DAY 15 See your instructor get your number

DAY 15 See your instructor, get your number and worksheet for the day Bridge/warm up: talk with another about your experience Lecture: Cancer Caring for People Who are Terminally Ill Caring for People Who are Dying Apply it : practice care with each stage

CURRICULUM CONTENT TO TEACH Cancer on form of terminal illness Caring for People Who are Terminally Ill Caring for People Who are Dying

OBJECTIVES DAY 15 At the end of day the student will be able to: Discuss how a nursing assistant can assist a resident by being a good listener; Discuss different cultures and how culture can affect resident care Discuss the comfort care of the dying person; Discuss the care of the deceased resident.

WHO ARE TERMINALLY ILL OBJECTIVES Define terminal illness List the stages of grief and how it affects terminally ill person Define supportive and palliative care. Explain how these maintains quality of life What is the role of hospice? How caring for terminally ill people can affect the NA
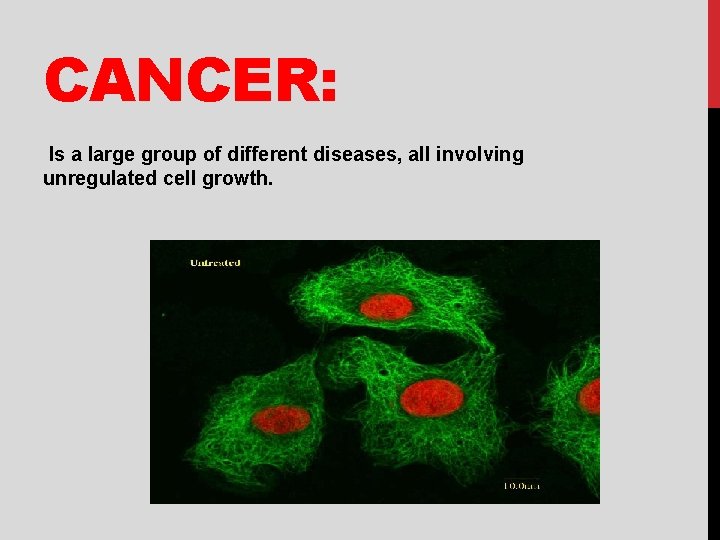
CANCER: Is a large group of different diseases, all involving unregulated cell growth.

TUMOR Mass of abnormal cells Benign non cancerous tumor Malignant cancerous tumor
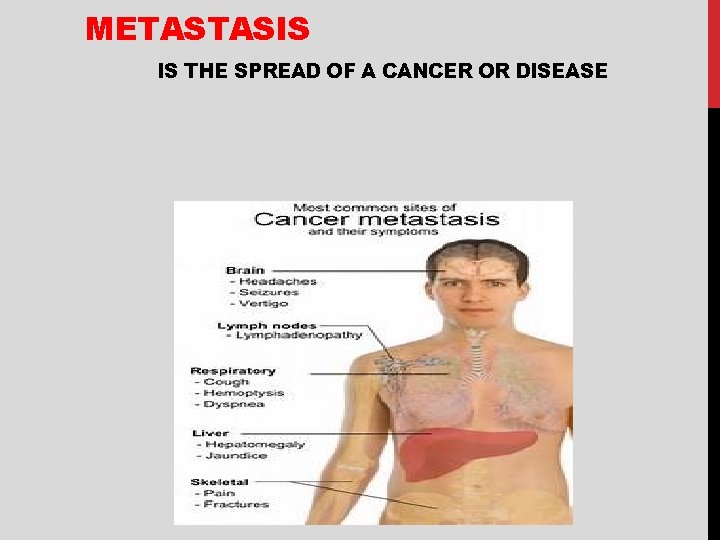
METASTASIS IS THE SPREAD OF A CANCER OR DISEASE

