Cryo Nerve Block Therapy Pain Management in Cardiothoracic
Cryo Nerve Block Therapy Pain Management in Cardiothoracic Surgery Pain Management PM-US-0178 A-1020 -G

Agenda – Cryo Nerve Block Therapy (cryo. NB) • • Background Pain Sources in Cardiac / Thoracic Surgery Anatomy / Science Technique Pain Types / Multi-modal Analgesia Summary of Literature FROST Clinical Trial Recap Pain Management

Background Pain Management
What is cryo. NB? • cryo. NB is a procedure used to temporarily block nerve conduction along peripheral nerve pathways; similar to the effect of local anesthetics. • The procedure, which involves freezing targeted nerves, allows for the complete regeneration of the internal structure and function of the affected nerve. Image: Nerve Schematic. Digital image. Web. 2 Aug. 2018. https: //pixabay. com/en/neuron-nerve-cell-axon-dendrite-296581/ Pain Management

Opioid Dependence Incidence • 1 in 7 thoracotomy patients develop an opioid addiction • 1 in 11 for minimally invasive lung surgery patients The Society of Thoracic Surgeons. (2018, January 30). 1 in 7 Lung Surgery Patients at Risk for Opioid Dependence [Press release]. Retrieved August 2, 2018, from https: //www. sts. org/media/news-releases/1 -7 -lung-surgery-patients-risk-opioid-dependence Pain Management

Risk Factors • • Gender: Male Age: < 64 years old Income: < $70, 000 History of Substance Abuse • Hospital Stay: >5 days post-op • Post-Op Chemotherapy/Radiation The Society of Thoracic Surgeons. (2018, January 30). 1 in 7 Lung Surgery Patients at Risk for Opioid Dependence [Press release]. Retrieved August 2, 2018, from https: //www. sts. org/media/news-releases/1 -7 -lung-surgery-patients-risk-opioid-dependence Pain Management
