Creating Positive Environments of Care Jayne Van Bramer

Creating Positive Environments of Care Jayne Van Bramer Former Director, Office of Quality Management

2 Note: This presentation was originally made on May 24, 2011. It has been modified and updated for accessibility.

3 The New York State Office of Mental Health wants to acknowledge the contributions of the National Association of State Mental Health Program Directors (NASMHPD) and its Office of Technical Assistance (formerly NTAC) for many of the concepts and some of the presentation slides that you will hear and see during this conference. Office of Technical Assistance National Association of State Mental Health Program Directors 66 Canal Center Plaza, Suite 302 Alexandria, VA 22314 (703) 739 -9333 http: //www. nasmhpd. org

4 It’s not about reducing restraint and seclusion… It’s about culture change I am here to talk about a subject that is near and dear to my heart. Not simply restraint reduction, but the creation of positive environments of care and the culture change that is necessary to achieve that. This work is not for faint of heart. Changing your organizational culture is the toughest task you will ever take on. Your organizational culture was formed over years of interaction between the participants in the organization. Changing the accepted organizational culture can feel like rolling rocks uphill.

5 Culture Change Organizational cultures form for a reason. Perhaps the current organizational culture matches the style and comfort zone of the company founder. Culture frequently echoes the prevailing management style. Since managers tend to hire people just like themselves, the established organizational culture is reinforced by new hires. Experts estimate that it takes 3 to 5 years to really change a culture. So let’s begin! What I want to share with you is a compilation of what I have learned from national experts, heard from hospitals in other states, and my private lessons learned.

6 Culture = Behavior, and it is Learned. People learn to perform certain behaviors through either the rewards or negative consequences that follow their behavior. When a behavior is rewarded, it is repeated and the association eventually becomes part of the culture. For us, much of our hospital culture is learned through interaction. Culture is difficult to change because it requires people to change their behaviors. It is often difficult for people to unlearn their old way of doing things, and to start performing the new behaviors consistently. Persistence, discipline, employee involvement, kindness and understanding, organization development work, and training can assist you to change a culture. It starts with the leadership. Leaders must first “talk the talk” (espouse the new values), and then “walk the walk” (model behaviors dictated by the new culture).

7 Culture Change through the Institute for Healthcare Improvement Framework 1. Set Direction: Mission, Vision and Strategy 2. Establish the Foundation 3. Build Will 4. Generate Ideas 5. Execute Change http: //www. ihi. org/Pages/default. aspx

8 The IHI Framework It is really also the framework for my talk today and what I hope to share with you - ideas for setting the direction, establishing a foundation for change, motivating employees, providing ideas, and making it happen.

9 Our Values �Commitment to Nonviolence and Non-Coercive Care �Commitment to Management of Dysregulation �Commitment to Trauma-Informed Care �Commitment to respectful interactions So how do we talk the talk? We do that by setting the direction which is our mission, vision, and values - who we are.

10 We Plan our Desired Organizational Culture… With a clear picture of where the organization is currently, the organization can plan where it wants to be next. Mission, vision, and values provide a framework for the assessment and evaluation of the current organizational culture Your organization needs to develop a picture of its desired future. What does the organization want to create for the future? Mission, vision, and values should be examined for both the strategic and the value based components of the organization. Your management team needs to answer questions such as: – What are the five most important values you would like to see represented in your organizational culture? – Are these values compatible with your current organizational culture? Do they exist now? If not, why not? – If they are so important, why are you not attaining these values? – Do your mission statements foster a recovery orientation? Are they strength-based? Hopeful? – And don’t forget the towards-what-end piece. You will provide safe, effective, high quality care in order for…

11 People do recover and regain meaningful life roles.

12 RESPECT: A Catalyst for Recovery by Joel C. Slack I remember a psychiatric hospital in which I spent 16 months as a patient. It was considered to be one of the most reputable private psychiatric hospitals in the country. It had the resources to purchase the best supplies for their occupational and rehabilitative therapies. The wards had wall to wall carpet. The antique furniture was professionally upholstered, and there was an Olympic size swimming pool and outdoor tennis courts. Undoubtedly, the professionals at this private hospital were administering the most updated technology available back then. But what I remember most about this hospital was that many of the professionals were insensitive, authoritarian, and often times they appeared to be more concerned with their reputation as researchers than as compassionate helpers. Upon reflection, it is no wonder that I ended up leaving that hospital in worse condition than when I was admitted.

