Crossing SFA CTO with a Wire William Bachinsky

Crossing SFA CTO with a Wire William Bachinsky MD, FACC, FSCAI Pinnacle Health Cardiovascular Institute Medical Director, Vascular Services Medical Director, Cardiac Catheterization Labs Harrisburg, PA

William Bachinsky MD, FACC, FSCAI Disclosures Medical Advisory Board: Abbott Vascular Consultant: Cordis, Abbott Vascular, Morris Innovative Research grants, Clinical trials: Abbott Vascular, Medtronic, Cordis, Rex. Medical

Improved Outcomes in Lower Extremity Endovascular Interventions Ann Vasc Surg 2011; 25: 44 -55

CTO Landscape & Technology • CTOs are present in ~40% of patients treated for symptomatic peripheral artery disease 1 • Historical data suggests 30 -40% of CTOs require adjunctive CTO device technology for crossing lesions 2 • Today, with better understanding of wires and CTO techniques, the majority of cases can be performed without expensive re-entry devices 1 A. Boguszewski, et al, Endovascular Today, May 2010, 33 -8. 2 2010 -2011 Global PI Tracking Study; US physicians; N= 70. 3 True lumen re-entry devices facilitate subintimal angioplasty and stenting of CTOs – Jacobs, D, et al, Journal of Vasc Surgery, Jun 2006. 4 PI MAB 2011 Feedback.

Microchannels Formation in CTOs J Am Coll Cardiol Img. 2010; 3(8): 797 -805. doi: 10. 1016/j. jcmg. 2010. 03. 013

CTO Access: 3 Options for Crossing (in order preference) The Front Door (Antegrade Approach) The Back Door (Retrograde Approach) The Side Door (Sub-Intimal and Collateral Approach) Slide provide by Boston Scientific, image by Stephen B. Williams, MD.

Challenges in Treating LE CTOs • Crossing of peripheral CTO is the most common reason for: – Failed intervention (13 – 34%) – Complications (~15%) • Crossing CTOs hurdles: – Penetration of proximal cap – Navigate collaterals and side-branches – Long segment/multi-level occlusions – Overcoming wire maneuverability issues – Entry into distal target vessel Jacobs et al. J Vasc. Surg. 2006; 43(6): 1291

Factors affecting guidewire selection • The Basics: – Wire length – Device compatibility – Wire diameter – Cost • Key wire elements important in CTO lesions 1. Core (Shaft) Functional Diameter (0. 014”/0. 018”/0. 035”) Core Diameter Core Material Core Taper/Grind 2. Tip Coatings Coils & Covers Tip Style 3. Covers and Coatings
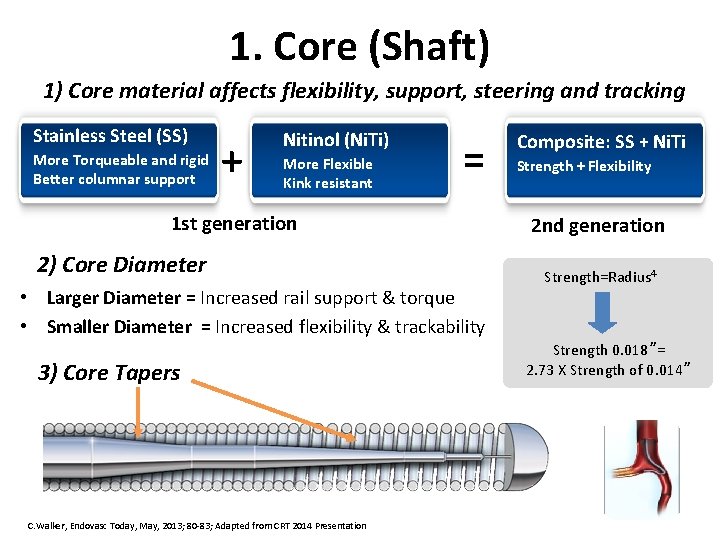
1. Core (Shaft) 1) Core material affects flexibility, support, steering and tracking Stainless Steel (SS) More Torqueable and rigid Better columnar support + Nitinol (Ni. Ti) More Flexible Kink resistant = 1 st generation 2) Core Diameter • Larger Diameter = Increased rail support & torque • Smaller Diameter = Increased flexibility & trackability 3) Core Tapers C. Walker, Endovasc Today, May, 2013; 80 -83; Adapted from CRT 2014 Presentation Composite: SS + Ni. Ti Strength + Flexibility 2 nd generation Strength=Radius 4 Strength 0. 018”= 2. 73 X Strength of 0. 014”
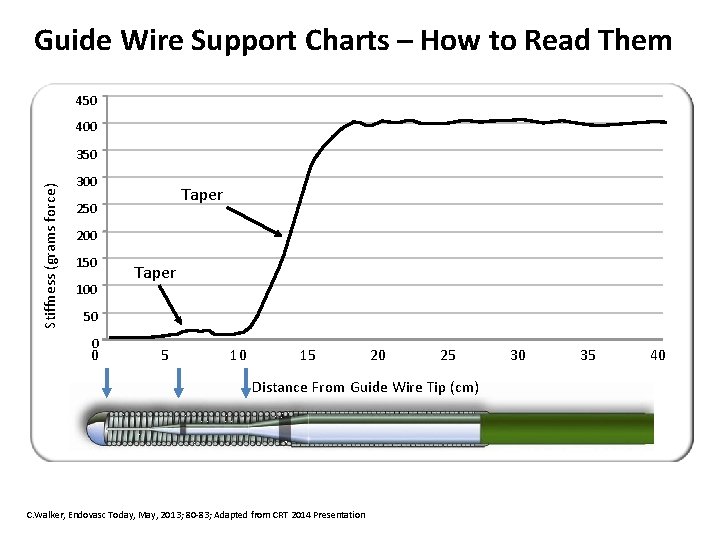
Guide Wire Support Charts – How to Read Them 450 400 Stiffness (grams force) 350 300 Taper 250 200 150 100 Taper 50 0 0 5 10 15 20 25 Distance From Guide Wire Tip (cm) C. Walker, Endovasc Today, May, 2013; 80 -83; Adapted from CRT 2014 Presentation 30 35 40