Pain sources in Cardiac / Thoracic Surgery Pain Management
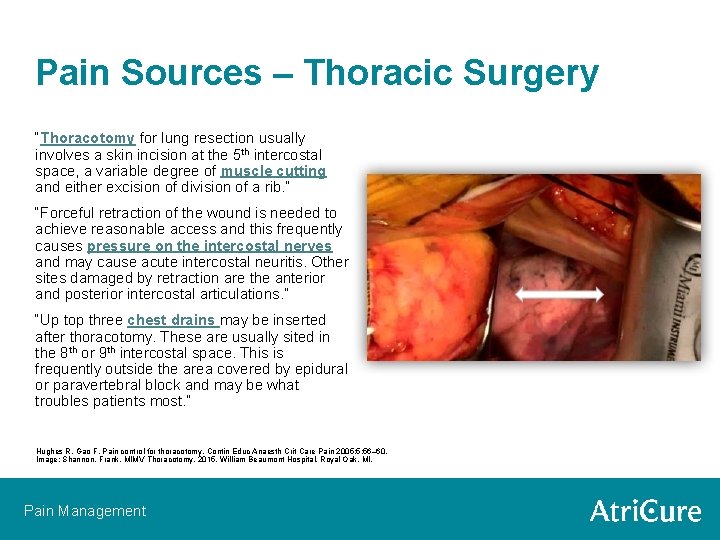
Pain Sources – Thoracic Surgery “Thoracotomy for lung resection usually involves a skin incision at the 5 th intercostal space, a variable degree of muscle cutting and either excision of division of a rib. ” “Forceful retraction of the wound is needed to achieve reasonable access and this frequently causes pressure on the intercostal nerves and may cause acute intercostal neuritis. Other sites damaged by retraction are the anterior and posterior intercostal articulations. ” “Up top three chest drains may be inserted after thoracotomy. These are usually sited in the 8 th or 9 th intercostal space. This is frequently outside the area covered by epidural or paravertebral block and may be what troubles patients most. ” Hughes R, Gao F. Pain control for thoracotomy. Contin Educ Anaesth Crit Care Pain 2005; 5: 56– 60. Image: Shannon, Frank. MIMV Thoracotomy. 2015. William Beaumont Hospital, Royal Oak, MI. Pain Management
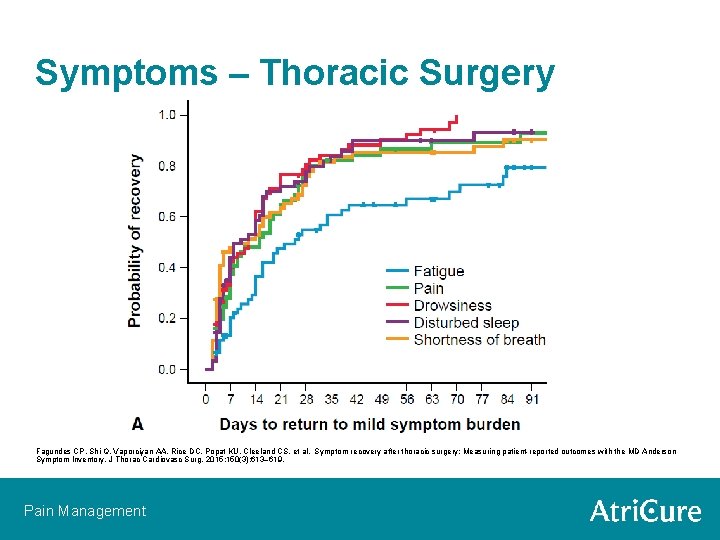
Symptoms – Thoracic Surgery Fagundes CP, Shi Q, Vaporciyan AA, Rice DC, Popat KU, Cleeland CS, et al. Symptom recovery after thoracic surgery: Measuring patient-reported outcomes with the MD Anderson Symptom Inventory. J Thorac Cardiovasc Surg. 2015; 150(3): 613– 619. Pain Management
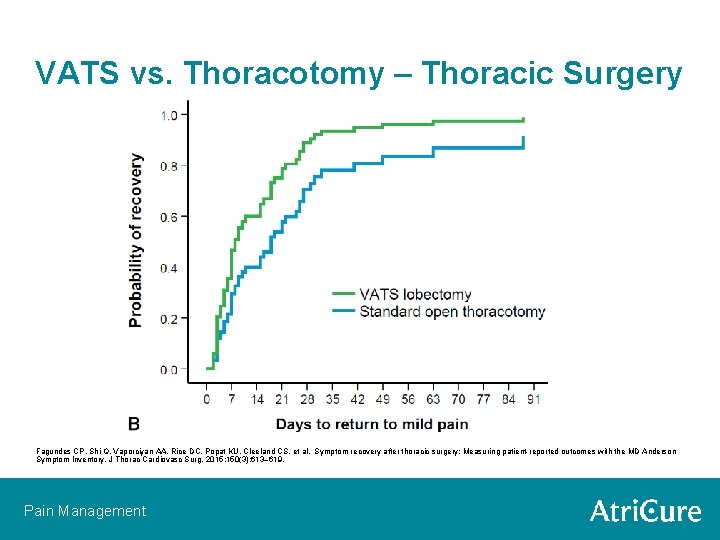
VATS vs. Thoracotomy – Thoracic Surgery Fagundes CP, Shi Q, Vaporciyan AA, Rice DC, Popat KU, Cleeland CS, et al. Symptom recovery after thoracic surgery: Measuring patient-reported outcomes with the MD Anderson Symptom Inventory. J Thorac Cardiovasc Surg. 2015; 150(3): 613– 619. Pain Management

