Crohns disease and Pouches Bruce George Oxford Kangaroo

Crohn’s disease and Pouches Bruce George Oxford Kangaroo Club 31 -5 -14 Colorectal

Crohn’s disease and Pouches Why is this a question? • Pre-pouch surgery – Crohn’s disease is a contra-indication to pouch surgery – What about indeterminate colitis? – Is it ever reasonable to make a pouch for known Crohn’s? • Post pouch surgery – If pouch function is poor/complication, could this be due to Crohn’s – What happens if you develop Crohn’s in a pouch? Oxford Colorectal
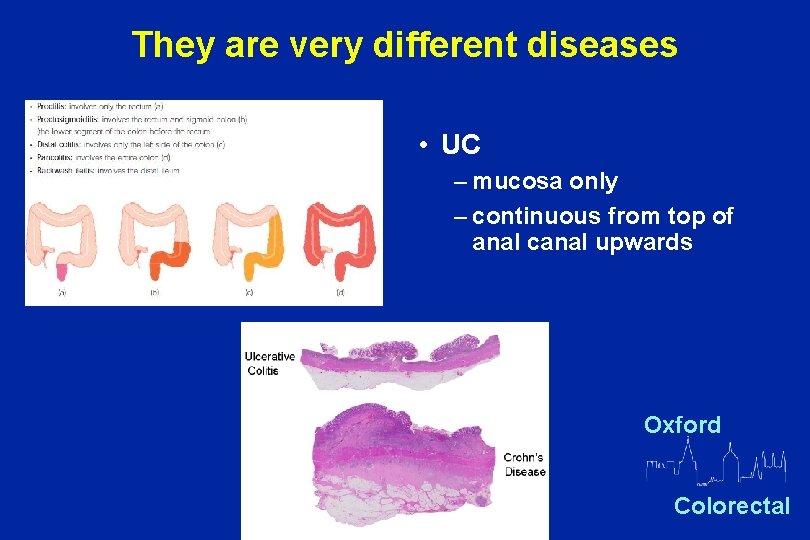
They are very different diseases • UC – mucosa only – continuous from top of anal canal upwards Oxford Colorectal

• If you don’t want to see pictures of bowels and bottoms: – Look away now!! Oxford Colorectal
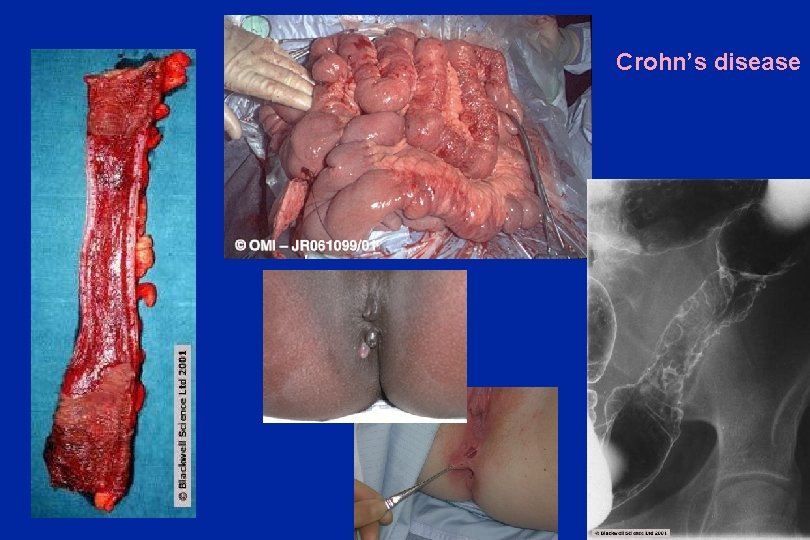
Crohn’s disease Oxford Colorectal

The problem • Pouch surgery for Crohn’s disease highly likely to fail – Small bowel and anal disease – Deep inflammation: fistulae, leaks, strictures • But sometimes Crohn’s can mimic UC – Isolated to colon – Similar histology Oxford Colorectal

Pre-pouch work-up • Review pathology available • Review distribution of disease – skip lesions – small bowel pathology – anal pathology • Indeterminate • UC, but minor features of CD • Effects of therapy • patchy • Ordinary anal pathology • piles • tears Oxford Colorectal

Cleveland Clinic • Over 3000 pouches • 204 for Crohn’s – 20 intentional – 97 immediate diagnosis on colon pathology – 87 delayed diagnosis • Outcome – 29% failure rate at 10 years (71% functioning) – Delayed group worse Metton et al 2008 Oxford Colorectal

Policy in Oxford • Not to offer pouch surgery for known Crohn’s disease • Minimise surprise finding of Crohn’s disease on proctocolectomy specimen • Review of all available pathology • Colectomy first approach • Slow lane for indeterminate • Increased risks • Delay in case features of Crohn’s develop Oxford Colorectal

