Created by Joshua English EMTP James Pointer MD

Created by Joshua English, EMTP James Pointer, MD Mike Jacobs, EMT-P

Objectives • Understand why we use capnography • Understand the physiology of respiration/ ventilation • Define normal & abnormal Et. CO 2 values/ waveforms • Understand the 4 major applications of Et. CO 2 – intubated applications (mainstream) – non-intubated applications (sidestream)

Why Capnography? Advanced Airway Management (Policy #10102) All devices used to confirm tube placement must be documented on the PCR. • Esophageal Detection Device (EDD) • End tidal CO 2 detector (ETCO 2) colorimetric or capnography “Conclusion: No unrecognized misplaced intubations were found in patients for whom paramedics used continuous Et. CO 2 monitoring. Failure to use continuous Et. CO 2 monitoring was associated with a 23% unrecognized misplaced intubation rate. [Annals of Emergency Medicine 2005; 45: 497 -503]”

Why Capnography? • Verification of proper tube placement There is simply NO BETTER WAY to confirm proper tube placement than with waveform capnography…. PERIOD!!!

Why Capnography? Because respiration, ventilation and oxygenation are VERY different concepts.
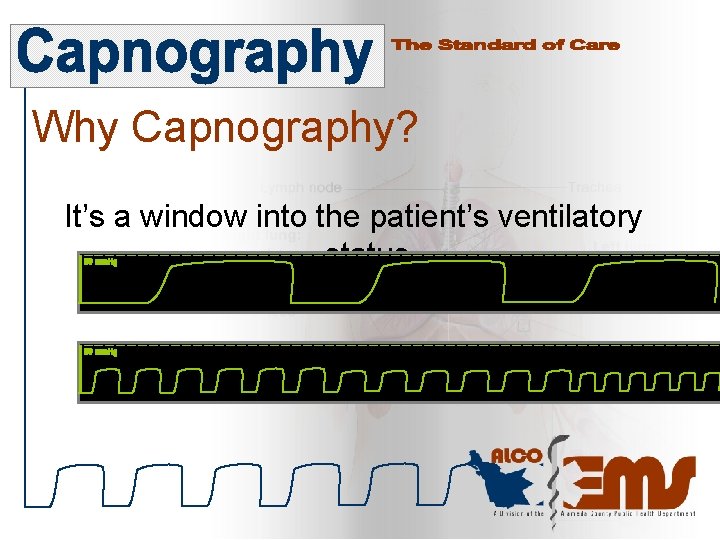
Why Capnography? It’s a window into the patient’s ventilatory status

Why Capnography? Core Concepts • What intubation verification method is most reliable? • How do oxygenation and ventilation differ?
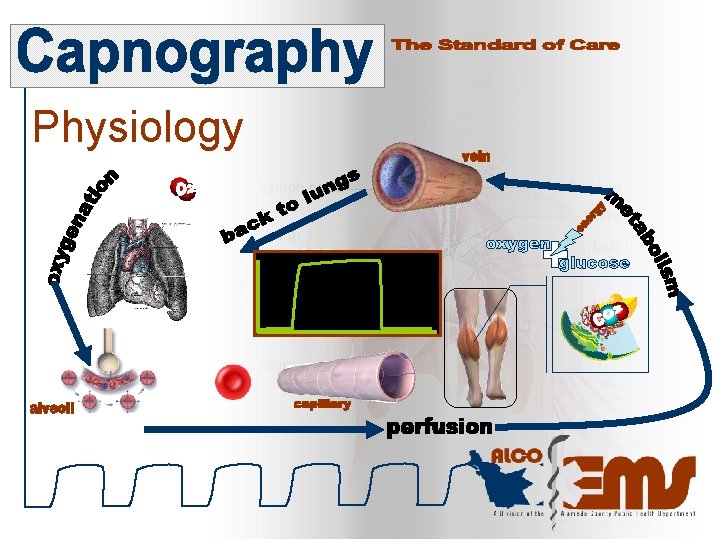
Physiology
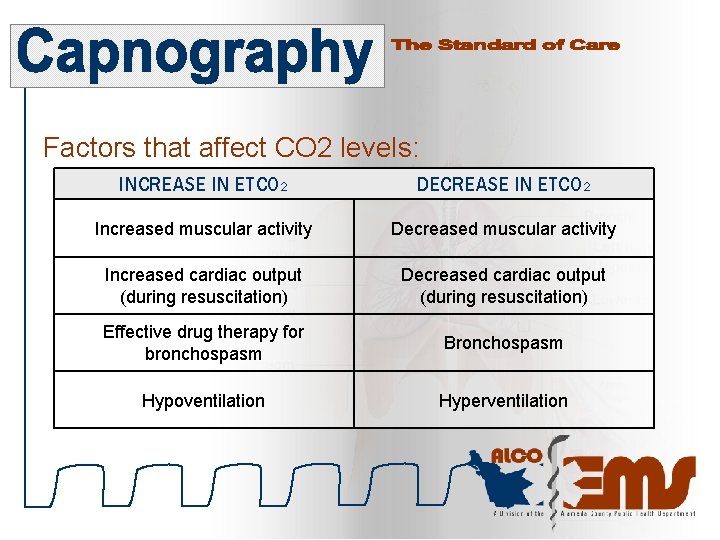
