Cubital Tunnel Syndrome Dr Ahmed Samir Mohamed Lecturer
Cubital Tunnel Syndrome Dr. Ahmed Samir Mohamed Lecturer of Orthopedic Physical Therapy South Valley University

Anatomical Point of View Cubital tunnel extends from the medial epicondyle of the humerus to the olecranon process of the ulna, it consists of: Floor: ulnar collateral ligament. The roof: an aponeurosis(the arcuate ligament, or Osborne’s band). Posterior border: medial head of triceps. Anterior and lateral border: medial epicondyle and olecranon, respectively. The volume of the cubital tunnel is greatest with the elbow held in extension. As the elbow is brought into full flexion, there is a 55% decrease in canal volume.

The ulnar nerve • The ulnar nerve travels down the posterior aspect of the arm to eventually traverse posterior to the medial epicondyle through an area known as the cubital tunnel. • The nerve runs superficial to the ulnar collateral ligament (UCL) and deep to the aponeurotic attachment of the flexor carpi ulnaris (FCU), which is also known as Osborne’s ligament. • Once the ulnar nerve reaches the proximal border of Osborne’s ligament distal to medial epicondyle (zone III) it is located in the cubital tunnel.
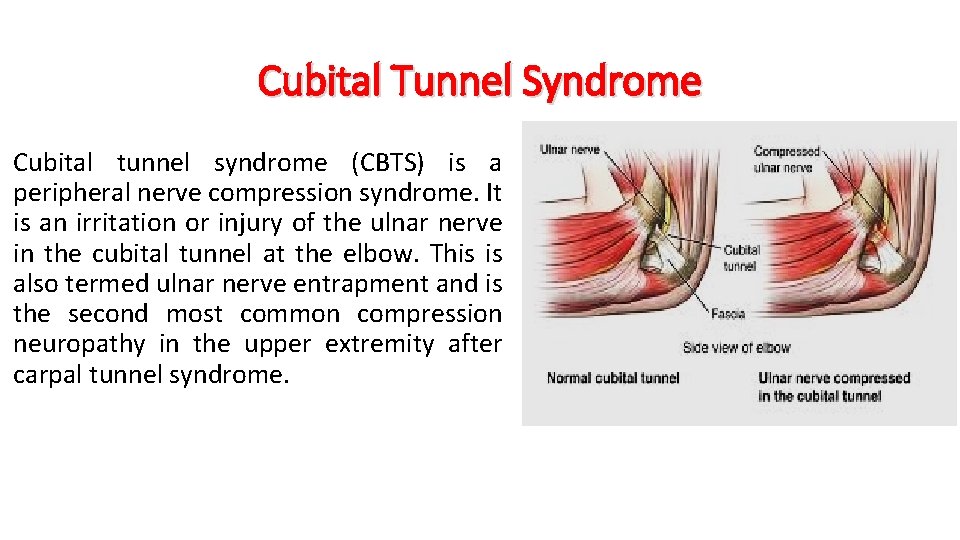
Cubital Tunnel Syndrome Cubital tunnel syndrome (CBTS) is a peripheral nerve compression syndrome. It is an irritation or injury of the ulnar nerve in the cubital tunnel at the elbow. This is also termed ulnar nerve entrapment and is the second most common compression neuropathy in the upper extremity after carpal tunnel syndrome.

Causes of CBTS 1. 2. 3. 4. 5. 6. 7. 8. 9. OA RA Heterotopic bone formation Trauma to the nerve (direct or indirect) Hypothyroidism D. M Renal failure Overhead throwing Traction injuries may be the result of longstanding valgus deformity and flexion contractures. 10. Hypertrophy of surrounding musculatures

Risk factors 1. 2. 3. 4. head injuries with upper extremity flexion contractures > 40 years old overhead throwing activities work which involves prolonged periods of elbow flexion, such as holding a telephone 5. persistently resting elbows on a hard surface 6. obesity