C CHANGE IN BOWEL MOVEMENTS OR BLADDER HIBITS A A SORE THAT DOES NOT HEAL U UNEXPLAINED WT LOSS, BLEEDING OR DISCHARGE T THICKENING OR LUMPS BREASTS & TESTICLES I INDIGESTION O OBVIOUS CHANGES IN WARTS OR MOLES N NAGGING COUGH, HORESENESS or difficulty swallowing
TREATMENTS Surgery Palliative care CHEMOTHERAPY:

CHEMOTHERAPY: (CHEMO) The use of medications to destroy malignant cancer cells. Stedman's

SIDE EFFECTS OF CHEMO OR RADIATION Wt loss, n/v Give fluids/food they can tolerate https: //www. google. com/search? q=aneroxia+picture&sa=X&rls=com. microsoft: en-US: IEAddress&nfpr=1&tbm=isch&tbo=u&source=univ&ved=0 ah. UKEwi. Tia. Xpu. IHa. Ah. WE 6 l. MKHZLMB 6 YQ 7 Ak. IRg&biw=392&bih=387#imgrc=Jk. Lzi 8 ql. By. EZTM: &spf=1521773509547
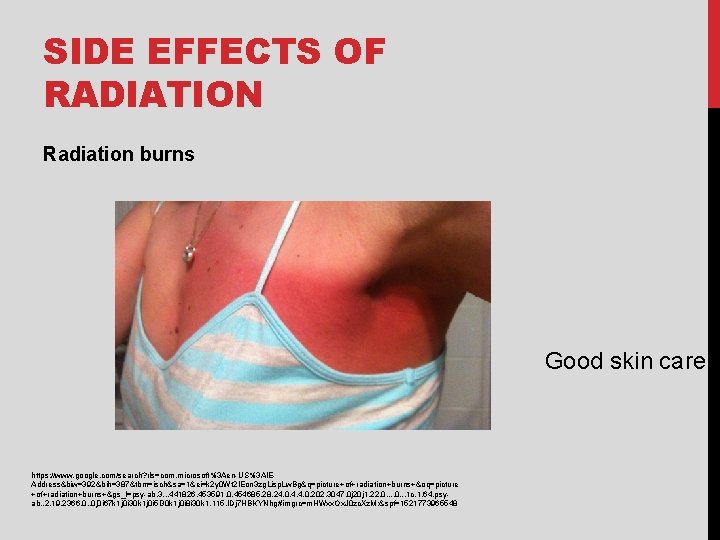
SIDE EFFECTS OF RADIATION Radiation burns Good skin care https: //www. google. com/search? rls=com. microsoft%3 Aen-US%3 AIEAddress&biw=392&bih=387&tbm=isch&sa=1&ei=k 2 y 0 Wt 2 IEon 3 zg. Lisp. Lw. Bg&q=picture+of+radiation+burns+&oq=picture +of+radiation+burns+&gs_l=psy-ab. 3. . . 441826. 453591. 0. 454685. 28. 24. 0. 4. 4. 0. 202. 3047. 0 j 20 j 1. 22. 0. . . 1 c. 1. 64. psyab. . 2. 19. 2366. 0. . 0 j 0 i 67 k 1 j 0 i 30 k 1 j 0 i 5 i 30 k 1 j 0 i 8 i 30 k 1. 115. IDj 7 HBKYNhg#imgrc=m. HWxx. Ox. J 0 zc. Xz. M: &spf=1521773965548
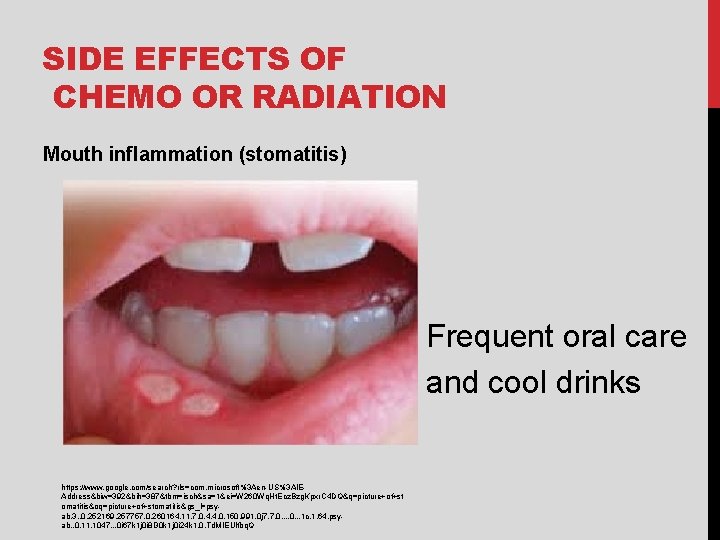
SIDE EFFECTS OF CHEMO OR RADIATION Mouth inflammation (stomatitis) Frequent oral care and cool drinks https: //www. google. com/search? rls=com. microsoft%3 Aen-US%3 AIEAddress&biw=392&bih=387&tbm=isch&sa=1&ei=W 260 Wq. Ht. Ecz. Bzg. Kpxr. C 4 DQ&q=picture+of+st omatitis&oq=picture+of+stomatitis&gs_l=psyab. 3. . 0. 252169. 257757. 0. 260164. 11. 7. 0. 4. 4. 0. 150. 991. 0 j 7. 7. 0. . . 1 c. 1. 64. psyab. . 0. 11. 1047. . . 0 i 67 k 1 j 0 i 8 i 30 k 1 j 0 i 24 k 1. 0. Td. MIEUlfbq. Q

