Data analysis by hospitals Data analysis by payers

Data analysis by hospitals. Data analysis by payers. RIC DRG Workshop Belgrade, 18 -22. November 2013.

ELEMENTS OF DATA MANAGEMENT • Data reporting policies and specifications – Data dictionary – Data set specification (eg NMDS) – Data entry tools – Data extraction tools – Data edits and validation processes • Data warehousing functions – (incl) metadata management, data access • Data analysis reporting DRG Workshop Belgrade, 18 -22. November 2013.
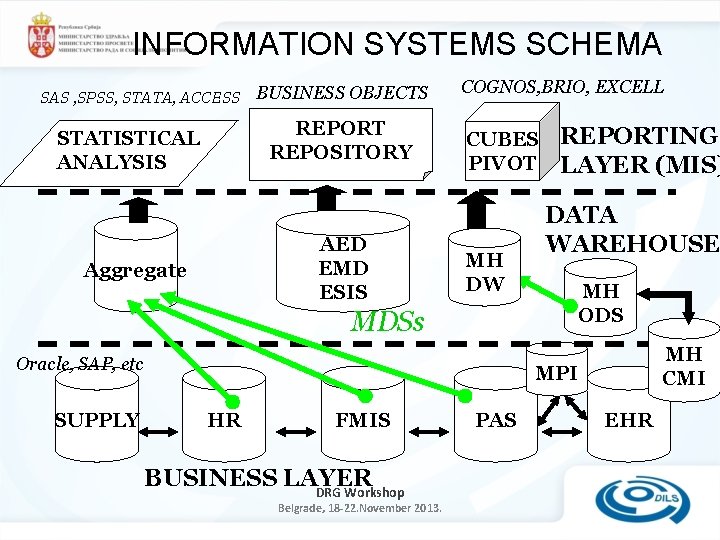
INFORMATION SYSTEMS SCHEMA SAS , SPSS, STATA, ACCESS BUSINESS OBJECTS REPORT REPOSITORY STATISTICAL ANALYSIS AED EMD ESIS Aggregate COGNOS, BRIO, EXCELL CUBES PIVOT MH DW MDSs Oracle, SAP, etc SUPPLY REPORTING LAYER (MIS) DATA WAREHOUSE MH ODS MH CMI MPI HR FMIS BUSINESS LAYER DRG Workshop Belgrade, 18 -22. November 2013. PAS EHR
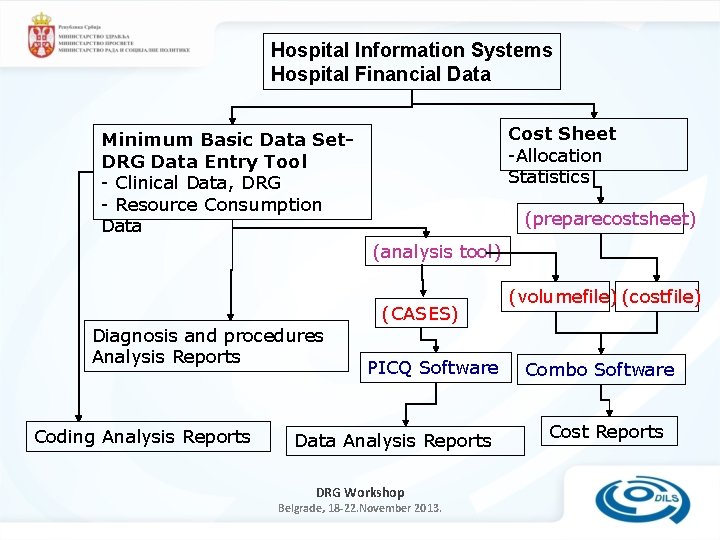
Hospital Information Systems Hospital Financial Data Cost Sheet -Allocation Statistics Minimum Basic Data Set. DRG Data Entry Tool - Clinical Data, DRG - Resource Consumption Data (preparecostsheet) (analysis tool) (CASES) Diagnosis and procedures Analysis Reports Coding Analysis Reports PICQ Software Data Analysis Reports DRG Workshop Belgrade, 18 -22. November 2013. (volumefile) (costfile) Combo Software Cost Reports

REPORTING FEEDBACK • The key to – GOOD DATA – EFFICIENCY GAINS – PERFORMANCE IMPROVEMENT • The basis for rational planning • A primary mechanism to assess innovation and investment priorities. DRG Workshop Belgrade, 18 -22. November 2013.

Standard reports may include • • • Productivity Complexity Allocative efficiency Technical efficiency Coding Completeness And various quality indicators – Outcome – Process • Some examples follow … DRG Workshop Belgrade, 18 -22. November 2013.

Productivity • Performance in total Weighted Episode (WEs) of all hospitals • Overall performance in total WEs against target by hospital • WEs by Major Diagnostic Categories (MDC) for Medical Diagnosis Related Group (DRGs) by hospital • WEs by MDC for Procedural DRGs by hospital • Top 10 increment DRG families by hospital • Top 10 decrement DRG families by hospital DRG Workshop Belgrade, 18 -22. November 2013.

Complexity – Casemix Index of Medical and Procedural DRGs of all hospitals – Casemix Index (CMI) by MDC by hospital – Average WEs per patient by MDC in by hospital – Average number of episodes per patient by MDC by hospital – Casemix – “ 1 Year On” DRG Workshop Belgrade, 18 -22. November 2013.

Allocative Efficiency • Percentage same day episodes by MDC of Medical and Procedural DRGs by hospital • Change in same day episodes of Ambulatory Medical DRGs • Percentage of episodes admitted via A&E Department by MDC by hospital DRG Workshop Belgrade, 18 -22. November 2013.

Technical Efficiency • Average Length of Stay (ALOS) of Medical & Procedural DRGs of all hospitals • Change in ALOS by MDC by hospital • Cost per weighted DRG by hospital DRG Workshop Belgrade, 18 -22. November 2013.

