CYSTS OF MOUTH AND JAW Definition classification pathogenesis































- Slides: 42

. CYSTS OF MOUTH AND JAW Definition, classification, pathogenesis.

SYLLABUS : CYSTS OF MOUTH AND JAW : Definition, classification, pathogenesis. Diagnosis – Clinical features, radiological, FNAC, use of contrast media and histopathology. Management – type of surgical procedures. Rational of the techniques, indications, contraindications, procedures complications etc.

DEFINATION OF CYST A cyst is defined as an abnormal cavity in hard or soft tissue which contains fluid, semifluid or gas and is often encapsulated and lined by epithelium (Killey and Kay 1966). Cyst is a pathological cavity having fluid, semifluid or gaseous contents and which is not created by the accumulation of pus. Most cysts, but not all, are lined by epithelium. (Kramer ).

A. EPITHELIAL-LINED CYSTS 1 DEVELOPMENTAL ORIGIN A. EPITHELIAL-LINED CYSTS (a) Odontogenic i. iii. iv. v. viii. ix. Gingival cyst of infants Odontogenic keratocyst Dentigerous cyst Eruption cyst Gingival cyst of adults Developmental lateral periodontal cyst Botryoid odontogenic cyst Glandular odontogenic cyst Calcifying odontogenic cyst i. iii. iv. Non-odontogenic cysts Midpalatal raphé cyst of infants Nasopalatine duct cyst Nasolabial cyst

TYPES OF CYSTS • • TRUE CYSTS: that which is lined by epithelium e. g dentigerous cyst, radicular cyst etc. PSEUDO CYSTS: not lined by epithelium, e. g. Solitary bone cyst, Aneurismal bone cyst etc

Cyst is defined as pathologic cavity, lined by epithelium having fluid, semifluid, or gaseous contents but not the pus in initial stages.

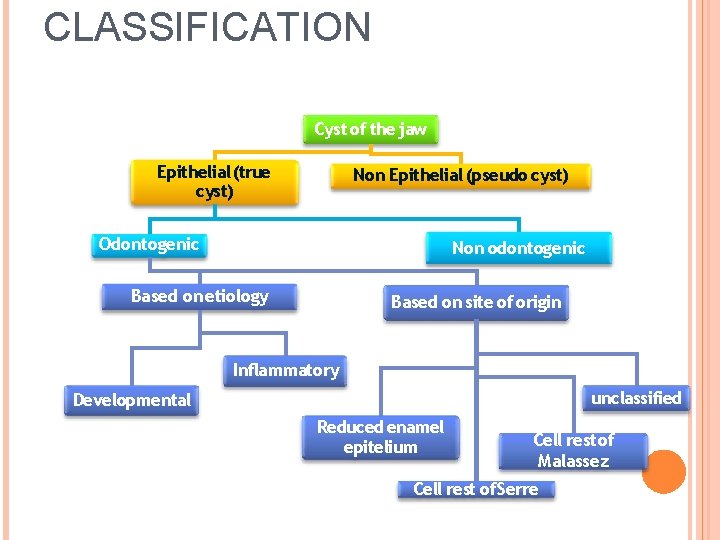
CLASSIFICATION Cyst of the jaw Epithelial (true cyst) Non Epithelial (pseudo cyst) Odontogenic Non odontogenic Based on etiology Based on site of origin Inflammatory unclassified Developmental Reduced enamel epitelium Cell rest of Malassez Cell rest of. Serre

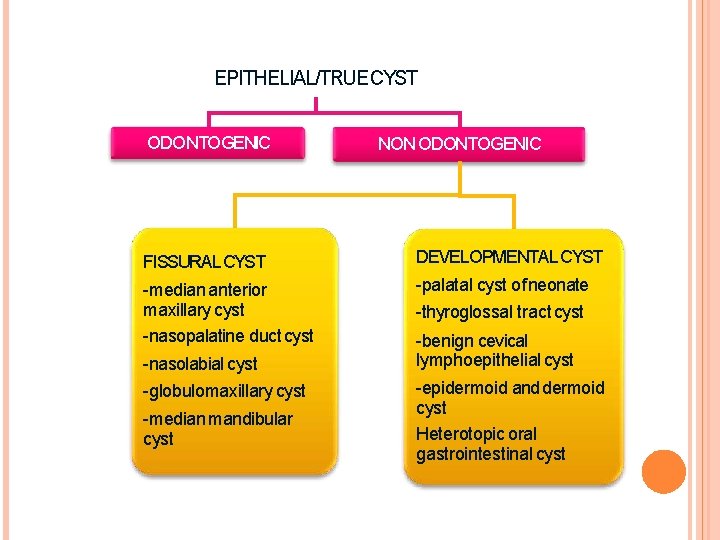
EPITHELIAL/TRUE CYST ODONTOGENIC NON ODONTOGENIC FISSURAL CYST DEVELOPMENTAL CYST -median anterior maxillary cyst -nasopalatine duct cyst -palatal cyst of neonate -nasolabial cyst -globulomaxillary cyst -median mandibular cyst -thyroglossal tract cyst -benign cevical lymphoepithelial cyst -epidermoid and dermoid cyst Heterotopic oral gastrointestinal cyst

