CRT 2013 Washington DC February 24 2013 Acute

CRT 2013 Washington, DC February 24, 2013 Acute Limb Ischemia: Medical and Endovascular Therapy Michael R. Jaff, DO Associate Professor of Medicine Harvard Medical School Medical Director Vascular Center Massachusetts General Hospital Boston, Massachusetts

• Michael R. Jaff, DO Consultant – Abbott Vascular (non-compensated) • – American Genomics, Inc – Becker Venture Services Group – Bluegrass Vascular Therapies – Cordis Corporation(non-compensated) – Covidien (non-compensated) – Ekos Corporation (DSMB) – Hansen Medical – Medtronic (non-compensated) – Micell, Incorporated – Primacea – Trivascular, Inc. • Equity – Access Closure, Inc – Embolitech, Inc – Hotspur, Inc – Icon Interventional, Inc – I. C. Sciences, Inc – Janacare, Inc – Northwind Medical, Inc. – PQ Bypass, Inc – Primacea – Sadra Medical – Sano V, Inc. – TMI/Trireme, Inc – Vascular Therapies, Inc Board Member – VIVA Physicians (Not For Profit 501(c) 3 Organization) • www. vivapvd. com

Acute Limb Ischemia Any sudden decrease in limb perfusion causing a potential threat to limb viability l True definition of a vascular emergency l Time is critical l n 6 hours to neurologic compromise n 12 -18 hours to non-salvagable limb TASC 2. J Vasc Surg 2007; 45 (Suppl): S 5 A-S 67 A

Embolic Etiology l 60 -70% from cardiac source n Previously n Currently from valvular disease from complications of ASHD (75%) –Especially anterior MI n. Atrial fibrillation

Site of Embolization 70% lower extremities l 10 -15% upper extremity l 10% visceral l 10 -20% cerebral l

Acute arterial occlusion Other causes: Artery-to-artery embolization AAA – ‘Blue toe syndrome’ Popliteal aneurysm Atheromatous embolization Lower extremities Cerebral Paradoxical embolization
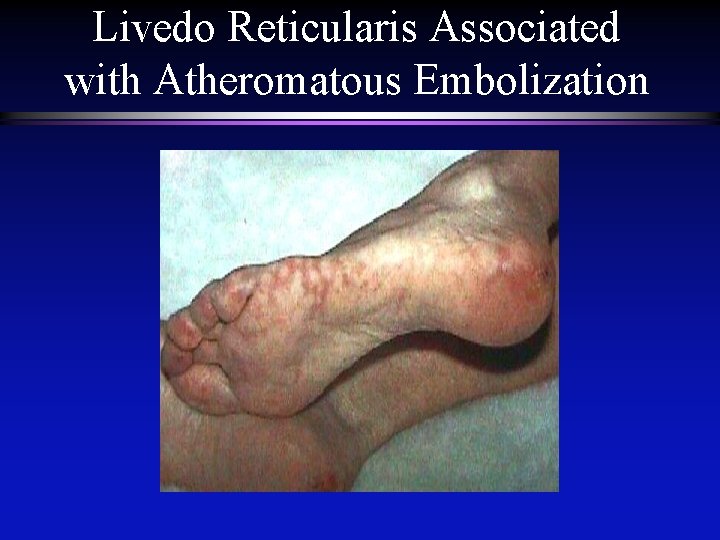
Livedo Reticularis Associated with Atheromatous Embolization