13 RESPECT: A Catalyst for Recovery by Joel C. Slack My parents finally had me transferred to a state psychiatric hospital. There was definitely no swimming pool, no tennis courts and the furniture was in disrepair. The wards had never been refurbished and to this day my stomach turns when I remember some of the meals they served us. The most updated therapies were never administered because there were no funds to purchase the accompanying training. But what I remember most about this state hospital was that the professionals were conscious about their reputation as being kind and thoughtful helpers. With no resources, respect was all they had to offer the patients. And they offered their respect generously. Consequently, I began to feel better and stronger about myself and then began to participate and respond to whatever (poorly funded) services were available. I began to recover. In light of all that is offered in mental health systems around the world, respect continues to stand tall among the catalysts for recovery. Joel Slack

14 Strategies to Operationalize Our Commitments Ø Ø Ø Ø Redesign processes Employ best practices Use information support tools and data Coordination Nothing about us without us Manage your talent Accountability

15 Where to Begin? Make the Status Quo Uncomfortable • Recognition of pervasiveness of trauma • Recognition of the harm of restraint and seclusion Make the Future Attractive • Envision the best • Nurture the vision

16 It’s About Trauma We start by helping staff understand the pervasiveness of trauma. Research has shown that the rate of reported abuse in childhood and/or adulthood among women living with mental illness is alarmingly high: 80% of psychiatric inpatients have been physically or sexually abused. Studies find rates of 60 -90%, the higher levels being found in populations like we treat. We teach a universal precautions approach, since so many individuals in care have traumatic backgrounds - and often, so do the caregivers. Rajan, D. (2004). Violence Against Women with Disabilities. National Clearinghouse on Family Violence (NCFV). [Online]. Cited September 20: http: //www. phacaspc. gc. ca/ncfvcnivf/familyviolence/pdfs/2005 femdisabl_e. pd

17 Make the Status Quo Uncomfortable � Restraint and seclusion causes harm both physically and psychologically. � Teach your staff about the dangers, so they begin to question. In your program… …Do minor rule violations lead to control struggles where privileges are withheld or threats are made? …Must privileges (rights) be “earned”? …Do points equate with access to activities and programming? …Are compliance and containment mistaken for actual learning of new skills and real improvement?

18 It’s About Leadership Inadvertently, we as leaders have reinforced to staff that their job was to keep things quiet. That their job was control. I shudder when I think back on how I made rounds in the evening at Manhattan or Bronx, because you know what I said? “Everything quiet? ” Behavior is a function of past traumas. Behavior is not noncompliance, not defiance, not manipulation. Noncompliance is somebody doing something that you don’t want them to do. I am the queen of noncompliance. Behavior is a function of past traumas. Talk to staff about how restraint and seclusion cause harm, and the focus is on violence prevention and keeping everyone safe.

19 All behavior has meaning Behavior is a function of past traumas. ◦ Not noncompliance… ◦ Not defiance… ◦ Not manipulation. How do we perceive the behavior of the individuals we serve?

20 “A riot is the language of the unheard” Martin Luther King, Jr. We need to understand this, and teach a replacement behavior.

21 Precipitants of Aggressive Behavior Frustration Pain Sadness Anger Feeling scared The core reason is often trauma. It’s very unlikely that the goal is to hurt someone!

22 Consequences: A dirty word? Train staff in use of collaboration rather than consequences. If consequences must be used, make sure they are effective (e. g. planned ahead, clear, consistent, brief, pleasant voice, follow through, teach to alternative) Beth Caldwell, Caldwell Management Associates

23 Consequences: A dirty word? The single biggest shift in attitude we have to help staff through is from the belief that consequences are the most potent agents of change, to the belief that education and emotional supports are the most effective ways to help people change their behavior. So what we need to do is train staff in collaboration and the use of positive behavioral interventions. We need to continually revise (every 3 months) or rid your program of Level Systems, and replace them with individual goals and/or everyday collaboration and choices.

24 Paradigm Shift The shift in thinking is the shift from prioritizing justice to prioritizing healing. When you think of behaviors as responses that are the best they can offer, rather than intentional misbehavior, it changes the paradigm. You don’t punish your piano student for making mistakes. You say… “You’re not ready for a performance yet, let’s keep practicing. Don’t give up. I’ll teach you. You can learn this. ” Not, for example… “I can’t let this guy get away with hitting a wrong note. They need to be punished or they’ll never learn. ”

25 From Power and Control to Collaboration "Kids do well if they can. If they can't then it’s our job to find out why and teach them the skills they need so they can do well. ” Ross Greene, Ph. D. And the same applies for adults.

26 A Matter of Life and Death I want to talk for a minute about the dangers of restraint in NYS. Why are these power struggles wrong? They lead to hands-on interventions. Power struggles can and do lead to death.

27 In New York State Jonathan Carey, 13, smothered to death in 2007 by improper restraint under OMRDD’s care. This event led to Jonathan's Law. 15 -year-old Darryl Thompson died after being restrained face-down by two aides at an OCFS juvenile facility in 2007. It didn’t get as much press as Jonathan Carey…perhaps because he was a poor African American child?

28 In New York State In NYS, William George Agency, Alexis Javier Cirino-Rodriquez, 20, died on 10/13/10 as staff were attempting to restrain him after he'd assaulted one of them. The forensic pathologist “determined the cause of death to be from probable mechanical asphyxiation, from chest and neck compression during a struggle, with the manner of death being accidental. ” Not in our system, you think? Well, thankfully, deaths are few and far between, but in 2010 we did have a restraint death in a CPEP, of an individual who had definite trauma issues that were not really attended to.