Clinically > 40 years Male or female Medial elbow pain. Numbness and tingling in 4 th and 5 th fingers, the ulnar side of the dorsum of the hand the hypothenar eminence. Wartenberg sign (abduction of the fifth digit due to weakness of the third palmar interosseous muscle) may be present.
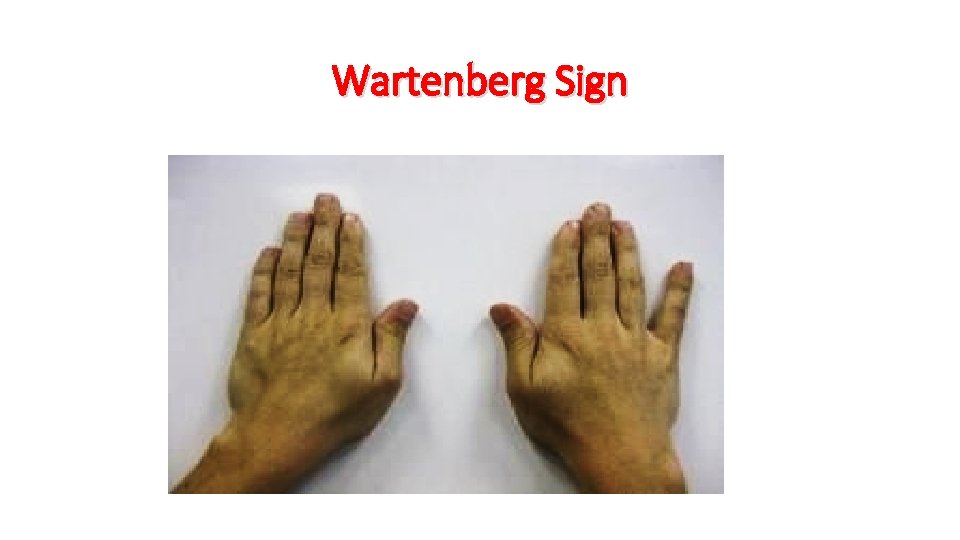
Wartenberg Sign
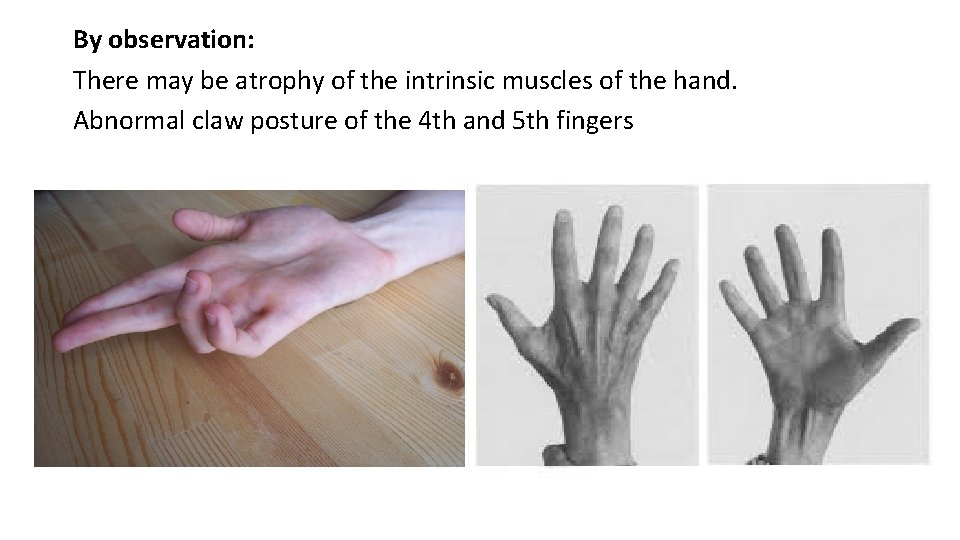
By observation: There may be atrophy of the intrinsic muscles of the hand. Abnormal claw posture of the 4 th and 5 th fingers

