COVID 19 Katherine West RN BSN MSEd Infection

COVID - 19 Katherine West, RN, BSN, MSEd Infection Control Consultant

Novel Coronavirus COVID-19 • A new coronavirus • China – 2019 • Animal to human transmission • Human to human transmission • Viral illness • Only seriously ill develop pneumonia - ? • First U. S. Case – Washington State -? 2

Causative Organism • SARS Co. V -2 Virus
Fever Signs & Symptoms Cough Tightness in chest Shortness of breath Newly added: Headache, sore throat, chills, loss of sense of smell or taste, muscle pain 4

Risk Groups • CDC, March 9, 2020 • Older adults • People who have serious chronic medical conditions like: • Heart disease • Diabetes • Lung disease • Immunocompromised – any age • All age groups

Close Contact Redefined – CDC • CDC Updated the definition of “prolonged” close contact • 15 MINUTES OR MORE – refers to the cumulative amount of time a person is exposed to one or more individuals with COVID-19 during a 24 hour time frame

Mode of Transmission Respiratory – droplet precautions (WHO/CDC) Contact Precautions – (WHO/CDC)

Conflicting statements from CDC

CDC Transmission Mixing droplet and airborne What does that mean ?

CDC Clarifies – Airborne Transmission • • Airborne transmission of SARS-Co. V-2 can occur under special circumstances • Pathogens that are mainly transmitted through close contact (i. e. , contact transmission and droplet transmission) can sometimes also be spread via airborne transmission under special circumstances. • Enough virus was present in the space to cause infections in people who were more than 6 feet away or who passed through that space soon after the infectious person had left. CDC, Oct. 5, 2020

Circumstances under which airborne transmission of SARS-Co. V -2 appears to have occurred include: • Enclosed spaces within which an infectious person either exposed susceptible people at the same time or to which susceptible people were exposed shortly after the infectious person had left the space. • Prolonged exposure to respiratory particles, often generated with expiratory exertion (e. g. , shouting, singing, exercising) that increased the concentration of suspended respiratory droplets in the air space. • Inadequate ventilation or air handling that allowed a build -up of suspended small respiratory droplets and particles. CDC, October 5, 2020

Incubation Period • 2 - 14 days after exposure • Change to 4 – 5 - days (12/2/2020)

Testing Issues Doctors order may be needed for insurance coverage

Types of Testing Antigen – looking for the virus Antibody – to identify who has had the virus
Testing Antigen - Virus Antibody • Current infection – • Past infection - CDC's guidance concludes antibody tests should not be used at this time “to determine immune status in individuals • False negatives • False positives

CDC – Feb. 28, 2020 • Patient wearing a facemask which can efficiently block respiratory secretions from contaminating others and the environment • Basic infection control – contain at the source!
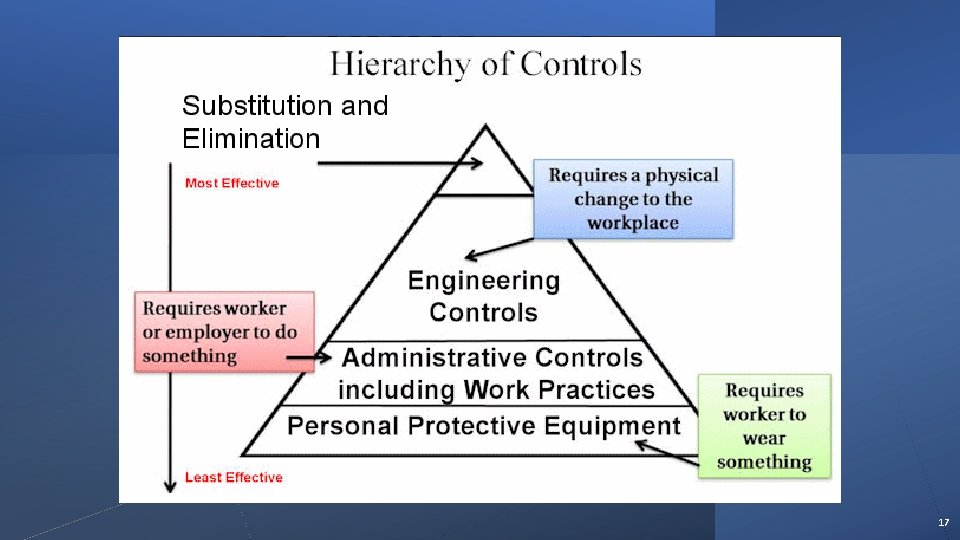
17