29 Primary Prevention: The Primacy of Safety – Safe for you – Safe for the people we serve – Safe place for families – Safe for staff and visitors

30 First do no harm. It is the Hippocratic Oath, but also the core of what we do. Without a safe environment, no one can recover, heal, or develop resiliency. Staff can’t perform competently. Leaders can’t lead effectively. Safety is the foundation for all our work. When we talk to staff about safety, we need to communicate the fact that coercion-free environments are also safer for staff. Data has shown that such environments have fewer assaults on staff and fewer allegations of abuse.

31 Help staff see the vision The future determines the present Imagine giving tours of your program. What do you want people to see? How would you want the environment to be different? How do you want people to feel?

32 Help staff envision a better future Imagine your hospital in five years. What does it look like? How does it feel? What are the policies? What is the admission process? Open? No door? Spa-like? Sanctuary? Peaceful, warm, friendly? A program that cares A program that’s safe A program that communicates A program that understands A program that heals Now what does that look like.

33 Inspire a Shared Vision Three essentials – Listen deeply to others – Discover and appeal to a common purpose – Give life to a vision by communicating expressively, so that people can see themselves in it Kouzes, J. and Posner, B. The Leadership Challenge, 2008

34 Give staff something to rally around It is those values and that vision and mission that becomes your roadmap and can be operationalized into a strategic plan Help staff get in touch with why they went into this field. Sit and talk to them. So how did you end up working in mental health? Why here and not an IBM or Mc. Donald’s? We want to save the world, right? Help them reconnect to those feelings of wanting to help people.

35 Good to Great by Jim Collins profiled why some companies make the leap and others fail. He also published a Good to Great Social Services monograph. In it he talks about how you apply the concepts to the social sectors. In terms of getting the right people on the bus, he sees an advantage to the social sectors because we can tap into their idealistic passions these are people who seek nobility of service and meaning beyond the mighty dollar.

36 Leadership and power I think some of our leaders try to lead through the use of power. State employees, unions, permanency (how good is that, right? ) underscore the need for us to lead through leadership. We don’t have that much traditional power. But we do have the power of inclusion. The power of language. The power of shared interests. And the power of coalition. When a new CEO was hired for the Girl Scouts of America, she was asked by a NY Times reporter how it felt to be on top of such a large empire. She paused and explained she was not on top of anything, yet she had the ability to lead hundreds of disparate councils, each with their own governing board and almost a million volunteers into a new era - where tough teen issues like teen pregnancy and use of alcohol were confronted and addressed through educational materials and badges could be garnered for such topics as math and technology. To get things done within a diffuse power structure you need to rely on persuasion and the powers just mentioned - inclusion, and shared interests, and language and coalition.

37 Lesson Learned Leadership comes in all shapes and sizes; Leadership is in your heart. Inspire Shared Vision “If you want to build a ship, don’t drum up the men to gather up the wood, divide the work and give orders. Instead, teach them to yearn for the vast and endless sea. ” Antoine de Saint-Exupéry

38 While I still believe that is the ideal scenario, we have seen success when a unit manager (super TA) has taken this on as a passion. True Leaders can be informal too, and inspiration can come from many sources. Who reading this is a leader? Raise your hand. . . Every hand should be up. You are not a leader because of your title or your salary. You’re a leader because you can talk the language of a visionary and an idealist. You are a leader because you can forge a path no one has taken previously.

39 Essential Leadership Starting to see a theme here on how to effect change? � Practice: Challenge the process Commitments: (1) Search for opportunities and (2) Experiment and take risks � Practice: Inspire a shared vision Commitments: (3) Envision the future and (4) Enlist others � Practice: Enable others to act Commitments: (5) Foster collaboration and (6) Strengthen others � Practice: Model the way to the desired objectives Commitments: (7) Set the example and (8) Plan small wins � Practice: Encourage the heart of everyone involved Commitments: (9) Recognize individual contribution and (10) Celebrate accomplishments Kouzes, J. and Posner, B. The Leadership Challenge, 2008

40 Leadership Towards Organizational Change – Provide Resources. It doesn’t have to be money. It could be time to work on this committee assignment or designation as lead of working group. – Acknowledge early adopters. – Recognize those staff with a passion for this and empower them! – Promote and Protect Flexibility and individualized approaches. – Strategic Use of Job Descriptions and Performance Evaluations. Don’t use the civil service job descriptions, make your own and set expectations of hope, collaboration and strength-based, trauma-informed interactions. – True Recipient and Family Involvement

