Day to Day Process and Quality Improvement Hardwiring
































- Slides: 37

Day to Day Process and Quality Improvement: Hardwiring Plan/Do/Study/Act Kathryn Harmes M. D. PCMH Director, Department of Family Medicine Grant M. Greenberg M. D. , M. A. , M. H. S. A. Associate Medical Director for Quality, UM Medical Group Associate Chair for Information Management and Quality, Department of Family Medicine

Disclosures None to report for either speaker

Learning Objectives • Recognize standard methodology and tools for rapid cycle problem solving • Prepare and utilize Plan Do Study Act (PDSA) cycles for daily process improvement • Practice methods of conducting root cause analysis and relate its importance for successful Quality Improvement

What went wrong: problem solving is not simple • We come across issues every day in clinical practice • When things don’t go exactly right, do we always understand why?

Typical Problem Solving Good people wanting to do the right thing and get work done, jumping to conclusions about perceived problems based on gut instinct and hearsay, applying poor fixes that are doomed to fail over the long-term.

Problems are Opportunities “No problem is problem” -Ohno, Toyota “I haven't failed, I've found 10, 000 ways that don't work. ” - Thomas Edison

Finding a Problem for Improvement • “If you don’t have standard work first, don’t expect any improvement” -Dave Lagozzo • Start by evaluating the current state • Required: consensus on desired outcome • “If we don’t know who owns the problem, it won’t get solved. ” John Shook • “Success depends on leadership having conversation around the problems, not the outcome” Steven Spear

Finding the problem: Root Cause Analysis • 5 Why’s • Flowcharts • Fishbone

5 Why Example Behind on Rx Refill Requests

5 Why Example Why Behind on Rx Refill Requests High Volume of Requests this Week

5 Why Example Why Behind on Rx Refill Requests High Volume of Requests this Week No Clinic Appointments Why

5 Why Example Why High Volume of Requests This week Behind on Rx Refill Requests Why Everybody at STFM Mtg No Clinic Appointments

5 Why Example Why Behind on Rx Refill Requests High Volume of Requests This week No Clinic Appointments Why It’s a great meeting Why Everybody at STFM Mtg

5 Why Example Why High Volume of Requests This week Behind on Rx Refill Requests Why I get to go to a workshop on PDCA No Clinic Appointments It’s a great meeting Why Everybody at STFM Mtg

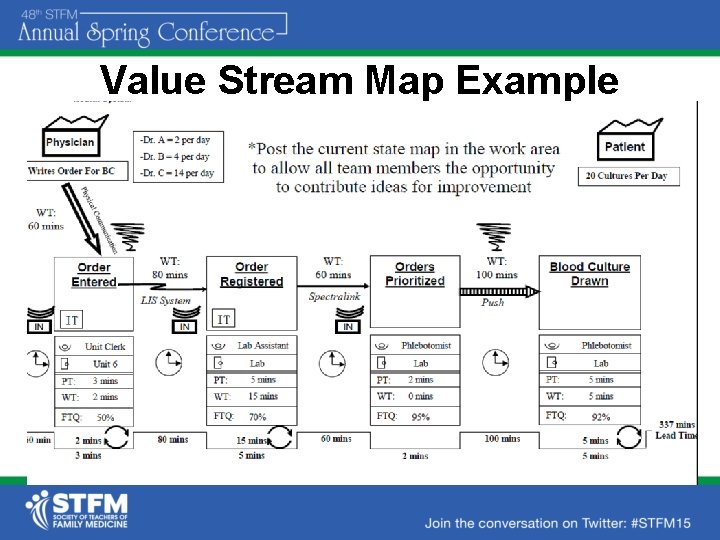
Flowcharts • Visual display of every step in a process • Can help identify: redundancy, complexity, delay, and waste in a process and answer the question “does each step add value? ” • Value Stream Mapping - LEAN

