Creating a Screening Algorithm for Sexually Transmitted Infections











- Slides: 18

Creating a Screening Algorithm for Sexually Transmitted Infections: Baiye N. Orock, MPH, U of S School of Public Health Dr. Mark Vooght, MHO, FHHR April 2015

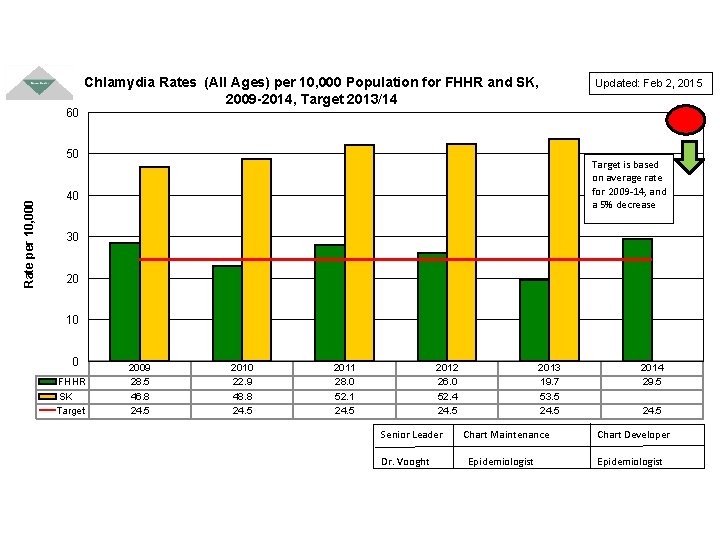
60 Chlamydia Rates (All Ages) per 10, 000 Population for FHHR and SK, 2009 -2014, Target 2013/14 Rate per 10, 000 50 Updated: Feb 2, 2015 Target is based on average rate for 2009 -14, and a 5% decrease 40 30 20 10 0 FHHR SK Target 2009 28. 5 46. 8 24. 5 2010 22. 9 48. 8 24. 5 2011 28. 0 52. 1 24. 5 2012 26. 0 52. 4 24. 5 Senior Leader Dr. Vooght 2013 19. 7 53. 5 24. 5 Chart Maintenance Epidemiologist 2014 29. 5 24. 5 Chart Developer Epidemiologist

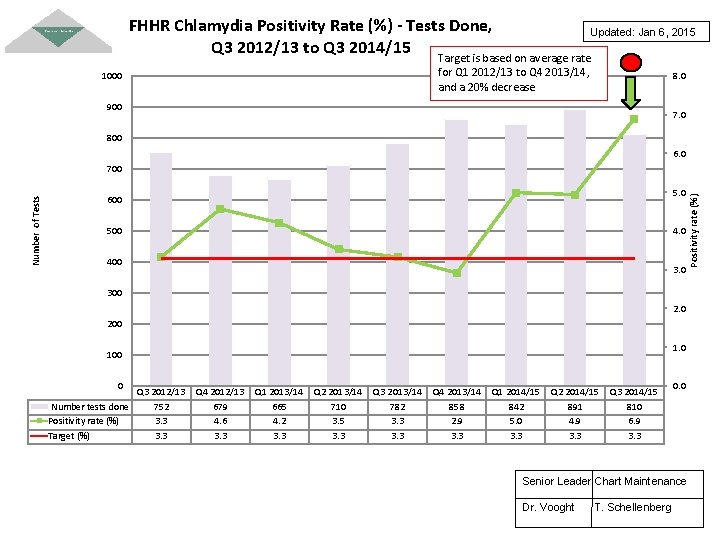
FHHR Chlamydia Positivity Rate (%) - Tests Done, Updated: Jan 6, 2015 Q 3 2012/13 to Q 3 2014/15 Target is based on average rate for Q 1 2012/13 to Q 4 2013/14, and a 20% decrease 1000 8. 0 900 7. 0 800 6. 0 5. 0 600 500 4. 0 400 3. 0 300 2. 0 200 1. 0 100 0 Q 3 2012/13 Number tests done 752 Positivity rate (%) 3. 3 Target (%) 3. 3 Q 4 2012/13 679 4. 6 3. 3 Q 1 2013/14 665 4. 2 3. 3 Q 2 2013/14 710 3. 5 3. 3 Q 3 2013/14 782 3. 3 Q 4 2013/14 858 2. 9 3. 3 Q 1 2014/15 842 5. 0 3. 3 Q 2 2014/15 891 4. 9 3. 3 Q 3 2014/15 810 6. 9 3. 3 0. 0 Senior Leader Chart Maintenance Dr. Vooght T. Schellenberg Positivity rate (%) Number of Tests 700

