CRT Washington DC February 24 2013 The Management

CRT Washington, DC February 24, 2013 The Management of Carotid Artery Disease: Who and When? Michael R. Jaff, DO, FACC Associate Professor of Medicine Harvard Medical School Chair, MGH Institute for Heart, Vascular, and Stroke Care Boston, Massachusetts 1

Michael R. Jaff, DO • Consultant – Abbott Vascular (non-compensated) • – American Genomics, Inc – Becker Venture Services Group – Bluegrass Vascular Therapies – Cordis Corporation(non-compensated) – Covidien (non-compensated) – Ekos Corporation (DSMB) – Hansen Medical – Medtronic (non-compensated) – Micell, Incorporated – Primacea – Trivascular, Inc. • Equity – Access Closure, Inc – Embolitech, Inc – Hotspur, Inc – Icon Interventional, Inc – I. C. Sciences, Inc – Janacare, Inc – Northwind Medical, Inc. – PQ Bypass, Inc – Primacea – Sadra Medical – Sano V, Inc. – TMI/Trireme, Inc – Vascular Therapies, Inc Board Member – VIVA Physicians (Not For Profit 501(c) 3 Organization) • www. vivapvd. com

Let Me Show You All My Cards Before We Start… • I am not a vascular surgeon • I am not an interventionist • I am not a neurologist • So, what the heck am I doing here? 3

What Is My Goal? • Provide just the facts, and let you make your decision 4

Stroke Statistics—Is This Really a Big Problem? • ~795, 000 new/recurrent strokes each year – 610, 000 first stroke – 185, 000 recurrent events 5 Circulation 2012; 125: e 2 -e 220
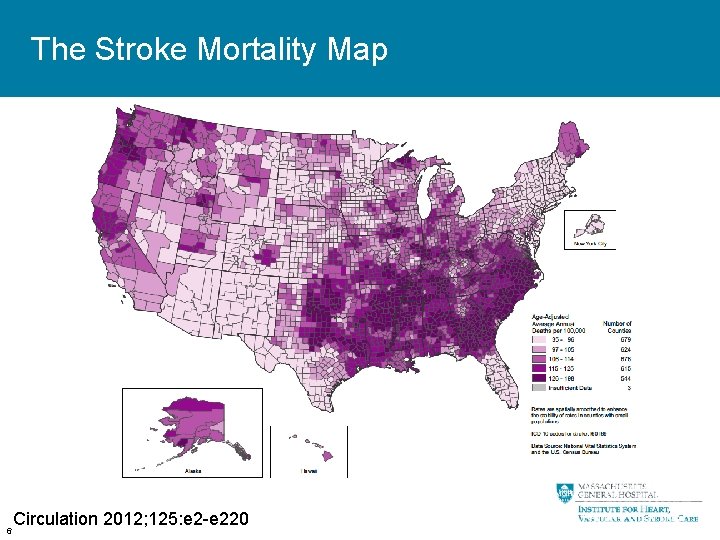
The Stroke Mortality Map 6 Circulation 2012; 125: e 2 -e 220

Stroke Stats • Fourth leading cause of death in the US – 134, 138 deaths in 2008 – 1 out of 18 deaths due to stroke in US • One American dies of a stroke every 4 minutes • Most common cause of adult disability – 31% of stroke survivors receive outpatient rehabilitation • 50% with some hemiparesis • 30% unable to walk without some assistance • 26% dependent in ADLs • 35% depressed • 26% institutionalized in a nursing home Circulation 2012; 125: e 2 -e 220

