Curbside Consults to Pulmonary Timothy Scialla MD Division

Curbside Consults to Pulmonary Timothy Scialla, MD Division of Pulmonary/Critical Care Medicine Duke University School of Medicine

Questions To Be Covered ♦ Is this really asthma? ♦ What is the evidence for supplemental oxygen in patients with chronic respiratory disease? ♦ Is there anything new with chronic cough management? PLEASE! ♦ What is the current state of lung cancer screening?

Case #1: Shortness of breath and bronchitis ♦ 42 year-old female with self-reported asthma presents to primary care for shortness of breath and productive cough ♦ She needs a refill of her high dose ICS/LABA and SABA. ♦ Requests antibiotics for bronchitis ♦ No reported allergies to common aeroallergens ♦ Exam: BMI 42. Chest is clear. Remainder of the exam is unremarkable.

Audience Response Question #1 What would be the next best step for this patient? 1. 2. 3. 4. 5. Review inhaler technique Order spirometry Obtain chest imaging Ask for more history looking for possible OSA or GERD Discuss weight loss and exercise


Rationale 1. Review inhaler technique: poor inhaler technique/low med adherence leads to poorly controlled asthma 2. Order spirometry: getting updated spirometry results to assess underlying lung function is reasonable if not done recently or unclear asthma diagnosis 3. Obtain chest imaging: if history suspicious for infection or further investigation into chronic lung disease 4. Ask for more history looking for possible OSA or GERD: it is reasonable to suspect co-morbidities contributing to underlying symptoms given her high BMI 5. Discuss weight loss and exercise: if clinical picture c/w asthma, GERD or OSA, weight loss could help alleviate symptoms

Asthma: Establishing the Correct Diagnosis ♦ Characteristic history ♦ Episodic symptoms ♦ Characteristic triggers ♦ Characteristic response to triggers ♦ Characteristic examination ♦ Inflamed nasal mucosa ♦ Atopy ♦ Diffuse musical wheezes ♦ Diagnostic Testing ♦ Spiromety (Pre-Post SABA)

Reevaluation of Diagnosis in Adults with Physician-Diagnosed Asthma ♦ 467 adults with physician diagnosis of asthma within last 5 years ♦ 33% had diagnosis of current asthma excluded by a thorough evaluation ♦ >50% with erroneous diagnosis of asthma had not undergone testing for airflow limitation at time of diagnosis References: Aaron SD, et al. JAMA 2017; 317: 269 -9
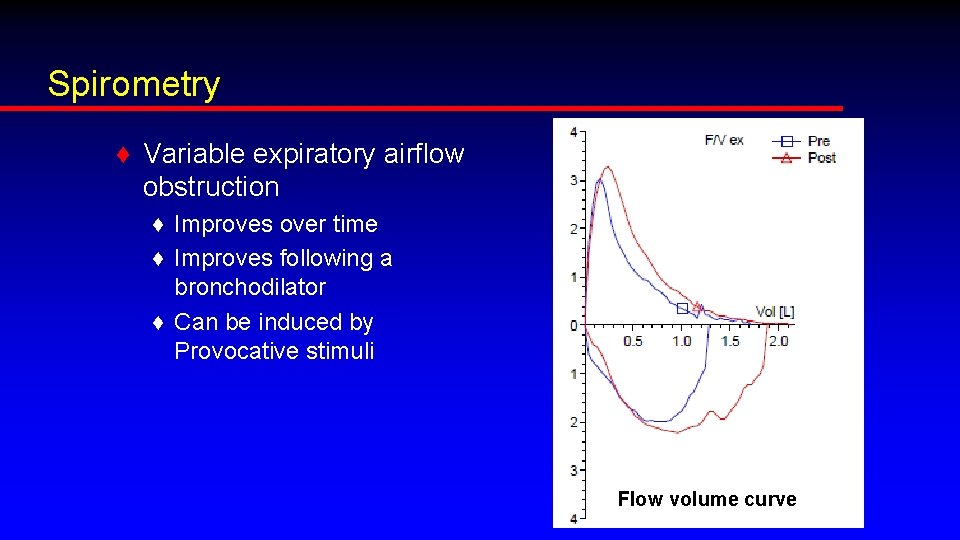
Spirometry ♦ Variable expiratory airflow obstruction ♦ Improves over time ♦ Improves following a bronchodilator ♦ Can be induced by Provocative stimuli Flow volume curve