41 Teaching doesn’t happen in a classroom. I tell you and you forget. I show you and you remember. I involve you and you understand. - Eric Butterworth We have had a lot of success where we used on-ward trainer-mentors who became part of the fabric of the organization and provided modeling and mentoring to staff on an ongoing basis. To have someone reframe in the moment and be willing to roll their sleeves up and identify and get involved in a difficult situation was very important.
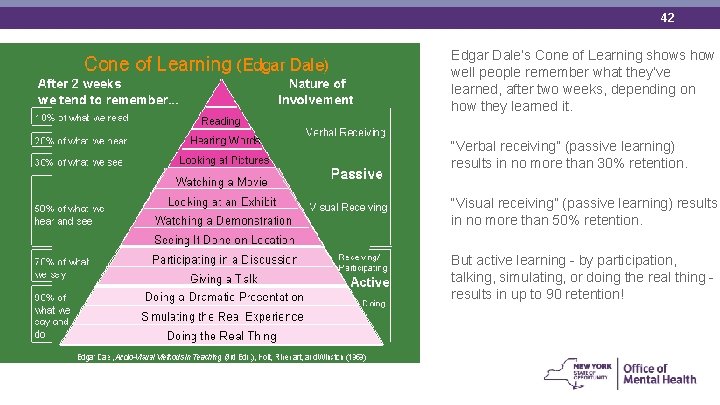
42 Edgar Dale’s Cone of Learning shows how well people remember what they’ve learned, after two weeks, depending on how they learned it. “Verbal receiving” (passive learning) results in no more than 30% retention. “Visual receiving” (passive learning) results in no more than 50% retention. But active learning - by participation, talking, simulating, or doing the real thing results in up to 90 retention!

43 Staff Training � Moment-to-moment assessment of level of stability/dysregulation � Matching an intervention to that level � Building Partnering Relationships � Pre-teaching � Motivation without threats � Early Intervention � Ways to build up mood and resilience/increase joy � Creating situations that are as safe as possible � Being persistent without escalating a situation � Individualizing your response � Emphasizing intrinsic rewards of positive behavior � Facilitating soothing and self-soothing � Power of refocusing attention Rob Terreden, Director Three Rivers Intensive Residential Treatment Program

44 We train staff in – CPR – Infection Control – Filling in an incident report – Writing notes All important stuff. But Rob Terreden’s items are the essence of the job that help a person’s recovery. These are what builds resiliency. They are skills that Maximize Staff Influence and Minimize the Use of Coercive Techniques.

45 So much for leaders. What about staff? Our job as mental health caregivers is to figure out the triggers and early warning signs for challenging behavior …and teach replacement behaviors.

46 The Role of Behavioral Health Staff �Teacher �Cheerleader �Positive Reinforcer �Healer …Not Rule Enforcers and Jailers. It’s about collaboration and not control.

47 The Role of Behavioral Health Staff And the job is to take opportunities to build positive experiences and teaching outside the context of a failure. This means offering support when a person is only slightly agitated - which also means becoming skilled at assessing an individual’s level of dyscontrol or agitation. The people we serve learn more from success than failures.

48 How do we support staff in using collaboration and empowering approaches? �Modeling and Mentoring �Training �Paying Attention �Strength Based Supervision �Capture Success; Record and Celebrate

49 "Do as I say, not as I do. " That approach is not good enough. To be a great leader you must be willing to get your hands dirty and show your people how it's done when the circumstances warrant it. What it doesn’t mean is swooping in when an individual is totally out of control to try and save the day. Because you know what will happen. Punched in the nose! Model the behavior you wish to see in staff. Training around collaborative, practice reframing directives with staff, empowering, strengthbased, trauma-informed interactions. Train in conflict avoidance. Do we do this? Do we assess these competencies? How hopeful and positive are we? Strength-based supervision - Public praise, Private feedback. Great Mr. Jones. Say something positive. Catch them doing something good. Every time you make rounds. Keep a notebook to remember.

50 University of Southern Florida USF taught teachers how to implement best practices. They measured uptake: Classroom and role-playing only: only 5% implementation Classroom, role-playing, coaching and supervision: 95% implementation! Supervision can be in groups, but staff need some individual time. Shape behavior by praising the competencies we want to see.

51 How do we support staff in using collaboration and empowering approaches? Reasonable Risk-Taking Encouraging Flexibility Promoting the Use of Individual Strategies …Scary, right?

52 I need you to support your staff in taking risks. I’m offering Individualized Care. It’s Risk Management gone amok.

53 What to do in a crisis? It’s difficult for folks to process during a crisis. Reception language skills are decreased. Broca’s area of the brain is actually deactivated. That area is responsible for speech, so it’s difficult to talk. The amygdala’s flight or fight response is activated. Think these sensory things will work? Oh wait I have some peppermint gum. I try to hand that to you… We need to provide comfort to assist individuals to re-focus.

54 Exercise Imagine that you’ve worked a very long day… Your Director wanted several things finished by COB. One of those days with no time to sit. We’ve all had them. Pull into your driveway and see a car. Through the sheer drapes you can see your husband kissing another woman. You are so angry that you can’t even lock the car - you go flying through the front door. Your sister-in-law is there and she hands you a stress ball and tells you to calm down. How are you feeling?

55 Don’t direct, but Ask… • How can I help you? • What do you need? • Are you HALTT? Don’t tell people to calm down. Ask: Are you Hungry? Angry? Lonely? Thirsty? Tired? You are angry and right then you want your anger validated…and that woman out of your house.

56 Use Visual Support Individual’s level Look, Listen and Observe Not yelling direction from across the room Do realize the person is not processing, and make adjustments as needed Give space Use a supportive stance Soft voice

57 That famous UCLA study: Communication is 93% nonverbal. Body language is so important. How do we talk to the individual in care? Stand over them? Take a safe and supportive stance. Talk to individuals on their level, not standing while they sit. Think about when you took your child to daycare or preschool for the first time. What did the teacher do?

