DDA Employment and Day Services Webinar 2 83116

DDA Employment and Day Services Webinar # 2: 8/31/16 1 -2: 30 PM Payment in

Agenda • Introduction • QUICK Review of P 1 access, profiles, basic billing, remittance advice, reports. • Q & A about review • Adjusting billing • Q & A about billing adjustments • Wrap up and reminder about next webinar 8/16/2016 2

Profiles in Provider. One • A profile is a type of access that when assigned to a user gives the user different capabilities. One person may have one or many profiles. – EXT Provider System Administrator - a role in the Provider. One system that is filled by one or more people in your organization to add or remove users and user profiles, unlock user accounts, and reset passwords. This is not used to view billing. – EXT Provider Social Services or EXT Provider Social Services Medical – a role associated with providers who have a DSHS contract linked to Provider. One of these two profiles will be used to view your employment and day services billing. 8/16/2016 3

Access to Provider. One 1. If your organization already bills in Provider. One using the same Tax ID for other services then you have a system administrator who can provide access to Provider. One. This existing system administrator may be in another department. 8/16/2016 4

The Provider. One User Access Request form was sent directly to those who need to set up a system administrator in Provider. One. The form can also be found here Provider. One User Access Request form. 8/16/2016 5

Adding new users or other profiles http: //hca. wa. gov/assets/billers-and-providers/setup. pdf 8/16/2016 6
I am replacing an existing system administrator. What do I do? Submit: 1. Provider. One user access request form – Contact information and instructions are listed on the form 2. A letter on your organization’s letterhead stating that the current system administrator (with their name) should no longer have access to Provider. One – The letter must be signed by an office manager or provider that is not the same person requesting access – Provider. One Security will expire the previous system administrator's access and assign confidential login credentials to the person named on the form – The login credentials will be sent in two separate emails to the individual email address listed on the Provider. One User Access Request form 8/16/2016 7
How do I unlock my account? • First check with other System Administrators in your organization, they can assist you. If you are the only System Administrator, To unlock your Provider. One account, go to the login page. Under the login button: • Select To Unlock Account and Reset Password, Click here. You will be required to answer the password reset questions, listed below, before a temporary password will be sent to the email address in your user file Security questions are: – Secret Question (case sensitive) – Date of Birth (mm/dd/yyyy) – Last Name (case sensitive) 8/16/2016 • If you get an error message saying your security questions are incorrect, contact your organization’s system administrator for verification. If you are a system administrator, email Provider. One Security to regain system access. 8

Provider. One Access Help 1. Contact your organizations System Administrator 2. Contact Provider. One Security at: – Email: provideronesecurity@hca. wa. gov – Phone: 1. 800. 562. 3022 ext. 19963 – Webform: https: //fortress. wa. gov/hca/p 1 contactus/ • Note: Provider. One Security is only able to assist with login credentials. 8/16/2016 9

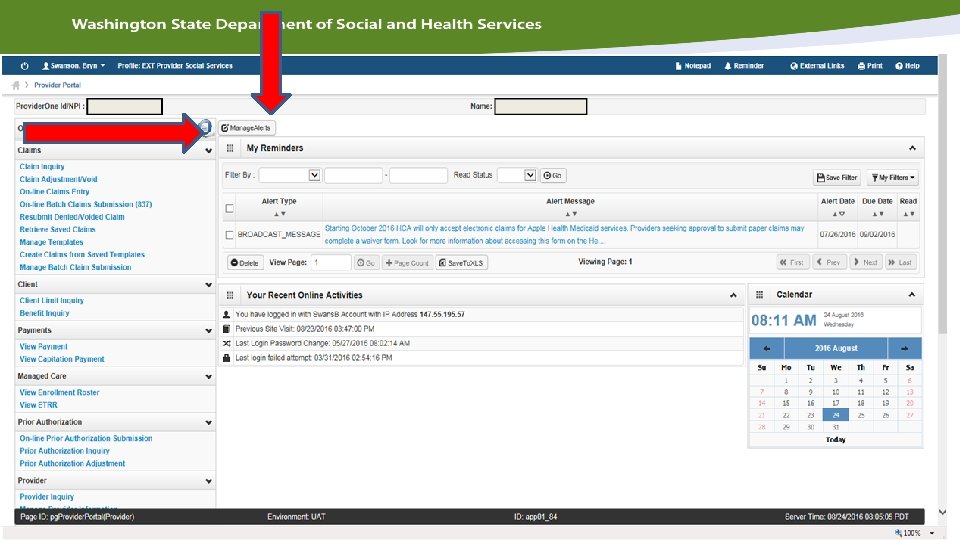
What is Available to View in P 1? (According to your profile. Different profiles have different levels of access. ) o View the Remittance Advice (RA) o View claims history o View adjustment history o View P 1 authorizations o 8/16/2016 View location information such as addresses and phone numbers and update your communication Preference (Email, Standard Mail, Provider. One Notice) 10

Dates of Service June 30, 2016 and before Submit an A-19 Invoice for payment after posting 8/16/2016 • After July 1, 2016 Submit a county billing summary and signed document after posting 11

