Cyanosis is the bluish or purplish discolouration of

Cyanosis is the bluish or purplish discolouration of the skin or mucous membranes due to the tissues near the skin surface having low oxygen saturation • Defined historically as the presence of 5 gm/d. L of deoxygenated hemoglobin (deoxy Hb) or greater. • Since estimation of hypoxia is usually now based either on arterial blood gas measurement or pulse oximetry Aisha Abu

• the presence of cyanosis is dependent upon there being an absolute quantity of deoxyhemoglobin, the bluish color is more readily apparent in those with high hemoglobin counts than it is with those with anemia. • When signs of cyanosis first appear, such as on the lips or fingers, intervention should be made within 3– 5 minutes because a severe hypoxia or severe circulatory failure may have induced the cyanosis. • The name cyanosis literally means the blue disease or the blue condition

• An oxygen saturation of 66% corresponds to an arterial oxygen tension (pa. O 2)= of approximately 35 mm. Hg. , the oxygen tension (Pa. O, ) at which cyanosis is detected will be even lower. Assume for example that the patient's Hb is now 10 gm/d. L. The saturation at which we will detect cyanosis (ie. , when the Deoxy. Hb = 5 gm/d. L) • EX. : Sa. O, = Oxy. Hb / (Oxy. Hb + Deoxy. Hb) Sa. O, = 5 / (5 + 5) = 50% An oxygen saturation of 50% corre- sponds to an oxygen tension (Pa. OJ of only 27 mm. Hg

• under optimal lighting conditions with no excessive skin pigmentation and a normal hemo- globin level, the earliest that cyanosis can be appreciated is at an oxygen saturation of approximately 85%. This corresponds to a Pa. O, of 55 mm. Hg. At a Sa. O, of 70% most clinicians will be able to detect cyanosis (Pa. O, of apptoximately 40 mm. Hg). • Cyanosis has been. When the hemoglobin level is 15 gm/d. L and 5 gm/d. L of this Hb releases oxygen to the tissues, the oxygenated hemo- globin portion (Oxy. Hb) is 10 gm/d. L. Hence the oxygen saturation is: Sa. O, = Oxy. Hb/ (Oxy. Hb + Deoxy. Hb) Sa. O, = 10 / (10 + 5) = 66%

• In severely anemic patients, oxygen saturation at which cyanosis is detectable will be lower than in normal patients. • - Hb level = 10 gm/d. L, 5 gm/d. L release O 2 -Sa. O 2 = Oxy. Hb / (oxy. Hb + Deoxy. Hb) = 5 / (5 + 5) = 50% SAO 2 of 50% corresponds to Pa. O 2 of only 27 mm. Hg • Under optimal conditions, the earliest that cyanosis can be appreciated is at an oxygen saturation of 85%(Pa. O 2 of 55 mm. Hg).
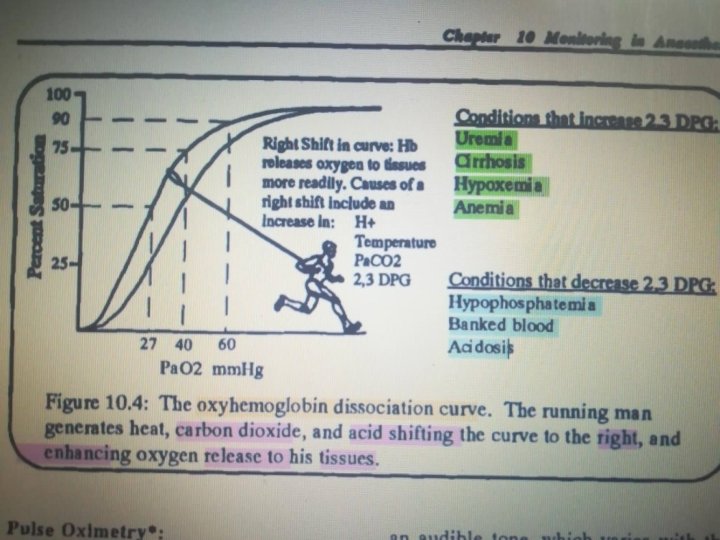

1. When Pa. O 2 is low ( Pa. O 2<60%), the hemoglobin affinity to oxygen falls rapidly, explaining the sharp sloping : 2. . • Shifting in the curve is a normal process depending on the site of circulation. • Right shift : Hb releases oxygen to tissues; muscles and placenta, more rapidly. • Left shift: Hb has a higher affinity for oxygen in the lungs 3. • Causes of shifting Include changes in Pa. CO 2, Ph, temperature and [2, 3 DPG]. Key Values: a. b. c. At PO 2 100 mm. Hg, Hb 100% saturation. At PO 2 40 mm. Hg, Hb 75% saturation. At PO 2 27 mm. Hg, Hb 50% saturation. • The lowest acceptable O 2 saturation level is 90%. • 2, 3 -diphosphoglyceric acid (conjugate base) is present in human red blood cells (RBC; erythrocyte) at approximately 5 mmol/L. It binds with greater affinity to deoxygenated hemoglobin

Remember that : left shift =less oxygen to tissue =tissue hypoxia Right shift =more oxygen to tissue


BY: Aisha Abu Rashed Thank you
- Slides: 11