2. Guide Wire Tip The guide wire tip configuration determines steering and durability Design Options ü Force transmission ü Better steerability ü Tactile feedback ü Easy tip shapeability ü Flexibility, softness ü Ability to prolapse ü More durable ü Ideal for peripheral vessels ü More delicate Adapted from C. Walker, Endovasc Today, May, 2013; 80 -83; Adapted from CRT 2014 Presentation Core-to-tip Shaping Ribbon

Guide Wire Tip: Penetration Power Tip Stiffness = 4. 0 g Tip Diameter 0. 012” Area of Guide Wire Tip r Penetration Power: (Pressure) Tip Stiffness / Area of Guide Wire Tip: . 004 kg/(3. 14*. 006” 2) Penetration Power = 40 Kg/in 2 Guide Wire Tip C. Walker, Endovasc Today, May, 2013; 80 -83; Adapted from CRT 2014 Presentation
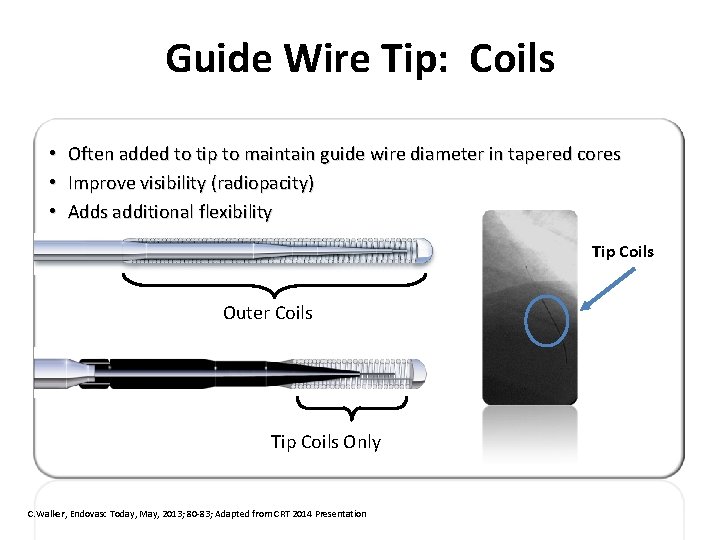
Guide Wire Tip: Coils • • Often added to tip to maintain guide wire diameter in tapered cores Improve visibility (radiopacity) Adds additional flexibility Affect tactile feedback Tip Coils Outer Coils Tip Coils Only C. Walker, Endovasc Today, May, 2013; 80 -83; Adapted from CRT 2014 Presentation
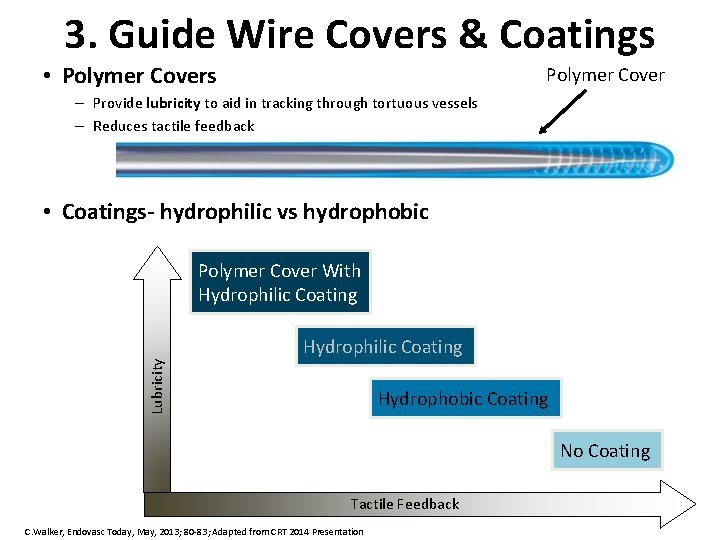
3. Guide Wire Covers & Coatings • Polymer Covers Polymer Cover – Provide lubricity to aid in tracking through tortuous vessels – Reduces tactile feedback • Coatings- hydrophilic vs hydrophobic Polymer Cover With Hydrophilic Coating Lubricity Hydrophilic Coating Hydrophobic Coating No Coating Tactile Feedback C. Walker, Endovasc Today, May, 2013; 80 -83; Adapted from CRT 2014 Presentation

