Cystic Fibrosis Part 2 Woe to that child

Cystic Fibrosis Part 2 "Woe to that child which when kissed on the forehead tastes salty. He is bewitched and soon must die. " This European adage accurately describes the fate of an individual diagnosed with cystic fibrosis during ancient times.

Diagnosis • Patients present with persistent pulmonary infections, pancreatic insufficiency, and elevated sweat chloride levels • Adults are more likely to present with GI symptoms, diabetes, and infertility • As of 2010 CF newborn screening is required in all states

Diagnostic Criteria • BOTH of the following criteria must be met to diagnose CF: 1. Clinical symptoms consistent with CF in at least one organ system, AND 2. Evidence of CFTR dysfunction (any of the following): • Elevated sweat chloride ≥ 60 mmol/L (on two occasions) • Presence of two disease-causing mutations in CFTR from each parental allele • Abnormal nasal potential difference

Sweat Chloride Test • Remains the primary test for the diagnosis of CF. • Intermediate results of sweat testing should be clarified by DNA analysis using a CFTR multi-mutation method, and sweat chloride testing should be repeated.

Treatment and Survival • Although CF shortens lifespan, survival has dramatically increased from the 1950’s – Between 1985 and 2007 the median lifespan increased from 25 to 37 years • 45% of CF patients are >18 years old • 10% of CF patients are >40 years old • In 2011 the median predicted survival for patient in the United States was 36. 8 years

Cornerstones of Chronic Cystic Fibrosis Therapy • Airway clearance – Manual percussion, oscillating vest, flutter valve • Mucolytic dornase alfa • Nebulized antibiotics – Tobramycin – Colistimethate, aztreonam • Oral azithromycin • Inhaled hypertonic saline • Aggressive antibiotic therapy for exacerbations • Nutritional support – High-caloric, high salt diet • Replacement of fatsoluble vitamins ADEK • Exercise

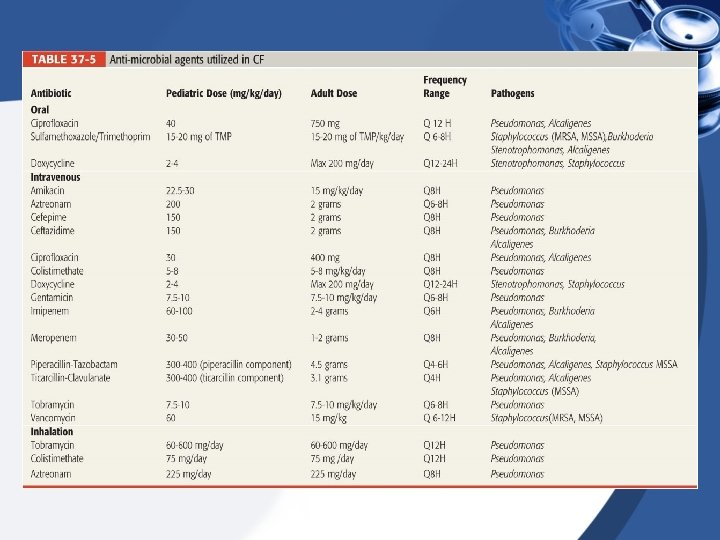
Pulmonary Treatments

Ivacaftor (Kalydeco®) • Only for patients with G 551 D mutation • 150 mg by mouth twice daily with high fat meal • Improves chloride transport by potentiating CFTR • Decreases sweat chloride, increases FEV 1, increases weight, decreases exacerbations, increases quality of life

Dornase Alfa (Pulmozyme®) • Reduces mucous viscosity • Dosed at 2. 5 mg daily or twice daily • Administered via nebulizer and should not be mixed with other drugs • Improves FEV 1 and decreases exacerbations

Hypertonic Saline • Improves airway clearance by hydrating the airway surface liquid • 3% or 7% saline twice daily to four times daily • Administered via nebulizer • Improved FEV 1 and decreased exacerbations

Inhaled Tobramycin (TOBI) • Antipseudomonal aminogylcoside antibiotic • Dosed at 300 mg inhaled every 12 hours for 28 days and then not taken for 28 days • Must be used with PARI-LC PLUS handheld nebulizer • Administer TOBI last and do not mix with other inhaled medications • Improves FEV 1 and decreases exacerbations

Aztreonam (Cayston®) • Antipseudomonal antibiotic • Dosed at 75 mg inhaled every 8 hours for 28 days and then off for 28 days • Utilizes Alteral Nebulizer System. Do not mix with other inhaled medications • Improves FEV 1 and decreases exacerbations

Azithromycin (Zithromax®) • Antibiotic that does not have antipseudomonal activity also exhibits some anti-inflammatory properties • Dosed at 250 or 500 mg orally three times a week • Decreases exacerbations
- Slides: 14