Stroke Costs • Total cost of stroke care 2005 -2050 (in 2005 dollars) $1. 52 Trillion---Non-Hispanic Whites $313 Billion---Hispanics $379 Billion---Blacks Circulation 2012; 125: e 2 -e 220
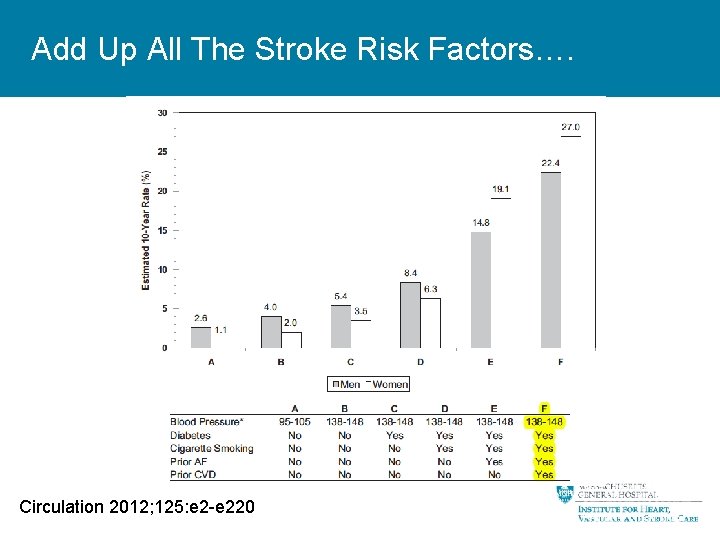
Add Up All The Stroke Risk Factors…. Circulation 2012; 125: e 2 -e 220

Recommendations for Primary Stroke Prevention • ASA • SBP <140 mm. Hg/DBP <90 mm. Hg • Abstinence from cigarette smoking • Diabetes • Hypertension – JNC VII Blood Pressure Control (ACEI/ARB) • Hypercholesterolemia – Statins for LDL goal NCEP/ATP III Goals Stroke 2011; 42: 517 -84
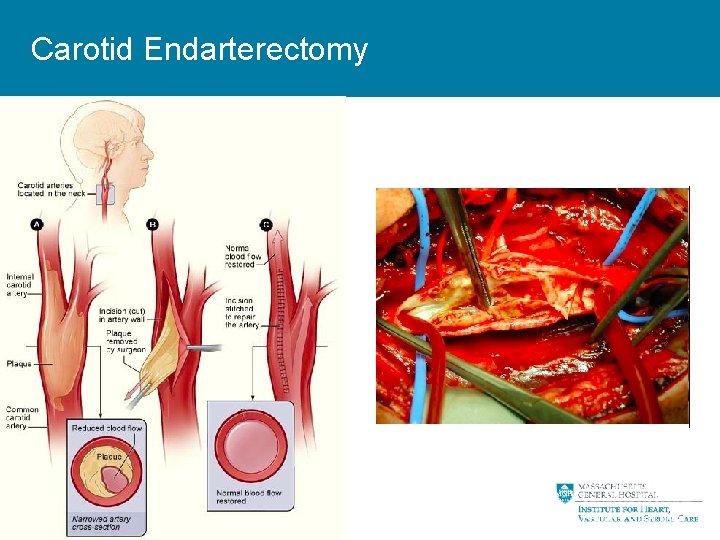
Carotid Endarterectomy
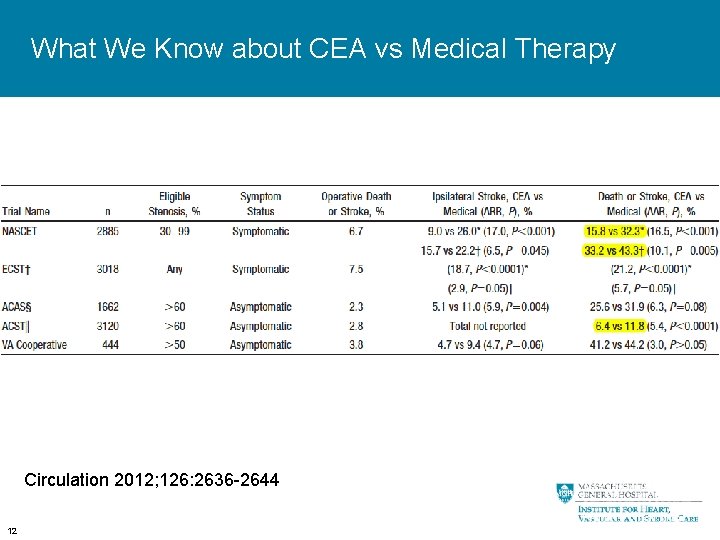
What We Know about CEA vs Medical Therapy Circulation 2012; 126: 2636 -2644 12
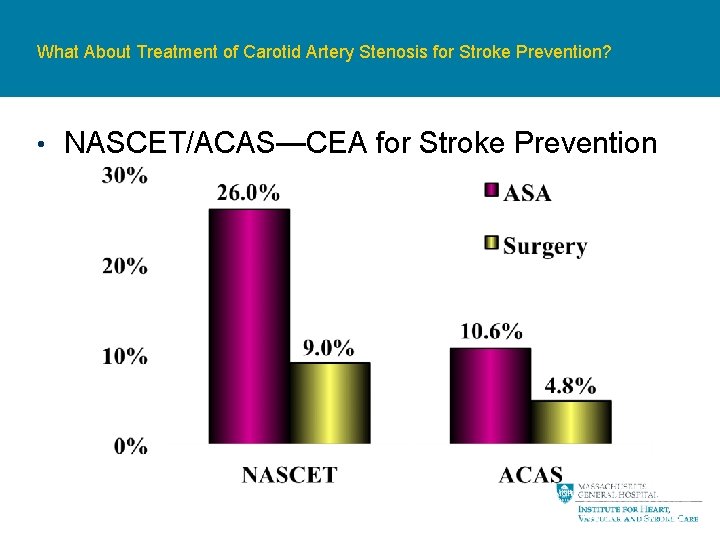
What About Treatment of Carotid Artery Stenosis for Stroke Prevention? • NASCET/ACAS—CEA for Stroke Prevention