Pouches behaving badly • What is normal? • Acute deterioration usually called pouchitis and treated with ciprofloxacin or metronidazole Oxford Colorectal

Pouchitis Histology Symptoms increased stool frequency looseness blood urgency incontinence abdominal pain fever arthralgia acute inflammation + chronic inflammation villous atrophy crypt hyperplasia chronic inflammatory infiltrate Endoscopy oedema granularity contact bleeding loss of vascularity haemorrhage ulceration Oxford Colorectal

Treatment • Cochrane meta-analysis of 11 RCTs • Acute pouchitis (4 RCT, 5 agents) Oxford Rifaximin and lactobacillus GG not significantly different to placebo Budesonide enemas = metronidazole Colorectal

Cochrane meta-analysis • Chronic pouchitis (4 RCT, 4 agents) • VSL 3 better than placebo in maintaining remission after treatment with antibiotics Oxford Colorectal

It’s probably not that simple • Many other causes of poor pouch function – many of which may respond to antibiotics – many patients fulfilling definition of pouchitis may have poor pouch function due to other causes Oxford Colorectal

Assessment of pouch dysfunction • Identification of – True pouchitis – Other causes of pouch inflammation (secondary) • Pathogens (C diff, cmv) • Adjacent inflammation (sepsis, ischaemia, intussusception) • Drugs (NSAIDS) Oxford • Crohn’s disease – Other causes of poor pouch function Colorectal

Phase 1 assessment of poor pouch function • History of poor function – Always bad – Recent deterioration • • • Review histology Review peri-operative course Clinical examination PR Pouchoscopy + biopsy Stool culture Oxford Colorectal

Common problems • Acute pouchitis – ciprofloxacin • Pouch-anal anastomotic stricture – EUA + gentle dilatation • Cuffitis topical steroids or mesalazine Oxford Colorectal
Phase 2 Assessment of persistent poor pouch function • Inside – Flexible pouchoscopy + biopsy – pouchogram • Outside – CT or MR pelvis • Below – Sphincter physiology and ultrasound – Pouchogram – EUA, pouch and cuff biopsies • Above – MRE – endoscopy • Emptying the pouch – Dynamic evacuating “proctography” Oxford Colorectal

INSIDE THE POUCH • • Chronic pouchitis Irritable pouch Small volume/non compliant pouch Cmv/c diff Oxford Colorectal
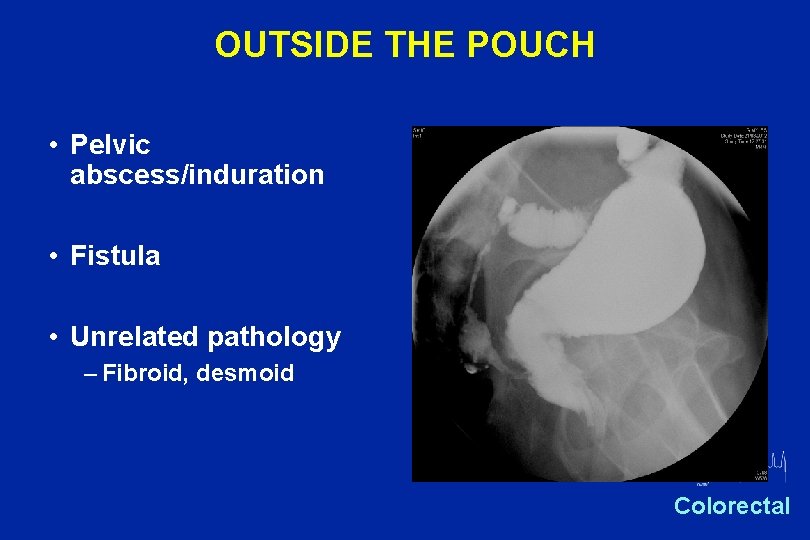
OUTSIDE THE POUCH • Pelvic abscess/induration • Fistula • Unrelated pathology – Fibroid, desmoid Oxford Colorectal
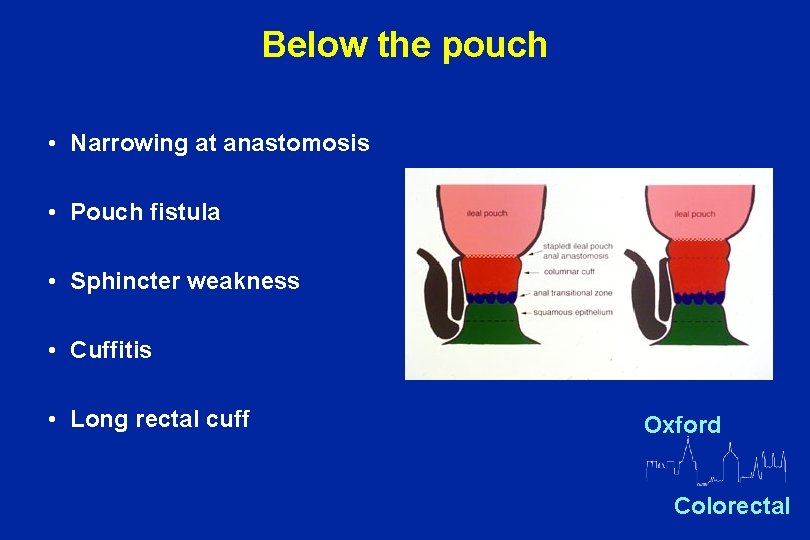
Below the pouch • Narrowing at anastomosis • Pouch fistula • Sphincter weakness • Cuffitis • Long rectal cuff Oxford Colorectal
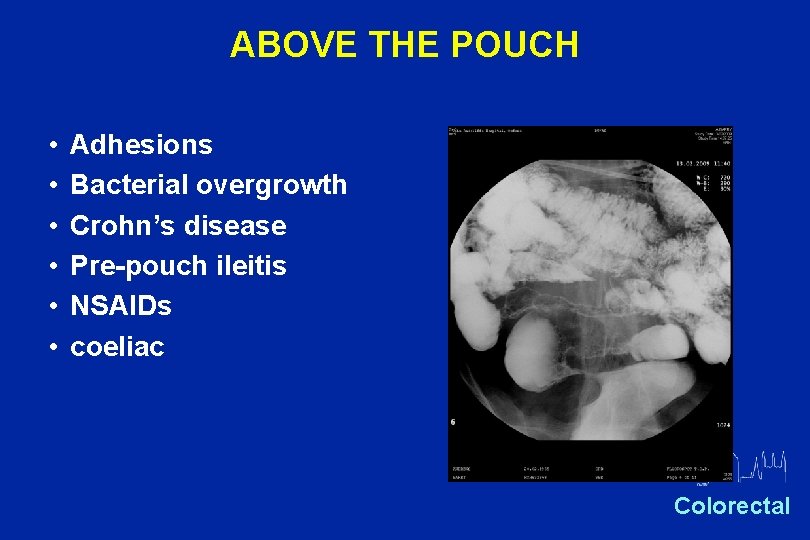
ABOVE THE POUCH • • • Adhesions Bacterial overgrowth Crohn’s disease Pre-pouch ileitis NSAIDs coeliac Oxford Colorectal