Coding Completeness – Percentage of total multi-day episodes for Medical and Procedural DRGs by severity level in all hospitals – Percentage of total multi-day episodes with Major Comorbidities and Complication (MCC) by MDC for Medical DRGs by hospital – Percentage of total multi-day episodes with MCC by MDC for Procedural DRGs in all hospitals – Percentage of total multi-day episodes with MCC by MDC by hospital – WE / CMI by discharged specialty: 4 -year trend analysis by hospital DRG Workshop Belgrade, 18 -22. November 2013.

WHY IS PATIENT LEVEL COSTING SO IMPORTANT? DRG Workshop Belgrade, 18 -22. November 2013. 12

The proposition Tracking utilisation to patients is actually more important than simply accurate cost weights. DRG Workshop Belgrade, 18 -22. November 2013.

How can this be true? MP Ann Clwyd wept in the House of Commons as she described t c= how her husband [Owen] died 'like a battery hen' r ? s e c Labour MP Ann Clwyd says her biggest regret was that she an didn't 'stand r su'callous lack of in the hospital corridor and scream'3 in protest of the n i lth a care' the NHS nurses showed her husband, as he e lay dying of hospital th u acquired pneumonia. Ann describes her husband's final days, crushed bo a s t achospital bed, wearing an 'like a battery hen' against the bars of his f / le c i t oxygen mask that was so tight it cut /his ar face and pumped cold air in to om his infected eye. Owen died after. csuffering 10 days of this treatment at e c the NHS University Hospital rof an Wales in Cardiff. Following her husband's u s n i death, the MP publicly spoke out on the 'normalisation of cruelty' that lth a e has become 'commonplace' in NHS hospitals. Owen had battled MS for 0 h 1 p 30 years, yet died to of hospital-borne pneumonia. Shockingly, around. w w 4 100, 000 patients catch an infection in UK hospitals every year, from : //w p t ht people sadly die. DRG Workshop which 5, 000 ab Belgrade, 18 -22. November 2013.

KEY POINTS 1. Good data for clinical care monitoring (inputs utilization analysis) is also good costing data. 2. Utilization by case type gives accurate detailed costing – AND benchmarking patient level variability is vital for both pricing and quality-of-care management. 3. Clinicians should be the primary users of utilization data and analyses – CLINICAL BEHAVIOURS << CLINICAL CULTURES << OPERATIONAL USE OF DATA 4. Key immediate strategies. DRG Workshop Belgrade, 18 -22. November 2013.