Acute arterial occlusion l Thrombotic arterial occlusion --Thrombosis of pre-existing atherosclerotic stenosis --Graft thrombosis --Hypercoagulable states --Trauma --Aortic dissection --Iatrogenic (catheterization) --Phlegmasia Cerulea Dolenx --Low-flow states
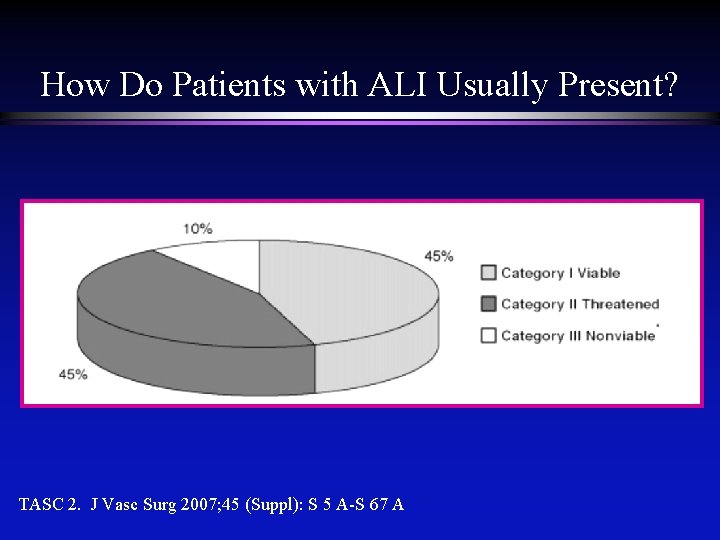
How Do Patients with ALI Usually Present? TASC 2. J Vasc Surg 2007; 45 (Suppl): S 5 A-S 67 A

Clinical Presentation l Pain l Pallor l Parasthesias l Pulselessness l Paralysis l Poikilothermia The 6 “P’s”

Clinical Characteristics Characteristic Embolus Thrombosis Onset of sx Rapid/immediate Slower/insidious Prior sx Infrequent Frequent Duration of sx before presentation Short Longer Opposite leg Normal Abnormal Heart disease (Afib, MI) Frequent =/- Goal of immediate Rx Eliminate embolus Correct underlying dz Pharmacologic Rx Anticoagulation Platelet inhibition Results of embolectomy Good Poor Amputation risk Lower Higher

Management l Identification l Intravenous of etiology Heparin l Arteriography +/-
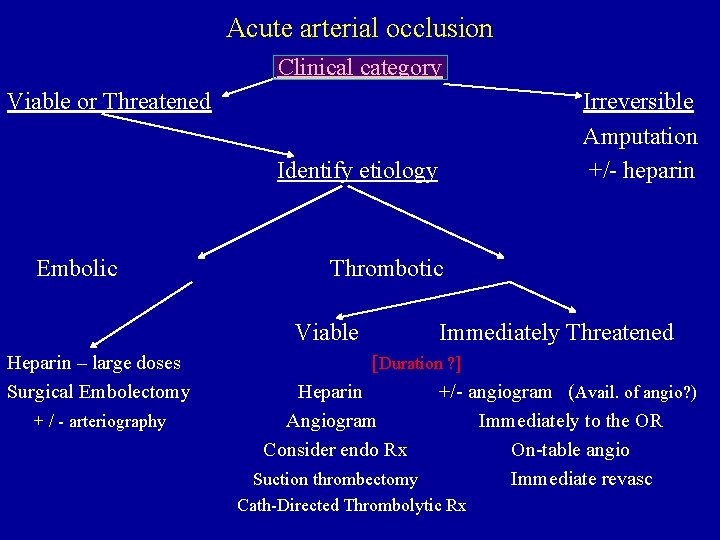
Acute arterial occlusion Clinical category Viable or Threatened Irreversible Amputation +/- heparin Identify etiology Embolic Thrombotic Viable Heparin – large doses Surgical Embolectomy + / - arteriography Immediately Threatened [Duration ? ] Heparin +/- angiogram (Avail. of angio? ) Angiogram Immediately to the OR Consider endo Rx On-table angio Suction thrombectomy Immediate revasc Cath-Directed Thrombolytic Rx