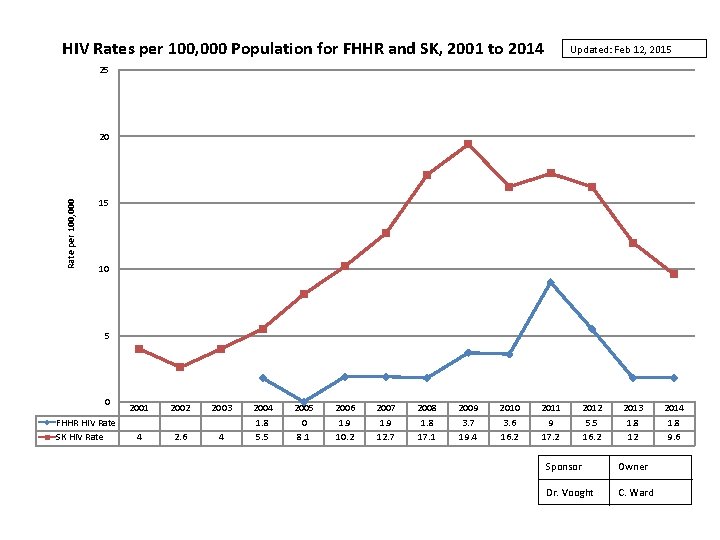
HIV Rates per 100, 000 Population for FHHR and SK, 2001 to 2014 Updated: Feb 12, 2015 25 Rate per 100, 000 20 15 10 5 0 FHHR HIV Rate SK HIV Rate 2001 2002 2003 4 2. 6 4 2004 1. 8 5. 5 2005 0 8. 1 2006 1. 9 10. 2 2007 1. 9 12. 7 2008 1. 8 17. 1 2009 3. 7 19. 4 2010 3. 6 16. 2 2011 9 17. 2 2012 5. 5 16. 2 2013 1. 8 12 Sponsor Owner Dr. Vooght C. Ward 2014 1. 8 9. 6

Issue: Develop an Evidence-based STI Screening Decision Tool • The development of an STI screening decision tool to be used by healthcare providers • Screening to be risk-based ? • This to be informed by conducting a literature review

RESEARCH QUESTIONS: • 1. What are the evidence-based algorithms for identifying sexually transmitted infection risk factors and testing requirements in adult patients presenting to primary care? • 2. What are the evidence-based guidelines regarding optimal risk grouping, age cohorts, risk categories, and timing of screening for sexually transmitted infections in adult patients?


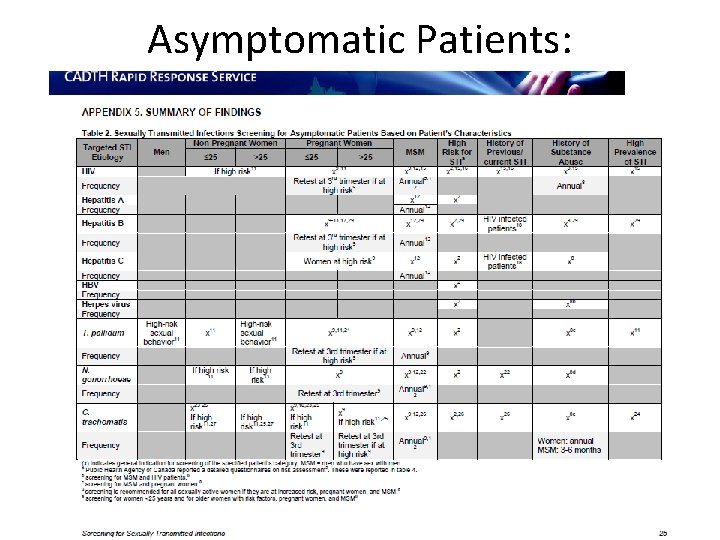
Asymptomatic Patients:

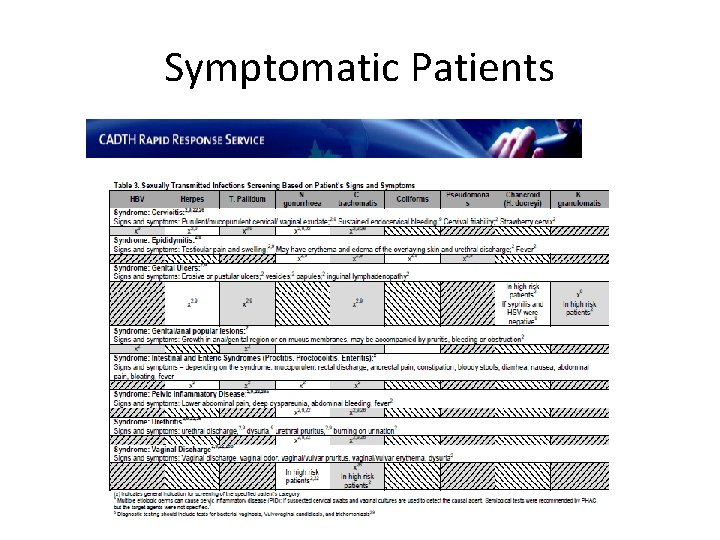
Symptomatic Patients

Utilizing the Evidence: • We predominantly used 6 STI Guidelines, to create a screening algorithm • Risk-based

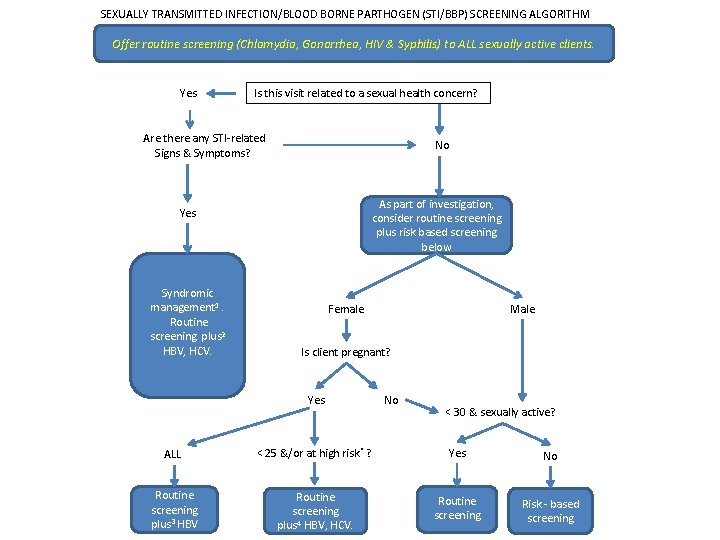
SEXUALLY TRANSMITTED INFECTION/BLOOD BORNE PARTHOGEN (STI/BBP) SCREENING ALGORITHM Offer routine screening (Chlamydia, Gonorrhea, HIV & Syphilis) to ALL sexually active clients. Yes Is this visit related to a sexual health concern? Are there any STI-related Signs & Symptoms? No As part of investigation, consider routine screening plus risk based screening below Yes Syndromic management 1. Routine screening plus 2 HBV, HCV. Male Female Is client pregnant? Yes No < 30 & sexually active? ALL < 25 &/or at high risk* ? Yes No Routine screening plus 3 HBV Routine screening plus 4 HBV, HCV. Routine screening Risk - based screening