How Will the Day I Post in AWA Effect the Pay Date? • Example Posting Dates and Resulting Pay Dates handout! • County posts to AWA, overnight an authorization is created in CARE, the following night a claim is generated in Provider. One • A claim entered into Provider. One by 5: 00 pm on Tuesday will pay out that Friday • On Monday and Tuesday CARE doesn’t run its nightly job
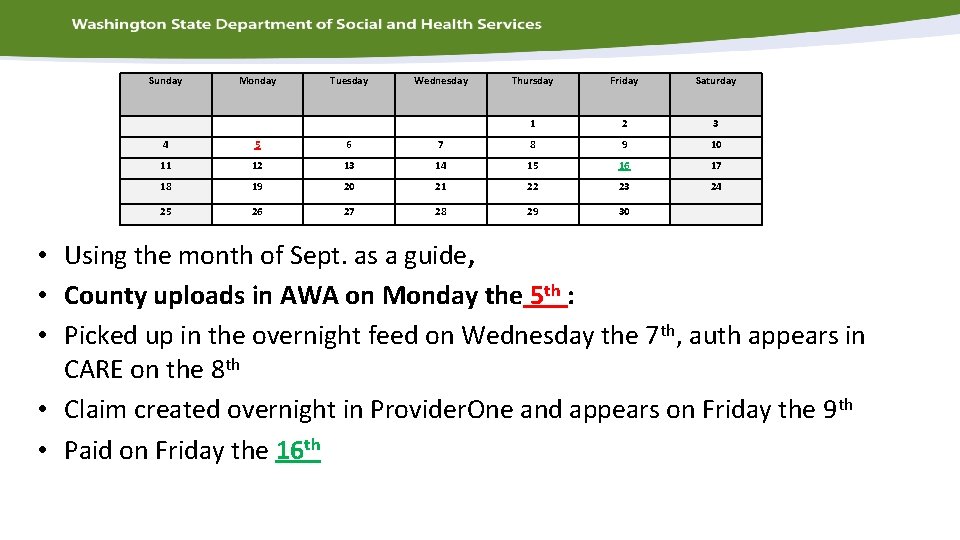
Sunday Monday Tuesday Wednesday Thursday Friday Saturday 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 • Using the month of Sept. as a guide, • County uploads in AWA on Monday the 5 th : • Picked up in the overnight feed on Wednesday the 7 th, auth appears in CARE on the 8 th • Claim created overnight in Provider. One and appears on Friday the 9 th • Paid on Friday the 16 th
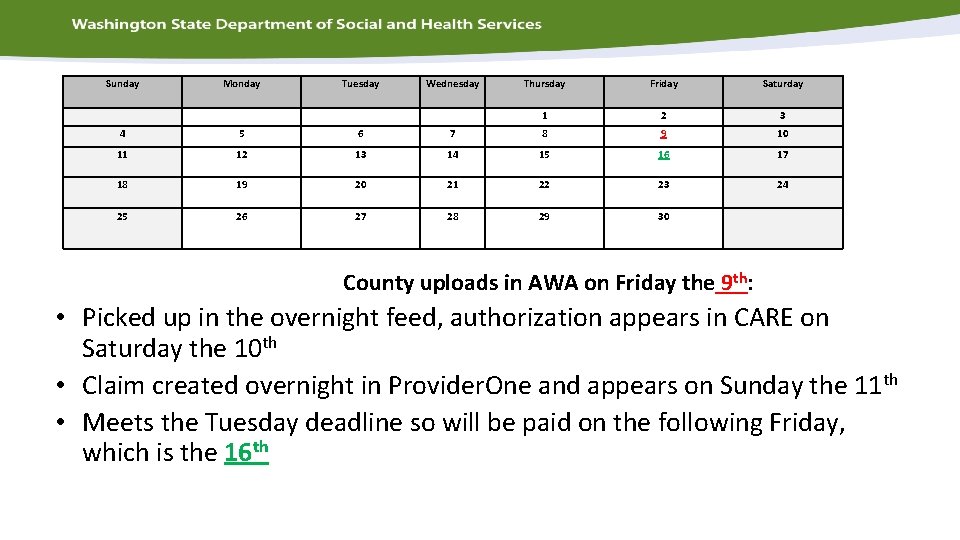
Sunday Monday Tuesday Wednesday Thursday Friday Saturday 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 County uploads in AWA on Friday the 9 th: • Picked up in the overnight feed, authorization appears in CARE on Saturday the 10 th • Claim created overnight in Provider. One and appears on Sunday the 11 th • Meets the Tuesday deadline so will be paid on the following Friday, which is the 16 th
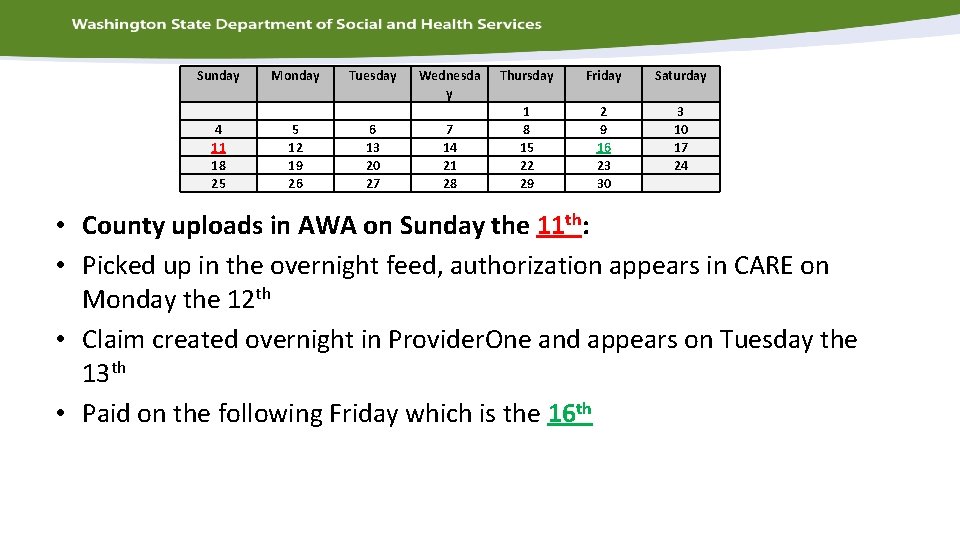
Sunday 4 11 18 25 Monday 5 12 19 26 Tuesday 6 13 20 27 Wednesda y 7 14 21 28 Thursday Friday Saturday 1 8 15 22 29 2 9 16 23 30 3 10 17 24 • County uploads in AWA on Sunday the 11 th: • Picked up in the overnight feed, authorization appears in CARE on Monday the 12 th • Claim created overnight in Provider. One and appears on Tuesday the 13 th • Paid on the following Friday which is the 16 th