Interpreting PFTs ♦ Significant bronchodilator response: ♦ Increase in FEV 1 of 12% AND ♦ Absolute increase of 200 ml ♦ Asthmatic response ♦ Typically 15 -20% increase in FEV 1
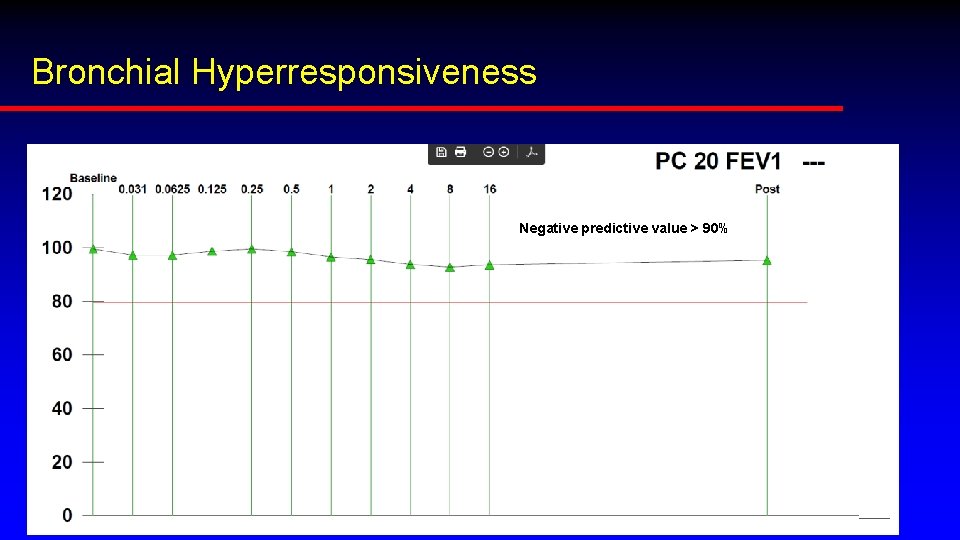
Bronchial Hyperresponsiveness Negative predictive value > 90%
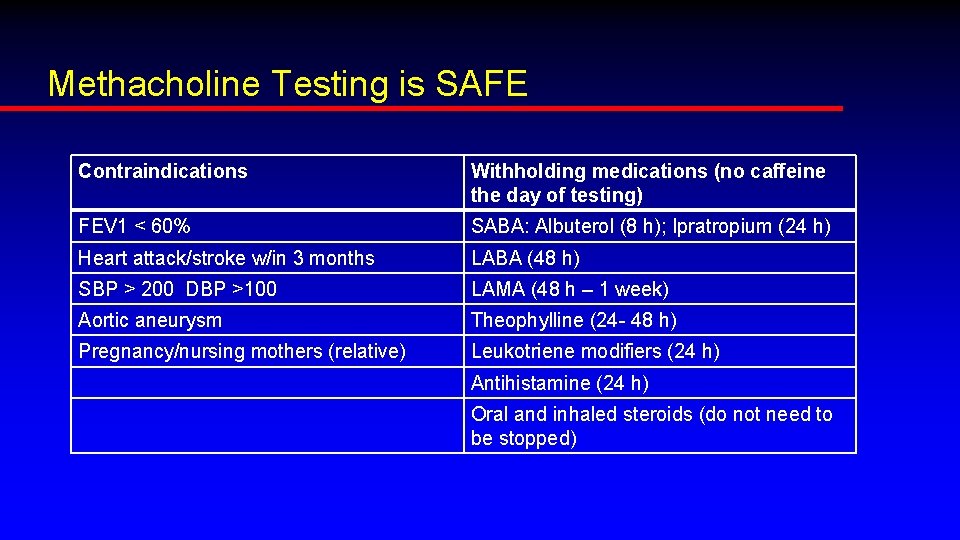

Methacholine Testing is SAFE Contraindications Withholding medications (no caffeine the day of testing) FEV 1 < 60% SABA: Albuterol (8 h); Ipratropium (24 h) Heart attack/stroke w/in 3 months LABA (48 h) SBP > 200 DBP >100 LAMA (48 h – 1 week) Aortic aneurysm Theophylline (24 - 48 h) Pregnancy/nursing mothers (relative) Leukotriene modifiers (24 h) Antihistamine (24 h) Oral and inhaled steroids (do not need to be stopped)

Misdiagnosis: The Textbook Differential ♦ Structural lung diseases ♦ Airways ♦ Bronchiectasis (CF & non-CF) and COPD ♦ Interstitial lung disease ♦ ♦ Pulmonary embolism Cardiac causes (cardiac asthma) Mechanical airway obstruction Inducible laryngeal obstruction (ILO) ♦ Vocal cord dysfunction and more! ♦ Irritants include post nasal drip and acid/nonacid esophageal reflux ♦ Non-asthmatic eosinophilic bronchitis

Case #1: My Differential ♦ Non-allergic Asthma with co-morbid Obesity/deconditioning ♦ Inducible laryngeal obstruction (ILO) ♦ Vocal cord dysfunction and more! ♦ Irritants include post nasal drip and acid/nonacid esophageal reflux ♦ More on this later in talk ♦ Non-asthmatic eosinophilic bronchitis ♦ Structural lung diseases

Case #1: My Plan ♦ Pre-Post Spirometry ♦ If normal: ♦ Methacholine challenge testing ♦ Chest imaging ♦ FENO testing (40 ppb suggestive of airway eosinophilic inflammation) ♦ If normal ♦ Referral to ENT or voice center to evaluate for ILO/VCD ♦ Lifestyle modifications ♦ Diet and exercise but mostly exercise!

Questions to be Covered ♦ Is this really asthma? ♦ What is the evidence for supplemental oxygen in patients with chronic respiratory disease? ♦ Is there anything new with chronic cough management? PLEASE! ♦ What is the current state of lung cancer screening?