Risk-Based Screening: Important: Go through ALL questions as the client may be in more than one risk category: Using IV drugs or other addictive substances? Add HBV 5, HCV. Same-sex partner( MSM 6/WSW) or bisexual? Add HAV 5, HBV 5, HCV. Sex trade workers and/or their clients? Add HBV 5. Recently in an STI endemic area 8? Add HBV 5 ; consider Chancroid#, LGV#, Granuloma inguinale # Are there any other risk factors 9? Routine screening & Other 2 Client requests STI screening consider Parasitic 7 STI

STI /BBP Screening Algorithm SEXUALLY TRANSMITTED INFECTION/BLOOD BORNE PARTHOGEN (STI/BBP) SCREENING ALGORITHM SUPERSCRIPT: 1 - Focused primary and secondary prevention counselling; treatment as necessary and partner follow up. 2 – Offer routine screening and/or screening based on institutional or local prevalence of STI. 3 – For all pregnant women, Chlamydia and Gonorrhea screening recommended for first prenatal visit. If positive, re-test within 3 – 6 months. 4 – For all pregnant women at high risk, Chlamydia and Gonorrhea screening recommended for first and third trimesters. Also repeat HIV serology during labour for those at high-risk. 5 - Offer serological screening and immunize accordingly following Hepatitis A and B immunization recommendations as per the Saskatchewan Immunization Manual, available at: http: //www. health. gov. sk. ca/sim-chapter 10 6 – Sample collection for MSM should be at site of receptive/penetrative oral or anal sex (Pharyngeal, urethral and/or rectal). 7 – Examples of a parasitic STI include trichomoniasis, pubic lice and scabies. Screening may be necessary only for trichomoniasis. 8 – For a list/map of STI endemic regions/countries, refer to: http: //www. who. int/gho/hiv_013. jpg --- HIV -endemic regions http: //www. cdc. gov/immigrantrefugeehealth/guidelines/domestic/sexually-transmitted-diseases. html -- Syphilis- endemic regions (see Table 3). NB: “The largest number of new infections occurs in the region of South and Southeast Asia, followed by sub-Saharan Africa, Latin America, and the Caribbean” CDC, 2011.

STI /BBP Screening Algorithm 9 - OTHER RISK FACTORS: -Sexual contact with person(s) with a known STI. ABBREVIATIONS -A new sexual partner or more than two sexual partners in the past year. HAV = Hepatitis A Virus. -Serially monogamous individuals. HBV = Hepatitis B Virus. -No contraception or the use of only non-barrier methods of contraception (i. e. no condoms). -Any individual engaging in unsafe (i. e. Unprotected) sexual practices -“Survival sex”: exchanging sex for money, drugs, shelter or food. -Anonymous or internet sexual partnering. -Victims of sexual abuse. -Previous history of STI -Living in an area with high prevalence of STI. HCV = Hepatitis C Virus. HIV = Human Immunodeficiency Virus. LGV = Lymphogranuloma venerum. #- Use professional discretion (i. e. screen based on prevalence of STIs in the countries recently visited). *- presence of one or more risk factors for STI/BBP.

Utility of the Screening Tool: • Used in concert with the STI Syndromic-based risk-assessment tool

STI Risk Assessment in Primary Care Settings Sexual health-related visit Presence of signs/symptoms Non-Sexual health-related visit No symptoms but concerns Brief risk assessment (See back of page) Risk identified No risk identified *Routine Asymptomatic screening Minimal prevention counseling Maintenance of safer practices Discussion of future risk avoidance Focused risk assessment Focused prevention counseling Syndromic management Testing/screening Treatment and partner follow-up

Testing Code Key

Survey Conclusion & Recommendations: v Of the Physicians, NPs and PHNs who participated in an implementation survey of the developed tools, (screening algorithm and clinical assessment tool): - 92% found them easy to use, - 46% found the algorithm cluttered - 100% rated the content as good to excellent, and Recommendations v Development of an accompanying STI risk-based client questionnaire v Creation of a partnership with e. Health to develop a province wide format for the Electronic Medical Records (EMR) system. v Have strategically located patient-specific posters or monitor displays, with appropriate STI prevention and control messages (especially risk factors), at waiting areas in physician offices and health clinics