Indication for cryo. NB • cryo. ICE® CRYO 2 Probe • November 2014 – FDA 510(k) clearance (K 142203) for a change in indication • “Atri. Cure’s cryo. ICE cryo-ablation probes are sterile, single use devices intended for use in the cryosurgical treatment of cardiac arrhythmias by freezing target tissues, creating inflammatory response (cryonecrosis) that blocks the electrical conduction pathway. The probe is also intended for use in blocking pain by temporarily ablating peripheral nerves. ” • cryo. ICE® cryo. SPHERE™ Probe • November 2018 – FDA 510(k) clearance (K 182565) • “Atri. Cure’s cryo. ICE cryo. SPHERE cryoablation probes are sterile, single use devices intended for use in blocking pain by temporarily ablating peripheral nerves. ” Pain Management
Pain Management Options Global Methods 1. Epidural analgesia 2. Spinal anesthesia 3. Intravenous pain medication 4. Oral Administration Image Left : Bruce Blaus / Wikimedia Commons / Public Domain Pain Management Local Methods 1. Paravertebral block 2. Local block 3. cryo. NB

Anatomy / Science Pain Management
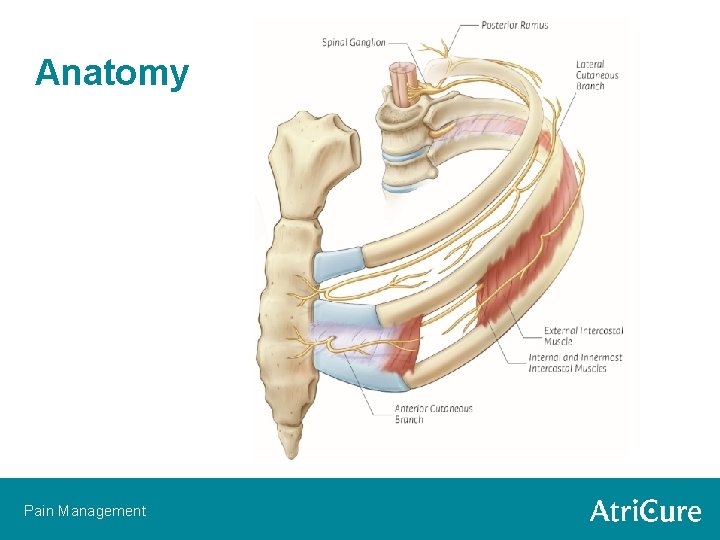
Anatomy Pain Management
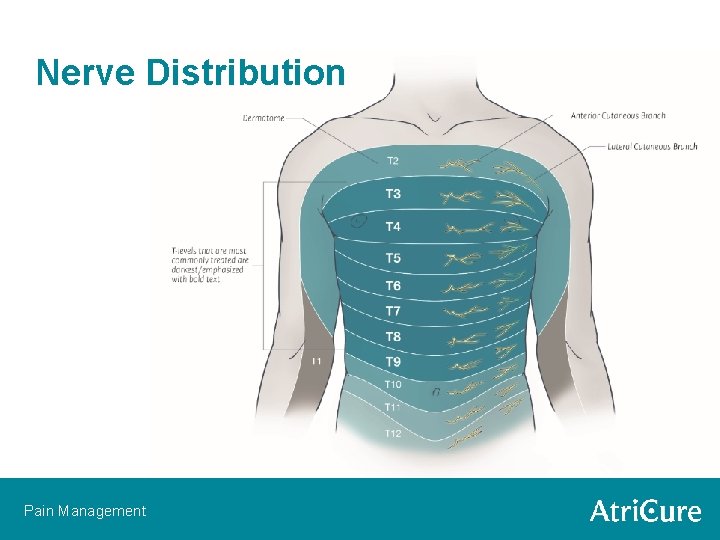
Nerve Distribution Pain Management
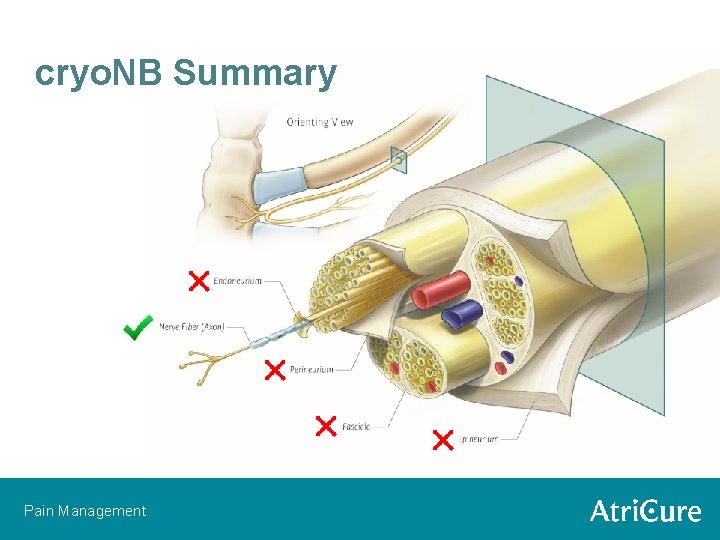
cryo. NB Summary Pain Management
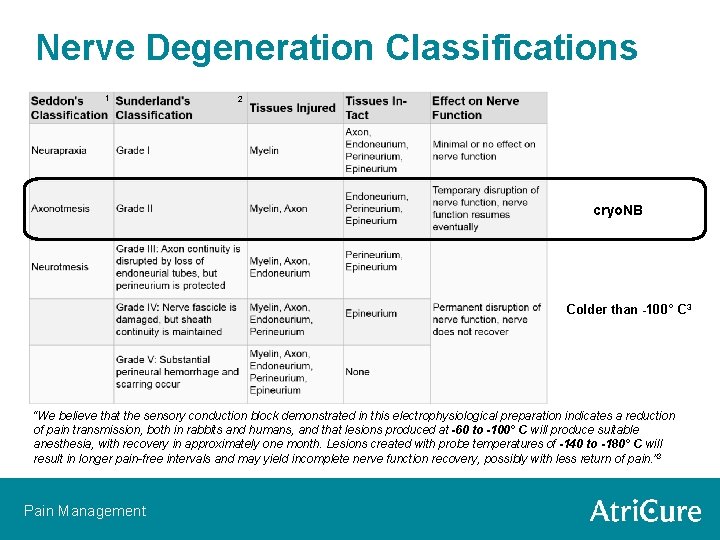
Nerve Degeneration Classifications 1 2 cryo. NB Colder than -100° C 3 “We believe that the sensory conduction block demonstrated in this electrophysiological preparation indicates a reduction of pain transmission, both in rabbits and humans, and that lesions produced at -60 to -100° C will produce suitable 1 Kaye, A. (1991). Classification of nerve injuries. Essential Neurosurgery. Churchill Livingstone, 333 -334. anesthesia, with recovery in approximately one month. Lesions created with probe temperatures of -140 to -180° C will 2 Greenberg, M. S. (1994). Injury classification system. Handbook of Neurosurgery, 3, 411 -412. 3 Zhou, L. , Shao, Z. , & Ou, S. (2003). Cryoanalgesia: electrophysiology at different temperatures. Cryobiology, 46(1), 26 -32. result in longer pain-free intervals and may yield incomplete nerve function recovery, possibly with less return of pain. ” 3 Pain Management