Case #2: Clinic scenarios: Who needs O 2? ♦ 68 year-old male ♦ Plethoric and hands slightly cyanotic ♦ Room air = 92% ♦ Walking = 78% ♦ HCT: 52% ♦ No symptoms ♦ Active ♦ 68 year-old male ♦ Pink puff /accessory muscle use ♦ Room air = 92% ♦ Walking = 78% ♦ HCT: 38% ♦ Breathless with any walking ♦ Sedentary/fearful of activity ♦ 68 year-old male ♦ Discharge follow up ♦ Sent home on supplemental O 2 ♦ Room Air = 94% ♦ Walking = 87% ♦ Improving symptoms ♦ Wants oxygen discontinued

Home Oxygen Therapy ♦ What is the evidence? ♦ What are the guidelines? ♦ What are the options for patients? ♦ At home ♦ Portability

Evidence of Clear Benefit ♦ In patients with: ♦ COPD ♦ Resting room air hypoxemia (O 2 < 88%) ♦ Long-term continuous oxygen therapy is disease modifying (ie. ↑ Life expentency) ♦ 2 studies ♦ Nocturnal Oxygen Therapy Trial (Annals of Internal Medicine. 1980) ♦ 12 h/d vs 24 h/d: at 24 months there was 18. 4% absolute mortality difference ♦ UK Medical Research Council trial (Lancet. 1981) ♦ 15 h/day vs Usual care: at 5 years there was 21% absolute mortality difference

Evidence of Unclear or No Benefit ♦ In patients with: ♦ COPD ♦ “Moderate hypoxemia” ♦ Resting saturation 89 -93% ♦ Exercise-induced desaturation (<90% for 10 seconds) ♦ Long-Term Oxygen Treatment Trial (NEJM 2016) ♦ Supplemental oxygen did not reduce mortality or other health-related outcomes compared to usual care

Home Oxygen Qualifying Guidelines www. cms. gov ♦ Fairly complex document ♦ Basic components ♦ Face to Face encounter (< 30 days from the CMN) ♦ Document diagnosis that would benefit from oxygen ♦ Alternative treatments considered and deemed ineffective ♦ Certificate of Medical Necessity ♦ Section A and C: completed by supplier ♦ Section B: completed by health care provider ♦ Qualifying oxygen saturation result

Qualifying Test Result. www. cms. gov ♦ Awake and resting Sp. O 2 < 88% breathing room air ♦ Awake and resting Sp. O 2 = 89% w/ secondary diagnosis ♦ Awake and exercising (patient is mobile) ♦ Exercise breathing room air Sp. O 2 < 88% ♦ Documented improvement during exercise w/ oxygen ♦ Sleeping ♦ Sp. O 2 < 88% for greater than 5 minutes ♦ Cannot get portable oxygen ♦ Recertify in 12 months: Face to Face + another CMN

Home (Domiciliary) Options Photo courtesy of Wikipedia ♦ Oxygen Concentrator ♦ Concentrates oxygen from ambient air ♦ Stationary compressed gaseous oxygen system ♦ Stationary liquid oxygen system

Portable Oxygen Options Photo courtesy of Wikipedia ♦ Portable gaseous oxygen tanks ♦ Portable oxygen concentrator ♦ Portable liquid oxygen system

Optimizing Home Oxygen Therapy Jacob et al. Annals ATS 15: 1369 -81. 2018 ♦ 1. 5 million Americans use supplemental oxygen ♦ “Home Oxygen” is a misnomer ♦ Goal of therapy is to “get out of the home!” ♦ Patients ♦ Personalized ♦ Portable ♦ Affordable ♦ Clinicians ♦ Streamlined orders ♦ Accessible and reliable DME companies ♦ Financial constraints favor restrictive choices ♦ No standard testing or orders ♦ Payer (Medicare) ♦ Competitive bidding driving DME companies to make hard choices ♦ Oxygen reimbursement outdated

Process not working well for anyone: Current state of “Out of” Home Oxygen Therapy ♦ Patients ♦ ♦ ♦ Inadequate and unmanageable 70% report < 4 hrs of portable O 2 80% desire > 5 hrs of portable O 2 Limited options at higher flow rates Most POC ♦ pulse dose only / continuous to 2 lpm ♦ Liquid O 2 best option for higher needs ♦ More expensive ♦ CMS requires this option if ordered ♦ CMS does not pay more for it ♦ Clinicians ♦ 40% of current patients on LTOT do not meet CMS criteria ♦ Less would meet “evidence-based” criteria ♦ DME companies ♦ Fixed prices and low reimbursement limiting equipment options and staffing ♦ Payers (Medicare) ♦ Competitive bidding has saved $3. 6 million ♦ “going smoothly with limited complaints and no negative impact on outcomes” Jacobs SS et al. Optimizing Home Oxygen Therapy. Annals. ATS. 15: 1369 -81. 2018

Audience Response Question #2 For which patient would supplemental oxygen be most appropriate? PATIENT #1 ♦ 68 year-old male ♦ Plethoric and hands slightly cyanotic ♦ Room air = 92% ♦ Walking = 78% ♦ HCT: 52% ♦ No symptoms ♦ Active PATIENT #2 ♦ 68 year-old male ♦ Pink puff /accessory muscle use ♦ Room air = 92% ♦ Walking = 78% ♦ HCT: 38% ♦ Breathless with any walking ♦ Sedentary/fearful of activity PATIENT #3 ♦ 68 year-old male ♦ Discharge follow up ♦ Sent home on supplemental O 2 ♦ Room Air = 94% ♦ Walking = 87% ♦ Improving symptoms ♦ Wants oxygen discontinued


Rationale PATIENT #1 ♦ 68 year-old male ♦ Plethoric and hands slightly cyanotic ♦ Room air = 92% ♦ Walking = 78% ♦ HCT: 52% ♦ No symptoms ♦ Active PATIENT #2 ♦ 68 year-old male ♦ Pink puff /accessory muscle use ♦ Room air = 92% ♦ Walking = 78% ♦ HCT: 38% ♦ Breathless with any walking ♦ Sedentary/fearful of activity PATIENT #3 ♦ 68 year-old male ♦ Discharge follow up ♦ Sent home on supplemental O 2 ♦ Room Air = 94% ♦ Walking = 87% ♦ Improving symptoms ♦ Wants oxygen discontinued

Questions to be Covered ♦ Is this really asthma? ♦ What is the evidence for supplemental oxygen in patients with chronic respiratory disease? ♦ Is there anything new with chronic cough management? PLEASE! ♦ What is the current state of lung cancer screening?