Helpful tip • Sunday (before 5 pm) is the latest you can post your billing in AWA in order to get paid that upcoming Friday, Posting billing in AWA any day after Sunday will mean you will not get paid until the following Friday. • This is because of the time it take to go though the different systems, AWA, CARE, Provider. One.

EFT: Electronic-Funds-Transfer • Follow the instructions and complete the Electronic Funds Transfer Form to stop receiving a paper check and start direct deposit. • Electronic Funds Transfer Form Instructions • Electronic Funds Transfer Form 8/16/2016 17

EFT Questions: • For questions regarding electronic funds transfers, please contact the Customer Service Department for Providers. You will call the same 800 number (800 -562 -3022), but you will need to follow the prompts for providers rather than putting in an extension. 8/16/2016 18
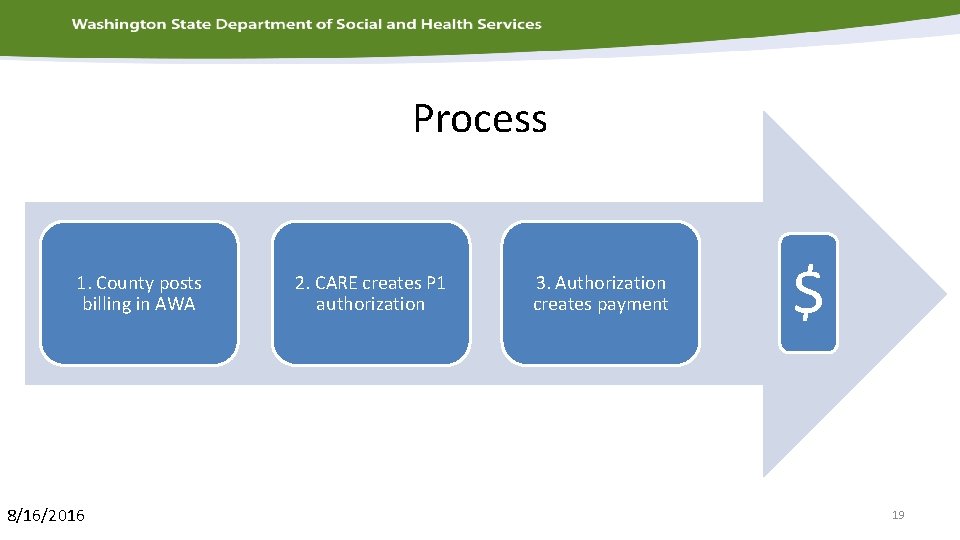
Process 1. County posts billing in AWA 8/16/2016 2. CARE creates P 1 authorization 3. Authorization creates payment $ 19
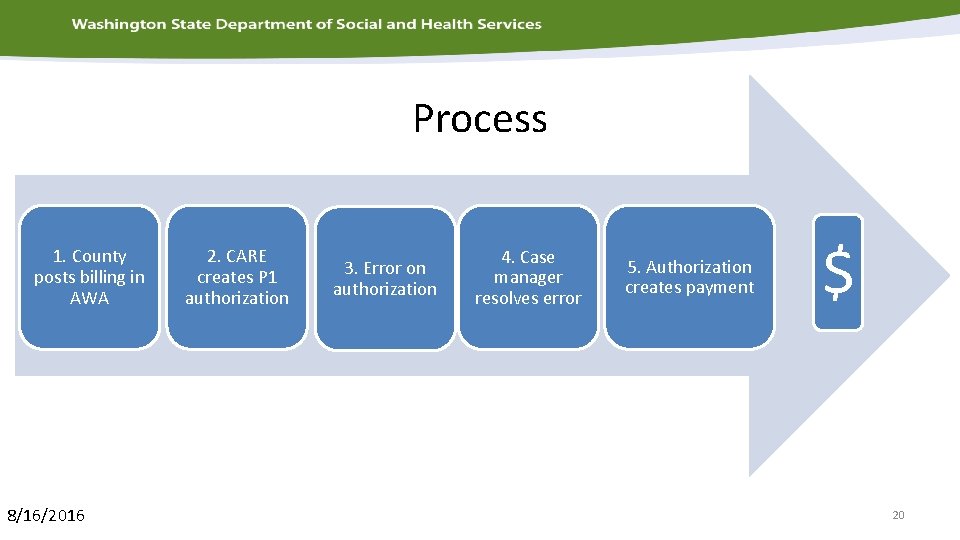
Process 1. County posts billing in AWA 8/16/2016 2. CARE creates P 1 authorization 3. Error on authorization 4. Case manager resolves error 5. Authorization creates payment $ 20