Interim Guidance for Emergency Medical Services (EMS) Systems and 911 Public Safety Answering Points (PSAPs) for COVID-19 in the United States Updated July, 15, 2020

Interim EMS Guidelines – COVID-19 • CDC – Review EMS guidelines to decide PPE to be used

• Community Transmission • No to minimal community transmission: Evidence of isolated cases or limited community transmission, case investigations underway; no evidence of exposure in large communal setting • Minimal to moderate community transmission: Sustained transmission with high likelihood or confirmed exposure within communal settings and potential for rapid increase in cases This is Where You Begin ! • Substantial community transmission: Large scale community transmission, including communal settings (e. g. , schools, workplaces) CDC EMS Guidelines, July 15, 2020 pg. 13 20

EMS personnel working in areas with moderate to substantial community transmission • Wear eye protection in addition to their facemask to ensure the eyes, nose, and mouth are all protected from splashes and sprays of infectious material from others. • Wear an N 95 or equivalent or higher-level respirator, instead of a facemask, for: • Aerosol generating procedures • Respirators with exhalation valves are not recommended for source control.

EMS personnel working in areas with minimal to no community transmission, • Universal eye protection and respirator recommendations described for areas with moderate to substantial community transmission are optional. • Universal use of a facemask for source control is recommended for EMS personnel.

New Guidelines Dispatch • To advise callers to wear masks prior to EMS arrival

New Screen Ask Implement Screen all staff & Visitors for symptoms Ask if they have been advised to self quarantine Implement source control • Dispatch should advise that patient and family wear masks before EMS arrives July 15, 2020 - CDC 24

Environmental Controls Insuring proper ventilation (exhaust fan) Environmental cleaning – standard disinfectant agents

NIOSH Statement • Engineering controls with regard to COVID-19 would include the use of HVAC systems in a vehicle. A recent NIOSH study showed that particle clearance could be improved by the use of the rear vent fan (when positioned on the “high” setting) in conjunction with the provision of outside air through the vehicle’s main HVAC systems. CDC Interim Guidelines for EMS 26

Return to Work Guidelines • HCP with mild to moderate illness who are not severely immunocompromised: • At least 10 days have passed since symptoms first appeared and • At least 24 hours have passed since last fever without the use of feverreducing medications and • Symptoms (e. g. , cough, shortness of breath) have improved CDC, July 15, 2020

Cleaning for COVID-19 • Nothing special is needed • Any EPA approved disinfectant

Cleaning / Disinfection Routine cleaning and disinfection procedures (e. g. , using cleaners and water to pre-clean surfaces prior to applying an EPA-registered, hospital-grade disinfectant to frequently touched surfaces or objects for appropriate contact times as indicated on the product’s label) are appropriate for SARSCo. V-2 (the virus that causes COVID-19) in healthcare settings, including those patient-care areas in which aerosolgenerating procedures are performed. CDC Interim Guidelines for EMS

Cleaning High Touch Areas • Clean and disinfect the vehicle in accordance with standard operating procedures. All surfaces that may have come in contact with the patient or materials contaminated during patient care (e. g. , stretcher, rails, control panels, floors, walls, work surfaces) should be thoroughly cleaned and disinfected using an EPA-registered hospital grade disinfectant in accordance with the product label.

This question is a key one to ask when evaluating the purchase of any automated disinfection system. Importance of Cleaning ! This question was recently answered by Dr. William Rutala a nationally recognized expert in disinfection and sterilization. In an interview for Healthcare Hygiene Magazine, January, 2020, Dr. Rutala stated: “ the rationale for rigorous manual cleaning/disinfection before use of UV technology, for example, is that organic material can interfere with disinfection technologies. Thus, surfaces must be cleaned/disinfected prior to use of automated disinfection technology. ” 31

Respiratory Protection • Surgical mask Vs. N 95’s • Depends on risk category • CDC EMS Interim Guidelines
PPE • • Gloves – double gloves are not needed Cover gown or coveralls Protective eyewear Surgical masks/ respirators (AGPs)