Case #3: Exhausted with coughing ♦ ♦ ♦ ♦ 55 year-old college professor Non-productive cough for past 10 years “Tried everything” Denies heartburn, allergies, history of asthma Non-smoker; No ACE inhibitor use Normal chest x-ray No constitutional symptoms Normal exam; BMI 25

Audience Response Question #3 After what length of time can unspecified cough symptoms be considered “chronic cough”? 1. 2. 3. 4. 5. More than 4 weeks More than 6 weeks More than 8 weeks More than 12 weeks More than 6 months

Chronic cough: Think in terms of 8 weeks ♦ Time needed to define “chronic cough” ♦ Time recommended to satisfy a therapeutic trial ♦ Time needed to withdrawal medication or exposure to reassess if improvement ♦ Time recommended to schedule follow-up and reassessment

Chronic Cough: The usual suspects ♦ Normal chest imaging / Not smoking ♦ Not on ACE-I; no “red flags” UACS -Sinus imaging -Nasopharyngoscopy -Allery evaluation -Treatments • A/D (First gen!) • Sinus rinse • Nasal steroid UACS: Upper Airway Cough Syndrome NAEB: Non-asthmatic eosinophilic bronchitis GERD: Gastroesophageal reflux disease ASTHMA -Spirometry -Methacholine challenge -Trigger history -Treatments • ICS/LABA • LTRA GERD -clear history of symptoms -dietary assessment for common triggers -Treatment • MORE THAN ACID SUPPRESION! • Lifestyle/dietary changes NAEB -Allergy assessment -Fractional exhaled nitric oxide (FENO) -Sputum eos -Treatment • ICS • Trigger avoidance Irwin RS et al. Classification of Cough as a Symptoms in Adults and Management Algorithms. CHEST 153: 196 -09. 2018
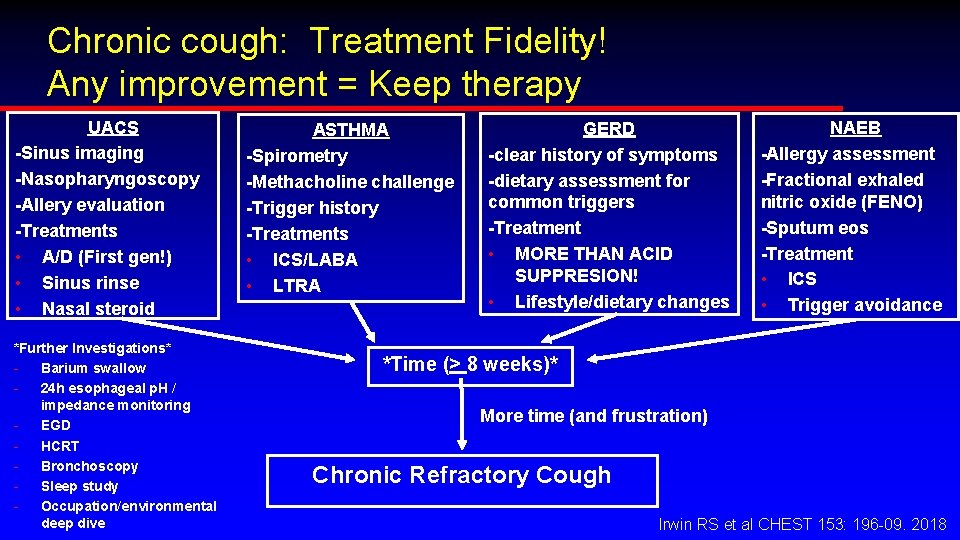
Chronic cough: Treatment Fidelity! Any improvement = Keep therapy UACS -Sinus imaging -Nasopharyngoscopy -Allery evaluation -Treatments • A/D (First gen!) • Sinus rinse • Nasal steroid *Further Investigations* Barium swallow 24 h esophageal p. H / impedance monitoring EGD HCRT Bronchoscopy Sleep study Occupation/environmental deep dive ASTHMA -Spirometry -Methacholine challenge -Trigger history -Treatments • ICS/LABA • LTRA GERD -clear history of symptoms -dietary assessment for common triggers -Treatment • MORE THAN ACID SUPPRESION! • Lifestyle/dietary changes NAEB -Allergy assessment -Fractional exhaled nitric oxide (FENO) -Sputum eos -Treatment • ICS • Trigger avoidance *Time (> 8 weeks)* More time (and frustration) Chronic Refractory Cough Irwin RS et al CHEST 153: 196 -09. 2018

? Chronic Refractory Cough (CRC) ? ♦ Persistent despite guideline directed treatments ♦ Cough Hypersensitivity Syndrome (CHS) ♦ Laryngeal Hypersensitivity ♦ Inducible Laryngeal Obstruction (ILO) ♦ Vocal Cord Dysfunction (VCD) ♦ Likely ALL Synonyms

