CRT 2020 February 2020 Washington DC USA Costeffectiveness

CRT 2020 February 2020 Washington, DC, USA Cost-effectiveness of LAA Closure Sameer Gafoor 1, 2 1 CVC Frankfurt: Jennifer Franke, Simon Lam, Stefan Bertog, Laura Vaskelyte, Ilona Hofmann, Markus Reinartz, Horst Sievert 2 Swedish Heart and Vascular: Ming Zhang, John Petersen II, Eric Lehr, Madalena Petrescu, Nimish Muni, Paul Huang, Darryl Wells, Adam Zivin, Eric Williams, Robert Bersin, Glenn Barnhart, Samuel Youssef, Pat Ryan, Irina Penev, Amanda Ray, Michelle Batjargal, Thearry Deap, Zachary Newhart, David Mazza, Heather Garcia CVC: Cardio. Vascular Center Frankfurt, Germany Swedish Heart and Vascular: Swedish Medical Center, Seattle, WA, USA

A step back…


How much is this costing us? • Review of 184 population studies – 2010: 33. 5 million cases, 5 million new/year – US: 1. 2 million cases in 2010 to 2. 6 million by 2030 • Why is prevalence increasing – Other interventions and medications that increase lifespan – 0. 5 -1%, more with age – 2010: 596. 2/100, 000 men and 373. 1/100, 000 female
What about hospitalizations? • 3, 960, 011 hospitalizations with afib as primary diagnosis from 2000 -2010 • Majority with Medicare/Medicaid as primary payer (70%) • South: 38. 5%, Midwest 24. 9%, Northeast 22. 2%, West 14. 4% • Co-morbidities of HTN, DM, COPD • Length of stay is 3 days • From 2000 -2010, Decrease in going home (80% now 70%) and now more likely to facility (8. 1% to 11. 5%)
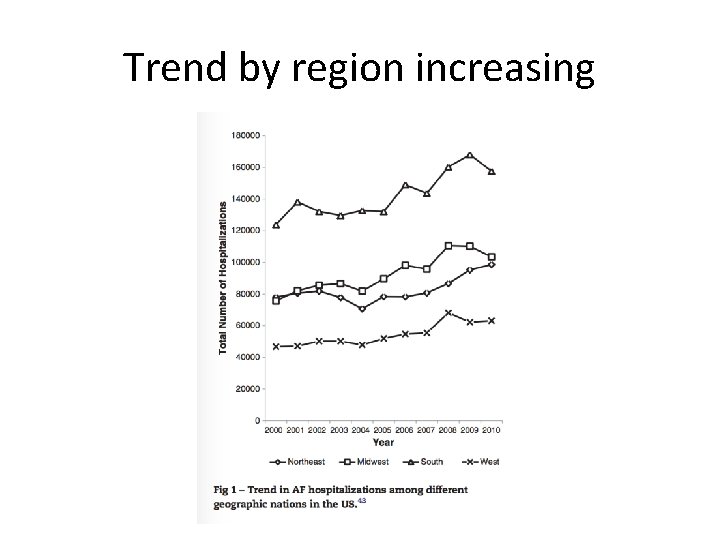
Trend by region increasing
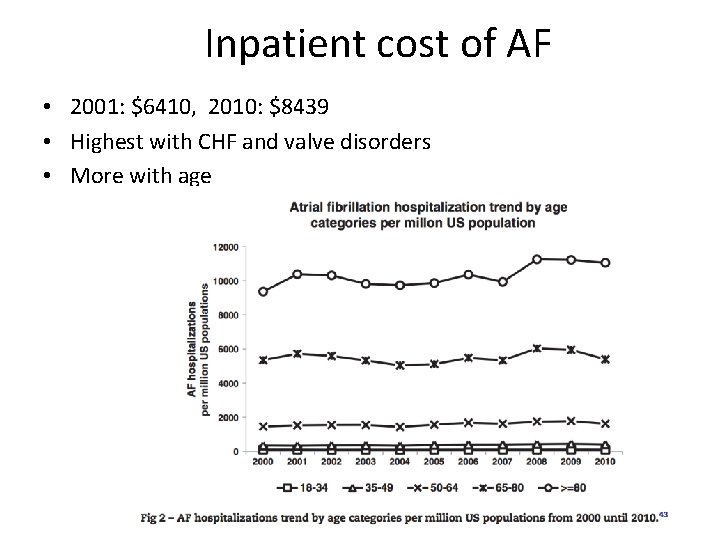
Inpatient cost of AF • 2001: $6410, 2010: $8439 • Highest with CHF and valve disorders • More with age
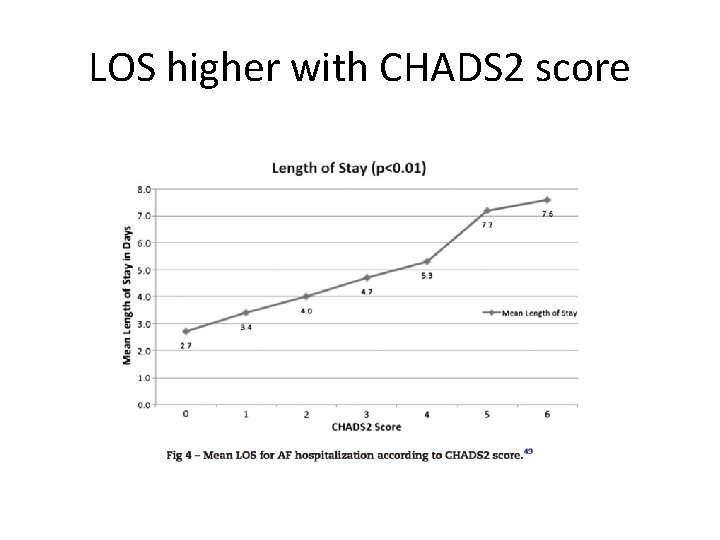
LOS higher with CHADS 2 score
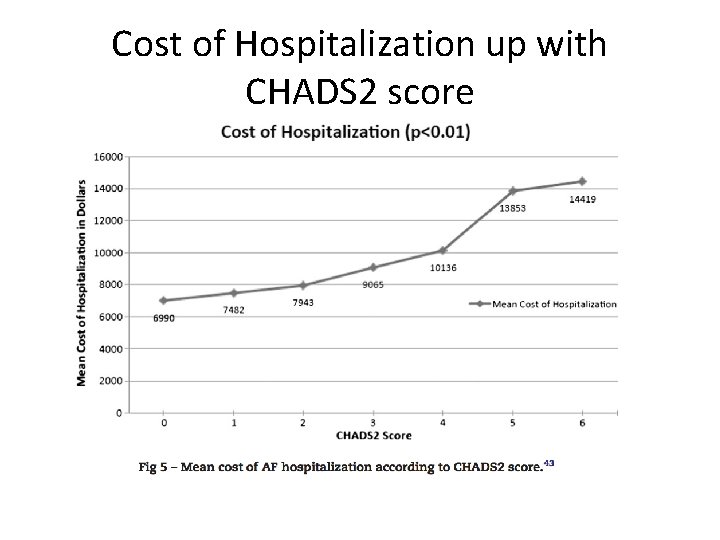
Cost of Hospitalization up with CHADS 2 score