Examples of edits that result in Authorization Errors • Provider does not have a valid contract for the service • Client is not financially eligible • Client is not functionally eligible

New Reports (Coming soon to ADS Reporting) • P 1_32092 DDA Employment and Day Services Billing Reconciliation Report • P 1_33810 DDA Employment and Day Services Billing Adjustment Report • Access reports at: https: //adsareporting. dshs. wa. gov/Login. aspx? Return. Url=%2 fdefault. aspx 8/16/2016 22

P 1_32092 DDA Employment and Day Services Billing Reconciliation Report Purpose of report: Identifies the difference between what counties have billed and what P 1 has paid or denied, broken out by Account Title/Service, Program/RAC, and associated detail. Summary Report shows: • Amounts billed through ADSA Web Access (AWA) by RAC and Account Title/Service Code. • Amounts paid through Provider. One, and the difference between P 1 amount paid and AWA amount billed. Detail Report shows: • Amounts authorized and paid by client identifier, authorization number, and different 23 8/16/2016 claims statuses.

P 1_33810 DDA Employment and Day Services Billing Adjustment Report • Purpose: To identify AWA and Provider. One authorizations that do not match payments out of Provider. One. The report shows P 1 amounts authorized and paid, as well as configuration data attached to the client or provider such as RAC, Taxonomy, Service, and Rate. • Report shows: Records with discrepancies between authorized and paid amounts. 8/31/2016 24

New Reports The reports info from Provider. One are updated every Tuesday AM The reports should be available to use early to mid September Please see Megan Bur if you are not able to access the reports 8/31/2016 25

Case Manager Role • No change to the referral process or County Service Authorization process for the case manager. Most case managers will experience little impact from this change. • Case managers already resolve authorization errors for services billed through Provider. One. • Case managers will be informed of the payment of county services through Provider. One via a Management Bulletin. Case Managers: Attend to CSA and Referral process Attend to P 1 authorization ticklers Escalate authorization or payment issues to supervisor Escalate CSA or referral issues to supervisor 8/16/2016 26

Regional Operations Managers Role • Yesterday -reconciliation occurs prior to payment – Fund Source and spending limits validated prior to payment • Today -reconciliation occurs after payment – Contract limits are reviewed after payment is made Regional Operations Managers: Manage authorizations for Indirect Consumer Supports Track expenditures and reconcile to spending plan 8/16/2016 27

County Role • The Counties will still upload billing into AWA using the same process, but will now have access to the Provider. One system. • Counties can now log in to Provider. One to view billing information if you choose to do so, it is not a requirement. County Role: Post billing in AWA Submit County Billing Summary and signed document to Regional Operations Manager Escalate Referral, CSA or P 1 authorization concerns to Case Manager Escalate Indirect Consumer P 1 authorization concerns to Regional Operations Managers 8/16/2016 28

Get Help • • • Direct Service CSA or Provider. One Authorizations- Case Manager Indirect Consumer Supports- Regional Operations Manager AWA billing issues- Employment Specialist AWA technical support- ADSHELPDESK@dshs. wa. gov Provider. One access and security: – – – 8/16/2016 Email: provideronesecurity@hca. wa. gov Phone: 1. 800. 562. 3022 ext. 19963 Webform: https: //fortress. wa. gov/hca/p 1 contactus/ 29

The Regional Operations Managers are: Region 1: Roger Van Allen (DSHS/DDA) Van. Al. RL@DSHS. WA. GOV 509. 329. 2952 Region 2: Joe Carter (DSHS/DDA) Carte. JF@dshs. wa. gov 425. 339. 4836 Region 3: Wendi Winchel (DSHS/DDA) Winch. WA@dshs. wa. gov 360. 725. 4264 8/16/2016 30

The Regional Employment Specialists are: • Region 1: Carrie Bayha. CS@dshs. wa. gov 509. 374. 2128 • Region 2: Rod Duncan Dunca. RA@dshs. wa. gov 425. 339. 4855 • Region 3: Geoff Nisbet Nisbeg@dshs. wa. gov 360 -725 -4304 8/16/2016 31

Communication Preference Many of you may have started to receive Provider. One (P 1) Authorization alerts in your email. This is because you are the designated contact for the County Location for P 1. You cannot opt out of this notification; however, you do have preferences in how you receive these notifications in P 1. See more info including screenshots below. Clients and NSAs will also receive monthly notification of authorized services via paper letter. This communication is for transparency purposes for clients and NSAs, and they also cannot opt out of this notification. Clients and NSAs do not have the ability to change this notification from paper letter as they do not have P 1 portal access. If individuals already receive other paid services then they already are receiving similar notification. This is only new for clients that solely receive employment and/or day services.
If you have email selected as your Communication preference:

If you have Standard Mail selected as your communication Preference you will receive a letter, this is also what Client and NSA will receive.
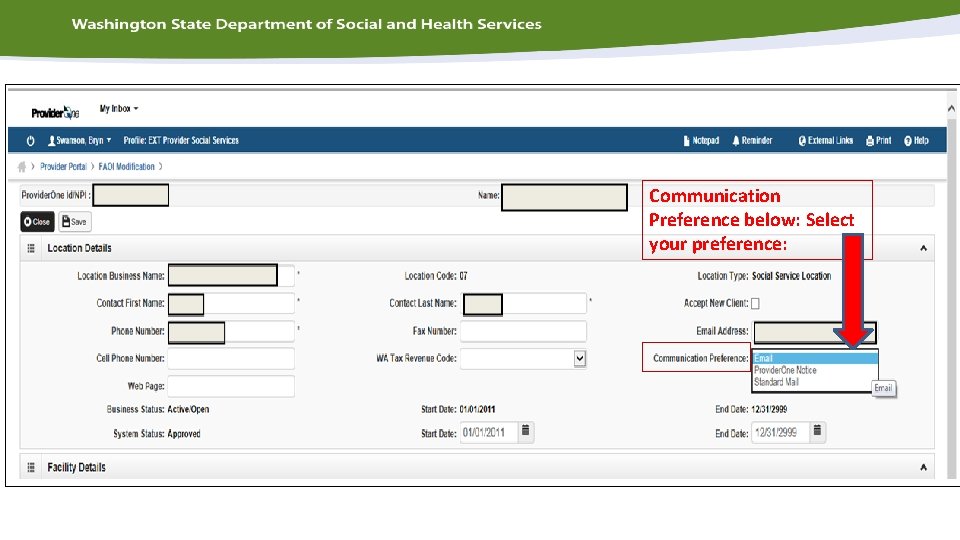
Communication Preference below: Select your preference:

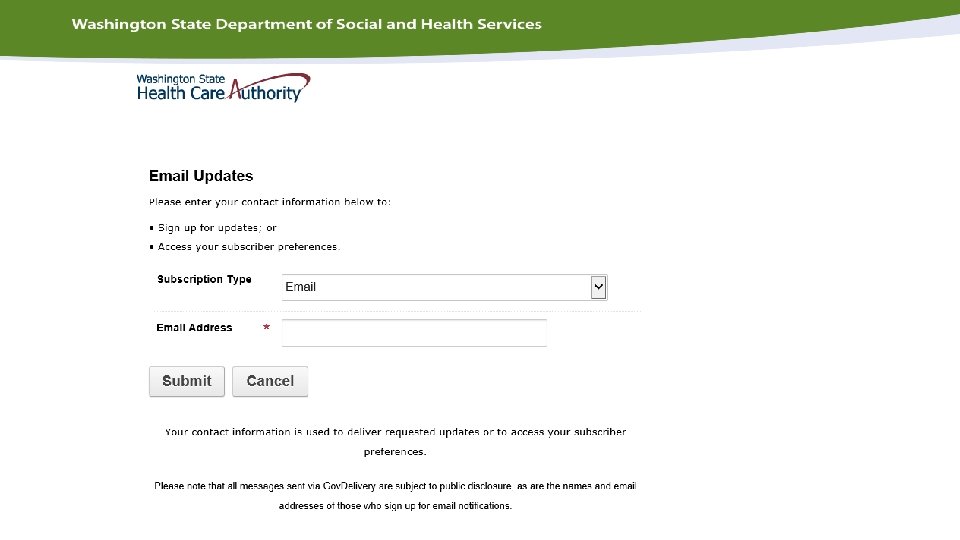
Sign up for Provider Alerts What is a Washington Apple Health (Medicaid) Provider Alert? • A Provider Alert is an email notification regarding program, authorization, or billing related changes to specific Washington Apple Health (Medicaid) programs. (This is not a requirement) • https: //public. govdelivery. com/accounts/WAHCA/subscriber/n ew • You will still get paid if you do not sign up for alerts.

1099 Social Services-Only Provider • 1099 social services-only provider • Non-medical social service providers: Receive a 1099 tax form from the state of Washington. • Provide services to clients who are eligible for Medicaid services. • Have a contract with DSHS. • Have business performing home care services. • Receive payment through use of a social services authorization. • If the above information is true, this page is for you!