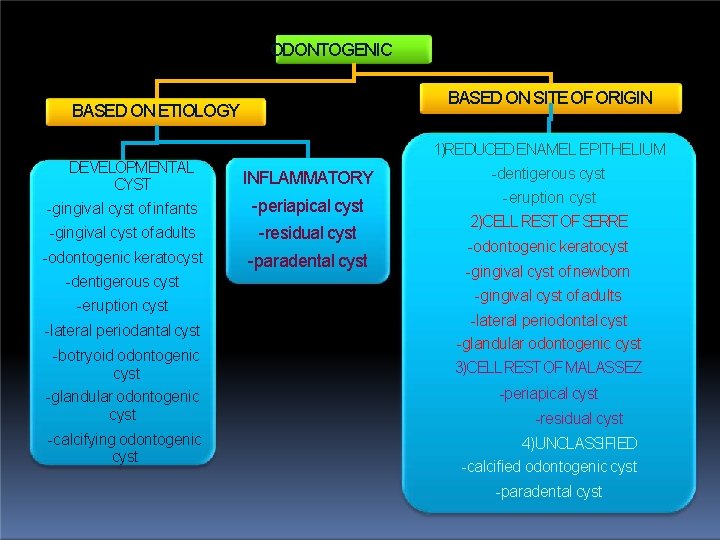
ODONTOGENIC BASED ON SITE OF ORIGIN BASED ON ETIOLOGY DEVELOPMENTAL CYST -gingival cyst of infants 1)REDUCED ENAMEL EPITHELIUM INFLAMMATORY -periapical cyst -gingival cyst of adults -residual cyst -odontogenic keratocyst -paradental cyst -dentigerous cyst -eruption cyst -lateral periodantal cyst -botryoid odontogenic cyst -glandular odontogenic cyst -calcifying odontogenic cyst -dentigerous cyst -eruption cyst 2)CELL REST OF SERRE -odontogenic keratocyst -gingival cyst of newborn -gingival cyst of adults -lateral periodontal cyst -glandular odontogenic cyst 3)CELL REST OF MALASSEZ -periapical cyst -residual cyst 4)UNCLASSIFIED -calcified odontogenic cyst -paradental cyst

“CYST LIKE” LESIONS 1. Hemorrhagic cysts ( Traumatic bone cyst) Static bone cavities ( Idiopathic or Stafne’s defect) Neoplasms of the bone presenting a radioluscent appearance , e. g. ameloblastoma, angioma, myxoma, giant cell lesions Fibrous dysplasia Metabolic dysfunction : bone tumour of hyperparathyroidism Hystiocytosis-X

CYST FORMATION Cysts occur more in the jaws than any other bones in the body Reason : cysts originate from numerous rests of odontogenic epithelium , which remain even after tooth formation Phases of cyst development: 3 phases A. Cyst initiation B. Cyst formation C. Cyst enlargement or expansion

The cyst initiation process for different epithelial lined cyst is different in different groups. But, cyst enlargement process is almost same CYST INITIATION: Basically stimulus of cyst initiation is not known. Infection is considered as common mode of stimulus for inflammatory cysts.

Some individuals have predisposition of cyst formation from developing odontogenic epithelium i. e. following tissues have potential to form cysts: a. Enamel organ b. Dental lamina and its remnants c. Extension of basal cells from the overlying epithelium d. Reduced enamel epithelium e. Cell rests of Malsses