Surgical Revascularization l l Embolectomy n Lower extremity n Upper extremity Fogarty catheter n 1963 l Bypass
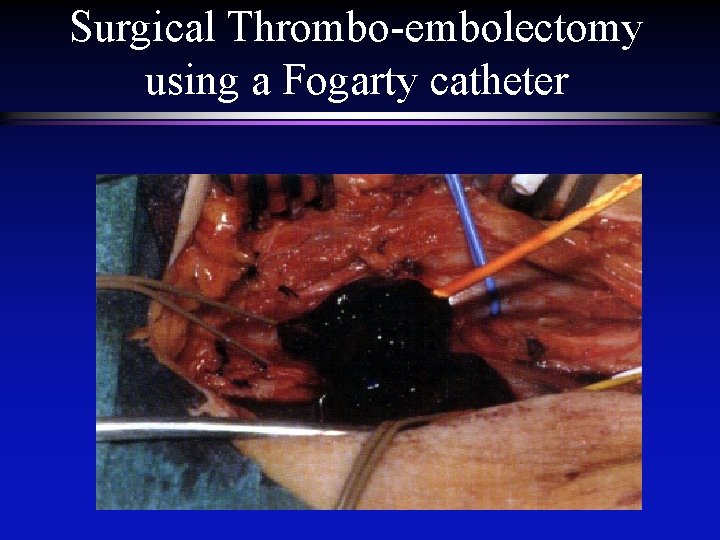
Surgical Thrombo-embolectomy using a Fogarty catheter

Endovascular l Catheter-directed thrombolysis l Catheter-directed thrombectomy l PTA/stent
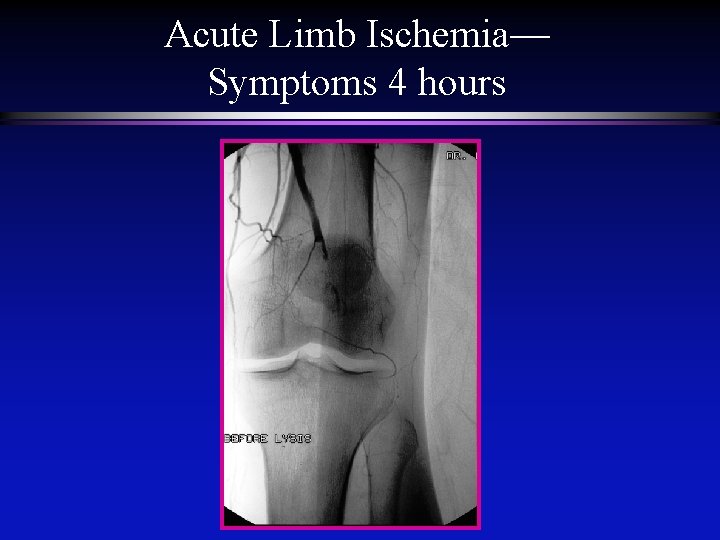
Acute Limb Ischemia— Symptoms 4 hours

Surgery vs CDT TASC 2. J Vasc Surg 2007; 45 (Suppl): S 5 A-S 67 A

Thrombolysis vs. Surgery-Randomized Trials in PAD Duration of Ischemic Limb Symptoms l Rochester n Mean 40 hours (but 50% of patients with symptoms < 24 hours) l STILE n Mean l 50 days TOPAS n Mean 4 days
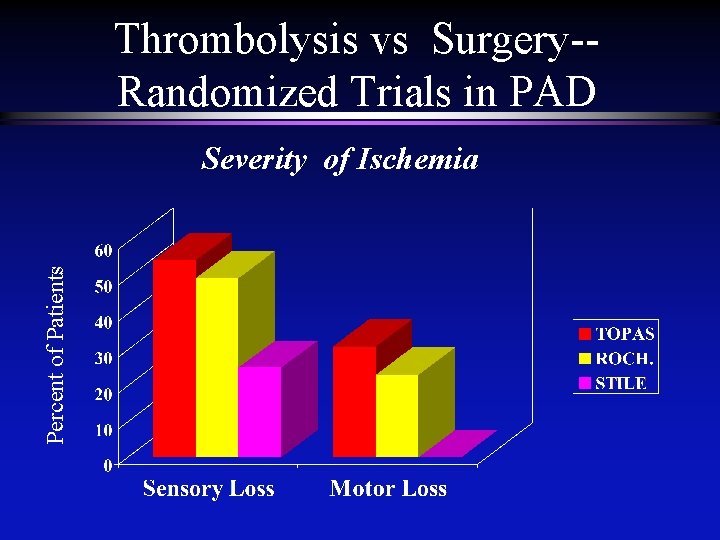
Thrombolysis vs Surgery-Randomized Trials in PAD Percent of Patients Severity of Ischemia