SIDE EFFECTS OF CHEMO OR RADIATION Fatigued (over tired) Offer exercise with periods of rest

SIDE EFFECTS OF CHEMO OR RADIATION Neutropenia: low white blood cells -Immunocompromised - Increased risk for infection https: //brevis. com/images/cca. neuback. jpg

SIDE EFFECTS OF CHEMO OR RADIATION Pain Good pain management program Reporting is key management Being there to listen and report changes

EMOTIONAL NEEDS Holistic approach-mind, body , spirit With the changes choices is all they have Don’t push them to talk Let them know that you are here for them Sitting or holding a hand may all they need.

Palliative care includes: . • Administration of medications to control pain • Use of chemotherapy or radiation to shrink a tumor • Use of oxygen therapy to help keep a person with breathing problems comfortable • Surgical procedures to remove a tumor that is interfering with the functioning of an organ system

CARING FOR PEOPLE WHO ARE TERMINALLY ILL

TERMINAL ILLNESS: Illness or injury that recovery is not expected.

DEATH AND DYING A Swiss American psychiatrist, a pioneer in Near-death studies The author of the groundbreaking book On Death and Dying (1969), where she first discussed what is now known as the Kübler-Ross model. [1] (Stage of grief)

LOSS Someone or something is taken from us Like (person, place, thing)

GRIEF To be very sad

GRIEVING PROCESS: Mourning the loss The stage a person having loss will progress through. The 5 stages of grief by Elizabeth Kubler-Ross.

STAGES OF GRIEF – Denial, Anger, Depression, Bargaining, Acceptance (DABDA)

DENIAL: One of the stages of grief; Person refuses to accept the diagnosis, unable to accept; unaware

ANGER: One of the stages of grief; Feelings of rage, which may be directed toward herself or others.

BARGAINING: One of the stages of grief; The person wants to "make a deal“

DEPRESSION: One of the stages of grief; Experiences sadness and regret.