Factors that affect CO 2 levels: INCREASE IN ETCO 2 DECREASE IN ETCO 2 Increased muscular activity Decreased muscular activity Increased cardiac output (during resuscitation) Decreased cardiac output (during resuscitation) Effective drug therapy for bronchospasm Bronchospasm Hypoventilation Hyperventilation
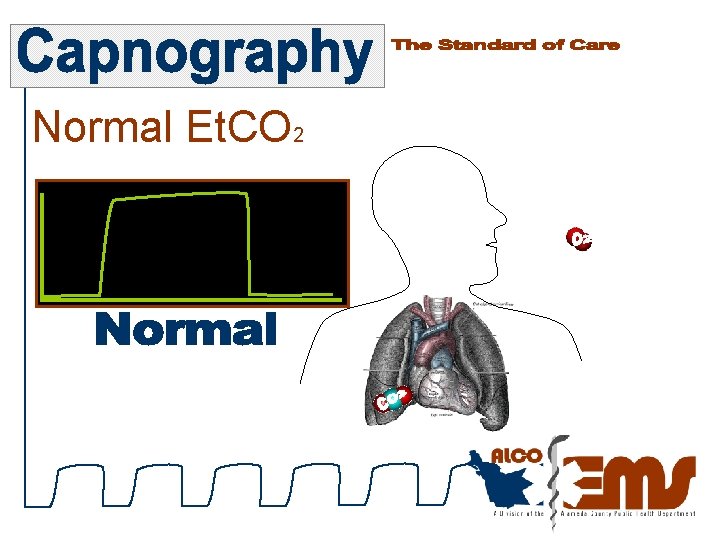
Normal Et. CO 2
Terminology Capnogram a real-time waveform record of the concentration of carbon dioxide in the respiratory gases Capnograph Capnogram waveform plus numerical value
Terminology Et. CO 2 – End Tidal CO 2 The measurement of exhaled CO 2 in the breath Normal Range | 35 -45 mm. Hg
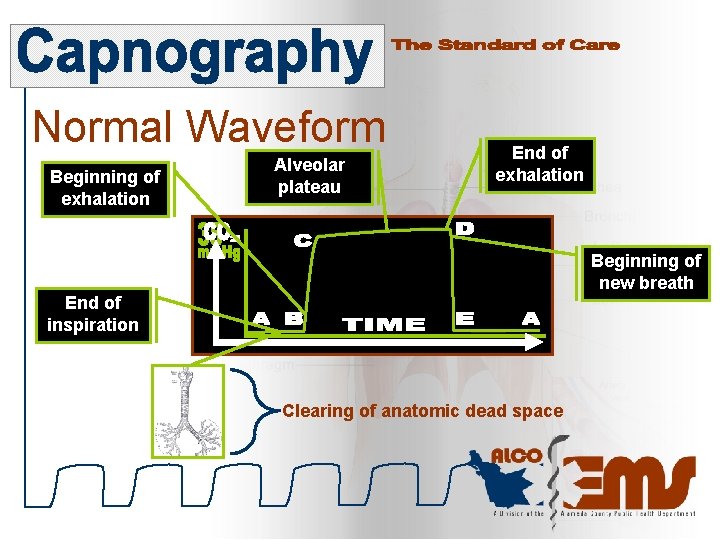
Normal Waveform Beginning of exhalation Alveolar plateau End of exhalation Beginning of new breath End of inspiration Clearing of anatomic dead space
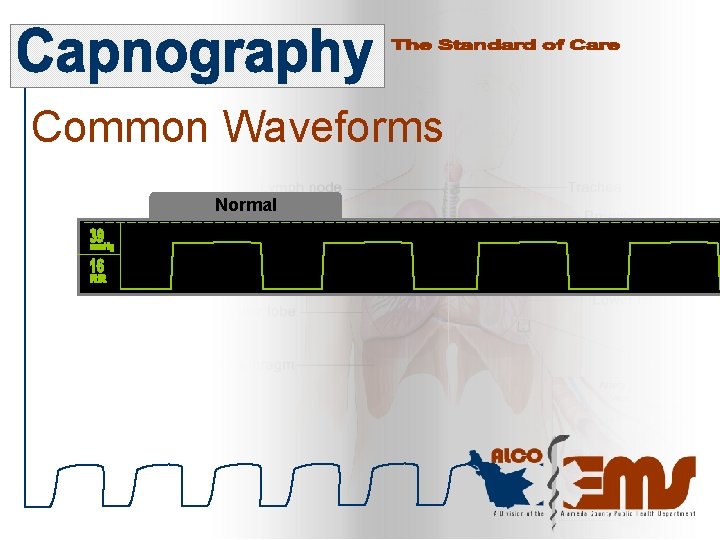