Palpation The ulnar nerve may be enlarged or palpable and tender in the groove.
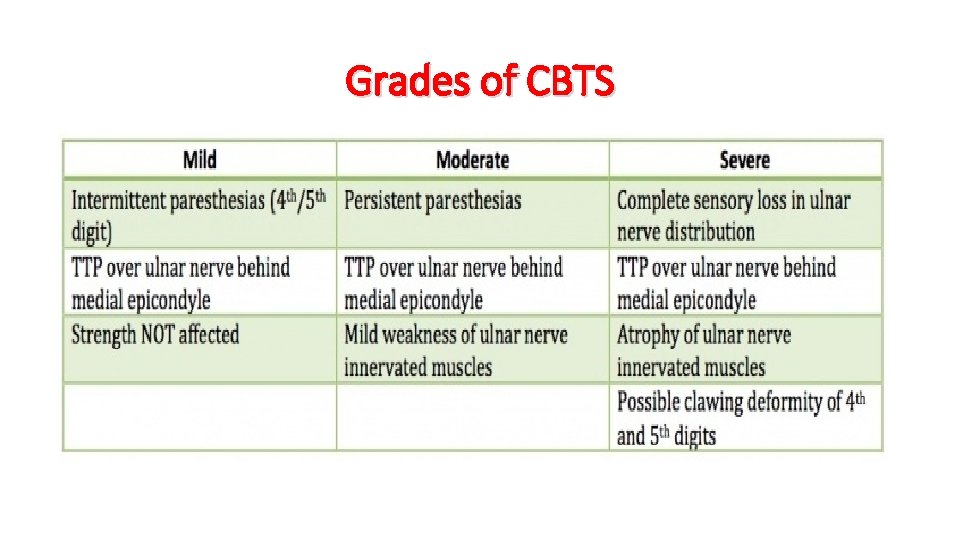
Grades of CBTS
Examination 1. Sensory changes in the ulnar nerve distribution (½ of the 4 th digit and entirety of the 5 th) pain 2. Atrophy of the intrinsic muscles of the hand innervated by the ulnar nerve 3. Neural provocation test of the ulnar nerve 4. Sparing of the flexor carpi ulnaris muscle

Special tests Flexion test: Typically performed bilaterally with the shoulder in full external rotation and the elbow actively held in maximal flexion with wrist extension held for one minute. Symptoms are produced as maximal elbow flexion reduces the cubital tunnel volume by approximately 55% causing increased neural pressure on the ulnar nerve. A positive test is reproduction of pain at the medial aspect of the elbow and numbness and tingling in the ulnar distribution on the involved side.

