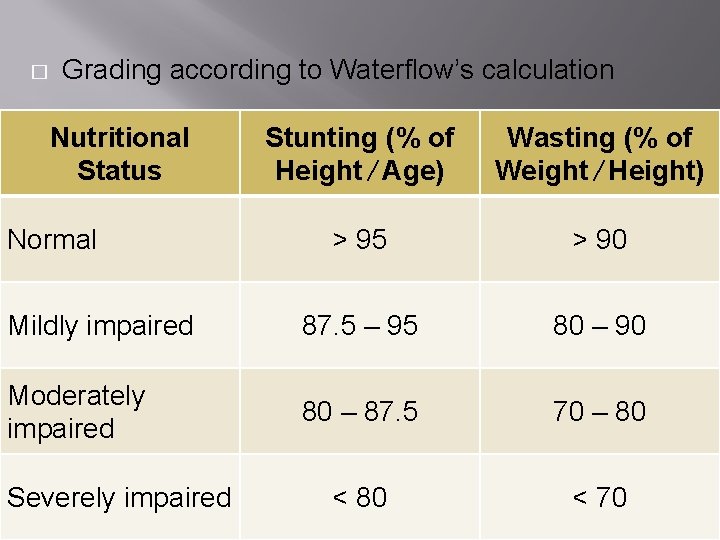
� Grading according to Waterflow’s calculation Nutritional Status Stunting (% of Height ∕ Age) Wasting (% of Weight ∕ Height) ˃ 95 ˃ 90 Mildly impaired 87. 5 – 95 80 – 90 Moderately impaired 80 – 87. 5 70 – 80 ˂ 70 Normal Severely impaired
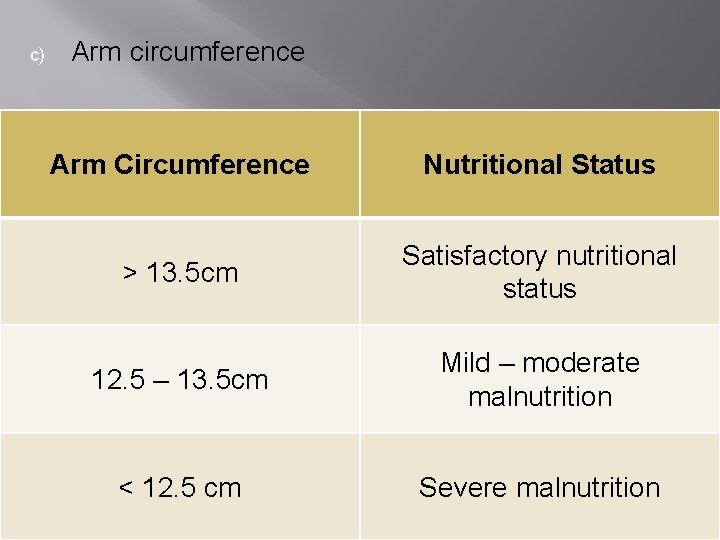
c) Arm circumference Arm Circumference Nutritional Status ˃ 13. 5 cm Satisfactory nutritional status 12. 5 – 13. 5 cm Mild – moderate malnutrition ˂ 12. 5 cm Severe malnutrition

PREVENTIVE MEASURES A) Health Promotion Ø Measures are directed to pregnant and lactating women (education and nutritional supplements. ) Ø Promotion of breast feeding. Ø Development of low cost weaning foods. Ø Improvement of family diet. Ø Nutrition education. Ø Home economics. Ø Family planning and spacing of birth.

PREVENTIVE MEASURES B) Specific Protection Diet of the child must contain protein and energy rich foods such as milk, eggs, fresh fruits. Immunization against diseases. Food fortification. Early detection and treatment. Ø Ø ü Periodic surveillance. ü Early diagnosis with degrees of malnutrition. ü In case of PEM, good quality protein 3 – 4 g ∕ kg body weight∕day should be given. ü ORS for children with diarrhoea. ü Deworming of infested children.

PREVENTIVE MEASURES C) Rehabilitation Ø Nutritional rehabilitation services Ø Hospital treatment in case of severe PEM. Ø Follow up care.

THANK YOU
- Slides: 16