Thrombolysis vs Surgery-Randomized Trials in PAD Limb Salvage Rates l l Symptom Onset <24 hours, SEVERE n Amputation rates low with either thrombolysis or surgery (ROCH) Symptom Onset 24 hr-14 days, MODERATE n Amputation rates low with either thrombolysis or surgery – ? Lower amputation rates with thrombolysis (STILE) l Symptom Onset >14 days, MILD-MODERATE n Amputation rates HIGHER with thrombolysis (STILE)
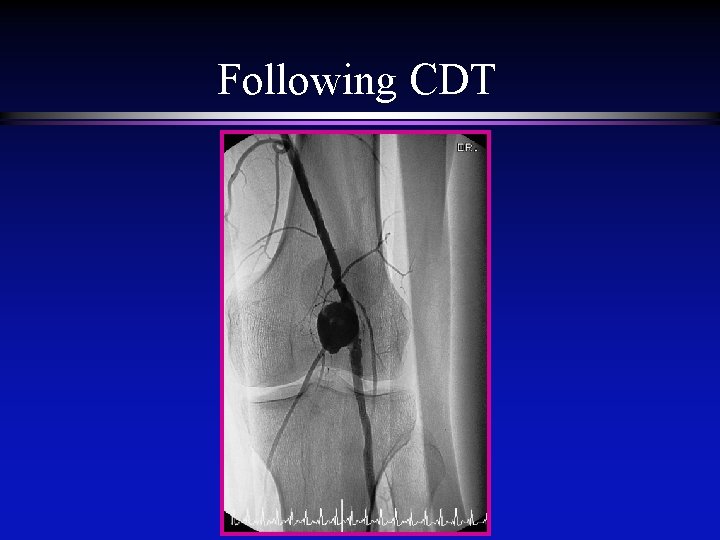
Following CDT

80 year old female s/p right total knee replacement 7 weeks ago presents with a 4 day history of severe right leg pain and swelling • PMH: – Polymyalgia rheumatica – Raynaud’s disease – Hypertension – OA of bilateral knees, s/p knee replacement – Left S 1 radiculopathy in the past treated with epidural injections – 24 Pack year h/o tobacco use • Patient reports that she called orthopaedic surgeon 2 days after pain onset; MRI of back was obtained and patient was given a Medrol dosepack

