CQCs approach to inspection and regulation of General




























- Slides: 35

CQC’s approach to inspection and regulation of General Practice Professor Nigel Sparrow OBE West Sussex Practice Managers Annual Conference 07 June 2018 1

Our purpose and role • We make sure health and social care services provide people with safe, effective, compassionate, high-quality care and we encourage care services to improve • • • Register Monitor and inspect Use legal powers Speak independently Encourage improvement • People have a right to expect safe, good care from their health and social care services 2

Our current model of regulation Register We register those who apply to CQC to provide health and adult social care services Monitor, inspect and rate We monitor services, carry out expert inspections, and judge each service, usually to give an overall rating, and conduct thematic reviews Enforce Where we find poor care, we ask providers to improve and can enforce this if necessary Independent voice We provide an independent voice on the state of health and adult social care in England on issues that matter to the public, providers and stakeholders 3

The landscape of care GP practices • 58. 9 m registered

What do the overall ratings mean? Outstanding The service is performing exceptionally well. Good The service is performing well and meeting our expectations. Requires improvement The service isn't performing as well as it should and we have told the service how it must improve. Inadequate The service is performing badly and we've taken action against the person or organisation that runs it. 5

Display of ratings A Provider Why? Public able to see rating of service quickly and easily Where? Providers should display in prominent area in public view and on website CQC will send a template for completion and display CQC will check this during inspections 6

Ambition Our ambition for the next five years: A more targeted, responsive and collaborative approach to regulation, so more people get high-quality care 7 7

Four priorities to achieve our strategic ambition 1. Encourage improvement, innovation and sustainability in care 2. Deliver an intelligence-driven approach to regulation 3. Promote a single shared view of quality 4. Improve our efficiency and effectiveness 8

The state of health care and adult social care 2016/17

Unique oversight of health and care • Full picture of the quality of health and social care in England, with ratings for all sectors • Now have a baseline from which to draw conclusions about quality and safety of care and what influences this • • 21, 256 adult social care services 152 NHS acute hospital trusts 197 independent acute hospitals 18 NHS community health trusts 54 NHS mental health trusts 226 independent mental health locations 10 NHS ambulance trusts 7, 028 primary medical care services • • • Is it safe? Is it effective? Is it caring? Is it responsive? Is it well-led? • Increasingly, CQC will report on quality of areas and coordination across services – for care fit for the 21 st century 10

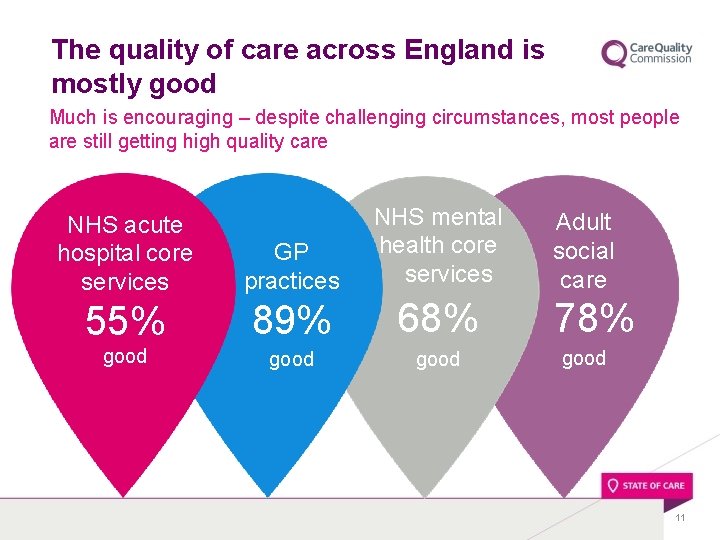
The quality of care across England is mostly good Much is encouraging – despite challenging circumstances, most people are still getting high quality care NHS acute hospital core services GP practices NHS mental health core services 55% 89% 68% good Adult social care 78% good 11