Define Exposure 35

• Risk Assessment - Patient s/s and duration of exposure Exposure • High Risk – HCP performed or were present when AGPs were performed on patients with COVID-19 without use of PPE • Medium Risk – prolonged close contact with COVID-19 patients and HCP hands or mucous membranes were exposed 36

• Pre-Screen: Employers should measure the employee’s temperature and assess symptoms prior to them starting work. Ideally, temperature checks should happen before the individual enters the facility. Post Exposure Asymptomatic • Regular Monitoring: As long as the employee doesn’t have a temperature or symptoms, they should self-monitor under the supervision of their employer’s occupational health program. • Wear a Mask: The employee should wear a face mask at all times while in the workplace for 14 days after last exposure. Employers can issue facemasks or can approve employees’ supplied cloth face coverings in the event of shortages. • Social Distance: The employee should maintain 6 feet and practice social distancing as work duties permit in the workplace. • Disinfect and Clean work spaces: Clean and disinfect all areas such as offices, bathrooms, common areas, shared electronic equipment routinely.

Signs & Symptoms • If the employee becomes sick during the day, they should be sent home immediately. • Surfaces in their workspace should be cleaned and disinfected. Information on persons who had contact with the ill employee during the time the employee had symptoms and 2 days prior to symptoms should be compiled. Others at the facility with close contact within 6 feet of the employee during this time would be considered exposed. CDC

Work Restriction • CDC EMS Interim Guidelines • EMS agencies should develop sick-leave policies for EMS personnel that are nonpunitive, flexible, and consistent with public health guidance. Ensure all EMS personnel, including staff who are not directly employed by the healthcare facility but provide essential daily services, are aware of the sick-leave policies.

Quarantine 40

Questions from the Infection Control Community Substitutions, alternatives, reuse and reprocessing of gowns, goggles, and masks/respirators to conserve supplies Accessing PPE for patients receiving care at home • Education of staff and patients to prevent misuse and overuse of PPE
Income loss – 14 days Unresolved Issues Quarantine Getting groceries Getting medications

CDC – Statement of Shortage of N 95 s • Interim Infection Prevention and Control Recommendations for Patients with Suspected Coronavirus Disease 2019 – • Update PPE – “Based on local and regional situational analysis of PPE supplies, facemasks are an acceptable alternative when the supply chain of respirators cannot meet the demand” CDC, March 10, 2020/ July 15, 2020

Center for Medicare & Medicaid Services • “today’s CMS memo implements CDC guidance by stating that facemasks are an acceptable temporary alternative to respirator”… • CMS, March 11, 2020

FDA Statement of Masks Shortages • If Surgical Masks and/or Gowns Are Running Low: • • • Extend the use of single use gowns for healthcare providers without changing the gown between patients with the same infectious disease diagnosis or exposure who are maintained in a confined area. If the gown becomes contaminated, replace it. Use surgical masks and/or gowns that meet CDC recommendations and/or ANSI standards for fluid resistance and bacterial filtration efficiency. Prioritize the use of unexpired FDA-cleared surgical masks for healthcare providers in procedures where it is important to protect the healthcare provider and/or the patient from risk of exposure to blood and body fluids. • Use surgical masks beyond the manufacturer-designated shelf life in a setting where there is a lower risk of transmission(e. g. , non-surgical). The user should visibly inspect the product prior to use and, if there are concerns (such as degraded materials or visible tears), discard the product. • Re-use surgical masks during care for multiple patients where they are used to protect the healthcare provider from an activity with low transmission risk (such as dispensing medications) and thus do not create a risk to the healthcare provider or patient. If the mask becomes contaminated, replace it. • Be aware that counterfeit masks and gowns may be on the market, especially during this time of reduced supply. FDA, March 11, 2020

Vaccines – as of Nov. 17, 2020 • 2 promising vaccines with 90% - 95% effectiveness • Need peer review of testing data • Require 2 doses • Storage at – 70 - -90 degrees (special refrigerators =$10, 000 each • Special glass for vials that can withstand that low temperature • Distribution plan


Questions ? 703 -365 -8388 info@ic-ec. com
- Slides: 48