80 year old female s/p right total knee replacement 7 weeks ago presents with a 4 day history of severe right leg pain and swelling • Physical Exam: – + Marked cyanosis of the right foot with dramatic coolness of the distal right calf, ankle and foot. – + Tenderness of the right calf tibialis anterior muscle group – + Weakness of the dorsiflexors of the right foot and toes. – Absence of LT on the dorsum of the right foot – Absent right popliteal, DP, PT pulses. – Doppler with absent right DP, PT arterial signal. • Preserved venous Doppler signal • Labs: CK-2229 Cr- 1. 3
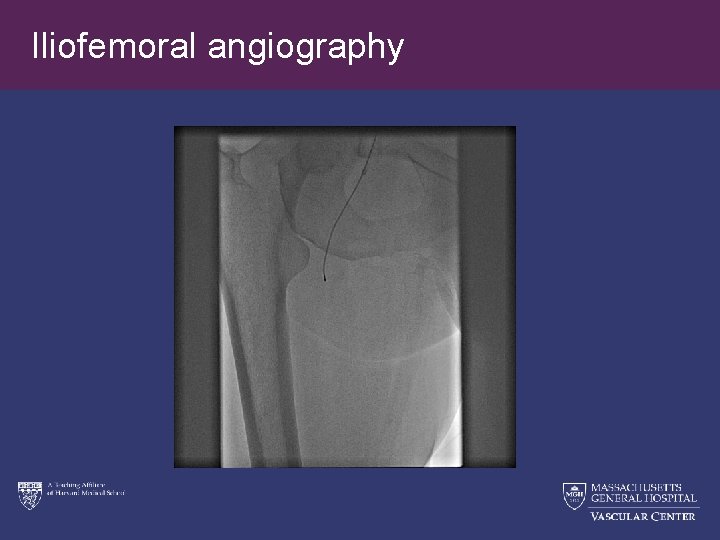
Iliofemoral angiography
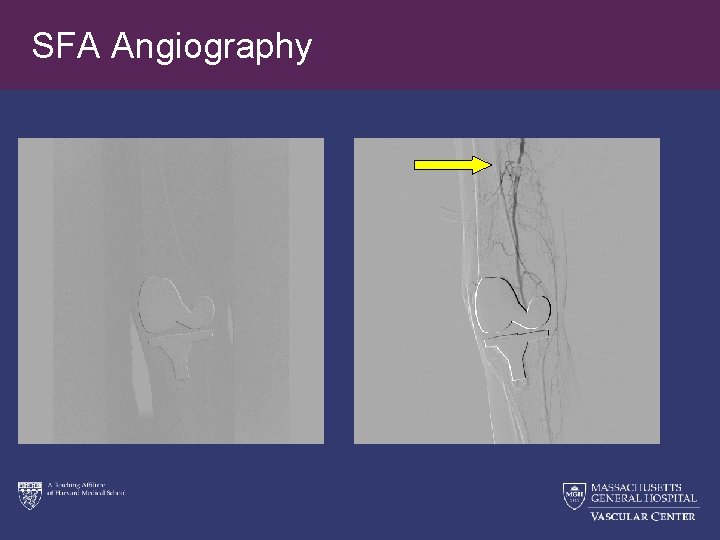
SFA Angiography
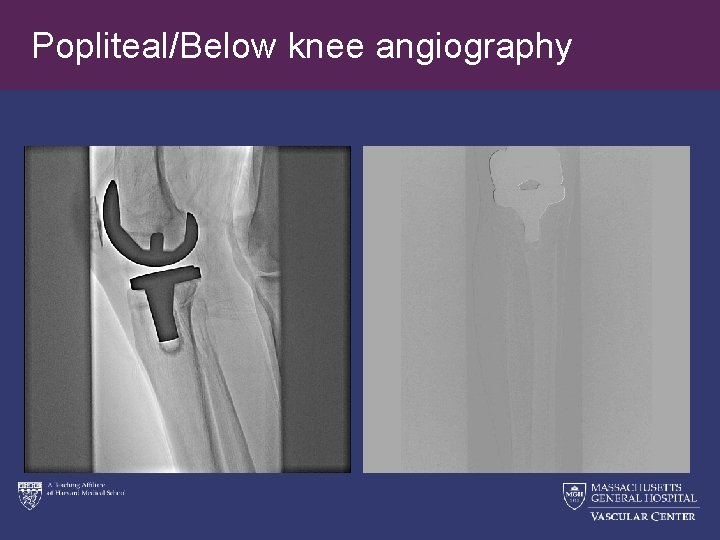
Popliteal/Below knee angiography
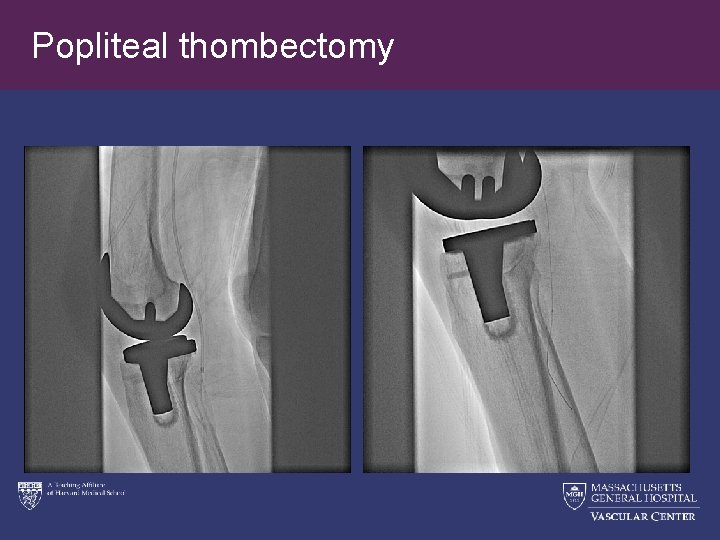
Popliteal thombectomy