Wallerian Degeneration Well-described process resulting in temporary pain relief Gaudett, 2011. 1 Burnett, 2004. 2 Trescot, 2003. 3 Stoll, 2002. 4 Wang, 20125 1 Gaudet AD, Popovich PG, Ramer MS: Wallerian degeneration: gaining perspective on inflammatory events after peripheral nerve injury. J Neuroinflammation, 2011; 8: 110. 2 Burnett MG, Zager EL. Pathophysiology of peripheral nerve injury: a brief review. Neurosurg Focus. 2004; 16 : 1– 7. 3 Trescot AM. Cryoanalgesia in interventional pain management. Pain Physician. 2003; 6: 345 – 360. 4 Stoll G, Jander S, Myers RR. Degeneration and regeneration of the peripheral nervous system: From Augustus Waller's observations to neuroinflammation. J Peripher Nerv Syst. 2002; 7: 13– 27. 5 Image: Wang J. T. , Medress Z. A. , Barres B. A. Axon degeneration: molecular mechanisms of a self-destruction pathway. J. Cell Biol. 2012; 196: 7– 18. http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 3255986/figure/fig 1/ Pain Management
Technique Pain Management

cryo. SPHERE Procedural Guide • BEND PROBE to ensure optimal placement on the intercostal nerve. • LOCATE THE NERVE in the incisional intercostal space and place the probe on top of it. • The ball tip of the probe should be in or walked slightly off the intercostal groove. • Maintain gentle probe pressure on tissue throughout cryoablation. • Do not move the probe during cryoablation. Pain Management

cryo. SPHERE Procedural Guide • ABLATE at the margin of the membranous section of the intercostal muscle (Green Zone). • Maintain a distance of: • 2 cm from the ganglia • 4 cm from the base of the spine • Cryoablation time should be performed for 120 seconds. • The cryo. SPHERE probe is designed to operate within the -50 to -70°C range, which should be verified during ablation. Reference on File at Atri. Cure Pain Management

cryo. SPHERE Procedural Guide • Five total ablations are recommended: • Two intercostal spaces above the incision • Two below • One at the level of the incision itself • Cryoablation above the 3 rd intercostal space is not recommended due to proximity of the sympathetic trunk. • Cryoablation below the 9 th intercostal space may cause temporary abdominal muscle bulging. Reference on File at Atri. Cure Pain Management

cryo. SPHERE Procedural Guide • The therapeutic effect of cryo. NB will be a function of location of the nerve ablation and not the length of actual nerve ablated. • Degeneration of the nerve occurs from the cryoablation site to the end organ (towards the sternum). • As an ablation cycle ends, the probe’s ACTIVE DEFROST feature allows it to warm to ambient temperature. • The probe should be movable without resistance once the frost disappears. Reference on File at Atri. Cure Pain Management

cryo. NB: Technique / Duration • POST-OPERATIVELY, REGENERATION OF THE AXONS occurs from the cryoablation site to the end organ (towards the sternum). • Axons within the intercostal nerve that send pain signals are destroyed distal to the cryoablation site. • The tubule structures (epineurium, perineurium and endoneurium) of the nerve remain intact allowing the axons to regenerate and nerve function to resume over the course of roughly 1 -3 months. Reference on File at Atri. Cure Pain Management