PRICING HEALTHCARE • 1. Improve data quality • 2. Increase comparability and consistency of data • 3. Improve transparency • 4. Develop the potential for new pricing mechanisms • 5. Proportionate regulatory cost • 6. Improve the use of cost data by managers DRG Workshop and clinicians Belgrade, 18 -22. November 2013.
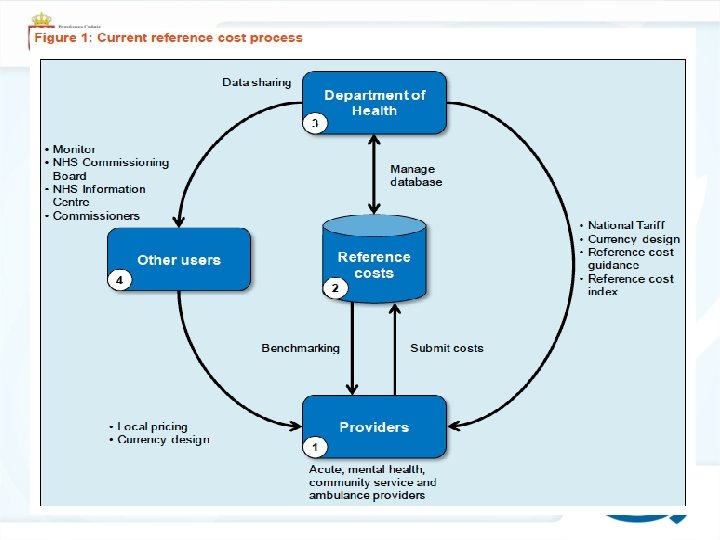
DRG Workshop Belgrade, 18 -22. November 2013.
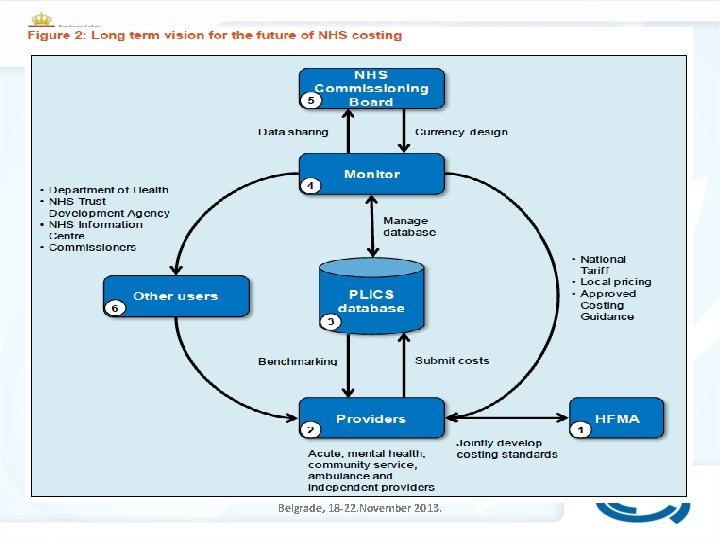
DRG Workshop Belgrade, 18 -22. November 2013.
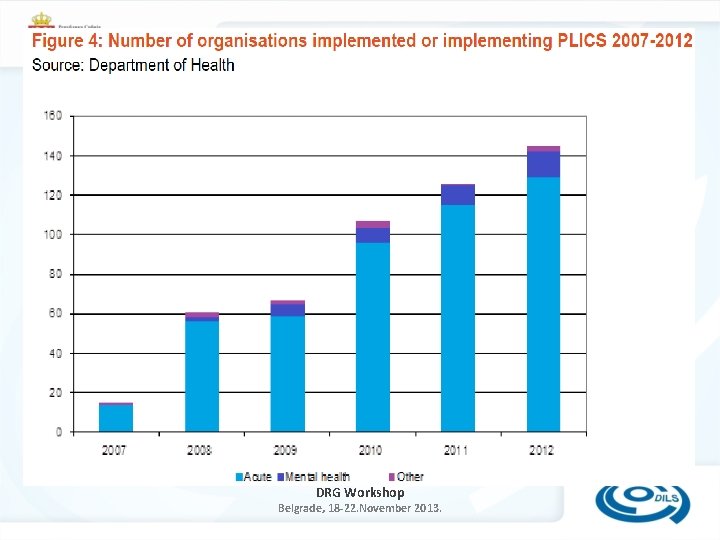
DRG Workshop Belgrade, 18 -22. November 2013.
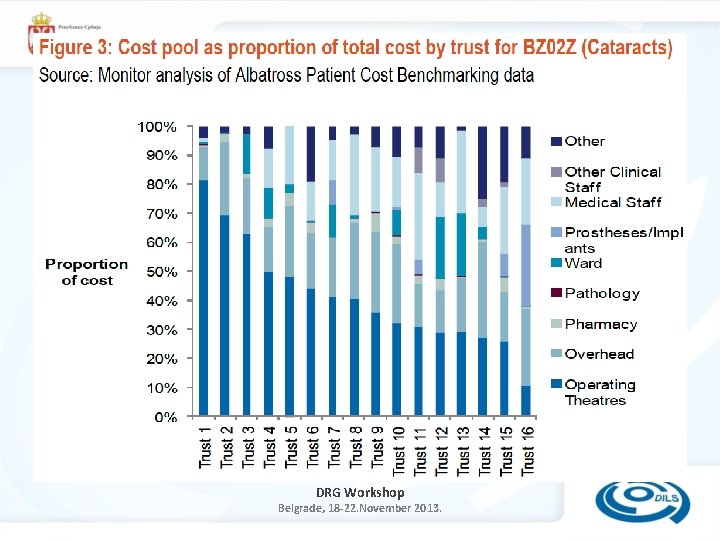
DRG Workshop Belgrade, 18 -22. November 2013.
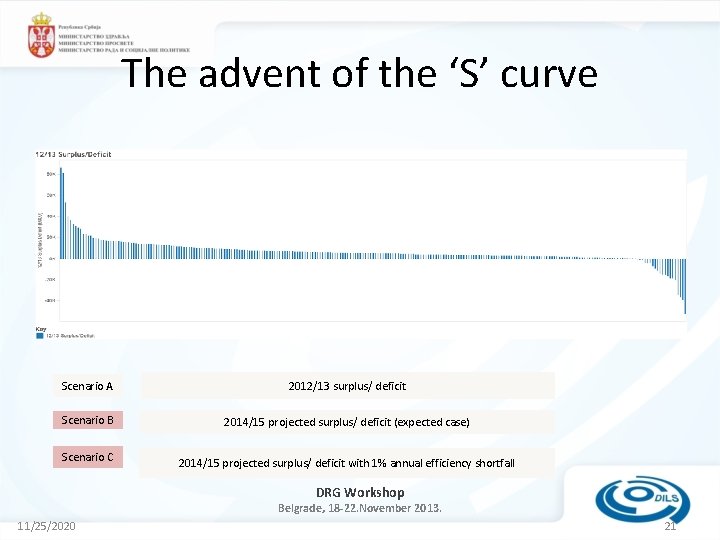
The advent of the ‘S’ curve Figures in £ 000 s) Scenario A 2012/13 surplus/ deficit Scenario B 2014/15 projected surplus/ deficit (expected case) Scenario C 2014/15 projected surplus/ deficit with 1% annual efficiency shortfall DRG Workshop Belgrade, 18 -22. November 2013. 11/25/2020 21
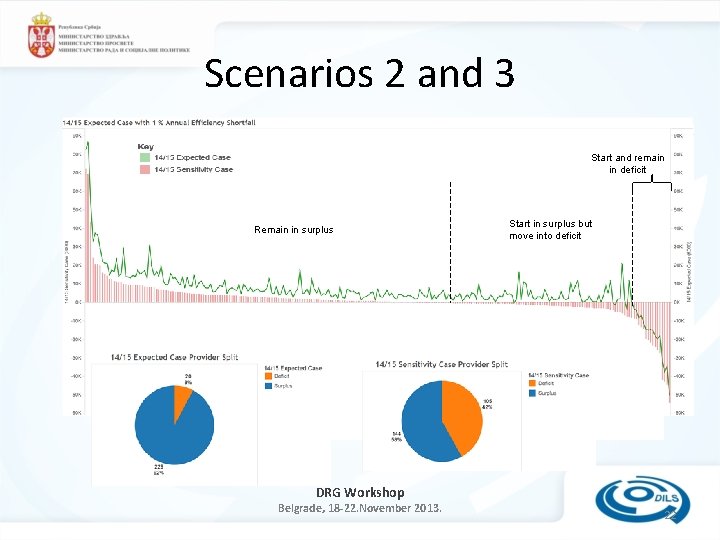
Scenarios 2 and 3 Start and remain in deficit Remain in surplus Start in surplus but move into deficit DRG Workshop Belgrade, 18 -22. November 2013. 22

The two key questions 1. How do we get the right data from costing systems into regular clinical review use? 2. How do we better enable clinicians to take the lead in performance improvement? DRG Workshop Belgrade, 18 -22. November 2013.

QUESTION 1. • How do we get the right data from costing systems into regular clinical review use? DRG Workshop Belgrade, 18 -22. November 2013.