Larynx: Ground Zero for Chronic Cough Photo courtesy of Wikipedia ♦ Primary Functions ♦ Safe passage of air in and out ♦ Prevent aspiration ♦ Phonation ♦ Complex Neural Control ♦ Reflexes ♦ Voluntary control ♦ Highest concentration of cough receptors ♦ Satisfies “Willie” Sutton’s Law ♦ “That’s were the $ is!”
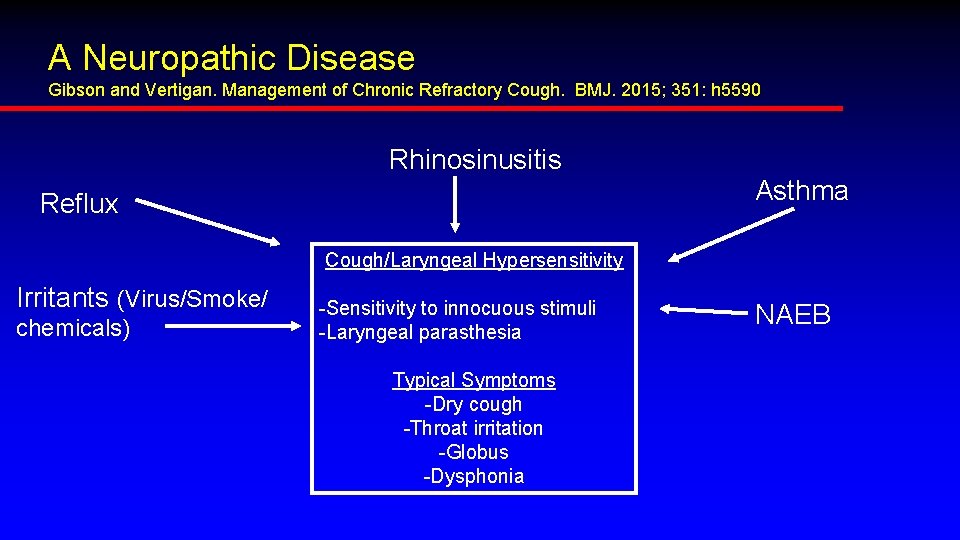
A Neuropathic Disease Gibson and Vertigan. Management of Chronic Refractory Cough. BMJ. 2015; 351: h 5590 Rhinosinusitis Reflux Asthma Cough/Laryngeal Hypersensitivity Irritants (Virus/Smoke/ chemicals) -Sensitivity to innocuous stimuli -Laryngeal parasthesia Typical Symptoms -Dry cough -Throat irritation -Globus -Dysphonia NAEB

Cough reflex: Presumed Pathophysiology Gibson and Vertigan. Management of Chronic Refractory Cough. BMJ. 2015; 351: h 5590 Photos courtesy of Wikipedia Cortex Cortical Potentiation Cortical Suppression Brainstem The Cough Center Larynx Sensory afferents Motor efferents

Additional Treatments: Speech Pathology Gibson and Vertigan. Management of Chronic Refractory Cough. BMJ. 2015; 351: h 5590 ♦ Education ♦ Cough not required ♦ Cough not always helpful ♦ Can be controlled ♦ Symptom control ♦ Suppressive swallowing ♦ Cough control breathing ♦ Vocal cord release breathing ♦ ↓ Laryngeal irritation ♦ Lifestyle changes to prevent reflux ♦ Hydration ♦ Reduce exposures to irritants ♦ Vocal rest ♦ Counseling ♦ Realistic goal settings ♦ Acknowledging the challenges

Additional Treatments: Neuromodulators ♦ Gabapentin ♦ Trial dosing was 600 mg tid ♦ Need to start low and titrate upward ♦ Not a failure unless at target dose or intolerable ♦ Amitriptyline ♦ Start low and titrate if effective ♦ Be aware of side effects (orthostatic hypotension) ♦ Morphine / Tramadol ♦ Baclofen Gibson and Vertigan. Management of Chronic Refractory Cough. 2015; 351: h 5590 BMJ.
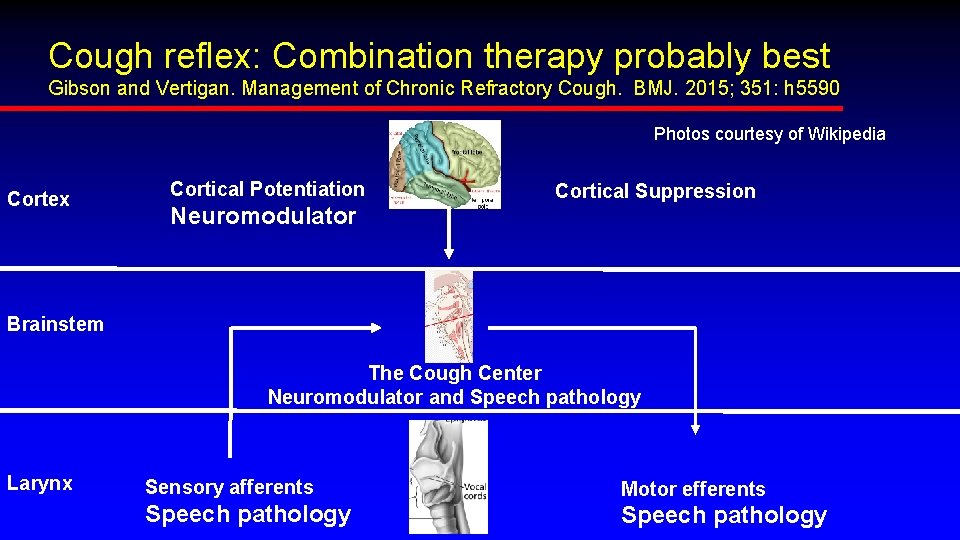
Cough reflex: Combination therapy probably best Gibson and Vertigan. Management of Chronic Refractory Cough. BMJ. 2015; 351: h 5590 Photos courtesy of Wikipedia Cortex Cortical Potentiation Cortical Suppression Neuromodulator Brainstem The Cough Center Neuromodulator and Speech pathology Larynx Sensory afferents Motor efferents Speech pathology