Why Carotid Endarterectomy? • Procedure has been around for a long time (over 50 years) • Techniques perfected • Results repeatedly solid • The gold standard • Patients often discharged within 24 hours • Never see the inside of an ICU
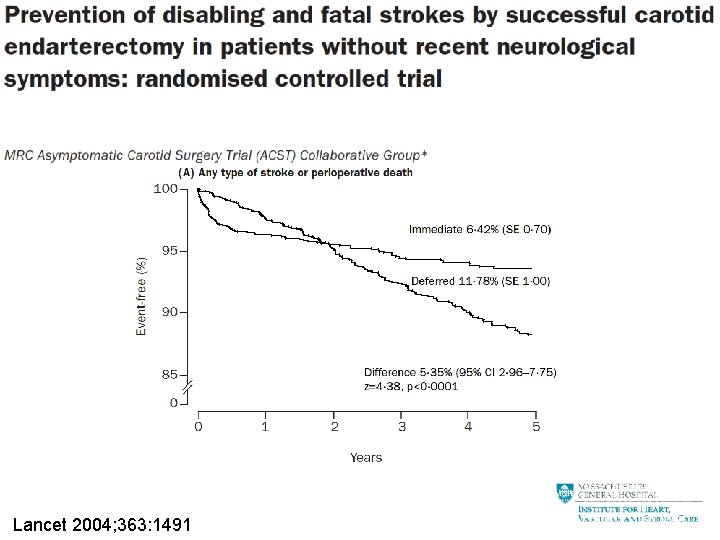
Lancet 2004; 363: 1491
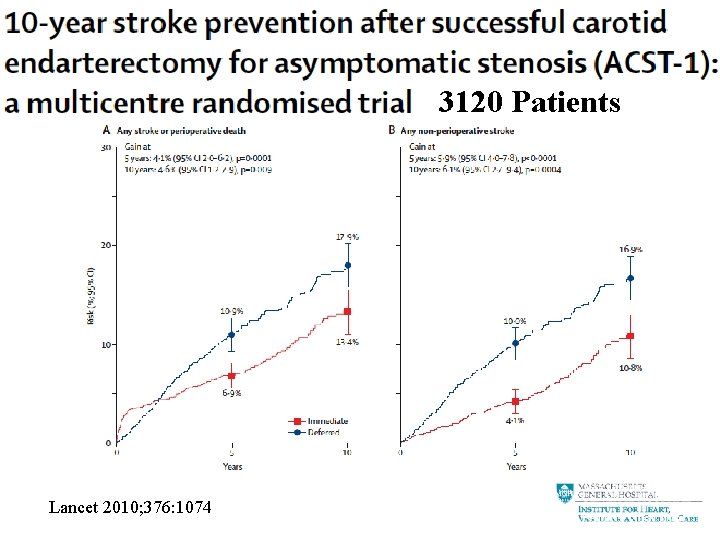
3120 Patients Lancet 2010; 376: 1074