58 Our wards are often too loud. Don’t yell down the hall. No screaming “Telephone!” at lunch time. Read incident reports. Staff seem to approach almost every issue like it is the line in the sand issue because we have indirectly reinforced that their job is control.

59 The underlying philosophy of 'collaborating' is premised on 'treating everybody with dignity and respect'. Beth Caldwell, Caldwell Management Associates

60 Collaboration is… Collaboration is about treating everyone with dignity and respect. One respects the person in care/co-worker/boss enough to approach him/her in every interaction using a kind and sensitive voice tone. Anyone remember Dr. John Oldham? He was a Medical Director for OMH. Monthly meetings get heated. The louder we got, softer he got. Very effective.

61 Respect is like Air Take it away and that is all people can think about Michael Woods, M. D.

62 Rule-Busting Committee This can be a really fun exercise. Have each shift write the rules down - each shift. Include both written and unwritten. Think they are the same across shifts? They differ even by different staff on the same shift! Go through each, and determine what rules are for recipient recovery, versus staff convenience. What is empowering versus easier for staff? What rules are absolutely necessary? Do we need rules about when to get up? When to shower? When to do laundry?

63 But…but… “But if I let John sleep in on Saturday, everyone will want to, and the day shift will be annoyed at the evening shift. ” Talk through/walk through the scenarios.

64 Not all change is good, but nothing gets better without it. Let’s not be so arrogant or rigid so as to believe that we can’t grow and learn. “Are you saying we’re no good? ” “I’m saying we’re great and can do better. ” Even “best practices” are only best until we imagine something better. In the face of dangerous behaviors, let’s not speculate about whether this new approach can work. Let’s ask, “Is there anything we haven’t tried yet to support getting the best from this youth? ” Rob Terreden, Director Three Rivers

65 All change is scary. We are creatures of habit, and talking to staff about change is an important part of the process. But nothing gets better without change. We can all grow and learn. We can all do better. We can all try something new.

66 The Advantage of 24/7 Care …Is that it is 24/7. The treatment milieu is a therapeutic agent to support a Trauma-Informed Culture We have a lot of opportunity to have an impact. With almost 30 years in mental health, I have been around long enough to see the term “therapeutic milieu” became almost a dirty word where the flavor of the day became structured programs and activities. The pendulum is swinging back. The brain can be changed. That is what treatment is about. That’s why it’s hard. It takes consistency, and working with individuals over and over again.

67 Practicing compassionate care involves: �Asking questions and listening attentively to the answers �Interpreting facial expressions and body language while maintaining an awareness of one’s own �Judging the best way to explain a diagnosis, treatment, and self-care to individuals and family members based on considerations such as language, culture, and education Putting the Care in Health Care, TJC

68 How to put individuals in care and their families at ease � Make eye contact. � Smile. � Sit rather than stand. � Listen without interrupting. � Convey attentiveness by leaning forward. � Keep arms uncrossed. � Respect silence. � Use touch appropriately. � Ask questions. � Discuss expectations and past experiences fully. Putting the Care in Health Care, TJC Ask yourself: On a daily basis, do we assess aides and nurses for these skills? Teach! Monitor! Reinforce!

69 Moving From Control to Collaboration Staff: • Are respectful • Understand 3 basket/plan approach (see next slide!) • Extinguish ‘control type statements’ - replace with collaborative statements • Offer choices • Identify triggers & respond with collaborative/gentle teaching approach Beth Caldwell Management Associates

70 The 3 Basket Approach The 3 basket approach to conflict involves deciding whether you can q Let it go q Compromise, collaborate q Hold firm Most of us have raised our kids this way. Remember the terrible twos? Adolescent daughters? Teenage boys? If you were like me you quickly learned to pick your battles. We have to decide what we can ignore or let go, what we can negotiate, and what is written in stone. Car seat - Must No drugs - Must Curfew - Negotiable Won’t eat dinner? Let it go

71 Employ Best Practices The Ultimate Clinical EBP – Congruence (genuineness, honesty with the individual in care) – Empathy (the ability to feel what the person in care feels) – Respect (acceptance, unconditional positive regard)

72 ACT, DBT, CBT, Supported Employment, Wellness, Co-occurring Treatment, Family Psychoeducation, Trauma Focused CBT, Multisystem Therapy… These are all great. But most powerful EBP? You don’t need to be a trained clinician to provide it. Consumers who were asked what made the difference in their recovery said it was care, compassion, and hope. Sometimes from one person. The Super EBP is within all of us. We don’t need a Ph. D. , we don’t need to be clinical. We want to decrease that 15 -year gap between what research tells us works and what we actually do.

73 Lesson Learned Numbers Crunching doesn’t tell the whole story. “Not everything that can be counted counts, and not everything that counts can be counted. ” Albert Einstein

74 Another lesson I learned through our grant: We submitted a ton of data and monitor patterns and trends monthly. What we didn’t capture was the human side of what we are doing: The story of the nurse who helped the child create a fort with her blanket and a chair and then crawled into the fort to administer meds… The adolescent who approached the nurses station with wrists turned outward asking for some of the cream that helps her sleep… The aide who walks around the ward with a bedtime basket with various pillow sprays the children can pick from… The child who felt better about their admission after the hospital allowed Mom to bring her pet rat into the hospital during the Mom’s visit… I could go on and on. We have decided as part of our final year activities that we are going to try to capture these moments.