Improvement • Common factors leading to improvement: • Patient-centred care • Strong leadership • Positive culture • Shared vision • Outward looking approach • Involving people, communities, partners and collaborating Of those services originally rated inadequate, most have improved Adult Mental social GP Hospitals practices Health care 80% 100% 82% 12

Deterioration While recognising improvement, there is deterioration to be addressed Where services rated good were re-inspected, some have fallen NHS acute hospitals GP practices Mental health 18% Adult social care 2% 26% 23% fallen 13

Primary medical services regulation We will begin to implement changes in how we regulate primary medical services in phases. Change Timescale Introducing our new Insight model June 2017 New assessment framework introduced and inspection interval of up to five years for providers rated good or outstanding Nov 2017 Refined approach to inspecting and rating population groups Apr 2018 and introduction of shorter inspection reports Introducing the new system of provider information collections and annual regulatory reviews for good and outstanding services Shift to focused, rather than comprehensive inspections of good and outstanding services based on intelligence Spring 2019

How do we monitor services? • Our monitoring helps us to identify possible changes in quality of care and target our operational activity effectively. • Refers to all practices, but especially important now as we move to longer inspection intervals for those rated as good and outstanding • Our intelligence comes from a number of sources: National intelligence (GMC etc) Local intelligence (CCG, Healthwatch, surveys) Relationship with provider Monitor Provider information collection CQC Insight

Provider information collection (PIC) For Good and Outstanding providers the provider information collection will underpin our monitoring of changes in the quality of care (both positive and negative): • An annual online information collection to replace the existing provider information return • We will ask providers for information every year through an online system, approximately six weeks before we plan to formally review the information we hold on a practice • Provider information collection will give practices an opportunity to champion the quality of care they are providing 16

Annual regulatory review (ARR) process • For Good and Outstanding providers we will introduce an annual regulatory review process to bring structure to our monitoring. • Every year inspectors will formally review the information they hold on each practice and consider whethere any indications of substantial changes (good or bad) in the quality of care since our last inspection. • This process will inform the scheduling of inspections and defining their focus. If we decide not to take any action, we will tell the practice we have carried out the review and update our website. Neither the PIC nor the ARR can change a practice rating, this can only happen following an inspection. 17

How will our inspections change? Frequency of inspection: • Practices rated Inadequate would be re-inspected after six months; • Requires Improvement within 12 months; • Good or Outstanding would move to an inspection interval of up to five years, although every year we will inspect a proportion. Scope: • Comprehensive inspections for providers rated Inadequate or those not inspected before • Providers rated Good and Outstanding most inspections will be focused – based on the intelligence we hold on a practice. These inspections will always look at effective and well-led as a minimum. 18

How will those inspections change? Continued Inspection team: • Continue to use specialist advisors in our inspections • More efficient use of Experts by Experience (Ex. E) • For example – gathering evidence using telephone calls rather than on site visits Notice periods • Increased flexibility including short notice and unannounced • Emphasis – more on the quality of care provided including population groups and conditions; less on policies and risk assessments 19

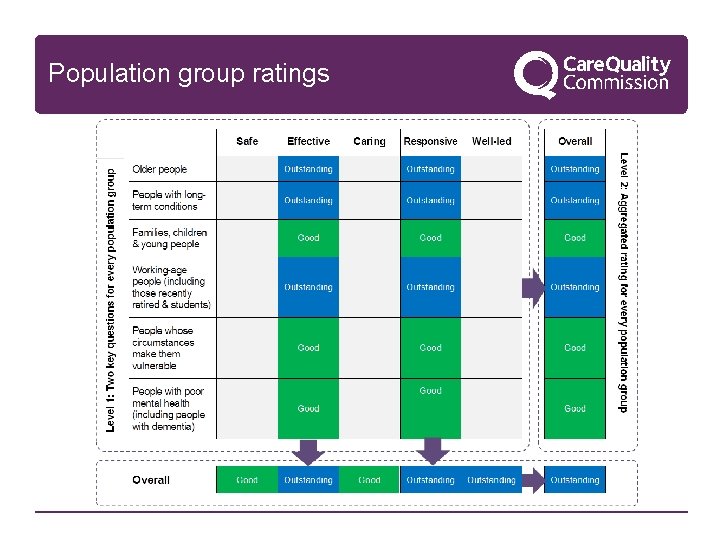
Key changes to ratings and reporting Content • Shorter summary report supported by an evidence table (from April 2018) Publishing reports • Commitment to publishing 90% within 50 days of inspection Updating ratings • Only changed on the basis of evidence from inspections • Six month limit for aggregating ratings dropped Population groups • We will only rate the six population groups for effective, responsive and overall – more focus on evidence and the components of good quality care for these six groups 20