Pain Types / Multi-modal Analgeisa Pain Management

Pain Types Nociceptive Pain Tissue Injury • cryo. NB primarily addresses Nociceptive Somatic Pain Somatic Visceral Skin, Soft Tissue, Skeletal Muscle Internal organs such as heart and lungs Neuropathic Pain Damage to Sensory Nerves Burning, Shooting, Electric, Tingling Inflammatory Pain Sharp, Aching, Squeezing, Stabbing, Throbbing Dull, Crampy, Achy Well Localized Poorly Localized Pain secondary to inflammation Pain Management

Multimodal Analgesia The use of more than one method or modality of controlling pain to obtain additive beneficial effects, reduce side effects, or both Cryoanalgesia is an adjunct to a surgeon’s multimodal pain management approach Examples of Post-Op Multimodal Therapies National Pharmaceutical Council. (n. d. ). Pain: Current Understanding of Assessment, Management, and Treatments [Press release]. Retrieved August 2, 2018, from http: //americanpainsociety. org/uploads/education/section_4. pdf Pain Management

Drug Family & Purpose Drug Family Acetaminophen Gabapentin NSAIDS Opioids Ketamine Pain Management Purpose Effective for noninflammatory pain, may be opioid-sparing Effective for neuralgic pain Effective for inflammatory pain, may decrease opioid requirements Effective for severe pain by acting on central and peripheral opioid receptors to inhibit the transmission of nociceptive input and perception of pain Has been used at subanesthetic doses as a N-methyl d-aspartate (NMDA) receptor antagonist to block the processing of nociceptive input in chronic pain syndromes

Chronic Post-Thoracotomy Pain Chronic post-thoracotomy pain syndrome • Chest incisional or chest wall pain lasting > 3 months • Incidence ranges: • 57% (17 Studies)1 • 30 -60% (5 Studies)2 • 9 -80% Thoracotomy; 5 -33% VATS (14 Studies)3; No difference found between Thoracotomy and VATS groups • Neuropathic pain features in 75% of this syndrome 2 Risk factors for chronic post-thoracotomy and neuropathic pain • Severe post-op pain, pre-op pain, female, age <602 1 Bayman, E. O. , Parekh, K. R. , Keech, J. , Selte, A. , & Brennan, T. J. (2017). A prospective study of chronic pain after thoracic surgery. Anesthesiology: The Journal of the American Society of Anesthesiologists, 126(5), 938 -951. 2 Niraj, G. , Kelkar, A. , Kaushik, V. , Tang, Y. , Fleet, D. , Tait, F. , . . . & Rathinam, S. (2017). Audit of postoperative pain management after open thoracotomy and the incidence of chronic postthoracotomy pain in more than 500 patients at a tertiary center. Journal of clinical anesthesia, 36, 174 -177. 3 Maguire, M. F. , Latter, J. A. , Mahajan, R. , Beggs, F. D. , & Duffy, J. P. (2006). A study exploring the role of intercostal nerve damage in chronic pain after thoracic surgery. European journal of cardio-thoracic surgery, 29(6), 873 -879. Pain Management

Peripheral & Central Sensitization Peripheral sensitization Increased responsiveness and reduced threshold of nociceptive neurons in the periphery to the stimulation of their receptive fields. Central sensitization Increased responsiveness of nociceptive neurons to their normal input, and/or recruitment of a response to normally subthreshold inputs. Allodynia Pain elicited by a stimulus that normally does not cause pain • Temperature or physical stimuli can provoke allodynia, which may feel like a burning sensation 1 Hyperalgesia Increased pain response produced by stimulus that normally would not be a cause for pain 2 1 Hooshmand, 2 Purves, H. (1993). Referred pain and trigger point. Chronic Pain, Reflex Sympathetic Dystrophy Prevention and Management, 83 -84. D. , Augustine, G. J. , & Fitzpatrick, D. (2001). et al. , editors. Hyperalgesia and Sensitization. Neuroscience. Sunderland (MA). Pain Management

International Association for the Study of Pain (IASP) Definitions 1 • Allodynia • Multimodal Treatment • Analgesia • Neuralgia • Anesthesia Dolorosa • Neuritis • Causalgia • Neuropathic Pain • Dysesthesia • Peripheral Neuropathic Pain • Hyperalgesia • Neuropathy • Hyperesthesia • Nociception • Hyperpathia • Nociceptive Neuron • Hypoalgesia • Nociceptive Pain • Hypoesthesia 1 Merskey, H. (1994). PART III pain terms, a current list with definitions and notes on usage. Classification of chronic pain-Descriptions of chronic pain syndromes and definitions of pain terms, 207 -214. http: //www. iasp-pain. org/Education/Content. aspx? Item. Number=1698 Pain Management