What is a cost-effectiveness analysis? • Relative costs from each course of action • Gives you a ratio – Numerator is cost associated with health gain – Denominator is gain in health associated • Common outcomes – Quality-adjusted life years • ICER = Incremental cost-effectiveness ratio Cost per QALY is important (<$50, 000/QALY in US, € 30, 000/QALY in Europe)

What is a cost-utility analysis? • Usually four quadrants with a cost-effectiveness plane (costs on y axis, QALY gained on x axis) I. less effective & more expensive III. Less effective & less expensive II: more effective & more expensive IV. More effective & less expensive

What about patients who are candidates for warfarin?
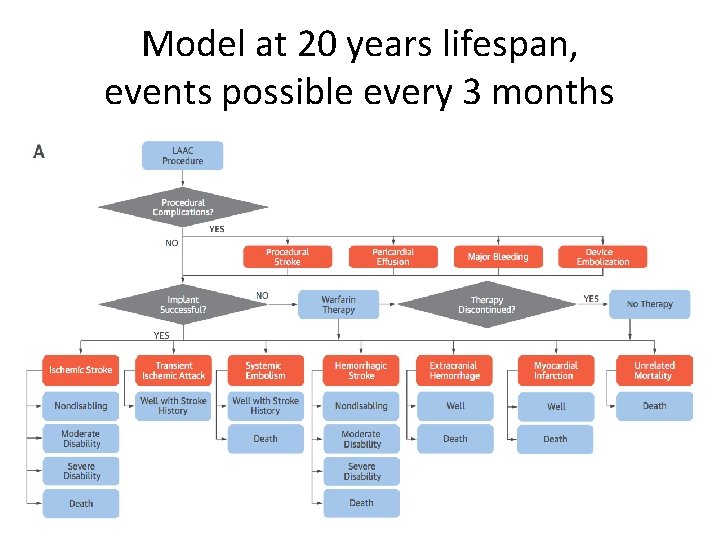
Model at 20 years lifespan, events possible every 3 months
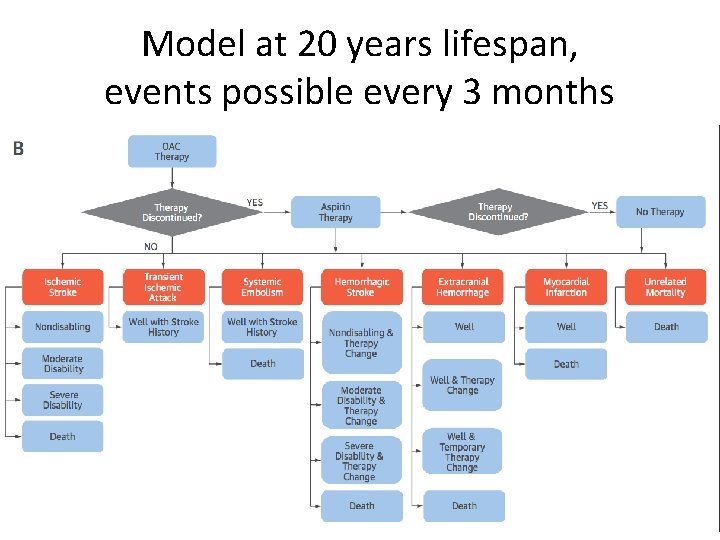
Model at 20 years lifespan, events possible every 3 months
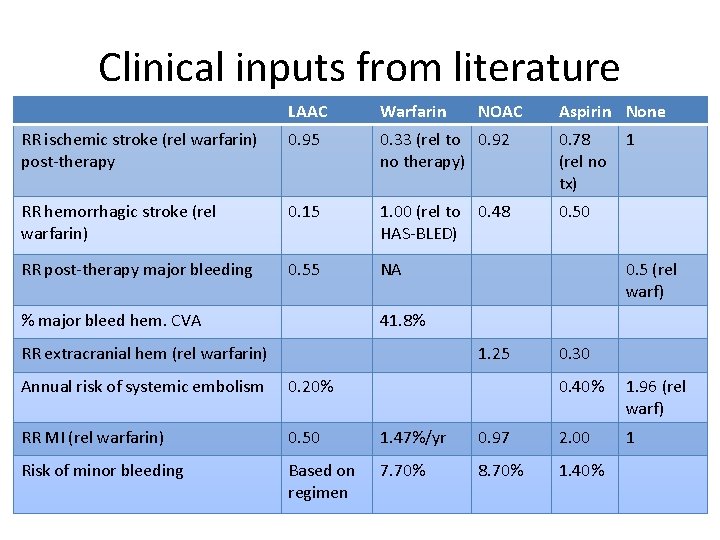