Common Waveforms Normal
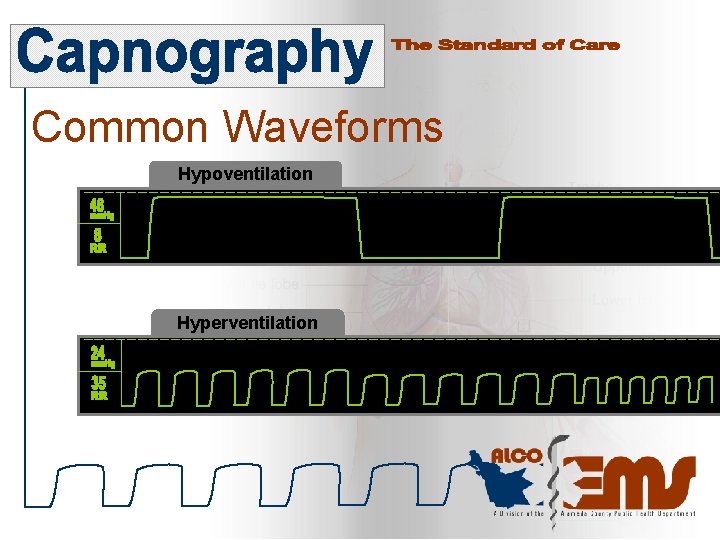
Common Waveforms Hypoventilation Hyperventilation

4 Main Uses of Capnography • • Severity of asthma patients Monitoring head injured patients Cardiac arrest Tube confirmation
Terminology Sidestream An indirect method of measuring exhaled CO 2 in non-intubated patients Mainstream Direct method of measuring exhaled CO 2 with intubated patients
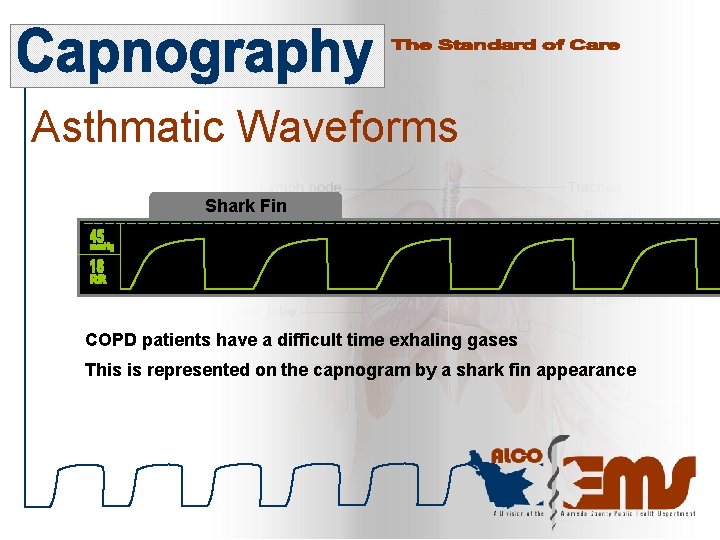
Asthmatic Waveforms Shark Fin COPD patients have a difficult time exhaling gases This is represented on the capnogram by a shark fin appearance
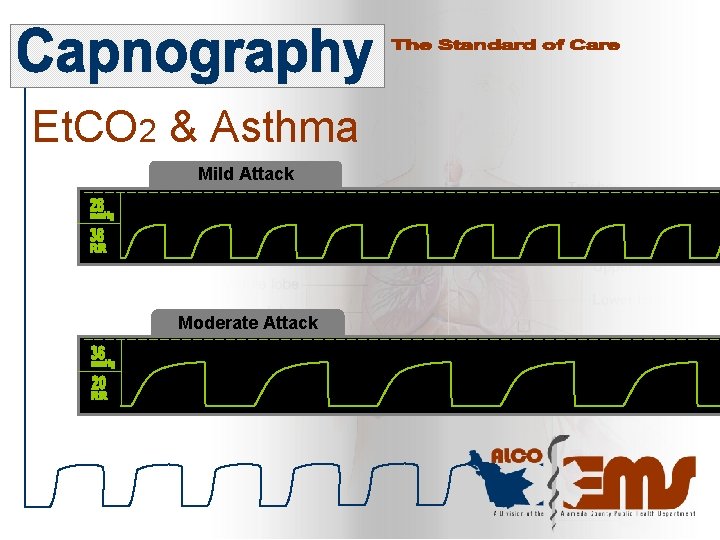
Et. CO 2 & Asthma Mild Attack Moderate Attack
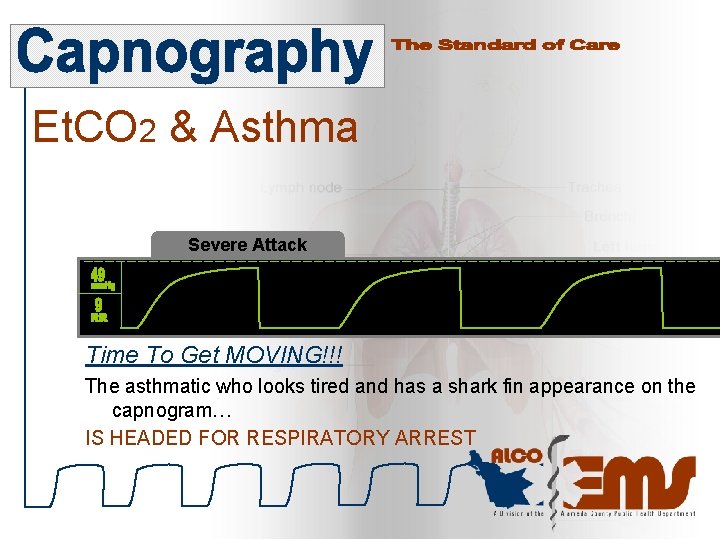