75 Turning Data into Information What did you find? What did you do about it? Who did you tell? Did you remember the story? “Could This Happen in Your Program? ” http: //www. justicecenter. ny. gov/sites/default/files/archivereports/Publications/00037. pdf Why is it so effective? It puts a face on it, makes issues come alive. Emphasis is on measurement, because that which can’t be measured can’t be improved. But we still need to remember the story. It is the story which inspires.

76 Lesson Learned It takes a village. Partially because this work is so hard, the effort needs to be all-inclusive.

77 Coordination Communication is key to recovery: Among clinicians, shifts, wards, treatment malls, families, support systems and the individual in care Collaboration, Coordination, and Communication The three C’s are mandatory for a successful transformation. TJC has concluded that upwards of 80% of adverse events have communication problems as root causes. SBAR Hand Off. It’s an opportunity to ask questions, to have a conversation, not a piece of paper: http: //www. ihi. org/resources/Pages/Tools/SBARTechniquefor Communication. ASituational. Briefing. Model. aspx

78 “Nothing About Us Without Us” There is agreement on – goals – tasks The relationship is experienced as – collaborative empathic – respectful trusting – understanding hopeful – encouraging empowering
79 Transparency Is Your Friend Move from “Recipient Council” to recipient and family involvement in hospital-wide committees! We need true involvement, not just an annual survey. Not just an advisory committee, but recipients and families participating in key hospital committees and task forces. It is having them to be a regular part of the review process (or sign-off) for new policies. We want the most honest feedback. Solicit it post-discharge. Ask recipients to manage the survey process.

80 Language/signage is important. We don’t always see the message we deliver.

81 Go though your facility with fresh eyes. Go with a family member or someone receiving outpatient services. See it with fresh eyes. Is your signage warm and welcoming? On a kids’ unit in a state PC, I saw a sign that said: “ 10 feet from the Nursing Station or lose 100 points. ” We see so many “Do Not (…)” signs and rules…“Police Leave Your Guns…”

82 Our language When we are talking, do we have the language down? Is it strength-based, trauma-informed, person-centered? Do we follow through on policies and practices?

83 Eight Steps for Leading Change John Kotter of Harvard Business School studied why transformation efforts fail, and suggested Eight Steps for “Leading Change”. Establishing a Sense of Urgency Forming a Powerful Guiding Coalition Creating a Vision Communicating the Vision Empowering Others to Act on the Vision Planning for and Creating Short-term wins Consolidating Improvements and Producing Still More Change Institutionalizing New Approaches

84 Leadership in Action Malcolm Gladwell’s The Tipping Point, 2000 Working the tipping point – Create an “epidemic” around the main thing – Talk it, write it, sell it …Identify champions – Make your ideas contagious …Memorable, motivating, practical and personal – Use early adopters to spread the word – Communicate, train, mentor and reinforce When you are working on culture change, keep in mind that you don’t have to convince everyone!

85 A whole new lens… Seeing the individuals in care differently. Knowing that people do well if they can. Training to help appreciate that if individuals have challenging behaviors, they are not doing it on purpose. Appreciate their “maladaptive behaviors” are their best attempts at coping with their difficulties in self-regulation and life’s daily challenges. Caroline Mc. Grath, Executive Director UMass Adolescent Treatment Programs Clinical Instructor UMass Medical School

86 Where we want to go �Adopt the concept of “universal precautions. ” �Appreciate the prevalence and pervasiveness of trauma and our responsibility to make sure our practices and policies are trauma-sensitive. �Seeing behaviors through a trauma-informed lens deepened our empathy for the adversity they faced, and helped us to understand that their “trauma logic” was not so crazy.

87 Lesson Learned Both staff and leadership want tools, something tangible. We have received repeated requests for tools from our grant sites both leadership and staff wanted us to give them the tools to be successful - tools apart from the Six Core Strategies. The fact is, the most important tool is inside them - it’s that strength-based, noncoercive interaction. It’s compassion, it’s empathy, but sites wanted something “tangible”. The grant allowed us to provide stuff on many levels. We have come to truly appreciate the power of sensory modulation. Try a Fireball PRN!

88 Why Use Prevention Tools? Prevent injury and trauma to staff and individuals in care Help de-escalate Meet individual’s identified sensory needs Help maintain a safe therapeutic environment We expand our tool box of interventions and strengthen therapeutic alliance

89 Prevention Tools Include: Calming Plans…Sensory Items… Calming Rooms…Calming Items…You! Get a PRN to go for a swing, or to pet a dog if there is one. Doctors in hospitals in other states write orders like this. Next time you call a doctor, ask them to write a PRN order for basketball. These are our tools to prevent R/S. Increased options in crisis and daily activities, for youth and staff Decreased agitation Clear, measurable way to decrease levels of distress Improved quality of care and therapeutic experience Improved work environment

90 Animal Assisted Therapy � To decrease depression, improve mood and affect � To reduce anxiety, isolation, and problem behaviors � To improve self esteem and feelings of self-worth � To improve socialization and communication � To provide affection, pleasure, and learn appropriate touch Denise Geissert, M. D. Child and Adolescent Psychiatric Fellow, University of Buffalo I am not a pet person, but I have become a believer in the unconditional love of an animal. Animals have been used for companionship for centuries. Evidence of a symbiotic relationship between humans and animals dates back to earliest forms of civilization. A positive bond between humans and animals has always existed.