Clinical inputs from literature LAAC Warfarin RR ischemic stroke (rel warfarin) post-therapy 0. 95 0. 33 (rel to 0. 92 no therapy) 0. 78 (rel no tx) RR hemorrhagic stroke (rel warfarin) 0. 15 1. 00 (rel to HAS-BLED) 0. 50 RR post-therapy major bleeding 0. 55 NA % major bleed hem. CVA NOAC 0. 48 Aspirin None 1 0. 5 (rel warf) 41. 8% RR extracranial hem (rel warfarin) 1. 25 Annual risk of systemic embolism 0. 20% RR MI (rel warfarin) 0. 50 1. 47%/yr Risk of minor bleeding Based on regimen 7. 70% 0. 30 0. 40% 1. 96 (rel warf) 0. 97 2. 00 1 8. 70% 1. 40%
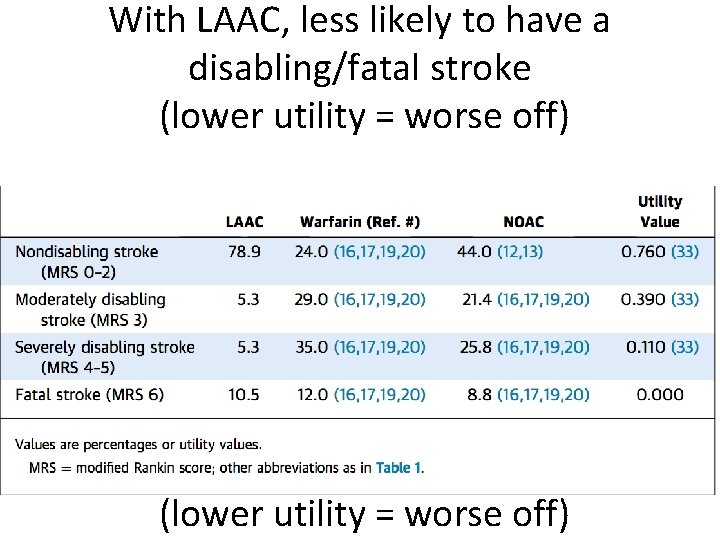
With LAAC, less likely to have a disabling/fatal stroke (lower utility = worse off)
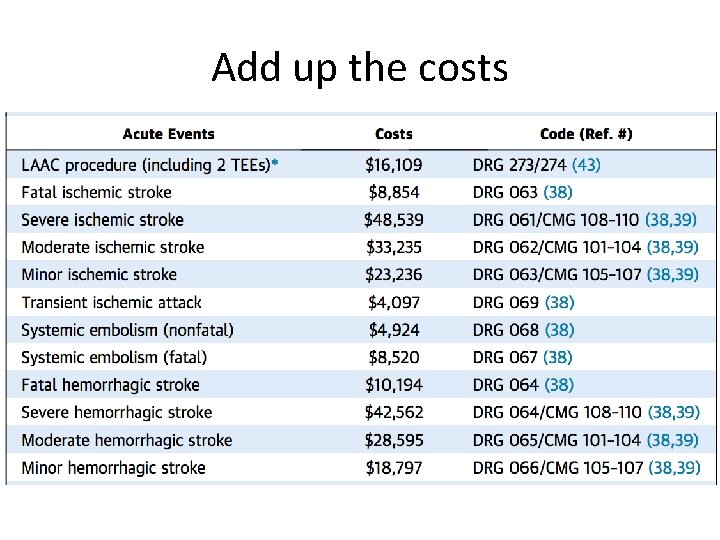
Add up the costs
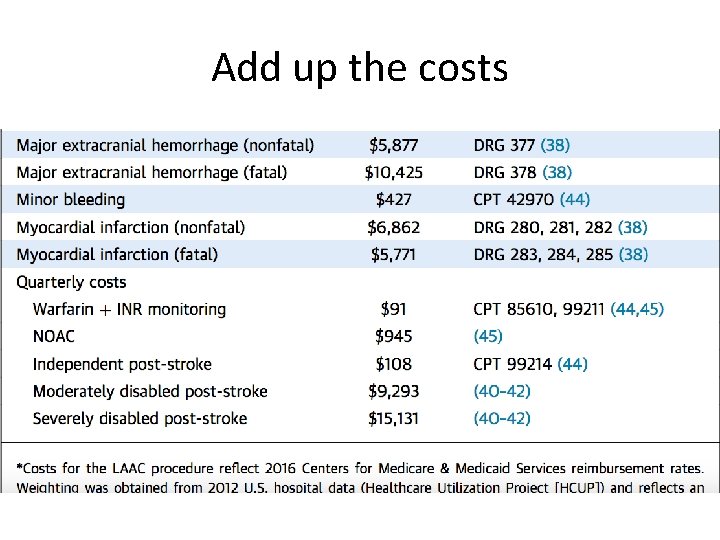
Add up the costs
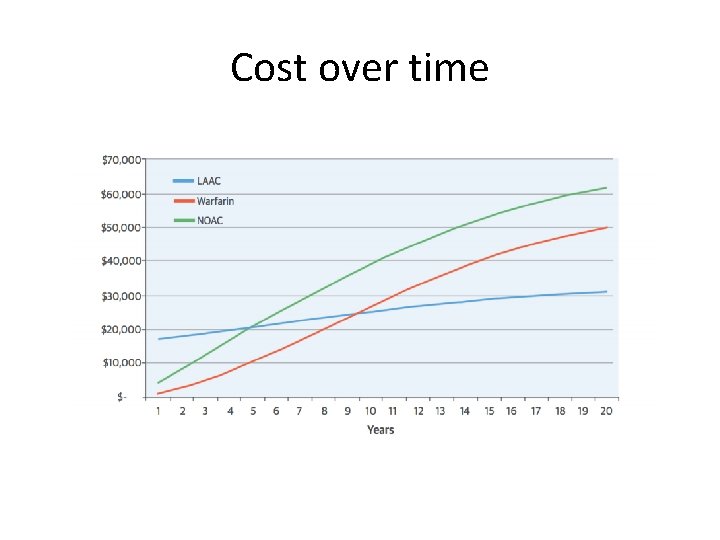
Cost over time
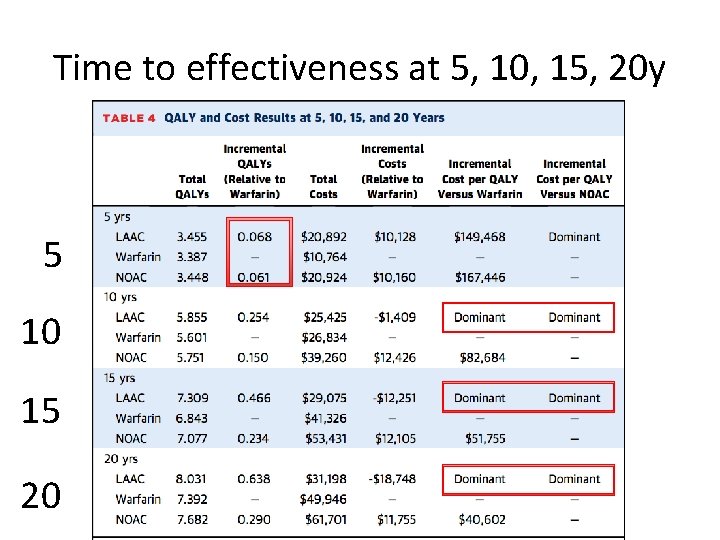
Time to effectiveness at 5, 10, 15, 20 y 5 10 15 20