Et. CO 2 & Asthma Severe Attack Time To Get MOVING!!! The asthmatic who looks tired and has a shark fin appearance on the capnogram… IS HEADED FOR RESPIRATORY ARREST
The Head Injured Patient Carbon dioxide dilates the cerebral blood vessels, increasing the volume of blood in the intracranial vault and therefore increasing ICP Recognizing the head injured patient and titrating their CO 2 levels to the 30 -35 mm. Hg range can help relieve the untoward effects of ICP
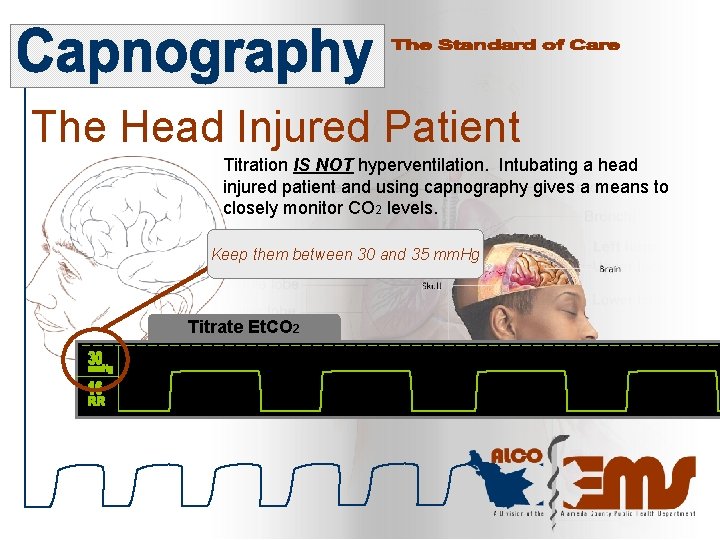
The Head Injured Patient Titration IS NOT hyperventilation. Intubating a head injured patient and using capnography gives a means to closely monitor CO 2 levels. Keep them between 30 and 35 mm. Hg Titrate Et. CO 2
Et. CO 2 and Cardiac Arrest The capnograph of an intubated cardiac arrest patient is a direct correlation to cardiac output Increase in CO 2 during CPR can be an early indicator of ROSC