Are There Patients at High Risk for CEA? 17 Circulation 2012; 126: 2636 -2644
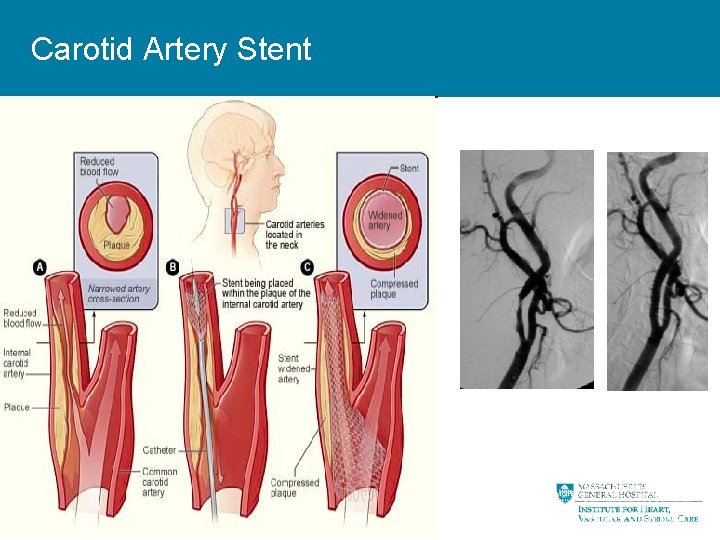
Carotid Artery Stent 18

Why Carotid Stenting? • No surgical incision • No need for general anesthesia – Conscious Sedation • Useful in patients at high risk for CEA 19
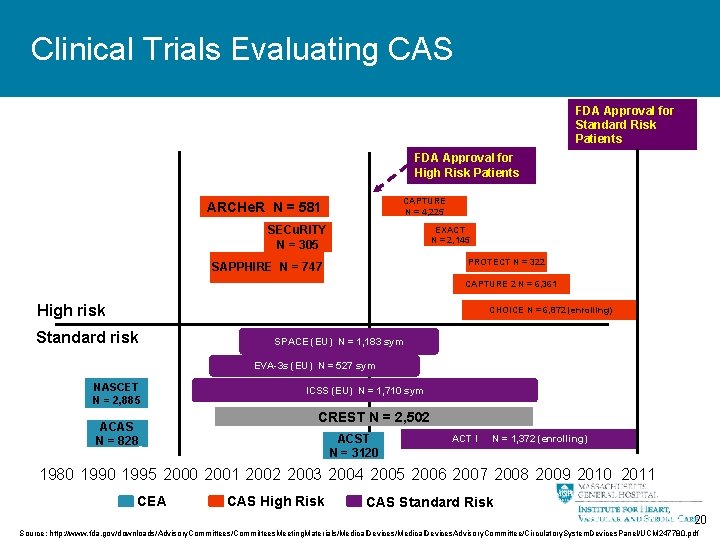
Clinical Trials Evaluating CAS FDA Approval for Standard Risk Patients FDA Approval for High Risk Patients CAPTURE N = 4, 225 ARCHe. R N = 581 SECu. RITY N = 305 EXACT N = 2, 145 PROTECT N = 322 SAPPHIRE N = 747 CAPTURE 2 N = 6, 361 High risk CHOICE N = 6, 872 (enrolling) Standard risk AHA Guidelines (pub. 1995) NASCET N = 2, 885 ACAS N = 828 SPACE(EU) NN==1, 183 sym EVA-3 s (EU) N = 527 sym ICSS (EU) N = 1, 710 sym CREST N = 2, 502 ACST N = 3120 = 1, 372 (enrolling) ACTACT I IN =N 1, 372 (enrolling) 1980 1995 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 2010 2011 CEA CAS High Risk CAS Standard Risk 20 Source: http: //www. fda. gov/downloads/Advisory. Committees/Committees. Meeting. Materials/Medical. Devices. Advisory. Committee/Circulatory. System. Devices. Panel/UCM 247780. pdf