Population group ratings

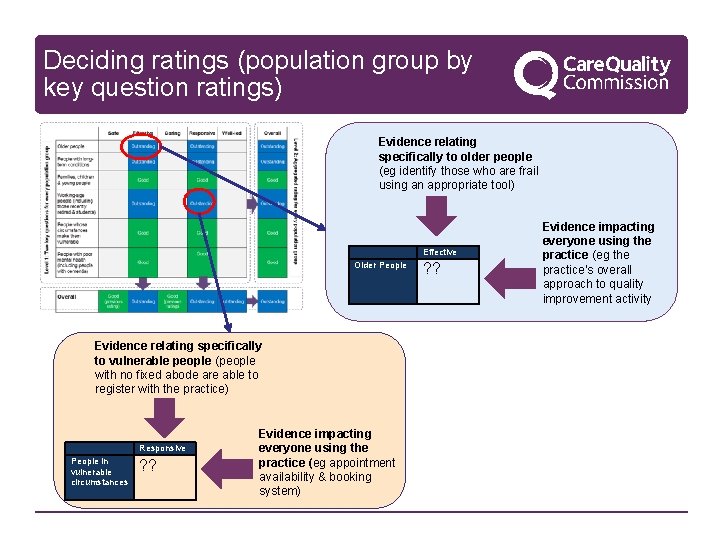
Deciding ratings (population group by key question ratings) Evidence relating specifically to older people (eg identify those who are frail using an appropriate tool) Older People Evidence relating specifically to vulnerable people (people with no fixed abode are able to register with the practice) People in vulnerable circumstances Responsive ? ? Evidence impacting everyone using the practice (eg appointment availability & booking system) Effective ? ? Evidence impacting everyone using the practice (eg the practice’s overall approach to quality improvement activity