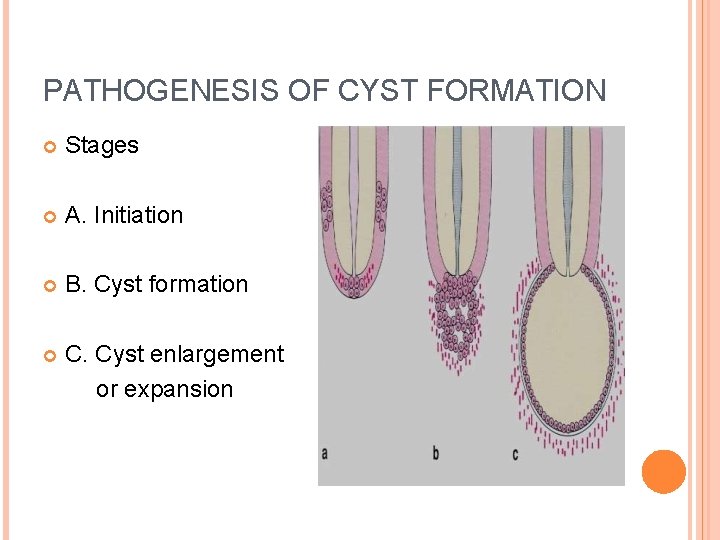
PATHOGENESIS OF CYST FORMATION Stages A. Initiation B. Cyst formation C. Cyst enlargement or expansion

CYST INITIATION • Proliferation of the epithelial cells, leading to mass of cells in response to inflammation or due to unknown factors.

CYST ENLARGEMENT : HARRIS (1974 1) Mural growth Peripheral cell division b) Accumulated contents a) 2) Hydrostatic Secretion b) Transuduation & exudation a) MECHANISM 1. Increase in the volume of its contents. 2. Increase in the surface area of the sac or epithelial proliferation. Resorption of surrounding bones 3.

INCREASE CYST VOLUME OF CYST CONTENTS TRANSDUTION AND EXUDATION: inflammatory cysts, in presence of infection release : Inflammatory cells release cofactors Lymphocytes release lymphokine Osteoclast activating factor (OAF) & Monocytes release interleukin which stimulates fibroblasts to release prostaglandin. The desquamated epithelial cells of cyst lining undergo autolysis/ breakdown and produce large number molecules of lower molecular weight , raising the osmolarity of fluid which has been suggested as an important cause of cyst enlargement. Lymphatic obstruction : Osmotic imbalance

Increased hyper-osmolarity: it produces three effects a. raises the internal hydrostatic pressure b. attracts external fluid within the cyst cavity c. retention fluid within the cyst cavity

RAISED INTERNAL HYDROSTATIC PRESSURE • Toller suggested the role of osmolarity by the cyst fluid in enlargement of cyst. The Mean Osmolarity was 296 mosmol compared with Serum Osmolarity of 282 mosmol. • The increase in the osmotic pressure is related to proteins present in the cyst fluid such as large molecules of albumin, globulin, fibrinogen. • Desquamated epithelial cells of cyst lining undergo autolysis & produce a larger number of molecules of lower molecular weight, raising the osmolarity of the fluid.

FUID ATTRACYION INTO THE CAVITY Increased hydrostatic pressure further draws in fluid from surrounding tissue. The cyst wall acts as semi permeable membrane • Fluid is attracted into the cyst cavity by products of epithelial cell autolysis, due to difference in molarity. • Water from the tissue fluid (surrounding tissue) is attracted into the cyst to raise the internal pressure. • The increased hydrostatic pressure is transmitted to adjacent peripheral bone

RETENTIONFLUID IN CYST CAVITY • • Cyst lining acts as permeable membrane – governs access into the cyst but prevents the escape of certain substances from the contents. attracted fluid inside the cavity are unable to diffuse out of the cavity. The products of epithelial autolysis could effect both osmotic attraction and retention within the cavity.

BONE RESORPTION • Increased internal pressure is transmitted to the adjacent bone which causes resorption of bone leading to enlargement of bony cavity. • Due to the above changes, the surface area of cyst lining is increased by cell multiplication. • Epithelial cells divide – cyst enlarges within bony cavity by the release of bone resorbing factors from the capsule. • Stimulate osteoclast function – eg: prostaglandins like PGE 1 & PGE 2

Further enlargement of cyst causes microcracks on the thinned out cortical plates. This produces “egg shell crackling” during the palpation of the lesion. In later stages as the enlargement continues , the thinned out cortex completely resorbs and the cysts lining comes in contact of oral mucosa , and fluctuation can be felt now. Perforation of cyst lining will cause escape of cyst fluid in the oral cavity producing a salty taste in the mouth.

CYST REGRESSION Any process which causes involution of oral epithelium e. g. extraction of tooth or marsupialization may cause connective tissue capsule to regress and obliteration of the cavity by bone or osteoid tissue.