International Association for the Study of Pain (IASP) Definitions 1 • Nociceptive Stimulus • Nociceptor • Nociplastic Pain • Noxious Stimulus • Pain Threshold • Pain Tolerance Level • Paresthesia • Sensitization • Central Sensitization • Unimodal Treatment 1 Merskey, H. (1994). PART III pain terms, a current list with definitions and notes on usage. Classification of chronic pain-Descriptions of chronic pain syndromes and definitions of pain terms, 207 -214. http: //www. iasp-pain. org/Education/Content. aspx? Item. Number=1698 Pain Management
Summary of Literature Pain Management

cryo. NB Literature Reviewed 19 clinical studies reviewed from 1980 -2013 for post-thoracotomy pain management using cryo. NB: Study designs • 18 randomized, controlled trials • 1 single arm trial Surgical procedures • Most (18) for thoracic procedures • Only (1) for cardiac procedures- mini-thoracotomy for CABG/VR Conclusions regarding cryo. NB • Supported – 9 • Neutral – 3 • Unsupported – 7 Pain Management
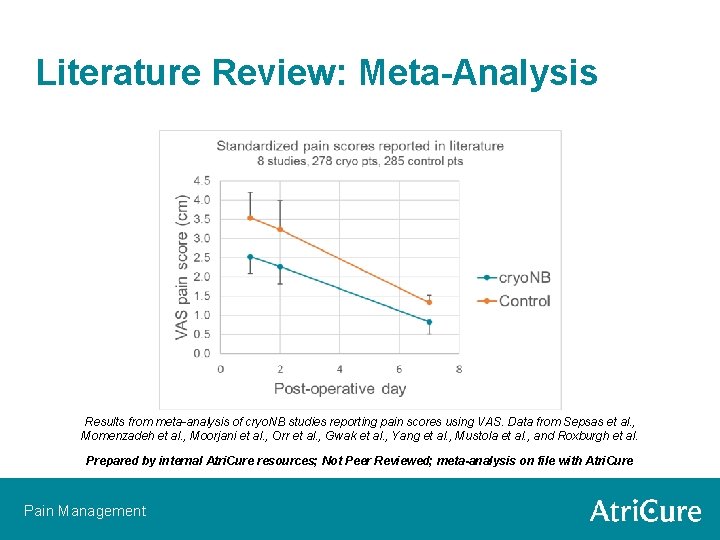
Literature Review: Meta-Analysis Results from meta-analysis of cryo. NB studies reporting pain scores using VAS. Data from Sepsas et al. , Momenzadeh et al. , Moorjani et al. , Orr et al. , Gwak et al. , Yang et al. , Mustola et al. , and Roxburgh et al. Prepared by internal Atri. Cure resources; Not Peer Reviewed; meta-analysis on file with Atri. Cure Pain Management
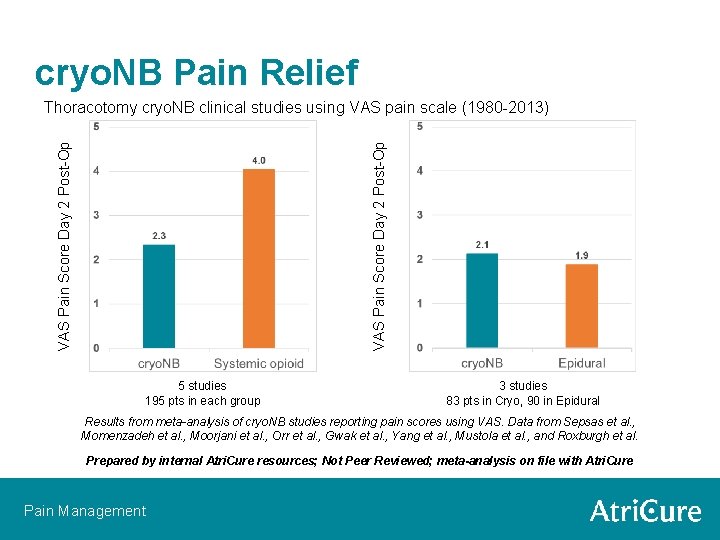
cryo. NB Pain Relief VAS Pain Score Day 2 Post-Op Thoracotomy cryo. NB clinical studies using VAS pain scale (1980 -2013) 5 studies 195 pts in each group 3 studies 83 pts in Cryo, 90 in Epidural Results from meta-analysis of cryo. NB studies reporting pain scores using VAS. Data from Sepsas et al. , Momenzadeh et al. , Moorjani et al. , Orr et al. , Gwak et al. , Yang et al. , Mustola et al. , and Roxburgh et al. Prepared by internal Atri. Cure resources; Not Peer Reviewed; meta-analysis on file with Atri. Cure Pain Management
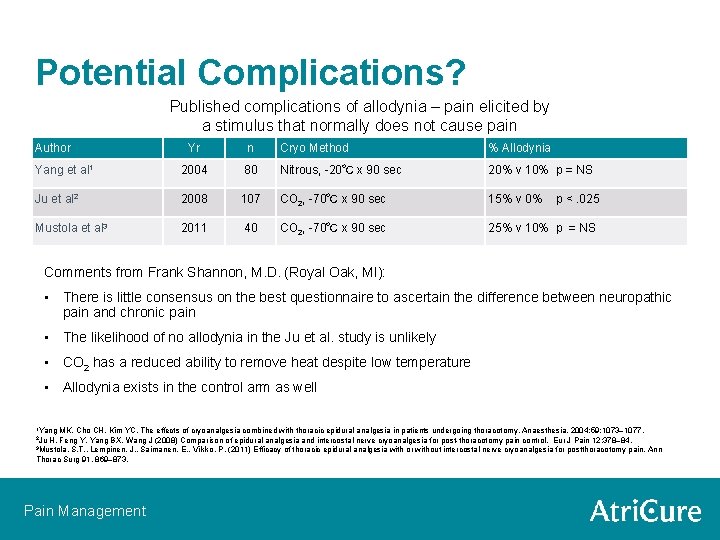