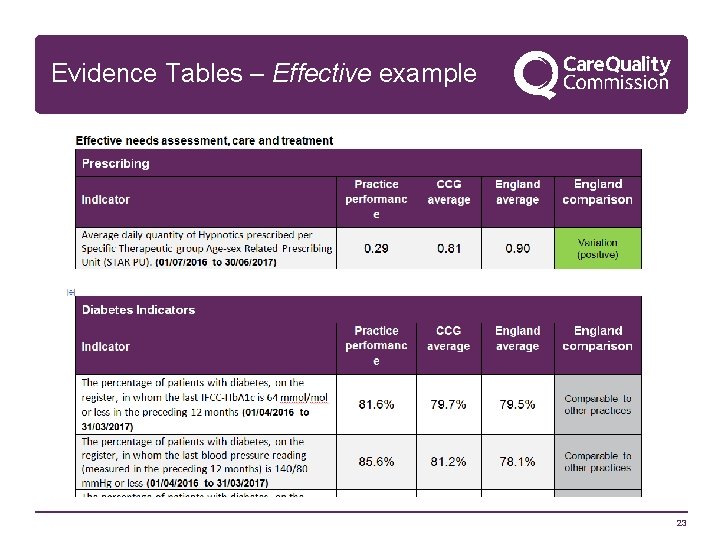
Evidence Tables – Effective example 23

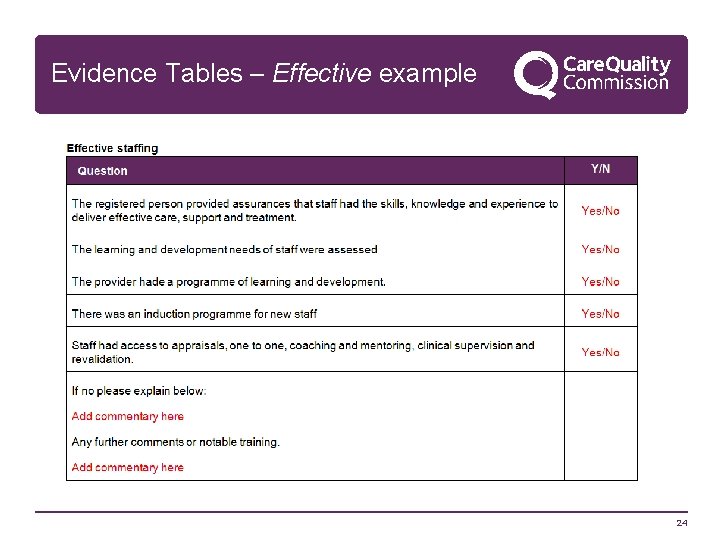
Evidence Tables – Effective example 24

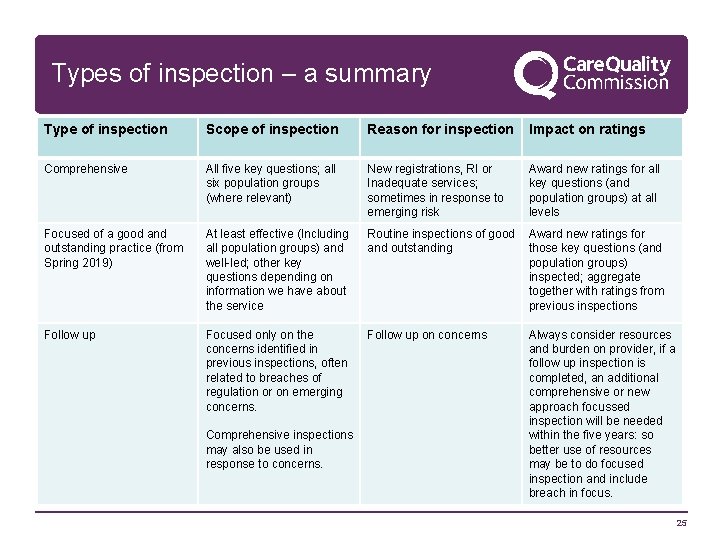
Types of inspection – a summary Type of inspection Scope of inspection Reason for inspection Impact on ratings Comprehensive All five key questions; all six population groups (where relevant) New registrations, RI or Inadequate services; sometimes in response to emerging risk Award new ratings for all key questions (and population groups) at all levels Focused of a good and outstanding practice (from Spring 2019) At least effective (Including all population groups) and well-led; other key questions depending on information we have about the service Routine inspections of good Award new ratings for and outstanding those key questions (and population groups) inspected; aggregate together with ratings from previous inspections Follow up Focused only on the concerns identified in previous inspections, often related to breaches of regulation or on emerging concerns. Follow up on concerns Comprehensive inspections may also be used in response to concerns. Always consider resources and burden on provider, if a follow up inspection is completed, an additional comprehensive or new approach focussed inspection will be needed within the five years: so better use of resources may be to do focused inspection and include breach in focus. 25

To summarise • Maximum five year inspection intervals for most • Closer working relationship with named inspector at CQC • More proportionate action - not only inspection • Increased emphasis on patient outcomes • A simpler process for low risk registration changes • More timely information about a provider’s performance 26

GP improvement report due to come out in June 2018 27

Driving improvement: Case studies from 10 GP practices • Case studies looking at the improvement journey of 10 practices • Encourage improvement by showcasing good and outstanding practice and celebrating where services have made improvements. Key themes • Importance of leadership – clinical leadership as well as an empowered practice manager • Avoiding professional isolation – practices should not hesitate to ask for support, locally or nationally • Value of a practice working as a team – working as a multidisciplinary model, recognising the value of nursing teams. 28