ACCEPTANCE: One of the stages of grief; Person comes to terms with the reality of his or her own impending death, and is finally at peace with this Knowledge. Stedmans

HOPE Throughout the grieving process, hope usually persists EXAMPLES: There is hope that a cure will be found Hope helps the person face another day or another painful treatment Hope drives the person to keep normal activities, such as eating etc… Responsibilities of a nursing assistant • Be responsive to, • Nurture a person’s hope, without being unrealistic

Empathy: To try to understand how another feels

DYING WITH DIGNITY

DYING Gradually ceasing to live; to the point of death

RIGHT TO MAKE HEALTHCARE WISHES KNOWN THROUGH ADVANCE DIRECTIVES AND DURABLE POWERS OF ATTORNEY Occurs on admission and changed per their desires Advance directive A document that allow the person to make his/her wishes regarding health care to family or health care worker. Incase he/she is unable to speak for oneself

http: //www. time. com/time/specials/packages/article/0, 28804, 1864940_18649 39_1864909, 00. html http: //en. wikipedia. org/wiki/Terri_Schiavo_case Terri Feb 1990 Karen April 1975 Removal of ventilator Removal of tube feeding (enteral) feeding

OBJECTIVE Two major type of advance directives Ways Durable power of attorney for health care Living will

Living will: legal paper saying how you want to be cared for Requests that death not be artificially postponed.

Directives An advance directive is a document in which a person makes his or her wishes known regarding health care in case the time comes when he or she is no longer able to Durable power of attorney for health care transfers the responsibility for medical decisions to a family member or friend to make in the event the person is no longer able to so.

PSDA – Patient Self-Determination Act of 1990 Ensures that the wishes of patients and patients’ family members are followed

POLST Physician's Orders for Life-Sustaining Treatments A quick overview of the patients wishes for care if unable to express these desires.

Life support: Techniques used to maintain life Machine that breathes for us Life-sustaining treatments tend to be more aggressive Examples are: • Respiratory ventilation • Cardiopulmonary resuscitation (CPR) • The placement of a feeding tube or intravenous (IV) line for the provision of nutrition • Antibiotics

DNRDO NOT RESUSCITATE CODE all life saving measures

PALLIATIVE (PAL-LEE-UHTIV) CARE INCLUDES: Focused on providing relief from the symptoms and stress of a serious ness. Medications to control pain Use of chemotherapy or radiation to shrink a tumor Use of oxygen therapy to help keep a person with breathing problems comfortab Surgery to remove a tumor that is interfering with the functioning of an organ system The goal is to improve quality of life for both the patient and the family.

Supportive care Offers treatments that will not prolong life but will make a person more comfortable Examples are: • • • Oxygen therapy Nutritional supplementation Pain medication Range-of-motion exercises Grooming and hygiene Positioning assistance

Information regarding legislation related to the right to die and assisted suicide can be found at http: //www. euthanasia. com http: //www. wnd. com/2005/03/29516/

Hospice care: care of the dying person To maintain their comfort with providing physical, emotional, spiritual needs Hospice agencies • Offer the terminally ill person the best quality of life possible • Ensure the person’s comfort and dignity

Friday, June 13, 2008 http: //myhospicehelp. blogspot. com/2008/06/dying-persons-bill-ofrights. html Dying Person's Bill of Rights I have the right to be treated as a living human until I die. I have the right to maintain a sense of hopefulness, however changing its focus may be. I have the right to be cared for by those who can maintain a sense of hopefulness, however changing this may be. I have the right to express my feelings and emotions about my approaching death in my own way. I have the right to participate in decisions concerning my care. I have the right to expect continuing medical and nursing attention even though “cure” goals must be changed to “comfort” goals. I have the right to not die alone. I have the right to be free of pain. I have the right to have my questions answered honestly. I have the right to retain my individuality and not be judged for my decisions, which may be contrary to the belief of others. I have the right to expect that the sanctity of the human body will be respected after death. I have the right to be cared for by caring, sensitive, knowledgeable people who will attempt to understand my needs and will be able to gain some satisfaction in helping me face my death.