Case #3: My Recommendations ♦ Confirm treatment fidelity ♦ HRCT (inspiratory/expiratory) ♦ Tracheobronchomalacia/bronchiectasis ♦ Barium swallow plus GI evaluation ♦ Methacholine challenge if not already done ♦ If unrevealing and even if revealing ♦ Referral to Voice center / Speech Language Pathology ♦ Trial of Gabapentin ♦ Participation in clinical trial (NIH looking at Zinc Oxide)

Questions to be Covered ♦ Is this really asthma? ♦ What is the evidence for supplemental oxygen in patients with chronic respiratory disease? ♦ Is there anything new with chronic cough management? PLEASE! ♦ What is the current state of lung cancer screening?

Case #4: Asymptomatic smoker ♦ ♦ ♦ 60 year-old male 1 ppd for past 45 years History of HTN, former heavy ETOH Comes to doctor sporadically Not aware of lung cancer screening Not a fan of “lots of tests”

Question 4: Which of the following statements regarding lung cancer screening is correct? A. Annual lung cancer screening in patients who are eligible with a lowdose Chest CT scan is associated with a 20% absolute risk reduction in lung cancer deaths compared to annual chest x-rays. B. If the current recommendations are followed on eligible patients, approximately two people will develop lung cancer related to the radiation of the screening scans over ten years while approximately 10 lung cancers death will be prevented over the same period. C. Since lung cancer screening has been covered by insurance, the false positive rates and number of lung biopsies has declined compared to the original NLST population. D. The lung cancer screening rates for eligible patients in the United States are similar to the rates of breast cancer screening with mammography.

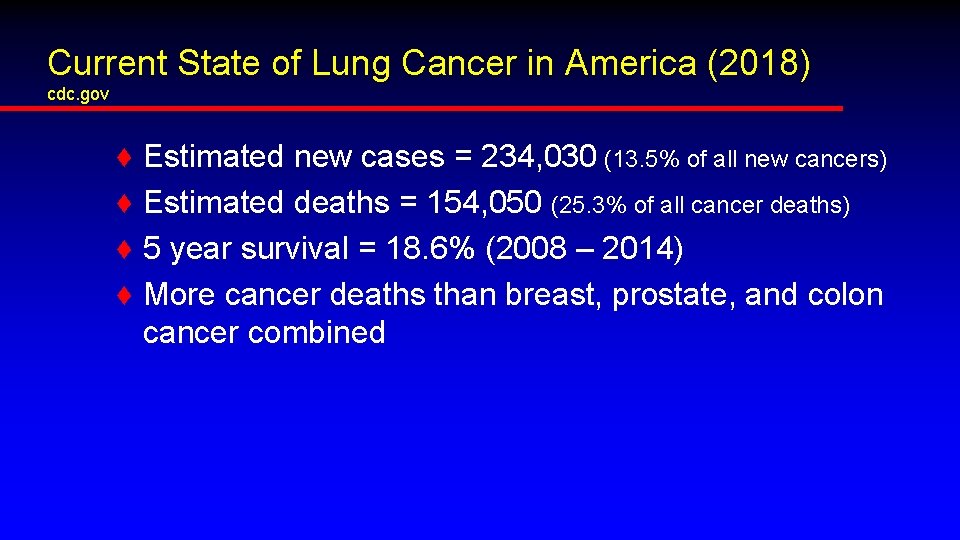
Current State of Lung Cancer in America (2018) cdc. gov ♦ ♦ Estimated new cases = 234, 030 (13. 5% of all new cancers) Estimated deaths = 154, 050 (25. 3% of all cancer deaths) 5 year survival = 18. 6% (2008 – 2014) More cancer deaths than breast, prostate, and colon cancer combined

Current State of Lung Cancer Screening ♦ Who should be screened? ♦ Heavy smoke exposure (> 30 pack years) ♦ Current smoker or quit within 15 years ♦ Ages 55 - 80 ♦ What are the risks of screening? ♦ False positives ♦ Overdiagnosis ♦ Radiation exposure over time ♦ When to stop ♦ Age 81 ♦ Quit more than 15 years ♦ Health problem that would not allow for surgery if cancer found
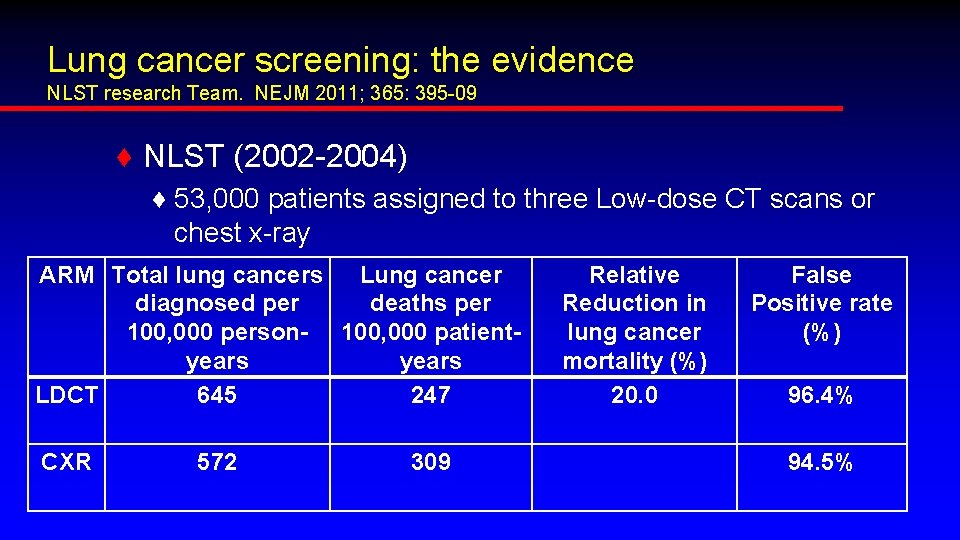
Lung cancer screening: the evidence NLST research Team. NEJM 2011; 365: 395 -09 ♦ NLST (2002 -2004) ♦ 53, 000 patients assigned to three Low-dose CT scans or chest x-ray ARM Total lung cancers Lung cancer diagnosed per deaths per 100, 000 person- 100, 000 patientyears LDCT 645 247 CXR 572 309 Relative Reduction in lung cancer mortality (%) 20. 0 False Positive rate (%) 96. 4% 94. 5%