Value Stream Map Example

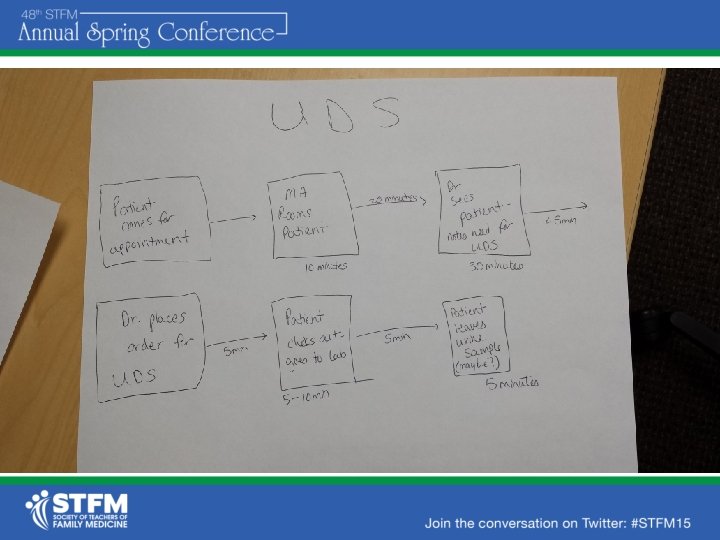
Flowchart - UDS

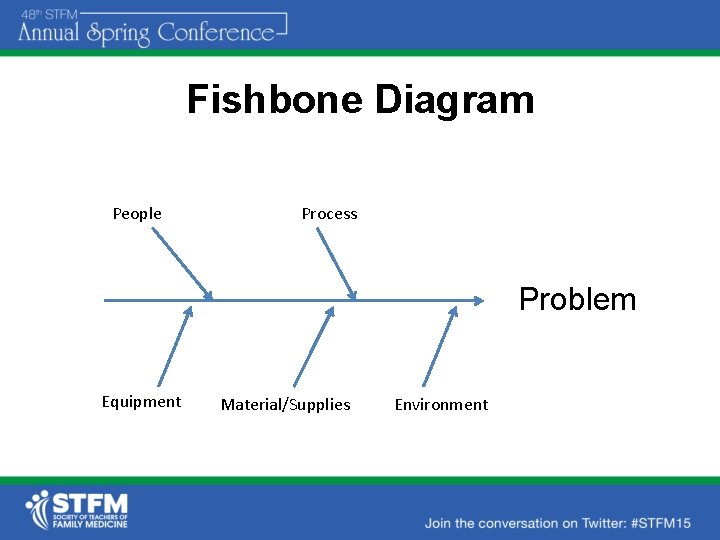
Fishbone Diagram • People, Process, Equipment, Materials, Environment • It helps teams understand that there are many causes that contribute to an effect • It graphically displays the relationship of the causes to the effect and to each other

Fishbone Diagram People Process Problem Equipment Material/Supplies Environment

Diabetic Foot Exam People Doctor forgets Process Done, not updated in EHR to capture data Not Done! Monofilament broken Equipment Monofilament not in exam room Material/Supplies Patient not in clinic for diabetes Environment (culture)

Know Normal From Abnormal. Right Now

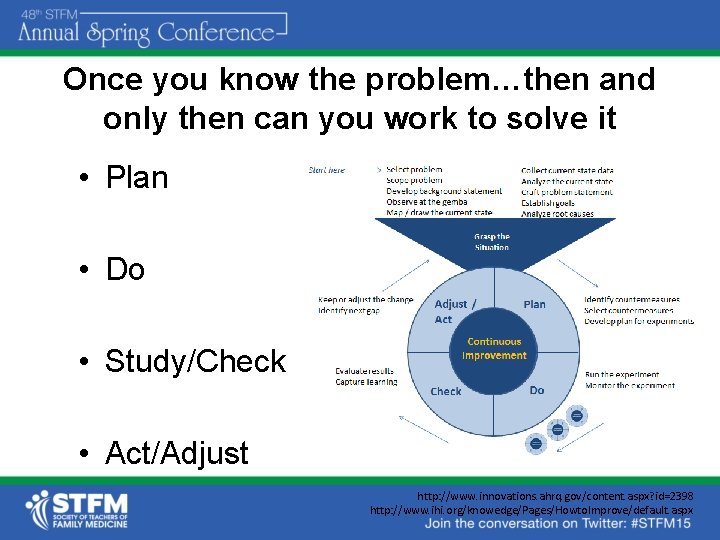
Once you know the problem…then and only then can you work to solve it • Plan • Do • Study/Check • Act/Adjust http: //www. innovations. ahrq. gov/content. aspx? id=2398 http: //www. ihi. org/knowedge/Pages/Howto. Improve/default. aspx

Plan • “A plan is an experiment you run to see what you don’t understand about the work” -Stephen Spear • “If you want to make God laugh, tell him your plans”. -Woody Allen • “When you’re not sure what to do next, that’s a good time to try something”. -John Long, MD

PLAN (with a capital P) • • • Have a well defined goal Form a team Clearly define your intervention List tasks needed to implement Assign responsibility, due dates Predict what will happen, determine how you will you define success

Data to Drive Change: Key Characteristics • Objective • Believable • Reproducible • Relevant • Accessible/Transparent

DO • Run the test • Suggest: small scale, pilot before larger scale if feasible “Just Do It” -Nike advertising campaign

Study/Check • How do the results compare to the predictions? • Reflection • If results differ from predictions, ask why? – Consider re-evaluating the original root cause analysis

Act/Adjust • Based on the P/D/S portions of the cycle: – What modifications need to be made for the next cycle? – What did you learn? – IF the plan is working…set a time frame for reevaluation (e. g. 30/60/90 days) – Streamline (eliminate wasted effort)

Final Thoughts • Make success understandable and doable • Make it easy to see problems • Make it clear what to do when a problem is encountered • Make it clear what will happen after notifying supervisor of a problem


STEP 1 • Generate a list of root causes that might contribute to low Chlamydia Screening rates – Use the technique of asking "why" 5 times, and/or use a fishbone diagram to evaluate for causes stemming from one of the main categories of problems: people, process, equipment, material/supplies, environment. • No Solutions!

STEP 2 What are your root causes?

STEP 3 Root Causes 1. Provider unaware of availability and reliability of urine testing 2. External labs not being captured into EMR 3. Providers not ordering at time of service 4. Providers uncomfortable ordering test due to sensitive nature of discussion 5. Patient not sexually active/declines testing NOW: Develop a PDSA plan using the worksheet

STEP 4/5 • Look at your data. Discuss with your small group: • Did your intervention have its intended impact? Why or why not? • What might you do as a next step? • What might you do differently next time?

Discussion • Why does standard work matter? • Did you find the “right root cause”? • Did you have consensus? • What will you try when you return to your own clinic/setting?

Contact Info Katy Harmes MD jordankm@umich. edu Grant Greenberg MD, MA, MHSA ggreenbe@umich. edu https: //twitter. com/Grant. G_MD http: //medicine. umich. edu/dept/family-medicine/ 734 -232 -6222 (for both of us!)

Please evaluate this session at: stfm. org/sessionevaluation