Potential Complications? Published complications of allodynia – pain elicited by a stimulus that normally does not cause pain Author Yr n Cryo Method % Allodynia Yang et al 1 2004 80 Nitrous, -20℃ x 90 sec 20% v 10% p = NS Ju et al 2 2008 107 CO 2, -70℃ x 90 sec 15% v 0% Mustola et al 3 2011 40 CO 2, -70℃ x 90 sec 25% v 10% p = NS p <. 025 Comments from Frank Shannon, M. D. (Royal Oak, MI): • There is little consensus on the best questionnaire to ascertain the difference between neuropathic pain and chronic pain • The likelihood of no allodynia in the Ju et al. study is unlikely • CO 2 has a reduced ability to remove heat despite low temperature • Allodynia exists in the control arm as well 1 Yang MK, Cho CH, Kim YC. The effects of cryoanalgesia combined with thoracic epidural analgesia in patients undergoing thoracotomy. Anaesthesia. 2004; 59: 1073– 1077. H, Feng Y, Yang BX, Wang J (2008) Comparison of epidural analgesia and intercostal nerve cryoanalgesia for post-thoracotomy pain control. Eur J Pain 12: 378– 84. 3 Mustola, S. T. , Lempinen, J. , Saimanen, E. , Vilkko, P. (2011) Efficacy of thoracic epidural analgesia with or without intercostal nerve cryoanalgesia for postthoracotomy pain. Ann Thorac Surg 91, 869– 873. 2 Ju Pain Management
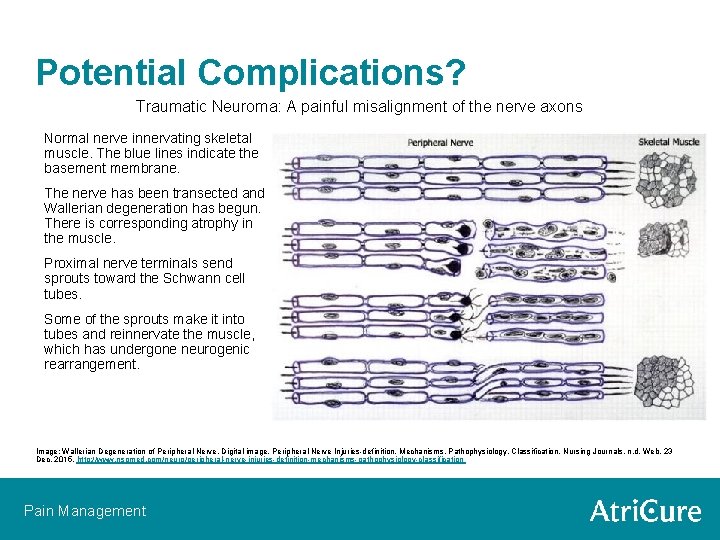
Potential Complications? Traumatic Neuroma: A painful misalignment of the nerve axons Normal nerve innervating skeletal muscle. The blue lines indicate the basement membrane. The nerve has been transected and Wallerian degeneration has begun. There is corresponding atrophy in the muscle. Proximal nerve terminals send sprouts toward the Schwann cell tubes. Some of the sprouts make it into tubes and reinnervate the muscle, which has undergone neurogenic rearrangement. Image: Wallerian Degeneration of Peripheral Nerve. Digital image. Peripheral Nerve Injuries-definition, Mechanisms, Pathophysiology, Classification. Nursing Journals, n. d. Web. 23 Dec. 2015. http: //www. nsgmed. com/neuro/peripheral-nerve-injuries-definition-mechanisms-pathophysiology-classification Pain Management
FROST Clinical Trial Pain Management