RELEVANCE Kane Gorny, 22, left to die of thirst in an NHS London hospital Kane Gorny, an active 22 -year-old, had already bravely beaten cancer the year before and needed a routine hip replacement due to the treatment. Whilst recovering from this simpleyo operation, u e r his doctors u s Kane suffered unthinkable neglect at the hands of n. e t i o t d e y Tooting. Having e a n and nurses in St. George's NHS hospital, been w u e althi o e n h y t o u nfor water; facdriven srefused his e i abo by s h t denied his medication and pleas e w c , n t a ticle/ n r r a e / u m s m 999 anfrom tcalled n i thirst and desperation, Kane a e. co his hospital bed. c e h r t t r l t ea the police h insu h t g l i a r e …Hwhen But arrived to his aide, they were maliciously h e 0 1 h p t o t. e by hospital v wwstaff i w / e / : turned away who claimed he was delirious. Kane c p htt re ] ? ? died of dehydration ? ! !!!! ce? src=tab just hours later! Whilst his grieving mother took [ n a moment to sit with her son's body, a nurse then heartlessly nsura asked if she was finished so that they could 'bag him up'1. Disgustingly, Kane's case not alone; 4 people die of DRG is Workshop Belgrade, 18 -22. November 2013. dehydration every day in our hospitals 2.

The locus of efficiency and effectiveness “EVERY CLINICAL DECISION IS AN EXPENDITURE DECISION” DRG Workshop Belgrade, 18 -22. November 2013. Don Hindle

Look! You spent too much on patient 15644 But patient 15644 was different from normal DRG Workshop Belgrade, 18 -22. November 2013. Don Hindle

I've checked, and patient 15644 wasn't different at all! Sorry, I'll try not to do it again DRG Workshop Belgrade, 18 -22. November 2013. Don Hindle
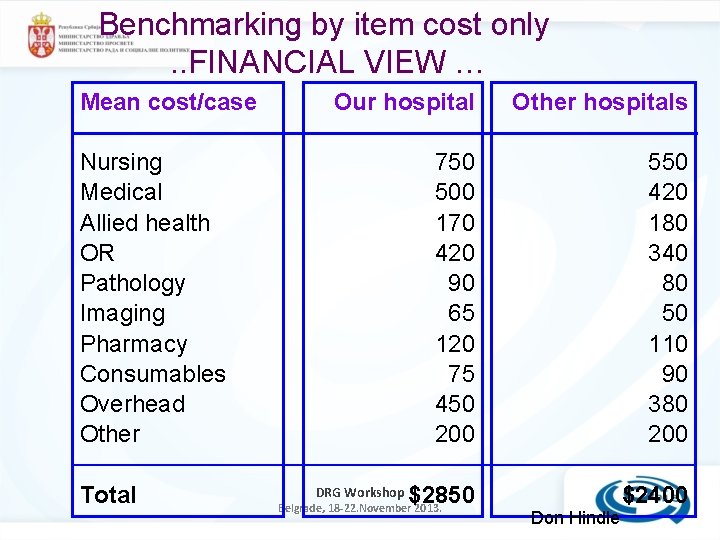
Benchmarking by item cost only. . FINANCIAL VIEW … Mean cost/case Our hospital Other hospitals 750 500 170 420 90 65 120 75 450 200 550 420 180 340 80 50 110 90 380 200 $2850 $2400 Nursing Medical Allied health OR Pathology Imaging Pharmacy Consumables Overhead Other Total DRG Workshop Belgrade, 18 -22. November 2013. Don Hindle
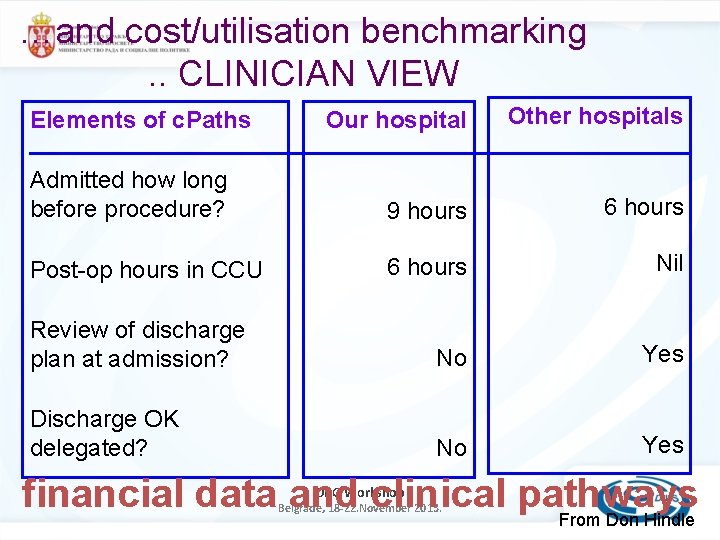
…and cost/utilisation benchmarking. . CLINICIAN VIEW Our hospital Other hospitals Admitted how long before procedure? 9 hours 6 hours Post-op hours in CCU 6 hours Nil Review of discharge plan at admission? No Yes Discharge OK delegated? No Yes Elements of c. Paths financial data and clinical pathways From Don Hindle DRG Workshop Belgrade, 18 -22. November 2013.