GENERAL CONSIDERATIONS OF CYSTIC LESIONS Problems in differential diagnosis X-ray examination Surgical techniques Post operative treatment and complications of surgery

DIAGNOSIS COMPONENTS OF DIAGNOSIS History Physical findings X-ray evaluation FNAC / Tissue biopsy Histological examination : required for correct diagnosis Clinical laboratory investigations are sometimes also necessary

Clinical symptoms are usually absent unless cyst becomes quite large and causes facial asymmetry. Pain, paresthesia or anesthesia may be a clinical complaint. It occurs due to compression on a nerve Cysts may be multiple, each from a separate group or multiple cysts may be indicative of systemic disease. Biopsy should not be done immediately to eliminate other studies. It should be deferred until its indications are clear

In large , cystic, bony defects that cause facial assymmetry, expansion takes place usually along the line of least resistance and in bone and generally in one direction. ( Note: a tumour will usually grow and expand in and through the bone in all the direction). Vital structures like nerves, blood vessels, and paranasal sinuses are usually displaced by the pressure exerted by cyst fluid ( Note : A tumour invades and surround these tissues)

If the swellings are painful and tender - infected cysts ? If the swelling is hard, rapidly growing at the angle of mandible producing facial assymmetry in the younger age group –primordial cyst ? First a provisional diagnosis is made and various investigations are done to confirm the diagnosis

ASPIRATION BIOPSY / FNAC One the needle enters the “cystic” cavity , the nature of cavity can be confirmed Negative aspirate : solid lesion Positive aspirate : cystic fluid Dentigerous cyst : clear straw colored fluid Periapialcyst : do The cyst fluid contain cholestrol crystals. If the syringe is held under a beam of light , these crystals are bright and glistening. OKC : creamy white suspension Fresh blood : vascular tumour

ESTIMATION OF PROTEIN IN CYST FLUID In OKC : aspirate is low in protein content. < 4 gm/100 ml Other cysts : > 5 gm/100 ml

X-RAY FINDINGS 1. It gives information about the extent and location, and involvement of teeth. Pressure of the cystic fluid within the cavity may cause formation of compact layer of bone in which the cyst sac is contained. This dense lamina is seen in x-ray film as a thin white line outlining the area containing the radiolucent cyst. Cysts usually have a smooth rounded, lobular outline and may be multi-locular in appearance, but if secondarily infected, the margins may be irregular

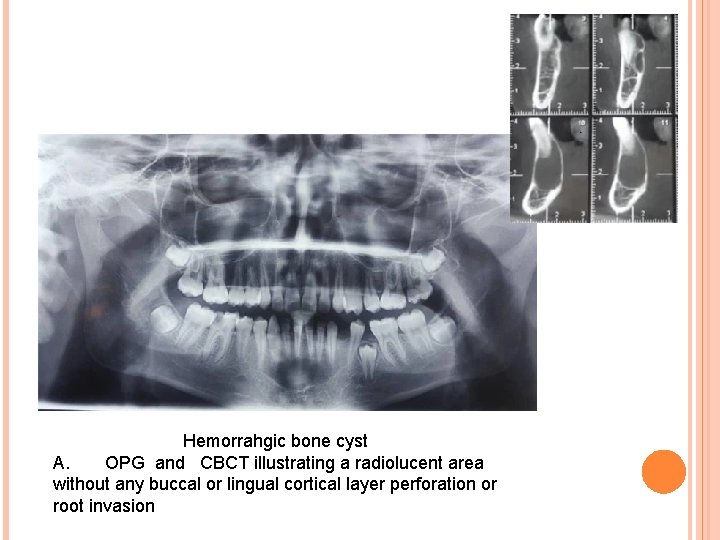
Hemorrahgic bone cyst A. OPG and CBCT illustrating a radiolucent area without any buccal or lingual cortical layer perforation or root invasion

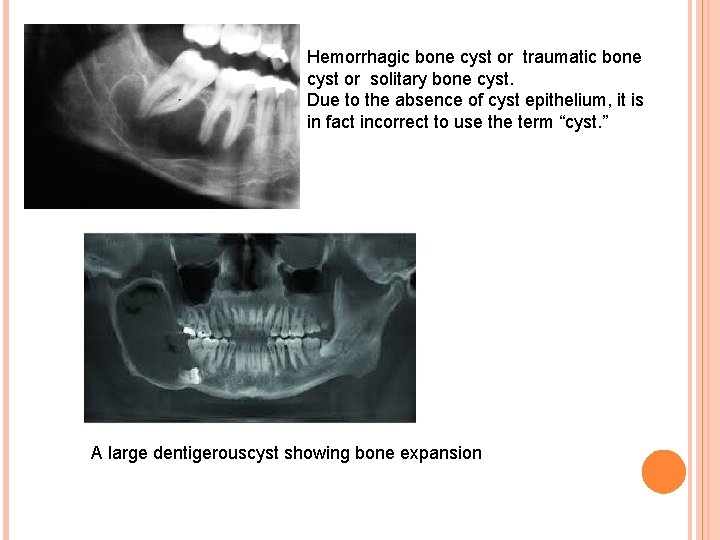
Hemorrhagic bone cyst or traumatic bone cyst or solitary bone cyst. Due to the absence of cyst epithelium, it is in fact incorrect to use the term “cyst. ” A large dentigerouscyst showing bone expansion

Cysts in maxilla are usually difficult to visualize in plane x-rays as shadows of paranasal sinuses overlap the structure. A radio-opaque dye may be injected after aspiration of cystic content and radiograph is taken. This technique is also used to visualize the soft tissue cysts and sinus tracts.