Questions & Answers 8/16/2016 40
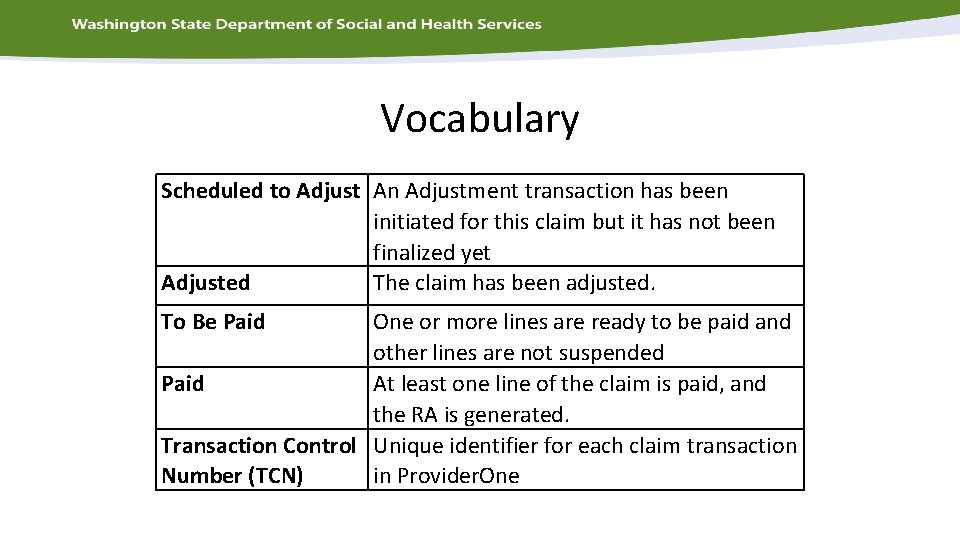

Vocabulary Scheduled to Adjust An Adjustment transaction has been initiated for this claim but it has not been finalized yet Adjusted The claim has been adjusted. To Be Paid One or more lines are ready to be paid and other lines are not suspended Paid At least one line of the claim is paid, and the RA is generated. Transaction Control Unique identifier for each claim transaction Number (TCN) in Provider. One

Adjusting previous billing 1. County posts revised billing 2. CARE changes authorization in Provider. One 3. Operations Manager sees difference between authorization and payment using report P 1_33810 DDA Employment and Day Services Billing Adjustment Report 4. Operations Manager submits ticket to HCA claims 5. HCA adjusts claim and difference is paid
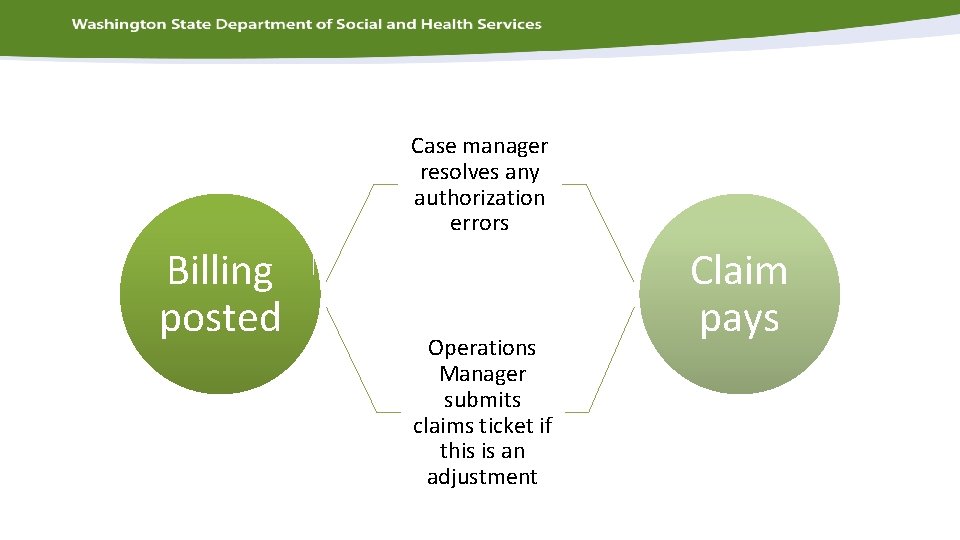
Case manager resolves any authorization errors Billing posted Operations Manager submits claims ticket if this is an adjustment Claim pays

• Adjustments to previous posted billing will not offset future payments or pay additional money automatically. Manual action triggers the claim to reprocess. • The primary process for triggering the claim to be reprocessed is for the Operations Manager or designee to submit a claims ticket to HCA.

Info and Ed Authorization should never have been created • Info and Ed: Bill a negative amount equal to previous billed amount. • Authorization will be cancelled by CARE

Info and Ed Authorization should never have been created • Cancelled authorization will display on report P 1_33810 as money being paid without an authorization • Operations Manager will submit claims ticket requesting offset of future payment.

Info and Ed Authorization should never have been created • After reprocessing the claim will show as denied because the original authorization now is cancelled and a credit will be created for the collection to be made.

Service Authorization should never have been created • Employment or Day service: Bill zero units. • Authorization will be cancelled by CARE

Service Authorization should never have been created • Cancelled authorization will display on report P 1_33810 as money being paid without an authorization • Operations Manager will submit claims ticket requesting offset of future payment.

Service Authorization should never have been created • After reprocessing the claim will show as denied because the original authorization now is cancelled and a credit will be created for the collection to be made.