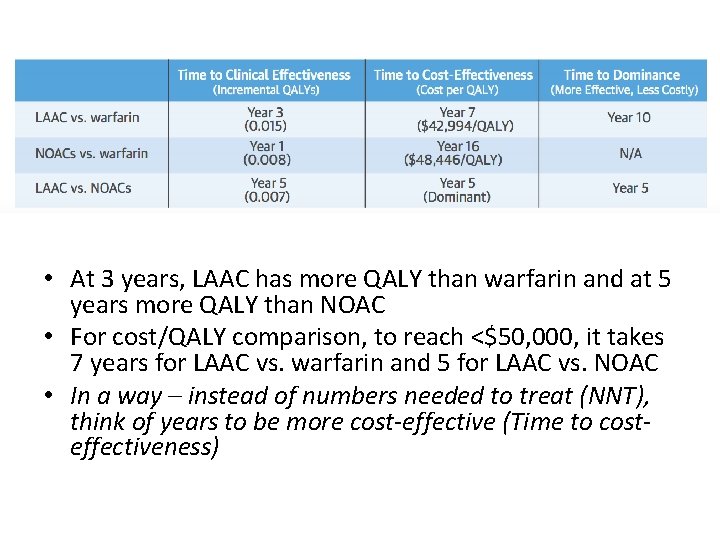
• At 3 years, LAAC has more QALY than warfarin and at 5 years more QALY than NOAC • For cost/QALY comparison, to reach <$50, 000, it takes 7 years for LAAC vs. warfarin and 5 for LAAC vs. NOAC • In a way – instead of numbers needed to treat (NNT), think of years to be more cost-effective (Time to costeffectiveness)
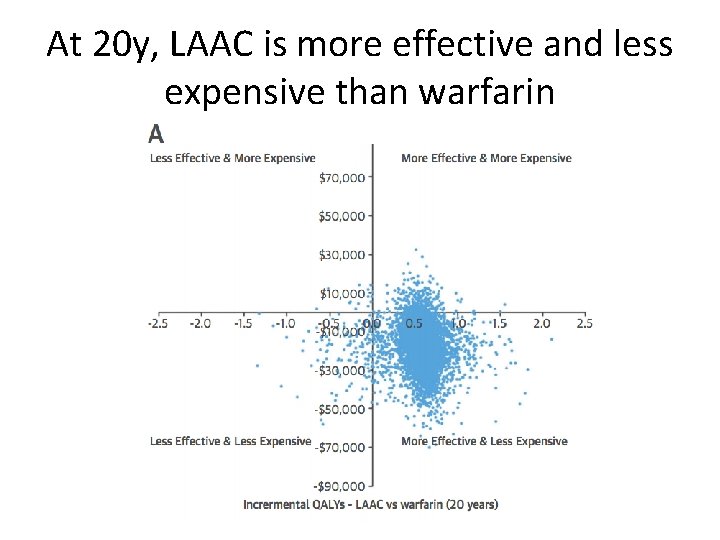
At 20 y, LAAC is more effective and less expensive than warfarin
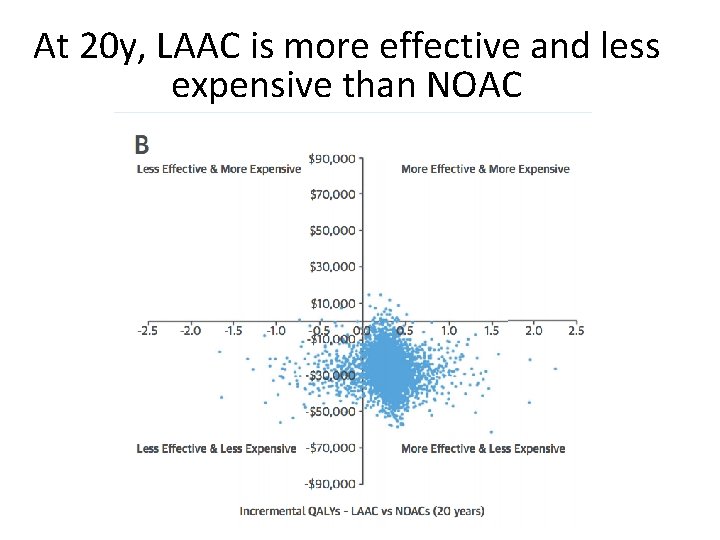
At 20 y, LAAC is more effective and less expensive than NOAC
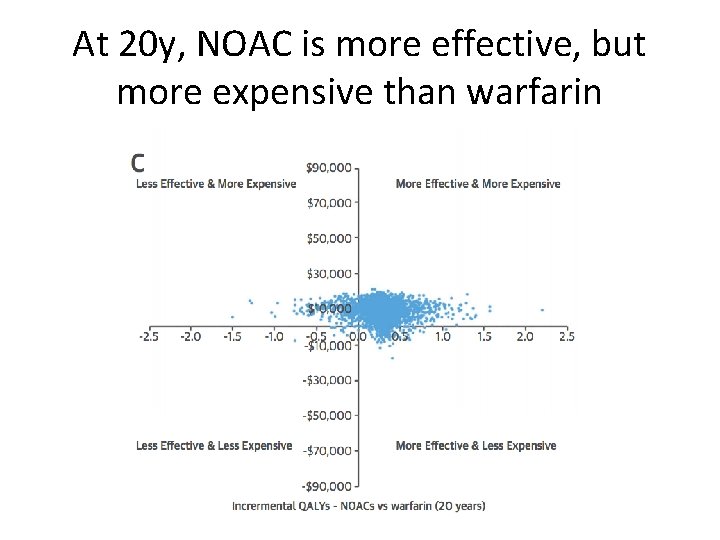
At 20 y, NOAC is more effective, but more expensive than warfarin • k

What did we learn • LAAC cost-effective to warfarin at 7 years; NOAC takes 16 years • LAAC had fewer disabling strokes • LAAC is more effective and less expensive • Adherence is an issue in NOAC

What about patients contraindicated for warfarin?