Termination of Resuscitation Et. CO 2 measurements during a resuscitation give you an accurate indicator of survivability for patients under CPR Non-survivors Survivors (to discharge) <10 mm. Hg >30 mm. Hg

ET Tube Verification • Verification of proper tube placement There is simply NO BETTER WAY to confirm proper tube placement than with waveform capnography…. PERIOD!!!

4 Main Uses of Capnography Core Concepts • What is the characteristic shape of a capnogram for a COPD patient? • Describe how to determine the severity of an asthma attack using capnography? • What level should you maintain a severe head injured patient’s CO 2 at? • What are two ways that capnography can assist during CPR?
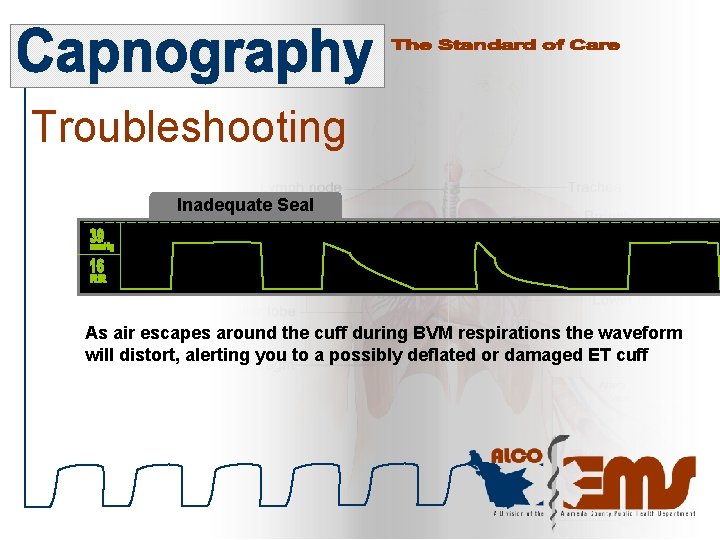