2 nd Generation Guidewires Hi-Torque Command TM 0. 014 “ and Connect TM 0. 018 “ (Abbott Vascular) Transitionless nitinol to stainless steel core 3 cm radiopaque coils Polymer jacket for lubricity Turbocoat. TM hydrophilic coating kink resistant shapeable nitinol tip Available in extra support and 30 G tip load Journey™ Wire 0. 014 “ (Boston Scientific) unique micro-cut nitinol hypotube with stainless steel core Adapted from slide provided by Abbottt Vascular and Boston Scientific Flat Portio hybrid hydrophilic coating with 1. 27 cm uncoated distal tip

Methods for Crossing SFA CTOs Subintimal- Percutaneous intentional extraluminal recanalization (PIER) – Intentional dissection plane through occlusion and re-entered into true lumen distally • Advantages – May use in simultaneous antegrade/retrograde – Creates of a smooth neo-lumen – Useful in short occlusions- quick procedure time • Disadvantages – – 10% - 20% failure rate Propagation of dissection distally lengthening treatment area Loss of collaterals from intentional dissection May limit use/benefit of adjunctive therapies atherectomy and DCB

Methods for Crossing SFA CTOs Intra(true)-Luminal Approach – Controlled wiring in an effort to remain in the true lumen – Use of CTO-designed wires to penetrate caps and remain in micro-channels • Advantages – Reduce costs by avoiding use of re-entry devices – May decrease need for stenting in “no stent zone” lesions and reduce overall lesion treatment length – More suitable for use of adjunctive therapies such as atherectomy and DCB where intraluminal treatment advantageous • Disadvantages – May increase procedural times especially in distal cap crossing or same sitting retrograde access approach (pedal) – Require increase operator “skill set” wire knowledge and techniques
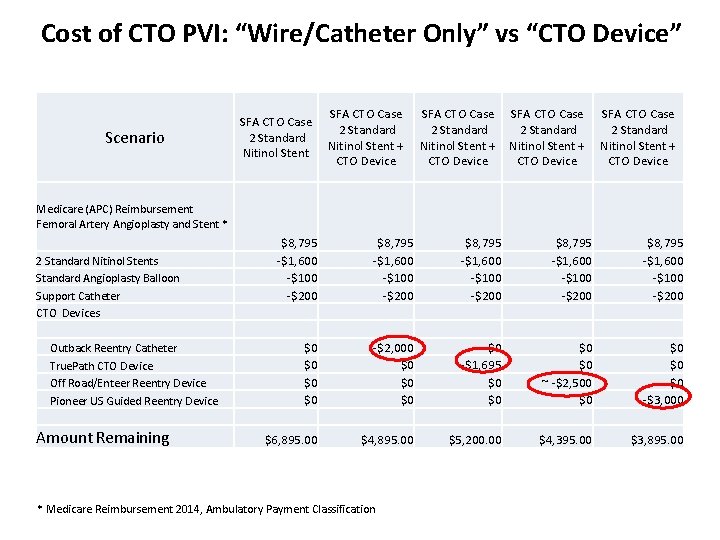
Cost of CTO PVI: “Wire/Catheter Only” vs “CTO Device” SFA CTO Case 2 Standard Nitinol Stent + CTO Device SFA CTO Case 2 Standard Nitinol Stent Scenario SFA CTO Case 2 Standard Nitinol Stent + CTO Device Medicare (APC) Reimbursement Femoral Artery Angioplasty and Stent * 2 Standard Nitinol Stents Standard Angioplasty Balloon Support Catheter CTO Devices Outback Reentry Catheter True. Path CTO Device Off Road/Enteer Reentry Device Pioneer US Guided Reentry Device Amount Remaining $8, 795 -$1, 600 -$100 -$200 $0 $0 -$2, 000 $0 $6, 895. 00 $8, 795 -$1, 600 -$100 -$200 $0 -$1, 695 $0 $0 $4, 895. 00 * Medicare Reimbursement 2014, Ambulatory Payment Classification $8, 795 -$1, 600 -$100 -$200 $0 $0 ~ -$2, 500 $0 $5, 200. 00 $8, 795 -$1, 600 -$100 -$200 $0 $0 $0 -$3, 000 $4, 395. 00 $3, 895. 00

Summary and Conclusions • With appropriate wire selection and technique, the majority of SFA CTOs can be crossed without the use of re-entry devices. • “Intraluminal first” approach is preferential in SFA CTO cases to limit treatment area and allow for adjunctive therapies. • We need to be cognizant of the cost/benefit of a successful SFA CTO case in the our current economic health care climate.
THANK YOU
- Slides: 20