Authorization units or rate increased. The total amount of the authorization changes from $109. 23 to $123. 75 • Month 1 county posts 109. 23 and is paid • Month 2 county posts 123. 75 – Report P 1_33810 shows authorization of 123. 75 but payment of 109. 23 – Operations Manager submits claims ticket to HCA – Claim is processed and additional 14. 52 is paid.
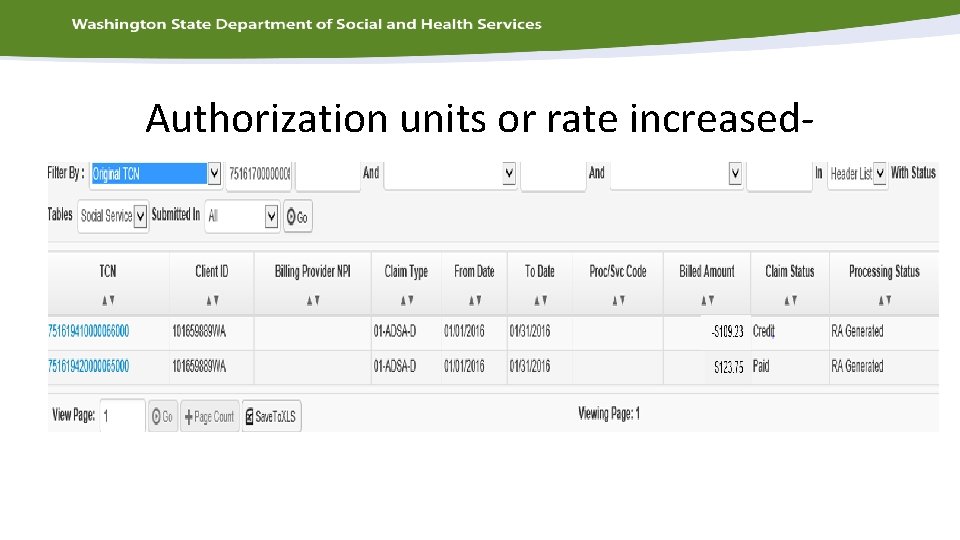
Authorization units or rate increased-

Summary of adjustments • Cancel Info and Ed-bill negative amount equal to previously billed amount • Cancel Service-bill zero units for previously billed month of service • Adjust rate or dollars up or down-Post revised billing, then operations manager or designee will initiate change to claim

Less common adjustment scenarios • Neutral adjustment-RAC change • Service code change

Neutral Adjustment-RAC Change 1. Case manager changes RAC 2. Case manager or operations manager submits claims ticket to HCA 3. Claim is reprocessed to obtain correct coding

Service Code Change • Cancel incorrect service by billing zero units • Bill with correct service code

Log in to Provider. One at https: //www. waproviderone. org/ Additional Provider. One Resources Billing: http: //www. hca. wa. gov/billers-providers/providerone-social-services Access and Security: http: //www. hca. wa. gov/billers-providers/providerone-security 8/16/2016 57

Webinar 3 (same material as Webinar 2 plus more) September 20, 2016 1: 00 -2: 30 https: //attendee. gotowebinar. com/register/8206691394139951620 • ◦ Review previous training topics • ◦ Billing adjustments (Change in previously billed units or rate) • 8/16/2016 August 2016 58
• County Webinar 8 -16 -16 questions and answers from the webinar (Next 11 slides) Q: How do credits work if the county received an overpayment? A: The September and October webinars will address the topic of overpayments. Q: If we already receive payments from HCA for other services, do we need to send in an additional electronic payment form? Just to clarify, if we are already receiving EFT payments, we are still required to complete a new EFT form for P 1, correct? A: You will need to check with HCA to confirm this. You can call Phone: 1 -800 -562 -3022 wait for prompts specific to EFT or email, Email: provideronesecurity@hca. wa. gov Q: Who will be the AWA billing issue contact persons for CDS? A: The same person it is today. Q: After I post the billing in AWA, when will I get paid? A: Once Counties post, authorizations that are in AWA by Saturday will pay the following Friday. 8/16/2016 59

County Webinar 8 -16 -16 questions and answers from the webinar Q: What is an indirect consumer P 1 authorization? A: I said an example of indirect services is Admin Cost. I have since been corrected. You should refer to your contract Q: Someone asked a question about "Indirect Consumer P 1 Authorization". You answered that it is for Admin Services. Is it also for Info/Ed and Training and other indirects? A: Please refer to your contract. Q: ARE WE ALLOWED TO BILL INDIRECT COST ASIDE FROM THE ADMIN FEE? A: Please refer to your contract.

Q: To clarify Indirect also refers to Information and Education, training etc. ie. "other consumer supports" A: Please refer to your contract. Q: If I am the billing person who bills the monthly DDA billing, do I have to access provider 1 for any reason? A: No, only if contact information for the county changes. You would need to update this in Provider. One. Q: Can you please elaborate on the answer you just gave that if someone handles the billing for their county, they do not need to access Provider. One? A: Billing will still be posted in AWA like it is today. You do not need to access Provider. One to upload your billing. Accessing Provider. One is not a requirement however, you will need to access Provider. One if you wish to View the Remittance Advice (RA), View claims history, View adjustment history, View P 1 authorizations and or to View location information such as addresses and phone numbers. 8/16/2016 61

Q: Why would counties want to access P 1 if all the billing and reports are in AWA? A: See above answer. Reports will be accessible through ADSA reporting. If you do not have access please speak to Megan Burr. Here is the link: https: //adsareporting. dshs. wa. gov/Login. aspx? Return. Url=%2 fdefault. aspx Q: What reports are going to be available 9/10/16? A: P 1_32092 DDA Employment and Day Services Billing Reconciliation Report and P 1_33810 DDA Employment and Day Services Billing Adjustment Report. Q: So it sounds like the billing process itself through AWA does not change, P 1 is just about how the Counties receive payment. A: YES