All Leading Up to the Mother of All Carotid Trials… N Engl J Med 2010; 363: 11 -23
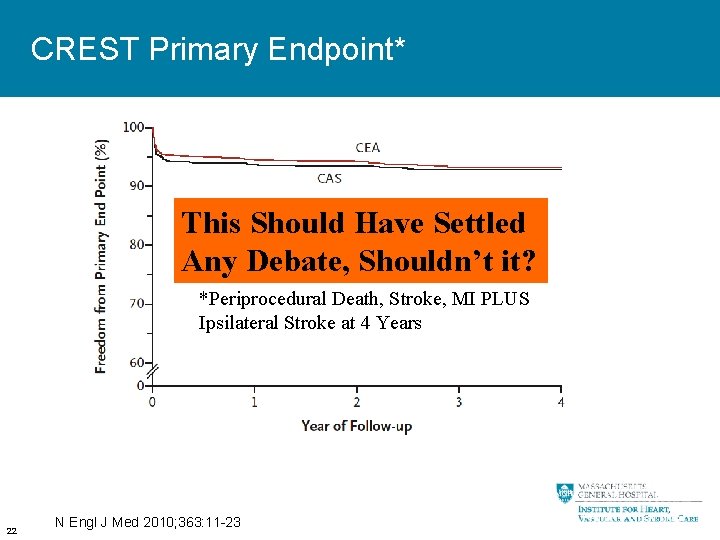
CREST Primary Endpoint* This Should Have Settled Any Debate, Shouldn’t it? *Periprocedural Death, Stroke, MI PLUS Ipsilateral Stroke at 4 Years 22 N Engl J Med 2010; 363: 11 -23

Why Didn’t CREST End the Debate? • Surgeons feel that carotid revascularization is performed for stroke prevention • CEA reduced stroke risk more than CAS • Excess MI rate with CEA less of an issue • Interventionists feel that CAS performed as safely as CEA • Excess stroke risk was minor stroke only • MI risk of CEA is important • Neurologists feel that although outcomes were low, medical therapy is more effective than any revascularization 23
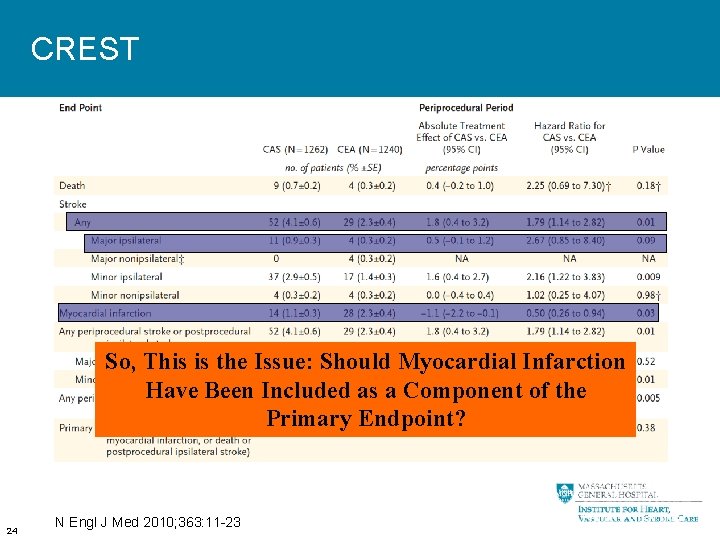

CREST So, This is the Issue: Should Myocardial Infarction Have Been Included as a Component of the Primary Endpoint? 24 N Engl J Med 2010; 363: 11 -23