Residual thrombus below knee
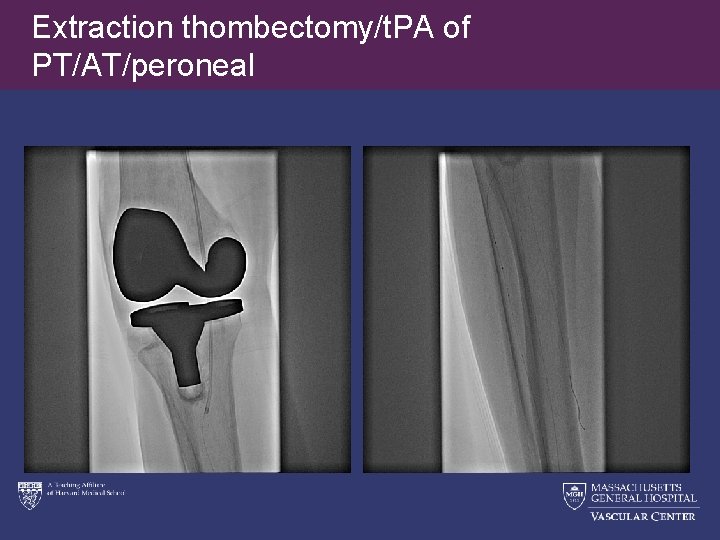
Extraction thombectomy/t. PA of PT/AT/peroneal
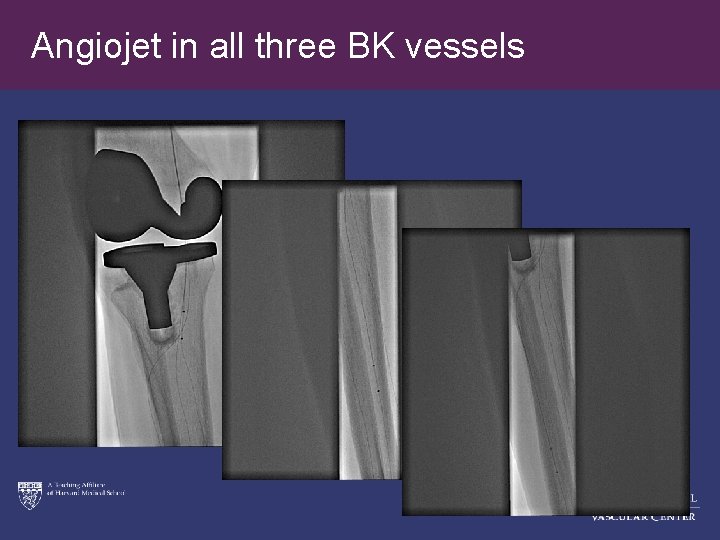
Angiojet in all three BK vessels
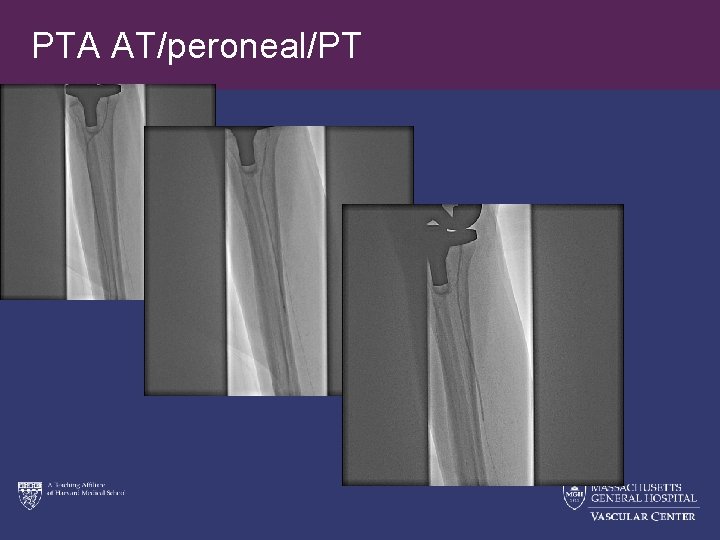
PTA AT/peroneal/PT
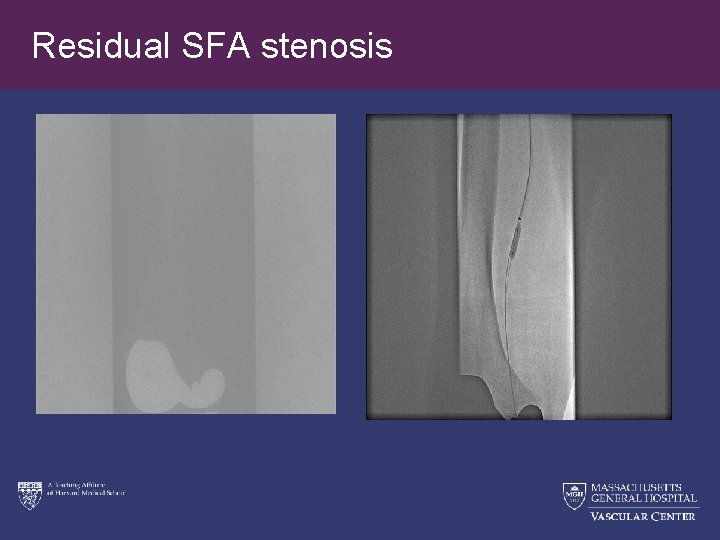
Residual SFA stenosis
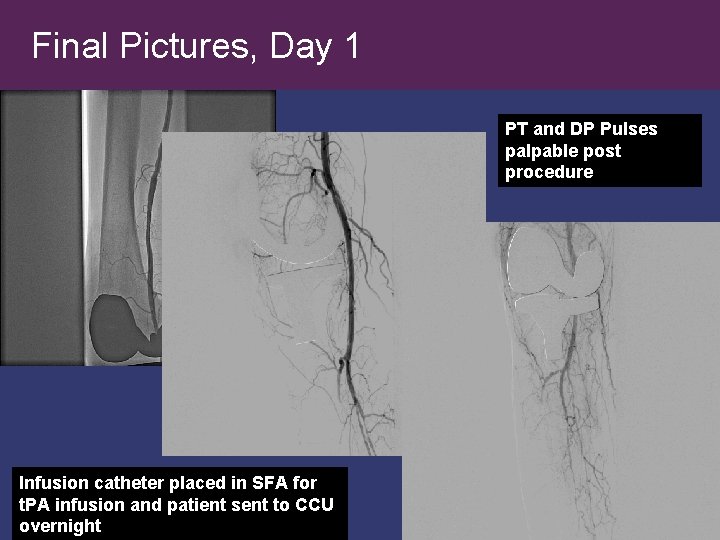
Final Pictures, Day 1 PT and DP Pulses palpable post procedure Infusion catheter placed in SFA for t. PA infusion and patient sent to CCU overnight
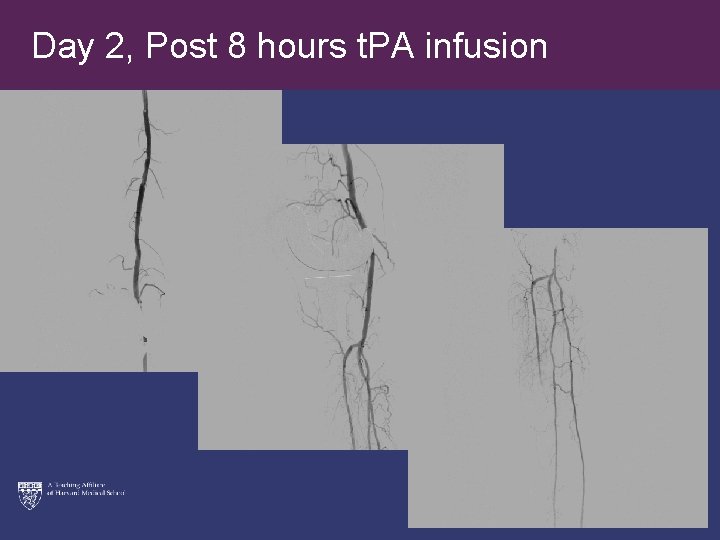
Day 2, Post 8 hours t. PA infusion