FROST: cryo. NB Study The cryo. ICE cryo. NB study For pain management in post tho. Racic procedures via interc. OSTal cryoanalgesia- FROST Objective: To demonstrate that intraoperative intercostal cryoanalgesia in conjunction with standard of care provides improved analgesic efficacy in patients undergoing unilateral thoracotomy cardiac procedures as compared to current standard of care ≤ 100 Subjects 3: 1 Randomization (Blinded) 5 Centers Pain Management ~75 Subjects ~25 Control Cryo. A + SOC
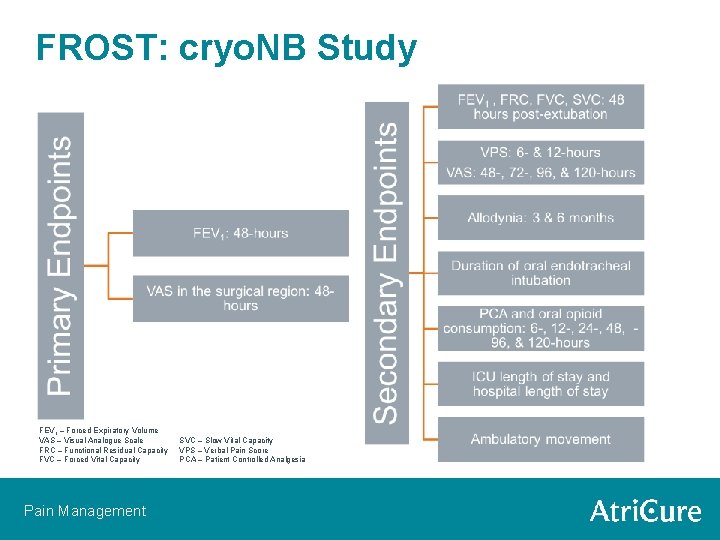
FROST: cryo. NB Study FEV 1 – Forced Expiratory Volume VAS – Visual Analogue Scale FRC – Functional Residual Capacity FVC – Forced Vital Capacity Pain Management SVC – Slow Vital Capacity VPS – Verbal Pain Score PCA – Patient Controlled Analgesia

FROST: cryo. NB Study Lead Principal Investigators Wei C. Lau, M. D. Department of Anesthesiology Division Cardiovascular Anesthesiology Beaumont Health System, Royal Oak, MI Francis L. Shannon, M. D. Director, Cardiovascular Research and Quality Assurance Beaumont Health System, Royal Oak, MI Scientific Advisor Andrea Trescot, M. D. Interventional Pain Physician Locations Beaumont Health System, Royal Oak, MI University of Michigan, Ann Arbor, MI University of Southern California, Los Angeles, CA United Hospital, St. Paul, MN Procedure – Control Arm • Pain management prescribed by attending physician or institutional SOC Procedure – Study Arm • Pain management prescribed by attending physician or institutional SOC • Cryoanalgesia • At the thoracotomy level • One to two intercostal spaces above • Two intercostal spaces below • At the level of the chest tube (recommended, but not required) • One or more intercostal nerve blocks (0. 5% Marcaine or equivalent) – acute pain management Pain Management

Recap Pain Management

Analgesia is a dynamic and multipronged algorithm • cryo. NB is a compliment to current analgesia Standard of Care (SOC) • cryo. NB is not a direct replacement for pain management • Consider the use of multi-modal analgesia • cryo. NB lasts longer than epidurals; up to several months depending on nerve regeneration Pain Management

Technique and Technology Matter • Time: 120 seconds • Temperature: -50°C to -70°C • Technique: 2 above, 2 below, 1 @ level of incision • Do not ablate the incision site • Earlier in the procedure is better • Minimum 4 cm from base of spine; 2 cm from ganglia • Posterior to the mid-axillary line • Active defrost helps avoid mechanical injury to nerve by allowing for easy probe removal • Above the 3 rd and below the 9 th are not recommended • Maintain gentle probe pressure on tissue throughout cryo. NB Pain Management
- Slides: 45