J Am Coll Cardiol 2003; 42: 1547 -54 25
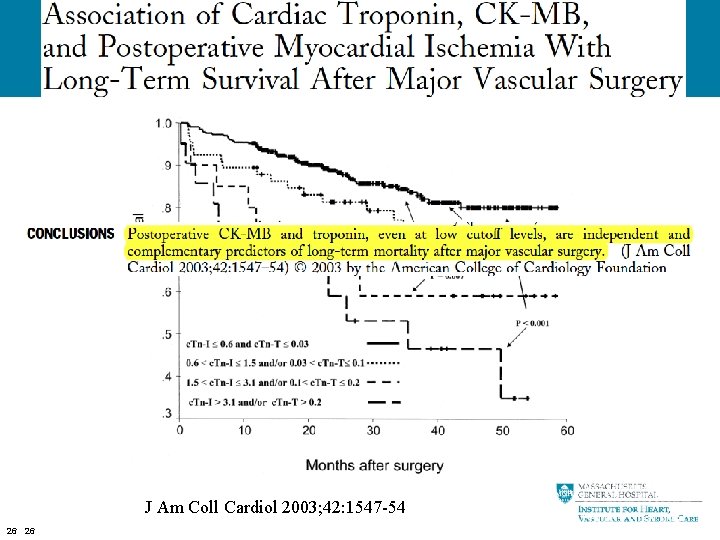
J Am Coll Cardiol 2003; 42: 1547 -54 26 26
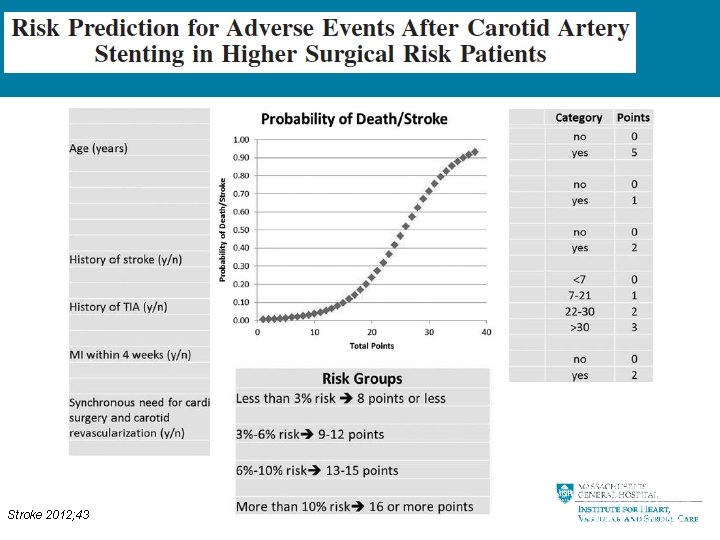
Stroke 2012; 43

What is Public Opinion?
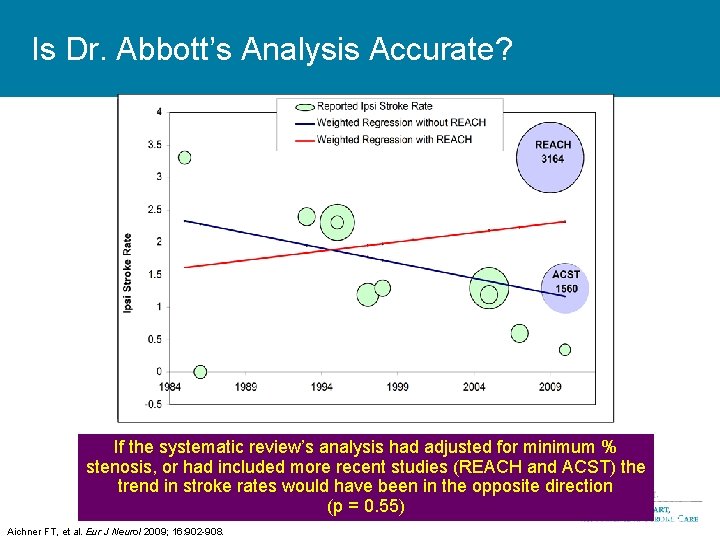
Is Dr. Abbott’s Analysis Accurate? If the systematic review’s analysis had adjusted for minimum % Largest and most recent REACH study (N = 3164) stenosis, or had included more recent studies (REACH and ACST) the The Change in Minimum Stenosis Thresholds in Studies Trend sensitive to effects of early study published after the systematic review contradicts the trend Over in stroke would have been in the opposite direction Timerates Mirrors the Reported Decline In Stroke Rates with more review (pcomplex = findings 0. 55) patients Aichner FT, et al. Eur J Neurol 2009; 16: 902 -908.