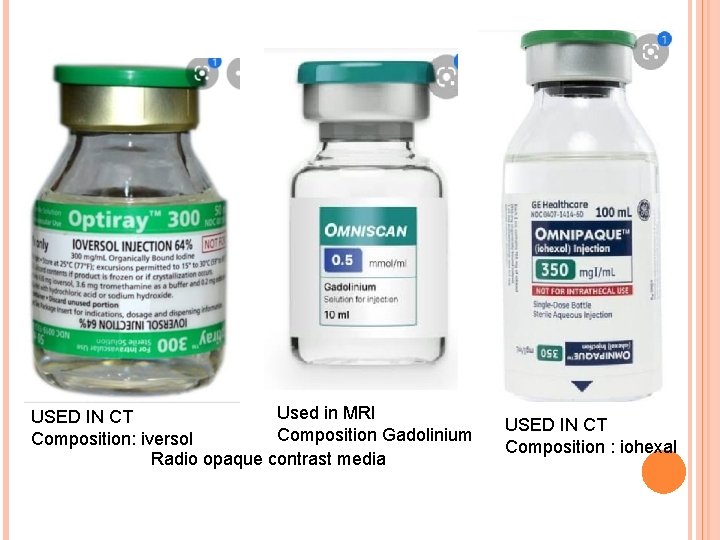
Radiocontrast agents are substances used to enhance the visibility of internal structures in X-raybased imaging techniques such as computed tomography (Contrast CT), and fluoroscopy. Radiocontrast agents are typically iodine, or more rarely barium-sulphate. They absorb external X-rays, resulting in decreased exposure on the X-ray detector.

Used in MRI USED IN CT Composition Gadolinium Composition: iversol Radio opaque contrast media USED IN CT Composition : iohexal

CT / CBCT clearly delineate the location and size of pathological lesion. When cyst is quite large, and both the cortical plates are involved, it usually give a punched out appearance.

Complete regeneration of these cortical plates rarely occurs and the defect will be always seen on the x-ray film. In such cases history of previous surgery or treatment will be important. It is always wise to inform the patient about this finding, so that if he attends any other surgeon for his any other problem, a needless operation may be avoided.

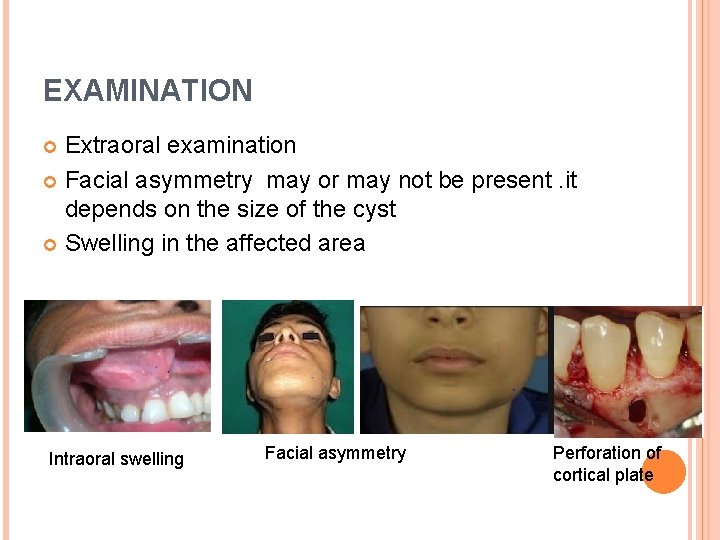
EXAMINATION Extraoral examination Facial asymmetry may or may not be present. it depends on the size of the cyst Swelling in the affected area Intraoral swelling Facial asymmetry Perforation of cortical plate

INTRAORAL EXAMINATION Examination 1. Bone expansion 2. Fluctuant swelling under oral mucosa 3. Non vital tooth 4. Missing tooth in normal series 5. Cyst fluid or pus discharging sinus , if infected. 6. Percussion Distortion of adjacent structures Hollow sound on percussion

THANK YOU