91 Benefits Animal Assisted Therapy �To increase the ability to trust others and express feelings �To improve concentration, attention, memory, and recall �To address loss and issues with grieving �To improve problem-solving abilities and cooperation Denise Geissert, M. D.

92 Tommy This is Tommy, the psychiatric service dog at Western New York Children’s Psychiatric Center

93 Grant sites have gone from no animals, to having therapy dogs come in once a week, to having a therapy dog belong to the agency. Parents now routinely bring family pets in when they visit. We ask them to do this in parent handbooks.
94 Dogs and Puppies Kids playing with fuzzy puppies. Doesn’t that feel good? Thanks to Robert Reusch at WNYPC for sending me this link. Please maximize this tool… It’s very, very effective. You could get an affectionate ward cat!

95 Not Enough Space? Consider Sensory Carts Brylin’s cart is used frequently. Warhead candies are available. They’ve seen a decrease in: ◦ Restraint use ◦ Property damage ◦ Self-destructive behavior ◦ Physical assaults/injury

96 Sensory Cart The House of the Good Shepherd was our first PARS grant site to recycle an old medication cart.

97 Sensory Input How we feel is directly impacted by information received through the different senses: 1. Sight 2. Sound 3. Smell 4. Touch 5. Taste 6. Proprioception 7. Vestibular input

98 Sensory Experience Sensory experience is something all human beings share. How we feel is directly tied to the sensory information we process through the 5 senses. We all have ‘sensory diets’ – primarily, we are either looking for stimulation or looking to avoid stimulation. These sensory needs change over time; they are not static. If you become ill or have a migraine headache, your sensory needs change.

99 Calming Environments Western NY Children’s Psychiatric Center There are some very simple enhancements that create positive sensory experiences and promote better feeling states. plants artwork music curtains music comfortable seating bedrooms with new bedspreads place to exercise low lighting (dimmer switches) aromas

100 Calming, Self-Soothing Activities hot shower/bath wrapping in a heavy quilt decaf tea rocking in a rocking chair beanbag tapping yoga drumming meditation Calming activities are particularly helpful for people with tension and anxiety who have difficulty unwinding and feeling physically relaxed. These strategies can be practiced. People who feel physically better will begin to feel better emotionally. The mind and body are connected. These are activities that can be used by the person in the home and community. Tai Chi was most effective for one person, and the hospital worked hard to link her up with this resource upon discharge.

101 Comfort Room: A prevention tool to reduce the use of seclusion and restraint Comfort rooms are places of sanctuary, right on the units. Persons served are an integral part of developing your comfort room. Teen Lounge at Brylin

102 Comfort Room The House of the Good Shepherd Use of a Comfort Room is voluntary - though staff may suggest its use and be present if the person desires it.

103 Brylin’s Comfort Room: Snoezelen tubes on left It is a sanctuary from stress, and/or a place to experience feelings within acceptable boundaries.

104 Other Environments To meet the calming needs expressed by youth, these spaces were developed at Western NY Children’s Psychiatric Center. The space outdoors was turned into a quiet garden where children can be alone with nature, with a staff member, or with family. Because so many children have “energy to burn”, the youth saw exercise as a way to self-regulate. This is particularly important for children who need motion to calm.

105 Murals The House of the Good Shepherd

106 Incorporate the use of sensory items into both the treatment plan and calming plan Practice calming plans. Self-control is of paramount importance. The most important skill we can teach our children is self-control. It’s also important for individuals in care. Write orders to implement calming plans.

107 Activities serve many purposes: Increase resilience to stress by creating a reservoir of pleasure Show we care Foster bonding with staff through having fun together Offer joint pressure, and heavy work to calm nervous system Foster feeling that life is worth living; counter feelings of hopelessness and apathy Activities and programming is not just busy work to pass the time. Poets and philosophers have proposed that joy and sorrow are actually just different ends of one emotion or continuum. When you increase joy and have fun, some of that other stuff does go away. Even symptomatology.
108 http: //www. bostoncf. org/ Let’s take a look at a new evidence-based intervention for addressing trauma. The program is called Rainbow Dance, out of Massachusetts. It’s primarily used with children who have experienced natural disasters, but it’s also used effectively with our population. When I look at it, I see joy.

109 Instill Joy! Have fun on your wards. Be silly. – – Dance Sing Tell Jokes Giggle Read “Teaching Your Children Joy” by Linda and Richard Eyre Create the joy of spontaneity. Have an upside down meal! Create a “Favorite things” wall. The joy of the earth: the smell of lilacs, treasures in a vegetable garden. (you can even plant in bags these days - check out Gardener’s Supply Company) The joy of creativity and imagination (art) The joy of sharing and service (find something wonderful to share a flower, something nice you heard on the news, a joke) Do secret good deeds.