EMPTYING THE POUCH Internal pouch prolapse Anismus Oxford Colorectal

Treatment • Dependant on identification of cause of poor pouch function • Emerging concept: – Inflammation in/around pouch/fistula. Suspicion but no proof of Crohn’s – Leuven group: • 88% improvement with infliximab/adalimumab Oxford Colorectal
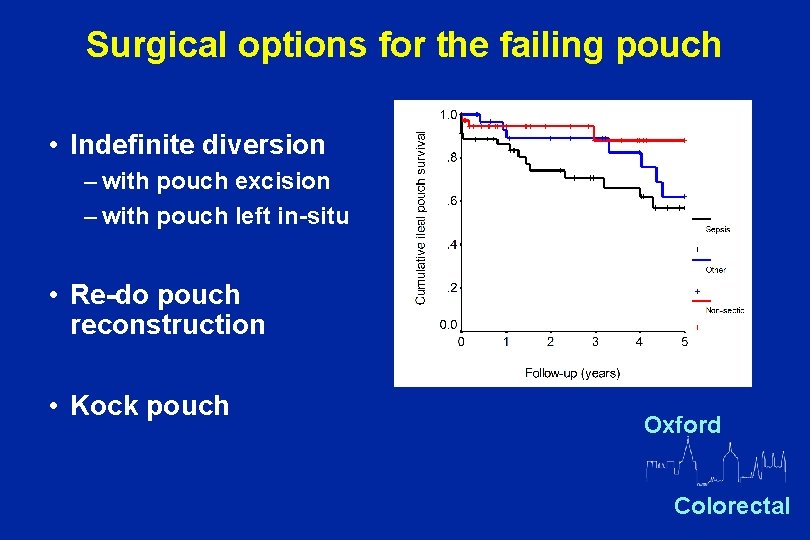
Surgical options for the failing pouch • Indefinite diversion – with pouch excision – with pouch left in-situ • Re-do pouch reconstruction • Kock pouch Oxford Colorectal

and finally. . . Summary of problems • Weather – 20 mph headwind • Under-estimating the task • Separation of cyclists and cyclists from van – Swanley underpass • Getting lost – Maidstone at 04. 15 • Different speeds – Non-chain gang • Food and drink • Strategy when problems occur • Negotiating skills Oxford – 22. 00, 45 miles from Paris Colorectal

Oxford Colorectal

Oxford Colorectal
- Slides: 28