The NELSON trial: Presented at WCLC 2018 International Association for the Study of Lung Cancer 19 th World Conference Abstract PL 02. 05 ♦ ♦ ♦ 15, 792 participant in Netherlands and Belgium 50 – 74 years LDCT scan vs usual care (no image) Imaging at: Baseline, 1, 3, and 5. 5 years Minimum of 10 year follow up Results: ♦ 26% Relative reduction in lung cancer deaths at 10 years ♦ Significant increase in surgical resections (67% vs 24. 5%) ♦ Appeared to have higher reduction in women
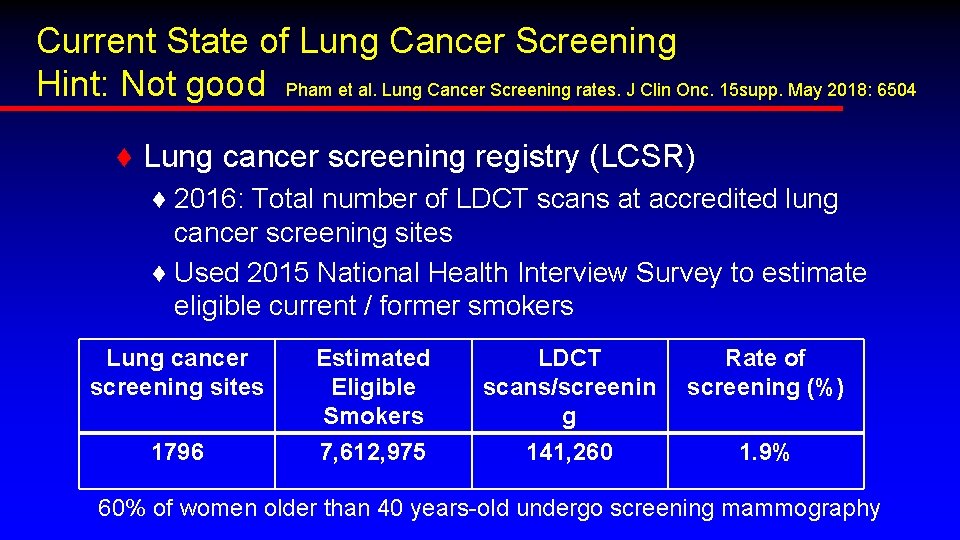
Current State of Lung Cancer Screening Hint: Not good Pham et al. Lung Cancer Screening rates. J Clin Onc. 15 supp. May 2018: 6504 ♦ Lung cancer screening registry (LCSR) ♦ 2016: Total number of LDCT scans at accredited lung cancer screening sites ♦ Used 2015 National Health Interview Survey to estimate eligible current / former smokers Lung cancer screening sites Estimated Eligible Smokers LDCT scans/screenin g Rate of screening (%) 1796 7, 612, 975 141, 260 1. 9% 60% of women older than 40 years-old undergo screening mammography