TIMELINESS • We need to be able to review whether changes are working • We need to be able to correct and steer regularly – monthly – weekly • We need to be able to check immediate activity against norms – agreed protocols - to guide decisions and choices DRG Workshop Belgrade, 18 -22. November 2013.
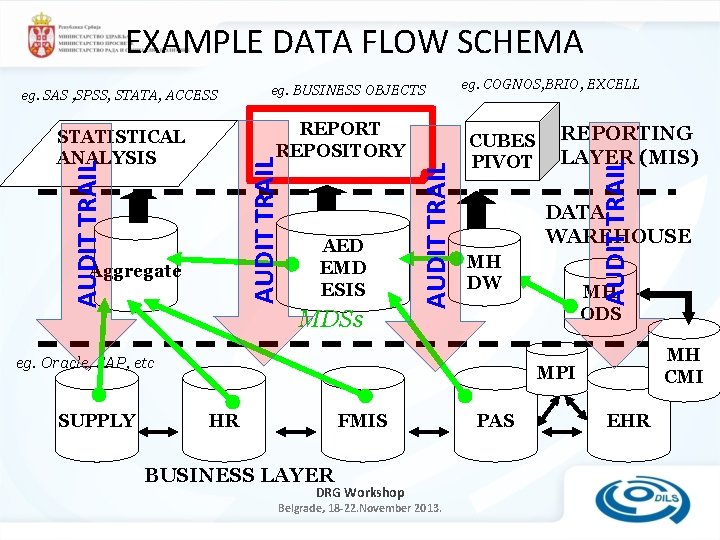
EXAMPLE DATA FLOW SCHEMA eg. BUSINESS OBJECTS AUDIT TRAIL Aggregate AED EMD ESIS MDSs AUDIT TRAIL REPORT REPOSITORY STATISTICAL ANALYSIS eg. COGNOS, BRIO, EXCELL CUBES PIVOT DATA WAREHOUSE MH DW eg. Oracle, SAP, etc SUPPLY REPORTING LAYER (MIS) AUDIT TRAIL eg. SAS , SPSS, STATA, ACCESS MH ODS MH CMI MPI HR FMIS BUSINESS LAYER DRG Workshop Belgrade, 18 -22. November 2013. PAS EHR

GRANULARITY • • Why are the costs higher / lower? What are we doing differently? Are our patient-type ratios different? Are we differentiating – tailoring the pathways to different patients – is our variability matching standard patterns DRG Workshop Belgrade, 18 -22. November 2013.

QUESTION 2. • How do we better enable clinicians to take the lead in performance improvement? DRG Workshop Belgrade, 18 -22. November 2013.

Clinical process review • • Patient journey Clinical pathway Evidence based practice Variance analysis DRG Workshop Belgrade, 18 -22. November 2013.

QUESTION 3 • How can clinicians match best practice and properly accommodate natural patient variability? DRG Workshop Belgrade, 18 -22. November 2013.

Culture eats reform for breakfast • “I am a doctor/nurse not a manager – I care for people not ‘cases’. Everyone is different. ” • Is the care team or the individual responsible • “Why are we doing this type of case differently? ” • What is the evidence that it works better? • “How can we redeploy the savings if we can achieve less costly practice? ” DRG Workshop Belgrade, 18 -22. November 2013.

So. . how well are we doing? Elderly and frail 'Mrs H'5 bruised, soaked in her own and ou urine h y t ig ns heavily dishevelled under NHS 'care' a h h t a atio l o a Mrs H was an independent 88 -year-old, u living in her own t r or thome - until she u t p Mrs H suffered f Trust, a e had a fall. Admitted to the Heart ofy. England NHS n r d g ing l a cbroken re ocollar n a n further disturbing ailments, including bone. Upon her o d n r t a s ' s voiced e concern t the nmanager i to over ther a e m transferral to a new care home, , l v , ab l n d i a s = o e l c i h tclothing that re ein srwas not al treat state. bruised, soiled andfdistressed She arrived s ? n u e e s att o ti reclips, s i anc bags of r l e i u her own, heldreintplace by large paper along with several b fac e p ins r e h o t l o t e w Sadly e. H died t Mrs ea into her cruel dirty clothes. before the investigation m t m h u i t n a t u e a riv o t bo y s w a a s f s treatment was complete and the NHS Trust admitted their failings. An c t I P i d e c l l a : d f / u rd 6 acomplaints nd n de are made icleabout the NHS every single astonishing t r wo nda 3, 000 /a a d. m l o c a ho that s'care' week, stillustrating the core t. c principle of nursing seems to be s e n t c n e practice. n from ra up rapidly tiits a u t disappearing NHS nurses even claim the new a s l o n i p t u h al 0 healt nofsuniversity-trained generation nurses believe basic care tasks, such as u o c ivid top 1 7. . bathing their patients, are 'beneath them' DRG Workshop d w w n i //w : http Belgrade, 18 -22. November 2013.

Definition of Clinical Pathways • Systematically developed written statements that: • Are evidence based • Incorporate the views of clinicians (medical, nursing, allied health) patients and managers • Prospectively describe how care will provided and how effectiveness, quality and efficiency will be monitored and assessed. DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

A clinical pathway enables a clinical team to: Ø prospectively describe the sequence of diagnostic and therapeutic events whose occurrence or non-occurrence will significantly affect quality, cost and outcome. Ø prospectively define the quality and outcome indicators that it will use to judge its performance. Ø prospectively cost the care that it provides and in so doing defines the cost indicators that it will use to judge its efficiency. Ø routinely and consistently monitor its performance on quality and cost Øalter its method for treating a condition, in light of what it [systematically] has learned about treating the condition. DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

Characteristics of Integrated care pathways Prospectively Costed Quality indicators Clinical Pathway Routine Review of Variance Outcome Indicators DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling
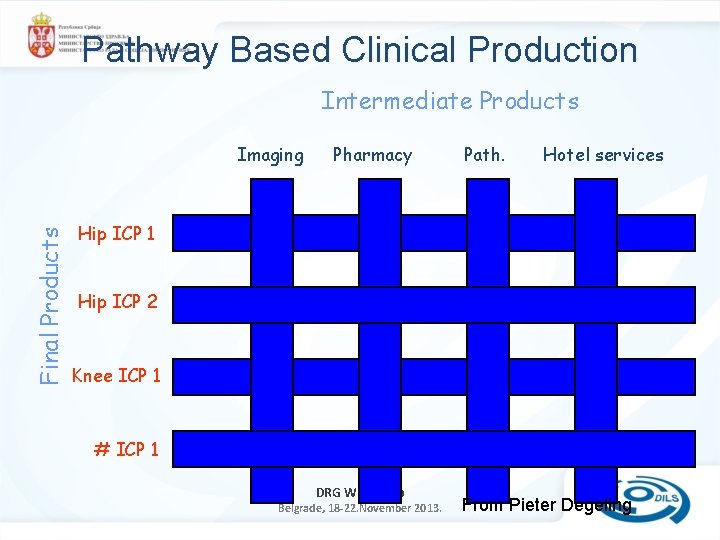
Pathway Based Clinical Production Intermediate Products Final Products Imaging Pharmacy Path. Hotel services Hip ICP 1 Hip ICP 2 Knee ICP 1 # ICP 1 DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