Methods • 3 studies – ASAP – watchman device – ACTIVEA – aspirin and clopidogrel – AVERROES – apixaban • CEA from German perspective 20 year time horizon
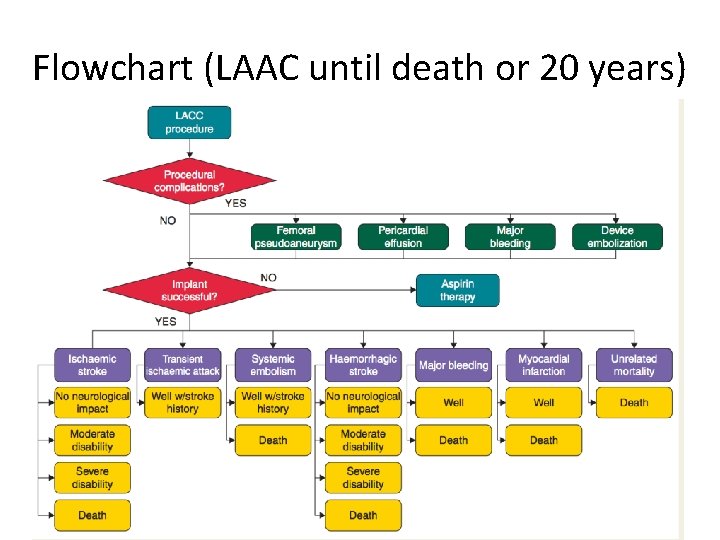
Flowchart (LAAC until death or 20 years)
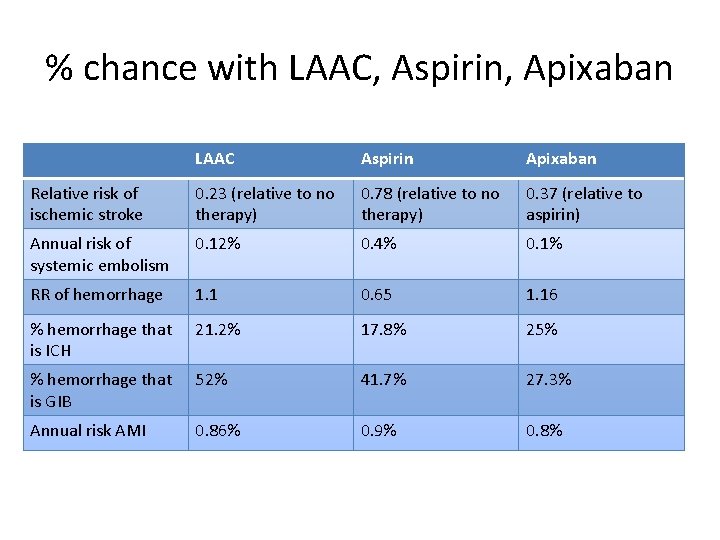
% chance with LAAC, Aspirin, Apixaban LAAC Aspirin Apixaban Relative risk of ischemic stroke 0. 23 (relative to no therapy) 0. 78 (relative to no therapy) 0. 37 (relative to aspirin) Annual risk of systemic embolism 0. 12% 0. 4% 0. 1% RR of hemorrhage 1. 1 0. 65 1. 16 % hemorrhage that is ICH 21. 2% 17. 8% 25% % hemorrhage that is GIB 52% 41. 7% 27. 3% Annual risk AMI 0. 86% 0. 9% 0. 8%
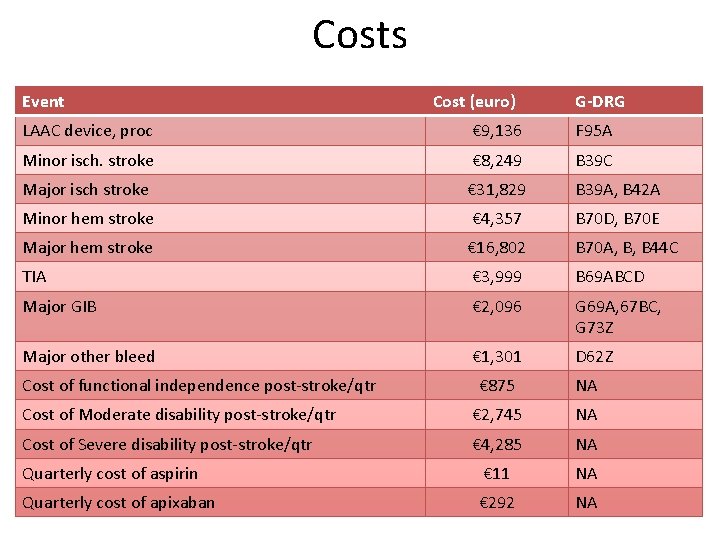
Costs Event Cost (euro) G-DRG LAAC device, proc € 9, 136 F 95 A Minor isch. stroke € 8, 249 B 39 C Major isch stroke € 31, 829 B 39 A, B 42 A Minor hem stroke € 4, 357 B 70 D, B 70 E Major hem stroke € 16, 802 B 70 A, B, B 44 C TIA € 3, 999 B 69 ABCD Major GIB € 2, 096 G 69 A, 67 BC, G 73 Z Major other bleed € 1, 301 D 62 Z Cost of functional independence post-stroke/qtr € 875 NA Cost of Moderate disability post-stroke/qtr € 2, 745 NA Cost of Severe disability post-stroke/qtr € 4, 285 NA Quarterly cost of aspirin € 11 NA Quarterly cost of apixaban € 292 NA
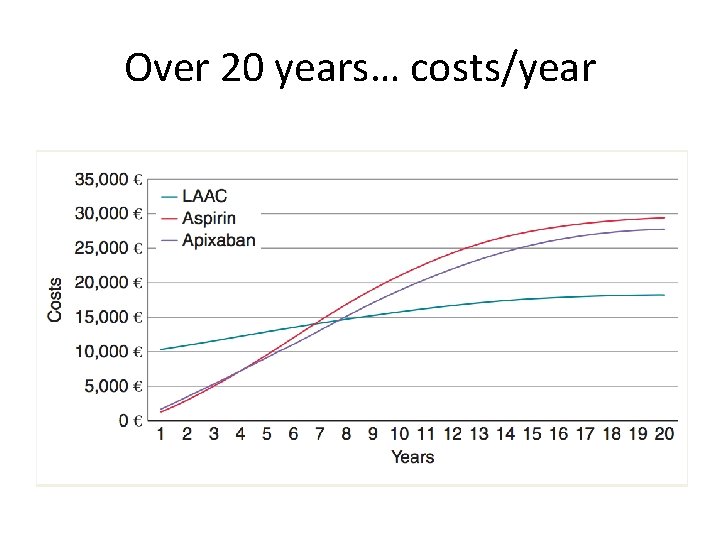
Over 20 years… costs/year

What happens with the ICER at 10 years? • Incremental Cost-effectiveness ratio • Baseline risk (8. 6% stroke risk) – LAAC € 15, 837 4. 82 QALY dominates over aspirin (€ 21, 077) or apixaban (€ 18, 869) alone • High risk patient (10. 9% stroke risk) – LAAC € 19, 236 4. 53 QALY dominates over aspirin (€ 29, 021) or apixaban (€ 25, 596) alone • Low risk patient (2. 2% stroke risk) – LAAC € 12, 529 5. 03 QALY ICER € 46 K-€ 51 K – Not so great, but this is the CHADS 2 <1 patient!