Troubleshooting Inadequate Seal As air escapes around the cuff during BVM respirations the waveform will distort, alerting you to a possibly deflated or damaged ET cuff
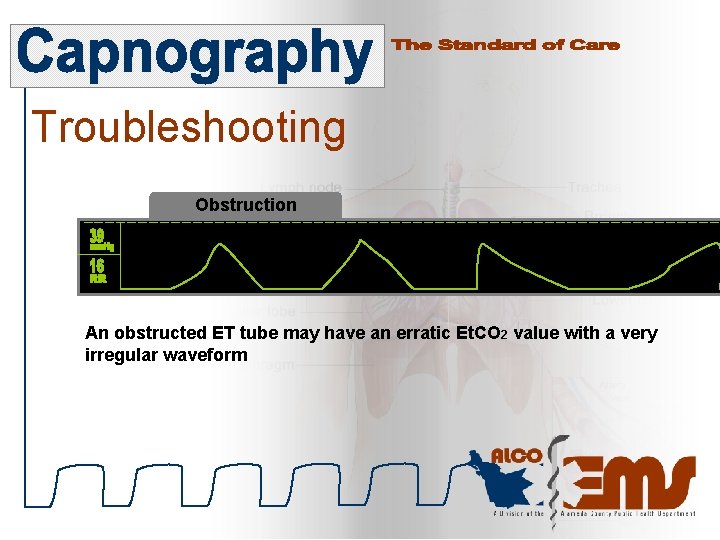
Troubleshooting Obstruction An obstructed ET tube may have an erratic Et. CO 2 value with a very irregular waveform
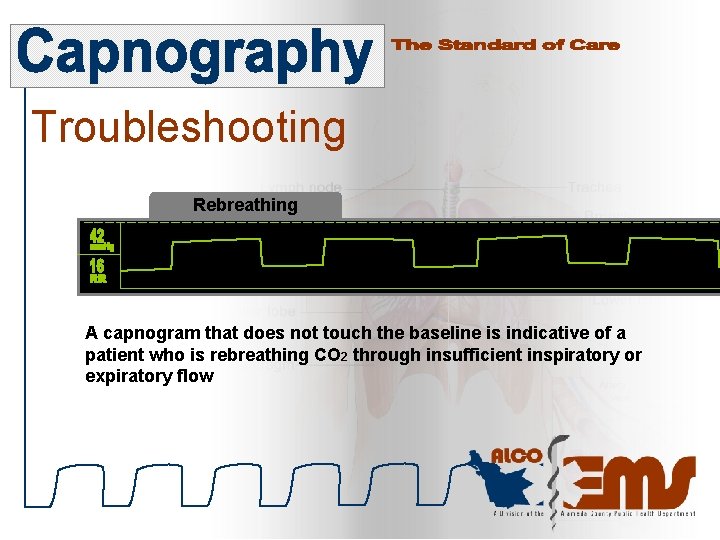
Troubleshooting Rebreathing A capnogram that does not touch the baseline is indicative of a patient who is rebreathing CO 2 through insufficient inspiratory or expiratory flow

QUIZ
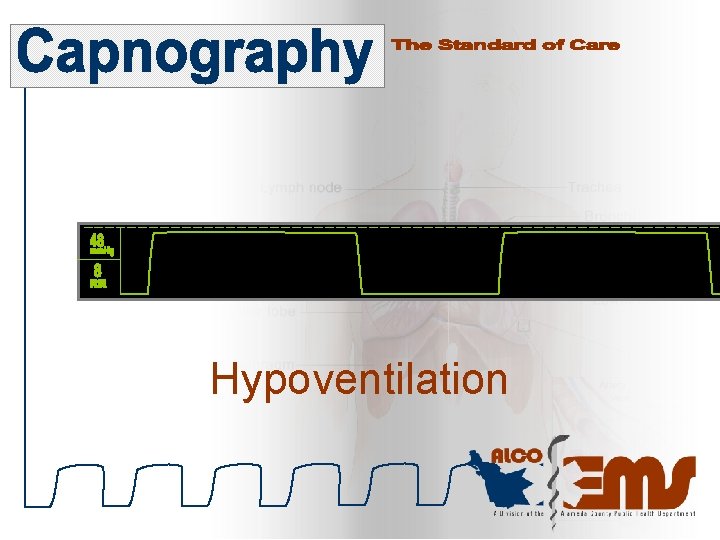
Hypoventilation
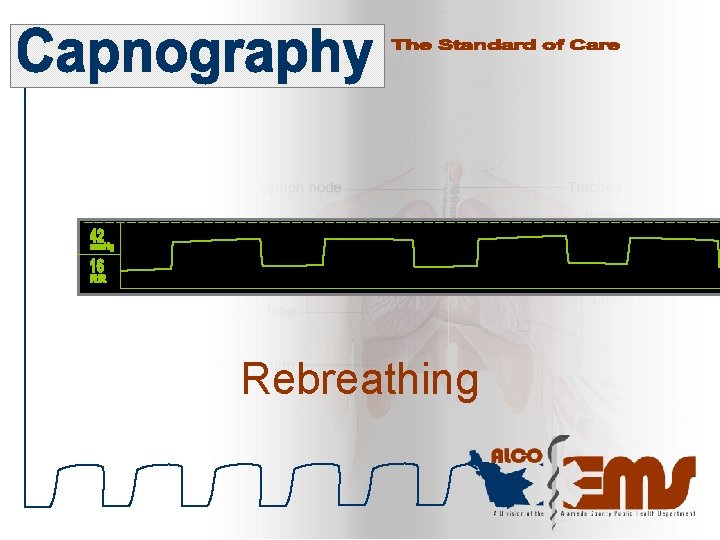
Rebreathing
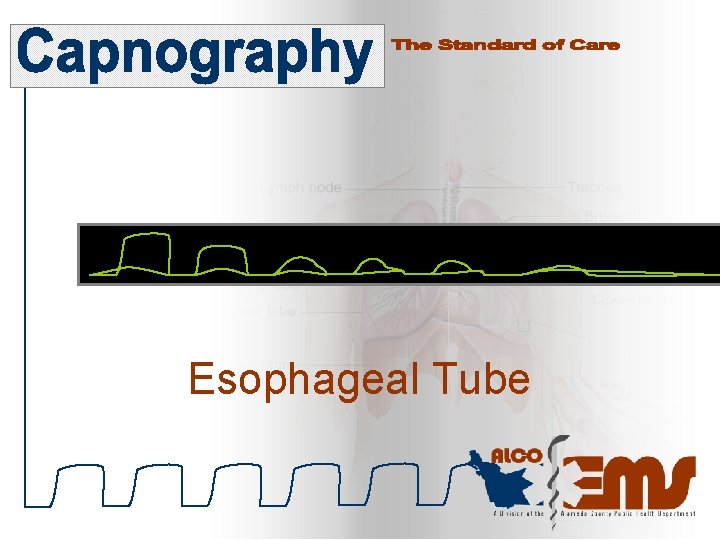
Esophageal Tube
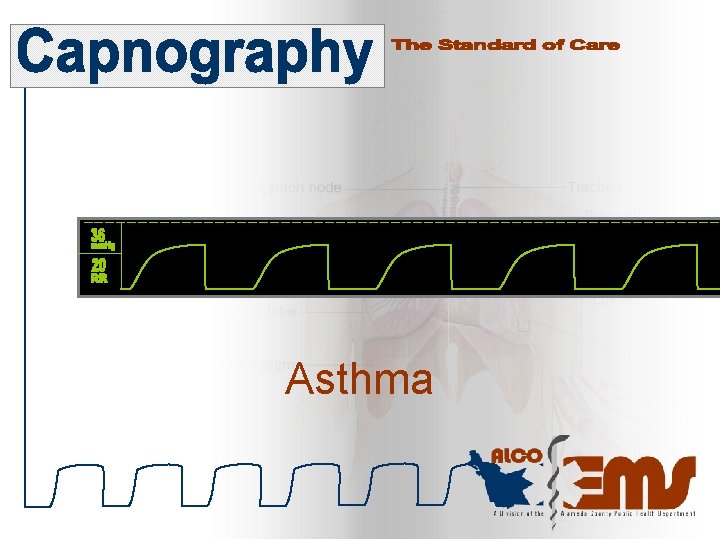
Asthma
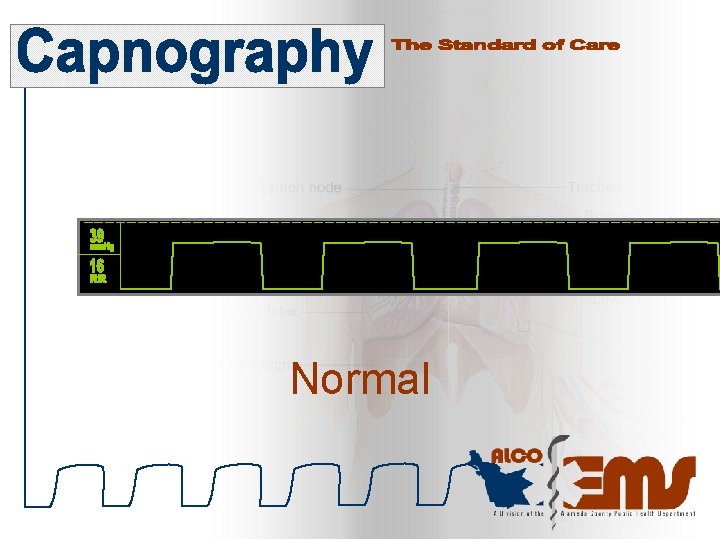
Normal

Questions?
- Slides: 36