COMMUNICATION WITH A TERMINALLY PERSON Talk like you would with anyone else No one-size-fits-all dialogue Asking open-ended questions Listen with empathy Be real

CARING FOR PEOPLE WHO ARE DYING Dying: A gradual systemic shutdown, followed by an absence of criteria that define life http: //cvc 3. coastline. edu/modelcvc 3 courses/elliswaller/lesson 13. htm

DEATH AND DYING: Death -process of leaving the world Death the cessation of all vital functions of the body. Dying -Process of no longer living Dying is the process of approaching death. "final stage of growth"

END OF LIFE CARE Care given during dying process

Have you cared for someone who is dying? How did you feel If you have ever care for someone who denied treatment or not want any more treatment? How did you feel?

END OF LIFE CARE Be a good listener LIFhttps: //www. google. com/search? q=end+of+life+care&rlz=1 C 2 CAFB_en. US 643&biw=785&bih=733&tbm=isch&imgil=c. Prq. SSH 2 pqgc 7 M%253 A%253 B-Ri 8 Bkb. JVgnu. M%253 Bhttp%25253 A%25252 Fwww. cambridgeshireandpeterboroughccg. nhs. uk%25252 Fend-of-life-care. htm&source=iu&pf=m&fir=c. Prq. SSH 2 pqgc 7 M%253 A%252 C-Ri 8 Bkb. Vgnu. M%252 C_&usg=__p 8 tavv 1 b 12 z. DAGa. Sh. ONCRLFm. AVw%3 D&ved=0 CCUQyjdq. FQo. TCJ 657 uezi. Mc. CFUORDQodi. IUFAQ&ei=Sw. G 9 Vd 7 n. A 8 Oi. Noi. Llgg#imgrc=ga. X 9 m 4 z. U_ok. PYM%3 A&usg

COMFORT CARE: (comfort measures) – things that makes your resident feel good Is aimed at relieving symptoms, enhancing the quality of remaining life, and easing the dying process.

Holistic Approach to Care Physical and emotional needs varies • Dying stages • Person preferences

Holistic Approach To Care The nursing assistant’s role • • Honor person’s right to die peacefully with dignity Be a good listener Be careful not to unconsciously compromise care Be aware of your own feelings about death

Effects on the Nursing Assistant May go through similar grief May feel inadequate at not being able to relieve a person’s suffering May question his or her professional calling Should talk to someone trusted about his or her feelings Should take time for himself or herself

Physical Signs of Impending Death Circulatory System Changes http: //cvc 3. coastline. edu/modelcvc 3 courses/elliswaller/lesson 13. htm Blood pressure drops Pulse becomes rapid and weak Skin feels cool and clammy, despite rise in body temperature May perspire heavily Skin may appear mottled (blotchy), very pale, cyanotic (bluetinged), or grayish

Physical Signs of Impending Death Respiratory System Changes Cheyne-Stokes respiration • Irregular, shallow breaths • Alternating fast-slow pattern • Periods of apnea Fluid or mucus may collect in the air passages, causing the noisy, rattling breathing called “death rattle”

Physical Signs of Impending Death Digestive System Changes Nausea Vomiting Abdominal swelling Fecal impaction, or bowel incontinence May not want food or water • Offer ice chips • Provide frequent oral hygiene

Physical Signs of Impending Death Urinary System Changes Decreased blood flow Decreased urinary output Urinary incontinence

Physical Signs of Impending Death Nervous System Changes Decreased muscle tone & relaxed causing weakness Loss of ability to speak Loss of sensation in the arms or legs Diminished pain Blurred vision Hearing remains normal

Physical Signs of Impending Death Mental Status Changes May lose consciousness (comatose) As consciousness diminishes, so does pain May drift in and out of a semi-comatose state May become alert and oriented right to death

EMOTIONAL SUPPORT Someone to understand you Offer care as directed by person

Meeting the Dying Person’s Emotional Needs Fears regarding death, including • • A fear of the unknown A fear of losing dignity and self-control A fear that death will be painful A fear about the effects on the people left behind People may have concerns about • Unfinished business • Facing death alone Cultural and religious beliefs influence feelings about death

Meeting the Dying Person’s Emotional Needs A nursing assistant role • • • Be a good listener Check on the person frequently and regularly Reassure you are close by if she needs anything Provide physical contact when speaking to her Comfort her with a back massage Respect cultural and religious beliefs, even if you do not share these beliefs

EMPATHY/EMPATHETIC To try to understand how another feels

VISITORS Emotional time for all those involved. Important time and reassuring Remember the right to privacy

INFORMATION REGARDING CULTURAL BELIEFS RELATED TO DEATH CAN BE FOUND AT: http: //www. medscape. com/viewarticle/525639 http: //www. factbites. com/topics/Culture-of-death .