Important provisos • CPs are not immutable documents setting out inviolable treatment regimens. • The existence of a pathway does not obviate clinicians’ responsibility to make clinical judgements and to tailor care according to their assessment of the clinical needs of individual patients. • Thus clinical variation remains a ‘to be expected’ (in the sense of an often required) feature of clinical practice. • The matter at issue is what a clinical team can learn from these variations and how they can systematize this learning. • Accordingly, when the care process varies from that described in the pathway, the reasons for the variance are recorded and become the focus of structured across-profession conversations described above. DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

High volume case types – how many pathways? Within a 600 -700 bed DGH in the NHS Ø Emergency admissions account for 53% of all inpatient episodes and 83% of all bed days consumed within the Trusts Ø 40 HRGs (of 603) account for 46% of emergency admissions and 42% emergency generated bed days Ø 40 HRGs account for 60% of in patient elective episodes and 40% of elective bed-days, and Ø 40 HRGs account for 84% of day elective episodes Ø 10 HRGs account for 98% of all maternity and births admissions and 97% of maternity and birth bed days DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling
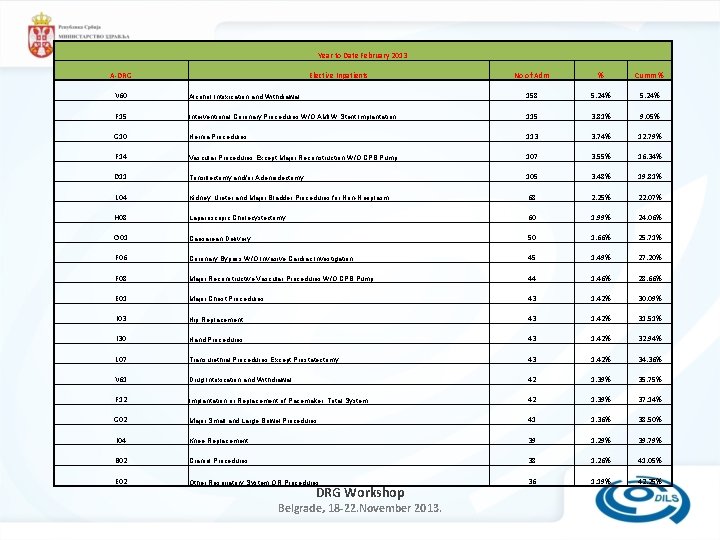
Year to Date February 2013 A-DRG Elective Inpatients No of Adm % Cumm % V 60 Alcohol Intoxication and Withdrawal 158 5. 24% F 15 Interventional Coronary Procedures W/O AMI W Stent Implantation 115 3. 81% 9. 05% G 10 Hernia Procedures 113 3. 74% 12. 79% F 14 Vascular Procedures Except Major Reconstruction W/O CPB Pump 107 3. 55% 16. 34% D 11 Tonsillectomy and/or Adenoidectomy 105 3. 48% 19. 81% L 04 Kidney, Ureter and Major Bladder Procedures for Non-Neoplasm 68 2. 25% 22. 07% H 08 Laparoscopic Cholecystectomy 60 1. 99% 24. 06% O 01 Caesarean Delivery 50 1. 66% 25. 71% F 06 Coronary Bypass W/O Invasive Cardiac Investigation 45 1. 49% 27. 20% F 08 Major Reconstructive Vascular Procedures W/O CPB Pump 44 1. 46% 28. 66% E 01 Major Chest Procedures 43 1. 42% 30. 09% I 03 Hip Replacement 43 1. 42% 31. 51% I 30 Hand Procedures 43 1. 42% 32. 94% L 07 Transurethral Procedures Except Prostatectomy 43 1. 42% 34. 36% V 61 Drug Intoxication and Withdrawal 42 1. 39% 35. 75% F 12 Implantation or Replacement of Pacemaker, Total System 42 1. 39% 37. 14% G 02 Major Small and Large Bowel Procedures 41 1. 36% 38. 50% I 04 Knee Replacement 39 1. 29% 39. 79% B 02 Cranial Procedures 38 1. 26% 41. 05% E 02 Other Respiratory System OR Procedures 36 1. 19% 42. 25% DRG Workshop Belgrade, 18 -22. November 2013.
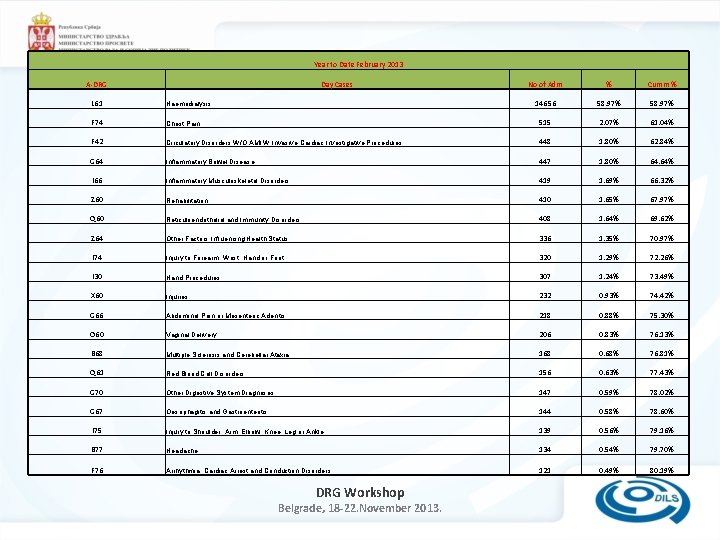
Year to Date February 2013 A-DRG Day Cases No of Adm % Cumm % 14656 58. 97% L 61 Haemodialysis F 74 Chest Pain 515 2. 07% 61. 04% F 42 Circulatory Disorders W/O AMI W Invasive Cardiac Investigative Procedures 448 1. 80% 62. 84% G 64 Inflammatory Bowel Disease 447 1. 80% 64. 64% I 66 Inflammatory Musculoskeletal Disorders 419 1. 69% 66. 32% Z 60 Rehabilitation 410 1. 65% 67. 97% Q 60 Reticuloendothelial and Immunity Disorders 408 1. 64% 69. 62% Z 64 Other Factors Influencing Health Status 336 1. 35% 70. 97% I 74 Injury to Forearm, Wrist, Hand or Foot 320 1. 29% 72. 26% I 30 Hand Procedures 307 1. 24% 73. 49% X 60 Injuries 232 0. 93% 74. 42% G 66 Abdominal Pain or Mesenteric Adenitis 218 0. 88% 75. 30% O 60 Vaginal Delivery 206 0. 83% 76. 13% B 68 Multiple Sclerosis and Cerebellar Ataxia 168 0. 68% 76. 81% Q 61 Red Blood Cell Disorders 156 0. 63% 77. 43% G 70 Other Digestive System Diagnoses 147 0. 59% 78. 02% G 67 Oesophagitis and Gastroenteritis 144 0. 58% 78. 60% I 75 Injury to Shoulder, Arm, Elbow, Knee, Leg or Ankle 139 0. 56% 79. 16% B 77 Headache 134 0. 54% 79. 70% F 76 Arrhythmia, Cardiac Arrest and Conduction Disorders 121 0. 49% 80. 19% DRG Workshop Belgrade, 18 -22. November 2013.