Photo courtesy of Wikipedia Why the low utilization? ♦ “In theory, theory and practice are the same but in practice, they are not. ” ♦ Higher false positive rates than in the trials ♦ Cumulative radiation exposure ♦ ♦ ♦ LDCT = 2 m. Sv; Full CT scan = 8 m. SV In one study: Estimated 10 year exposure Men = 9. 3 m. SV ; Women = 13. 0 m. SV 2. 4 cases of radiation cancer over ten years 1 case for every 108 Lung Cancers detected ♦ Not enough clinic band-width to deal with results Rampinelli et al. Exposure to low dose CT scan and risk of cancer. BMJ. 2017;
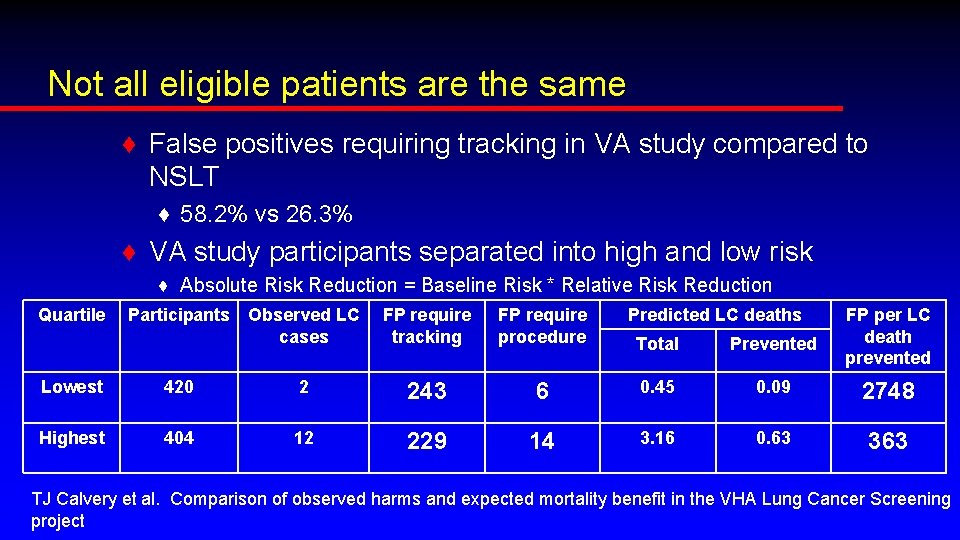
Not all eligible patients are the same ♦ False positives requiring tracking in VA study compared to NSLT ♦ 58. 2% vs 26. 3% ♦ VA study participants separated into high and low risk ♦ Absolute Risk Reduction = Baseline Risk * Relative Risk Reduction Quartile Participants Observed LC cases FP require tracking FP require procedure Predicted LC deaths Total Prevented FP per LC death prevented Lowest 420 2 243 6 0. 45 0. 09 2748 Highest 404 12 229 14 3. 16 0. 63 363 TJ Calvery et al. Comparison of observed harms and expected mortality benefit in the VHA Lung Cancer Screening project

The need for shared decision making https: //www. cdc. gov/cancer/lung https: //effectivehealthcare. ahrq. gov/decision-aids/lung-cancer-screening/patient. html

My 2 minute approach: Best with visual aid! ♦ “Based on guideline, you are eligible for lung cancer screening” ♦ “If we take 1000 people like you and follow them with CT scans every year, 3 of you will be cured of lung cancer who otherwise would have died from it. ♦ “Of the 1000 people, over 300 of you will have false alarms. Most of these false alarms we follow with additional scans but some of you will have a biopsy that is not cancer” ♦ “If you choose to do the scan, it is more likely you will be one of the 300 than the 3. Are you OK giving up your chance to be one of the 3 cancer deaths that is prevented”
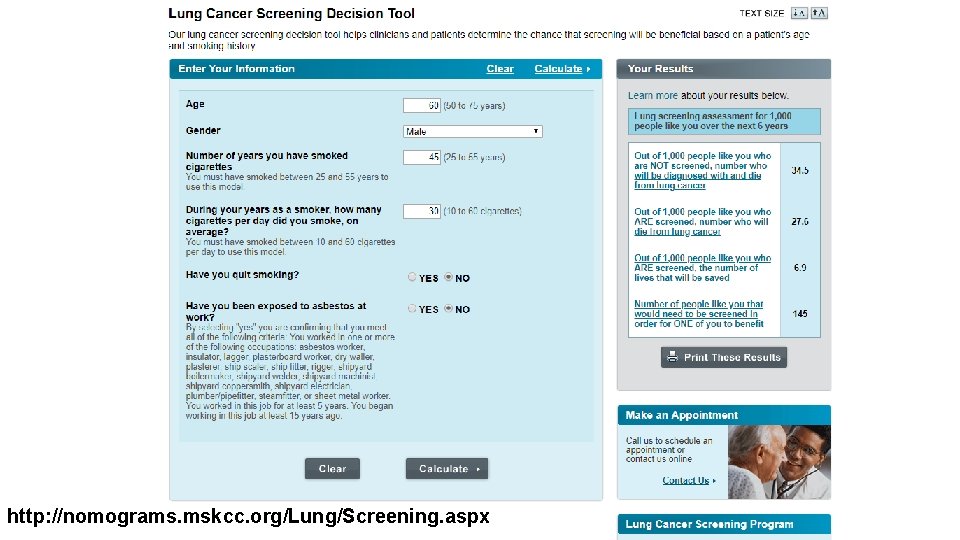
http: //nomograms. mskcc. org/Lung/Screening. aspx

Lung Cancer Screening: Final Thoughts ♦ ♦ ♦ 8. 6 million American meet criteria for screening Lung Cancer screening could prevent 12, 000 deaths/year Changes to Nodule guidelines will reduce false positives Reimbursement remains low Find an accredited near you Duke Lung Cancer Screening Program ♦ Full service process (shared-decision making / imaging /schedule all the follow-up scans) https: //www. acraccreditation. org/lung-cancer-screening-center

Take home points ♦ Methacholine Challenge testing ♦ Safe ♦ High negative predictive value (>90%) ♦ “Out of” Home Oxygen Therapy ♦ Resting hypoxemia: Saves lives! ♦ Exertional hypoxemia: Asymptomatic or doesn’t want it then DO NOT give it. If symptomatic AND will be more mobile then GIVE it.

Take home points ♦ Chronic Cough ♦ Treatment fidelity: Follow the guidelines ♦ Cough Hypersensitivity Syndrome ♦ Speech pathology ♦ Neuromodulators ♦ Lung Cancer Screening ♦ ♦ Benefits vs. Harms Shared Decision Making Evidence favors screening eligible patients (Lung Cancer is BAD!) Fine tuning ♦ Risk assessment / Intervals for scanning / Delivery in the “Real World”

Questions?
- Slides: 62