Enough Controversy? Oh No…. 30

CREST: No Difference in Cost-Effectiveness

Stroke 2012; 43: 2408 -2416 32

We Have Got To Stop Debating in the Lay Press….

So, Can I Make Sense of the Data? Firstly, it still never ceases to amaze me how even after Level A Multicenter Randomized Trials that Meet the Primary Endpoint, Physicians Don’t Agree on the Interpretation Options for Patients with Carotid Artery Disease 34 • CEA: Effective when performed by skilled surgeons with excellent track record • CAS: Effective when performed by skilled interventionists • Medical Therapy: Still must be tested head-to-head with revascularization, but impact likely improving—

Current and Future Investigation: What’s on the Horizon? ? ? • Asymptomatic Patients (standard surgical risk): D E P P – ACT I study to complete 1658 patient TO randomized S T S U J I T enrollments CAS vs. CEA AC ! ! ! O N

Current and Future Investigation: What’s on the Horizon? ? ? • Asymptomatic Patients (standard surgical risk): – ACT I study to complete 1658 patient randomized enrollments CAS vs. CEA – ACST 2 and SPACE 2 underway in Europe • High surgical risk: – New US studies to enroll shortly for: • Proximal protection via direct carotid access (Silk Road) • Mesh-covered stent (WL Gore) • CREST 2 application for funding pending 2 nd review by NIH – Asymptomatic patients with OMT vs. revascularization + OMT 36
37
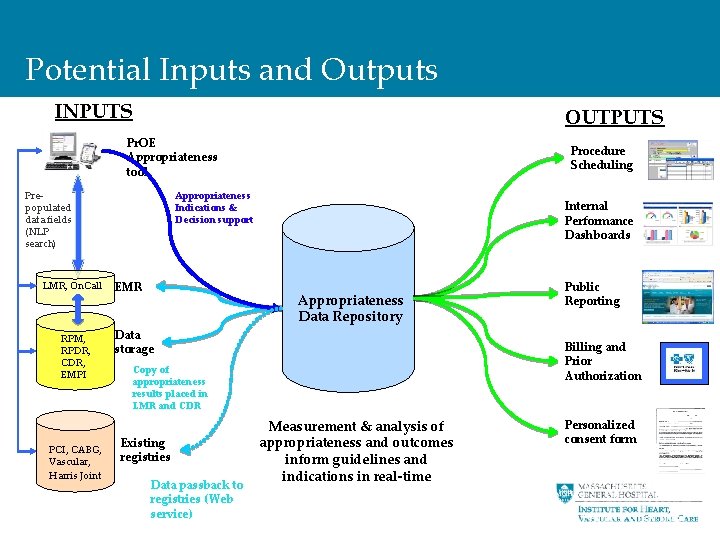
Potential Inputs and Outputs INPUTS OUTPUTS Pr. OE Appropriateness tool Prepopulated data fields (NLP search) LMR, On. Call RPM, RPDR, CDR, EMPI PCI, CABG, Vascular, Harris Joint Procedure Scheduling Appropriateness Indications & Decision support EMR Internal Performance Dashboards Appropriateness Data Repository Data storage Billing and Prior Authorization Copy of appropriateness results placed in LMR and CDR Existing registries Data passback to registries (Web service) Public Reporting Measurement & analysis of appropriateness and outcomes inform guidelines and indications in real-time Personalized consent form
- Slides: 38