Flexion test

Tinel Sign: Reproduction of tingling and numbness into the 4 th and 5 th digits by tapping of the ulnar nerve at the cubital tunnel. The clinician will proceed with percussions on the ulnar nerve as it passes through the cubital tunnel after the ulnar groove, posterior of the medial epicondyle of the humerus (4 to 6 taps) reproduce symptoms. A positive test is the reproduction of tingling and numbness in the ulnar nerve distribution on the involved side.
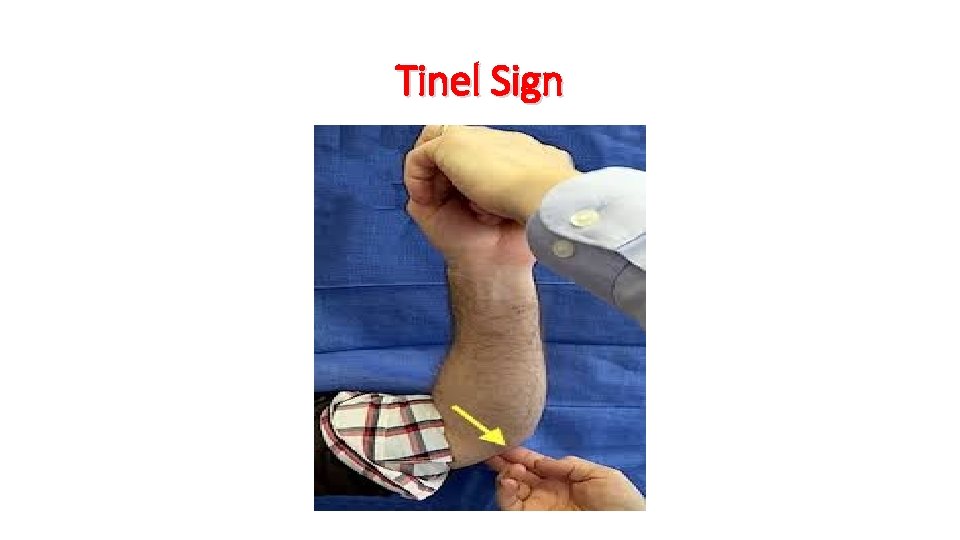
Tinel Sign
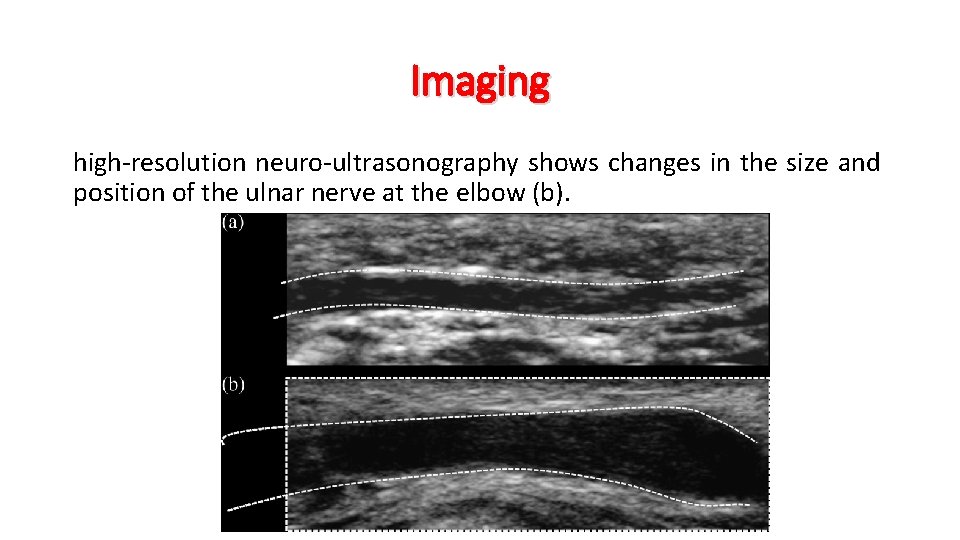
Imaging high-resolution neuro-ultrasonography shows changes in the size and position of the ulnar nerve at the elbow (b).
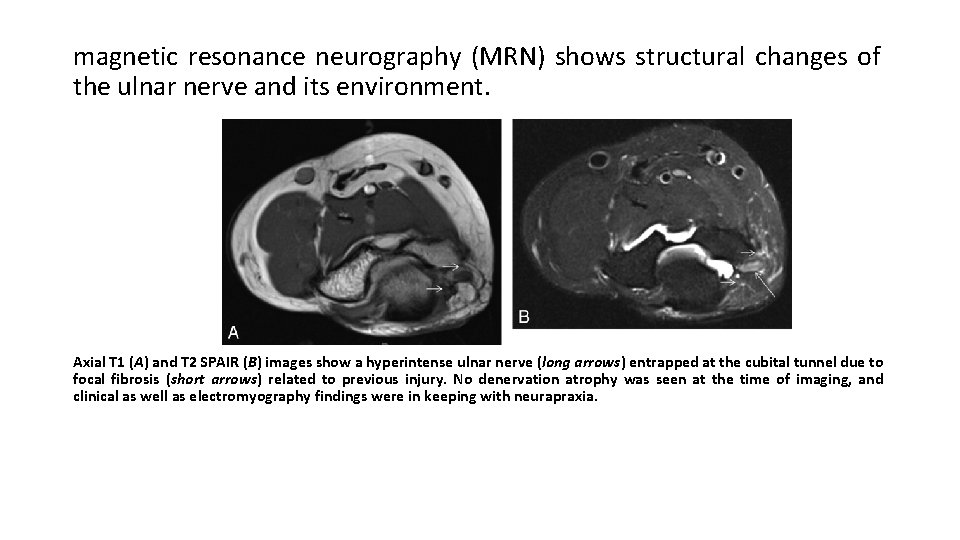
magnetic resonance neurography (MRN) shows structural changes of the ulnar nerve and its environment. Axial T 1 (A) and T 2 SPAIR (B) images show a hyperintense ulnar nerve (long arrows) entrapped at the cubital tunnel due to focal fibrosis (short arrows) related to previous injury. No denervation atrophy was seen at the time of imaging, and clinical as well as electromyography findings were in keeping with neurapraxia.