Providing Holistic Care Holistic care involves meeting a person’s emotional and physical needs Holistic care: • • Being patient, and understanding the underlying fears the person may have Spending more time with the person Keeping in mind the stages of grief Not being judgmental about the role the person’s actions may have had in causing his or her disease • Accepting decisions the person makes concerning his or her quality of life
CARE OF THE DYING PERSON SKIN CARE SPIRITUALITY RE-POSITIONS HYDRATION ORAL CARE FAMILY EMOITIONAL CARE COMFORT PRIVACY COMMUNICATION GOOD LISTENER

Meeting the Dying Person’s Physical Needs Care of the skin • Frequent skin care and linen changes • Regular checks for urine and fecal incontinence Care of the mucous membranes • Frequent mouth care • Remove mucus crust from eyes • Application of ointment, moist eye pads, lubricants Positioning • Frequent position changes

Meeting the Dying Person’s Physical Needs Other comfort measures • • Provide back massage Play soft music Give enemas Provide suctioning and oxygen therapy Keep the room well lit and ventilated Remove soiled linens, bedpans, or emesis basins Use air freshener to eliminate unpleasant odors

RIGIDITY: Inflexible, set, hard or Stiffness, inability to bend or be bent

RIGOR MORTIS – The stiffening of the muscles that usually develops within 2 to 4 hours after death

Postmortem Care: Your Duties If you are present at time of death • Notify the nurse and note the time • You may need to document the absence of vital signs

How do feel about touching a dead body? Is it OK for you to attend funeral ? Postmortem practices you seen?

POST MORTEM CARE: Care of the body after death
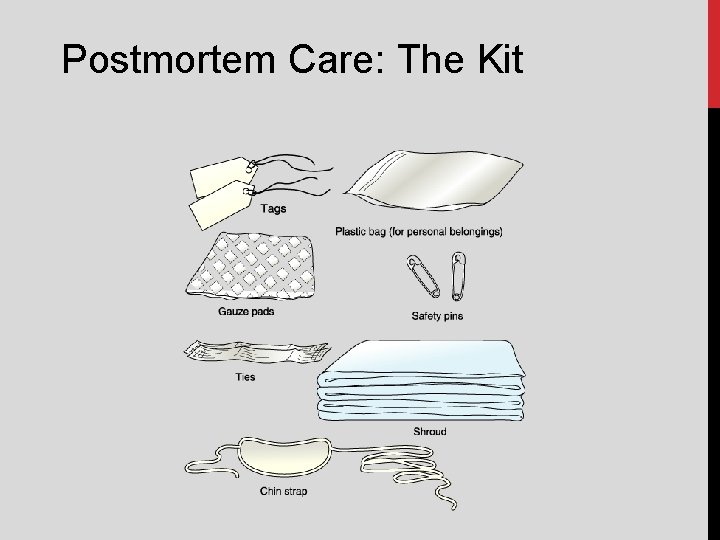
Postmortem Care: The Kit

Postmortem Care: Autopsy • Examination of the person’s organs and tissues after the person has died

RELATED WORKS A person who has died (Deceased, expired) Interment- burial, typically with funeral rites

APPLY IT Practice care for the stages of death

E TICKET your role in the dying process Define living will , comfort care and post mortem care List one way to meet physical needs of the dying List one way to meet the emotional needs of the dying List one way to meet the spiritual needs of the dying
- Slides: 84