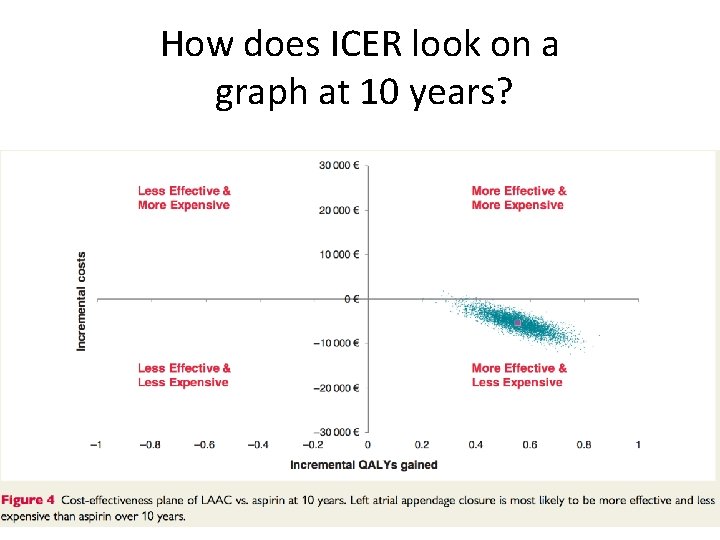
How does ICER look on a graph at 10 years?

What if we compare this to 2017 post-FDA event risk • LAAO Procedural risk – ischemic stroke 0. 05% – hemorrhagic stroke 0. 03% – major bleeding 0. 55% – effusion 1. 02% – Device embolization 0. 24% – Death 0. 10% • NOAC – Minor bleeding 8. 7% – Nonclinical discontinuation rates
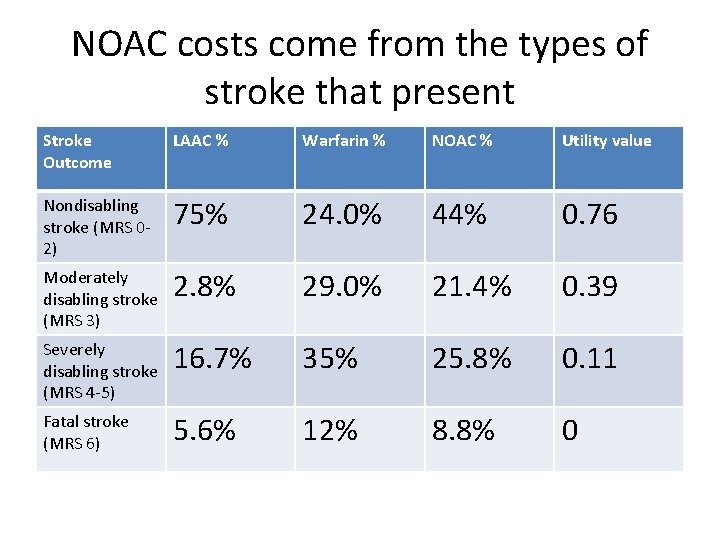
NOAC costs come from the types of stroke that present Stroke Outcome LAAC % Warfarin % NOAC % Utility value Nondisabling stroke (MRS 02) 75% 24. 0% 44% 0. 76 Moderately disabling stroke (MRS 3) 2. 8% 29. 0% 21. 4% 0. 39 Severely disabling stroke (MRS 4 -5) 16. 7% 35% 25. 8% 0. 11 Fatal stroke (MRS 6) 5. 6% 12% 8. 8% 0
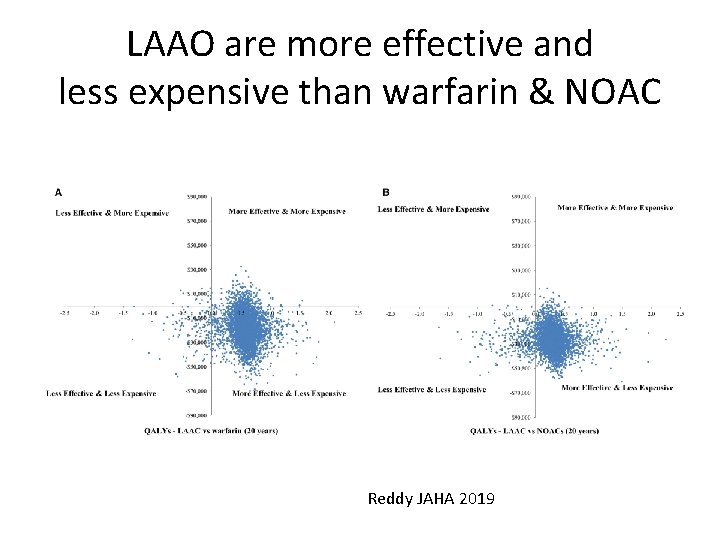
LAAO are more effective and less expensive than warfarin & NOAC Reddy JAHA 2019
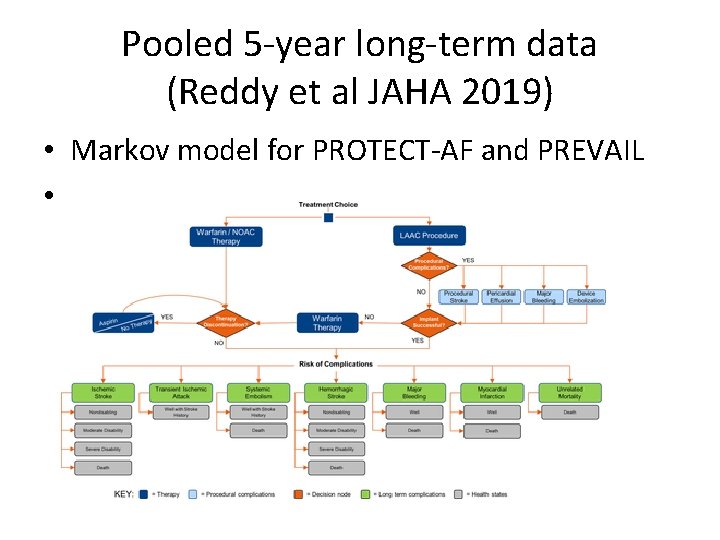
Pooled 5 -year long-term data (Reddy et al JAHA 2019) • Markov model for PROTECT-AF and PREVAIL •

Some US-based patient level data for 2020
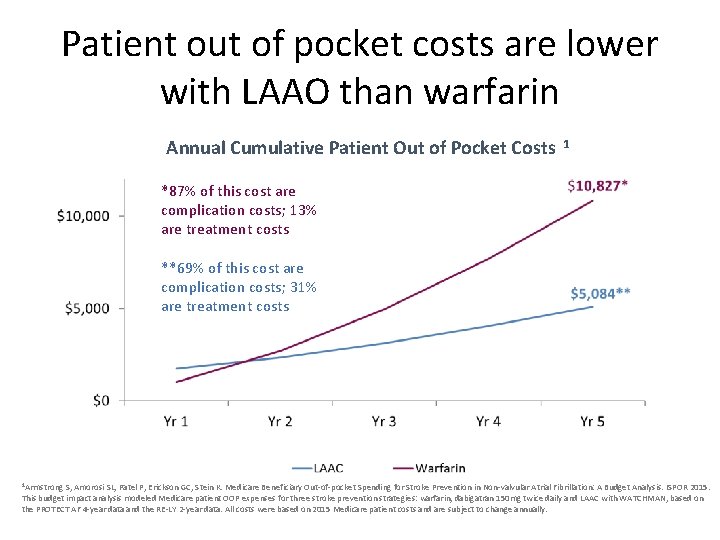