Medical Management Operative Management: It is indicated when: 1. Failure of three month conservative treatment. 2. An electrodiagnostic test of less than 39 -50 meters per second across the elbow. 3. Progressive symptoms 4. Sensorimotor deficits 5. Lack of clinical and electro-neurographic improvement 6. Worsening of the objective findings on follow up several weeks after the initial visit.

Operative techniques Simple decompression Medial epicondylectomy Anterior transposition

Physical Therapy Management 1 - Splint or rigid night splinting: ØAt 45 degrees of flexion and the forearm in neutral rotation. ØThe lowest value of these pressures is at an elbow position of 40 -50 degrees of flexion. Pressures are significantly higher in full flexion or extension of the elbow. ØSplinting is designed to alleviate symptoms and prevent the progressive dysfunction of nerves
Splinting

2 - Patient education and activity modification: ØThe patient is educated about pain provoking movements and how best to avoid them in ADLs. ØPatient should avoid positions that develops symptoms such as stretching or compressing the nerve when collaterally tilting the head or abducting. ØAvoid prolonged elbow flexion (static or repetitive) puts strain on the ulnar nerve and increases extraneural and intraneural pressure in the cubital tunnel.

Pain Relieving Modalities ICE TENS LASER ULTRASOUND THERAPY
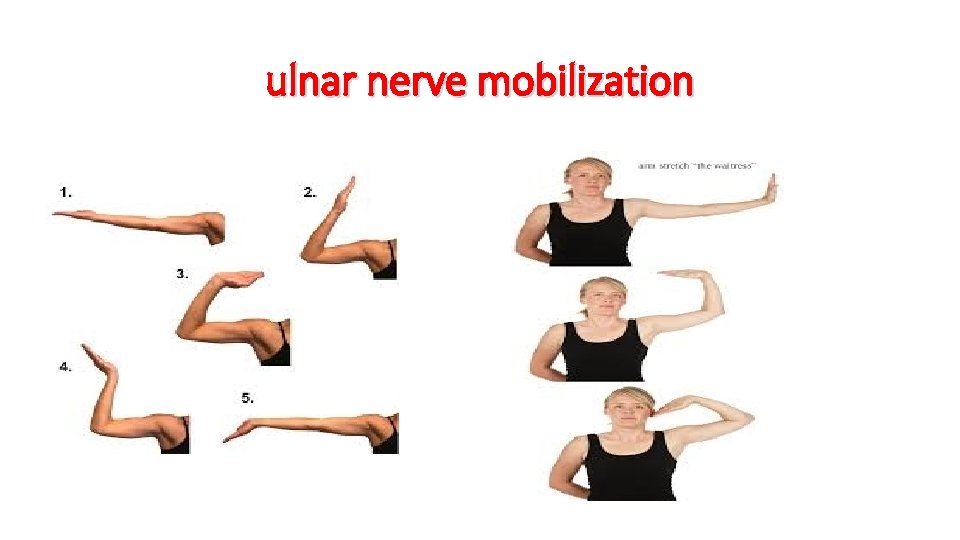
ulnar nerve mobilization

Exercises must not reproduce the distal nerve symptoms and may, there ore, initially need to be performed in limited arcs of motion to avoid putting tension on ulnar nerve.

Thank you
- Slides: 27