Why high volume case types? High volume case types are those for which: • Pathways will produce the biggest ‘bang for the buck’ as we strive to improve: • Efficiency • Effectiveness • Quality DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

Variance Analysis For each high volume case type collect, collate and analyze data on: - the occurrence and non occurrence of the events described in a pathway - quality indicators, clinical outcomes indicators and resource usage These data are then used to: - profile and compare performance within and between hospitals over time - identify changes in practice that will lift performance to the benefit of improvements in quality, appropriateness, safety and efficiency including changing the pathway DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

QUESTION 4 • Which data on their caseload patterns and peer norms are most useful? DRG Workshop Belgrade, 18 -22. November 2013.

MACRO TO MICRO DRILLDOWNS • Totals to clinical units – individual clinical teams • Totals to particular DRGs – patient types – • Inputs across peers for sub sets of case categories DRG Workshop Belgrade, 18 -22. November 2013.

VARIANCES FROM TARGETS • Monthly patterns – modelled utilisation • Modelled seasonal variations • Modelled patient type demand/supply projections – Population factors – Supply factors – eg leave – theatre rostering – training schedules – DRG Workshop Belgrade, 18 -22. November 2013.

QUESTION 5 • How can quality and safety risk processes/practices be identified before the scandal / disaster / avoidable mortality rates / avoidable complications rates arise? DRG Workshop Belgrade, 18 -22. November 2013.

Quality and efficiency improvement oriented clinical unit management Requires condition specific multidisciplinary conversations on questions such as: Are we doing the right things? l In light of assessed health needs and existing resource constraints, are we delivering value for money? l How appropriate and effective is the composite of activities that we undertake in treating this condition? Are we doing things right? l How systematized and reliable are our care processes for this condition? l Are we clear about who should do what and when? l How are we performing on risk, safety, quality, patient evaluation, clinical outcomes and efficiency? What can and must we do to improve quality and efficiency? DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

The evidence shows that: The improvement focus of funding and clinical unit management systems are sharpened greatly with the development and implementation of clinical pathways that for each high volume case type: – – describe the detailed composition of the care process, define cost, define quality and outcome measures , provide clinical teams with a basis for monitoring and improving their performance DRG Workshop Belgrade, 18 -22. November 2013. From Pieter Degeling

USING DRG DATA TO ASK THE QUESTIONS THAT STIMULATE CHANGE. DRG Workshop Belgrade, 18 -22. November 2013. 55
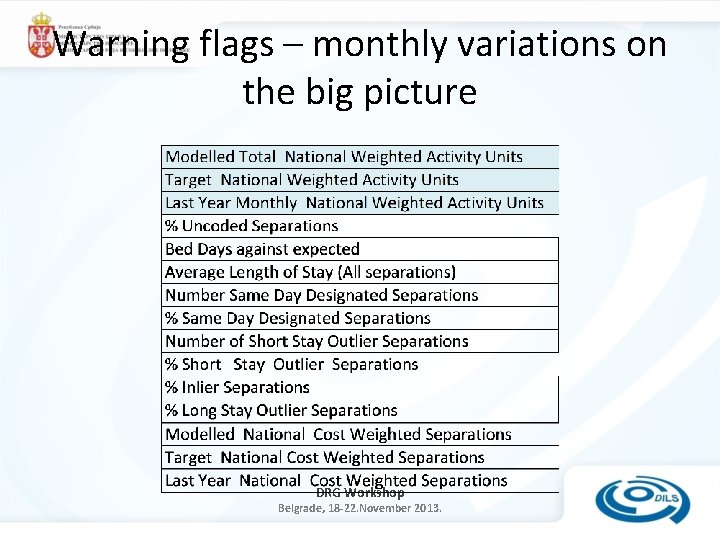
Warning flags – monthly variations on the big picture DRG Workshop Belgrade, 18 -22. November 2013.