Patient out of pocket costs are lower with LAAO than warfarin Annual Cumulative Patient Out of Pocket Costs 1 *87% of this cost are complication costs; 13% are treatment costs **69% of this cost are complication costs; 31% are treatment costs 1 Armstrong S, Amorosi SL, Patel P, Erickson GC, Stein K. Medicare Beneficiary Out-of-pocket Spending for Stroke Prevention in Non-valvular Atrial Fibrillation: A Budget Analysis. ISPOR 2015. This budget impact analysis modeled Medicare patient OOP expenses for three stroke prevention strategies: warfarin, dabigatran 150 mg twice daily and LAAC with WATCHMAN, based on the PROTECT AF 4 -year data and the RE-LY 2 -year data. All costs were based on 2015 Medicare patient costs and are subject to change annually.
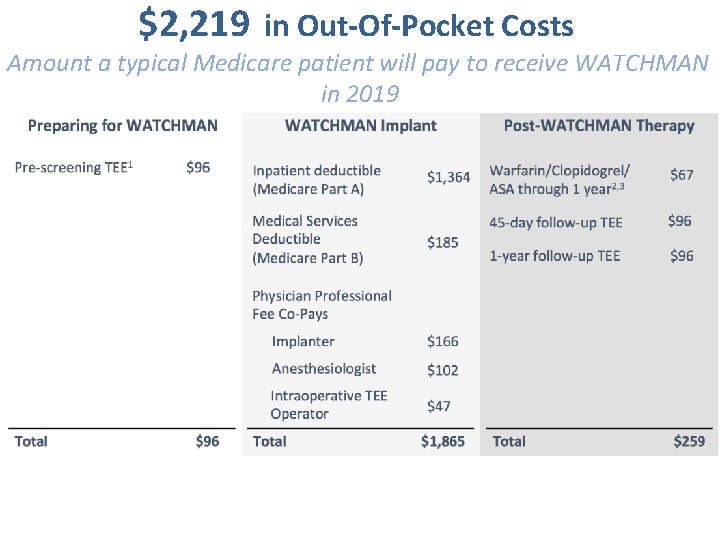

$2, 219 in Out-Of-Pocket Costs Amount a typical Medicare patient will pay to receive WATCHMAN in 2019

Future work • Cost-effectiveness incorporated in the decision-making tool • Use of this data in other countries and by US payors • Expansion of this to younger patients with longer lifespans – more likely to be costeffective
- Slides: 41