Q: Why would counties want to access P 1 if all the billing and reports are in AWA? A: See above answer. Reports will be accessible through ADSA reporting. If you do not have access please speak to Megan Burr. Here is the link: https: //adsareporting. dshs. wa. gov/Login. aspx? Return. Url=%2 fdefault. aspx Q: What reports are going to be available 9/10/16? A: P 1_32092 DDA Employment and Day Services Billing Reconciliation Report and P 1_33810 DDA Employment and Day Services Billing Adjustment Report. Q: So it sounds like the billing process itself through AWA does not change, P 1 is just about how the Counties receive payment. A: YES 8/16/2016 63
Q: We also discussed at ACHS, counties can continue to use and sign the A-19 form. . it's just not the mechanism for payment. A: YES Q: There is no designated line to sign on the county billing summary. Do we sign anywhere and send to Roger Van Allen (or whomever is in Van Allen's position)? A: YES, you would send this to your Regional Operations Manager. Q: What is the signed document that we are going to be signing? (Instead of the A-19) A: County Billing Summary is the signed document that you will be signing. If you would like you can still sign and submit A-19 as well but you only need to sign and submit the County Billing Summary. Q: Where do we get the summary form? Can you show us where to access the county billing summary in AWA? Q: Can you show us where to access the county billing summary in AWA? A: SCREEN SHOT OF BILLING SUMMAR Y IN AWA: (next slide)
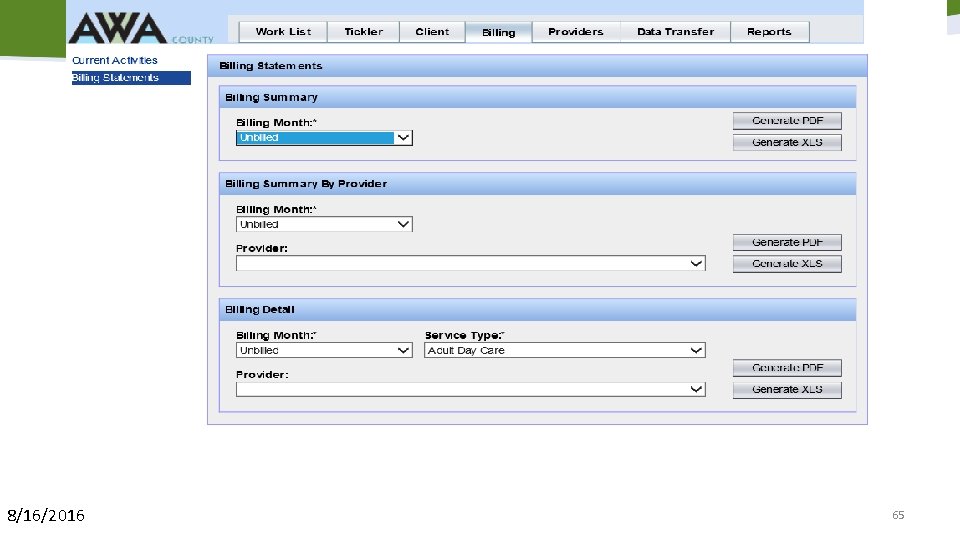
8/16/2016 65

Q: Since we are reconciliation after the fact, what are the timelines that we can submit amended billings? A: The webinars in September and October will go over this process more in depth. Q: Clarify please, if we currently bill through AWA and receive electronic payment are we good to go, or do we have to submit a new authorization for electronic payment? A: You will need to submit an Electronic Fund Transfer Q: what is the phone number for the social service customer service center? A: 1 -800 -562 -3022 ext. 19963 Q: CSA being done through provider one? A: No, the CSA will be done the same way it is today. Payment will come through Provider. One. 8/16/2016 66

Q: Where do I find the National Provider Identifier #? A: NPI- The National Provider Identifier is a federal system using a standardized unique identifier for all providers of health care services, supplies, and equipment. It is mandated as part of HIPAA. Your employer should have this on file. You can also find this in Provider. One. Q: Can the summary be sent by email - as a pdf? A: Please check with your Regional Operational Manager (ROM). Q: Are we able to keep billing the way we have been A: YES Q: Can the summary be sent by email - as a pdf? A: Please check with your Regional Operational Manager (ROM). 8/16/2016 67

Q: Are we able to keep billing the way we have been A: YES Q: If we have multiple programs does this only cover the dd program A: This webinar is only addressing the DD program at the county. Q: so we can still use A-19 s for payment A: No, not for services provided after July 1, 2016. You can use A-19 for services provided June 30 th, and prior, as well as any billing adjustments for services provided 6/30/16 and before. Q: Are you seeing my questions? Are you getting my questions? A: Yes, sorry it was hard to see them but listed in this document are all of the questions that were typed. Q: Still able to post only once a month? A: Yes, still only post in AWA once a month, just like you currently do. 8/16/2016 68
Q: The errors that are created from no fund source or units billed exceeds units will be sent automatically to the CRM for correction? A: No, AWA/CARE errors will not be sent to CRMs. You will still need to work with them to fix errors. P 1 errors will be automatically sent to CRMs. Q: how does the payment generated? Is it when I hit update in AWA? A: Yes, when you post in AWA. Q: What is Peggy's phone #? A: 360 -725 -2541 (peggy. dotson@dshs. wa. gov) Q: If there are errors and it delays payments will payments be issued with multiple checks/deposits? A: Yes 8/16/2016 69
- Slides: 69