Outstanding characteristics • Easy to access appointments and services through several communication channels • Good and effective leadership extends beyond the manager and those values are cascaded to inspire staff • Staff training and support • Open culture – people who use services/ staff/ relatives shared views and issues • Strong links with local community • Working with multi-professional colleagues and from other organisations • Support patients and carers with emotional needs • Services empowering patients to self manage long-term conditions 29

Inadequate characteristics • Weak leadership, Chaotic and disorganised environment • Isolated working, not involving other local providers to share learning and best practice • A lack of vision for the organisation and clarity around individuals’ roles and responsibilities • A poor culture of safety and learning ie. lack of learning from complaints/events analysis • Poor systems for quality improvement • Disregard for HR processes ie. DBS checks • Unsafe medicines management • Low/insufficient practice nurses or sessions

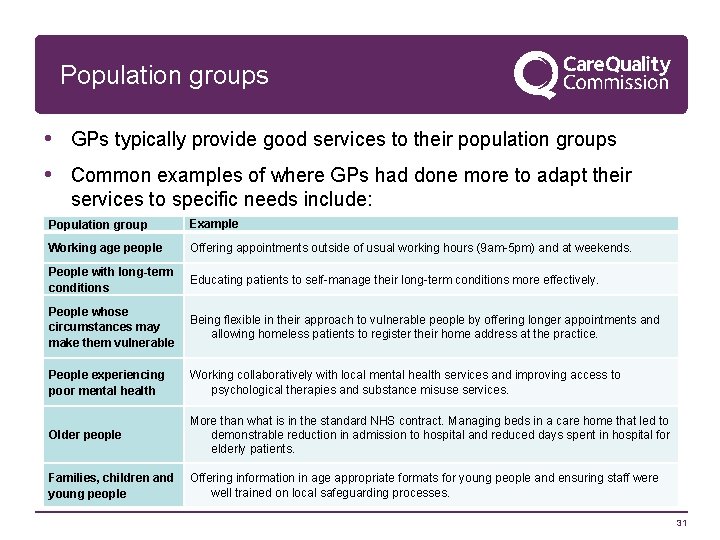
Population groups • GPs typically provide good services to their population groups • Common examples of where GPs had done more to adapt their services to specific needs include: Population group Example Working age people Offering appointments outside of usual working hours (9 am-5 pm) and at weekends. People with long-term conditions Educating patients to self-manage their long-term conditions more effectively. People whose circumstances may make them vulnerable Being flexible in their approach to vulnerable people by offering longer appointments and allowing homeless patients to register their home address at the practice. People experiencing poor mental health Working collaboratively with local mental health services and improving access to psychological therapies and substance misuse services. Older people More than what is in the standard NHS contract. Managing beds in a care home that led to demonstrable reduction in admission to hospital and reduced days spent in hospital for elderly patients. Families, children and young people Offering information in age appropriate formats for young people and ensuring staff were well trained on local safeguarding processes. 31

Find out more • Read the monthly bulletin for primary care providers • Sent to all providers and registered managers, or sign up through our website • Join our provider and public online communities • Visit our new guidance page for GP practices www. cqc. org. uk/gpintroguide Find all of the above and more at: www. cqc. org. uk/GPProvider 32

Helpful resources for practices ü Make sure you’ve read our provider handbook, and understand the key lines of enquiry our inspectors will focus on ü Read our mythbusters for tips and further guidance ü Read our outstanding practice web tool kit and consider what would make care for people who use your services outstanding ü Read our ‘What to expect from an inspection’ and case studies to understand what an inspection looks and feels like We’ve signposted all of these resources and more in our provider toolkit. Simply visit: www. cqc. org. uk/GPProvider 33

Support for poor performing practices What happens when a practice enters special measures? • We will inform the NHS clinical commissioning group, and NHS area team • The Royal College of GPs provides peer support to practices, using a local turnaround team • The RCGP helps practices identify and deliver an improvement plan 34

Thank you www. cqc. org. uk enquiries@cqc. org. uk @Care. Quality. Comm 35