Statistical and clinicial review DRG Workshop Belgrade, 18 -22. November 2013.
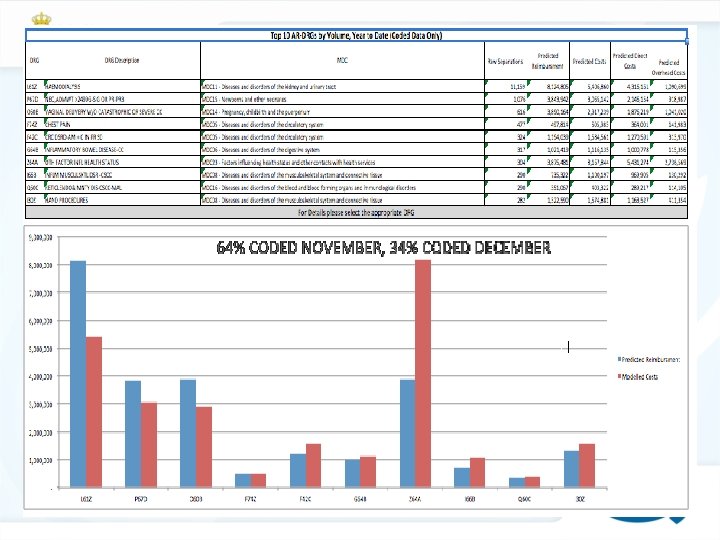
DRG Workshop Belgrade, 18 -22. November 2013.
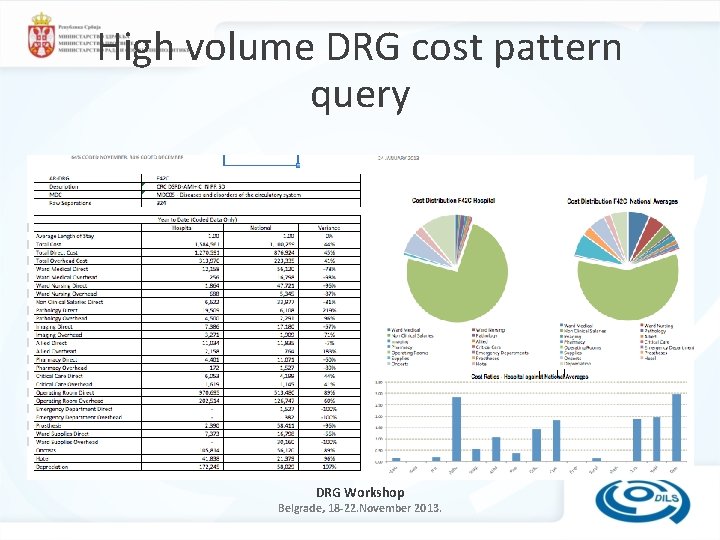
High volume DRG cost pattern query DRG Workshop Belgrade, 18 -22. November 2013.
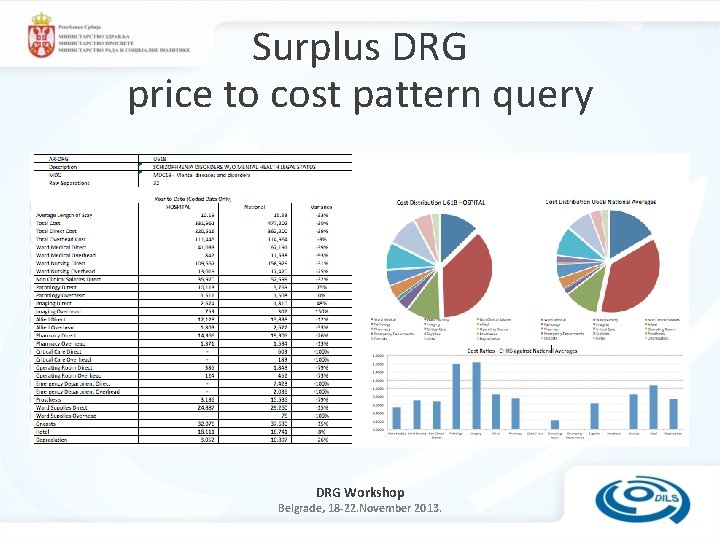
Surplus DRG price to cost pattern query DRG Workshop Belgrade, 18 -22. November 2013.
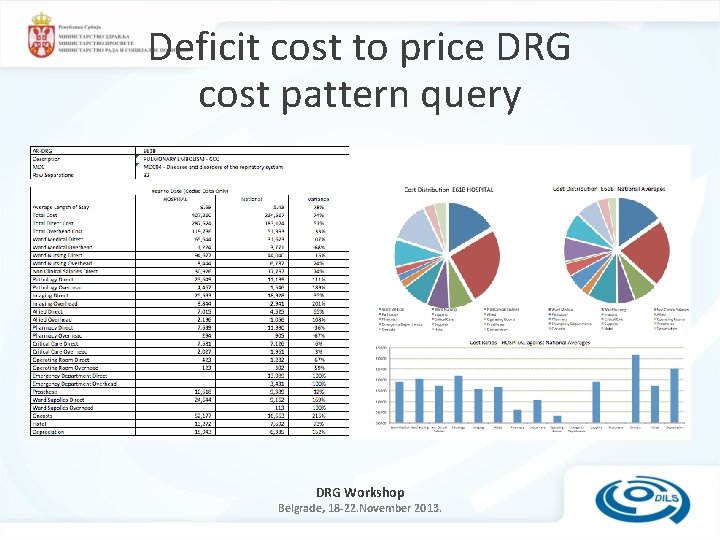
Deficit cost to price DRG cost pattern query DRG Workshop Belgrade, 18 -22. November 2013.

So now to the next generation of casemix - caremix • Eg MODELS OF CARE • Includes efficiency – that incorporates value – the ‘right thing’ and the ‘thing right’ • So new types of episodes – integrated plans across settings/providers – eg “year of care” • How do we cost these cross setting/provider episodes and find a like with like benchmarking mechanism? • The answer is we have to do both – not either-or. DRG Workshop Belgrade, 18 -22. November 2013.

Example of clinician feedback and data validation dynamics? Data Governance and Standards and Quality Technical and programming Executive of Hospital Division ABF Operational analyst DRG Workshop Belgrade, 18 -22. November 2013. Performance Reporting
- Slides: 63