110 What are Community Meetings and why are they important? �They are daily group meetings with individuals in care and staff. The meetings are empowering. They provide a forum to voice needs and concerns. �It’s a group process to create a community of safety and build trust. Community Meetings are the best way to ensure that individuals in our facilities are understood and respected.

111 Community Meetings Exercise What are you feeling? What is your goal for today? Who can you ask for help if you need it? Sandra Bloom, M. D. Creator of the Sanctuary Program http: //www. sanctuaryweb. com/

112 Importance of Workforce Development Tell them… Reduction of R/S is your job You are part of the “team” You are a role model You are a leader You are an agent of change You are a primary prevention tool! Our best asset…Our workforce.

113 Lesson Learned Culture involves how we treat individuals in care… …and how we treat staff

114 The Golden Rule As Management does unto Staff… So shall Staff do unto Consumers Beth Caldwell, Caldwell Management Associates

115 Workforce Caliber �An informed and skilled workforce is critical to make a transformed system of mental health care a reality. �A recovery-oriented system of care must, first and foremost, be informed by the prevalence of trauma among the people it serves. �It is imperative to have a workforce completely indoctrinated in the value and power of full inclusion of service recipients in interdisciplinary teams. Building A Better Mental Health Workforce Kevin Ann Huckshorn, RN, MSN, ICADC

116 Kevin Ann Huckshorn is the national leader at the forefront of these efforts. A skilled workforce is key to system transformation. A skilled workforce understands trauma and person-centered care.

117 So make the best of this resource. Manage your talent. Hire smart • Look for compassion • Discuss hot buttons and response • Perceptions from individuals in care Use the probationary period when they are the best they can be Practice management by walking around Make supervision and guidance strength-based Develop and mentor staff Remember: You need your staff more than they need you

118 Not everyone is cut out for this work. It is okay to someone in an interview: You know, I am not sure this job is for you.

119 A Leader's Guide to Rewarding and Recognizing Others 1. Set clear standards 2. Expect the best 3. Pay attention 4. Personalize recognition 5. Tell the story 6. Celebrate together 7. Set the example Encouraging the Heart Kouzes and Posner, 2003 Can you think of a time a boss recognized you or praised you? So what was special about that?

120 Encouraging the Heart 1. Set clear standards. The first prerequisite for encouraging the heart is to set clear standards (goals and values or principles). To be successful in encouraging the heart, it's absolutely critical that everyone cherish a common set of standards. 2. Expect the best. Only high expectations have a positive impact on actions and on feelings about oneself. Thus, passionately believing in people and expecting the best of them is another prerequisite to encouraging the heart. 3. Pay attention. One way of showing you care is to pay attention to people, to what they're doing, and to how they're feeling. If you are clear about the standards of behavior you're looking for, and you believe and expect that people will perform like winners, then you're going to notice lots of examples of people doing things right, and doing the right things. Every time you make rounds.

121 Lesson Learned Debriefing is easier said than done. Almost everyone is having a hard time meeting the requirements of OMH policy and regulation. People ask about post-event debriefing, who needs to be there, what they need to ask. There’s been too much focus on the process and not the outcome. Get feedback from the person.

122 How Do We Say It? “Is there anything that you would do differently? ” “What could we have done to make the restraint (or seclusion) less hurtful? ” “What upset you most? ” “What did we do that was helpful? ” “What can we do better next time? ” It’s critical that we use the right language to debrief an incident. There are many things to take into consideration. Can you think of a few things to consider? (Age, developmental age, state of mind, physical location, language or cultural barriers, etc. ) It is important that questions are asked in non-threatening, non-judgmental manner.

123 Effective Debriefing a. k. a. Giving Up Control �“When would you like to have the debriefing? ” �“Where would you like to meet to talk about how we can better help you get through times like yesterday? ” �“Are there any special staff you would like to be present? Are there family members you would like us to get on the phone or invite to the meeting? ” �“Is there anyone you don’t want there? ” What is your mechanism for documenting their perspective?

124 NASMHPD/NTAC Six Core Strategies © to Reduce the Use of Restraint and Seclusion Has been recognized as an EBP! Leadership towards organizational change Use of data to inform care Workforce development Restraint and Seclusion Prevention Tools Use of Consumer Roles Rigorous Debriefing

125 A quick plug for the Six Core Strategies© • Leadership builds consensus about values, vision, and mission and brings together a guiding coalition to make a strategic plan. • Leadership provides pre-and post-witnessing on the use of restraint and seclusion, 24/7. • Leadership appreciates the facets involved in changing a culture to improve the care and treatment environment. These facets include the norm, language, and customs. “It’s the way things get done around here. ” • Data is elevated and reviewed daily, hung in all areas for stakeholder review as well.

126 “Do not go where the path may lead, go instead where there is no path and leave a trail. ” Ralph Waldo Emerson
- Slides: 126