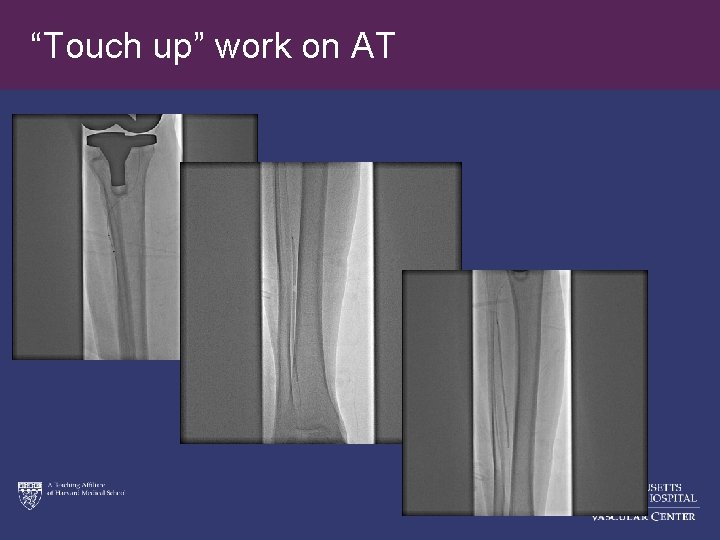
“Touch up” work on AT

Final Angiographic Result

Final Angiographic Result

45 minutes post procedure… • Patient develops intractable pain in right leg • Pulses in DP/ PT preserved • Anterior compartment with tenderness to palpation, decrease in sensation to sharp and light touch between the first and second toes • Stryker Pressure (anterior compartment): 11 and 13 • Despite borderline anterior compartment pressures, clinical suspicion prompted transfer to OR for four compartment fasciotomy
Follow up • Post op, patient wound vac placed; in hospital closure of the posterior compartment; anterior compartment to heal by secondary intention • Warfarin/heparin during hospitalization; complicated by GI bleeding (single gastric angiodysplastic lesion which was cauterized) • Patient discharged to rehab facility on ASA and Plavix; will have follow up Ig. M anticardiolipin Ab (mildly positive) in 4 months

Acute Limb Ischemia l Prompt recognition is key n Time is of the essence Rapid administration of IV heparin l Lysis vs Surgical Thrombectomy l Treatment of culprit lesion/etiology l Mechanical Thrombectomy may emerge as useful tool l
- Slides: 41