COVID 19 Assessing the Risks A webinar for

COVID 19 - Assessing the Risks A webinar for Primary Care Thursday 9 th July 2020 10 am-11. 30 am NHS England NHS Improvement

10: 00 -10: 05 Opening Remarks Dr Jo Sauvage FRCGP Chair, NHS North Central London CCG Jo has been a GP in Old Street, London since 1999 and has always been committed to supporting education & staff development, including offering work experience in GP to local young people as a means of broadening opportunities to understand careers in the NHS. She is Clinical Lead for Workforce across North London Partners in Health & Care and an advocate for collaborative multi-disciplinary education, to supporting learning together when working together across health & social care. Jo is now Chair of NHS North Central London CCG & is Clinical Commissioner representative on our newly formed London People Board. As London Region representative on the board of NHS Clinical Commissioners since 2017, she is working to inform the NHS Confederation ‘Reset’ on Workforce for the future. NHS England NHS Improvement.

10: 00 -10: 05 Opening Remarks Dr Nikki Kanani Medical Director for Primary Care, NHS England NHS Improvement (NHSE/I) Dr Nikki Kanani is a GP in south-east London and is currently Medical Director for Primary Care for NHS England NHS Improvement. Prior to joining NHS England as Deputy Medical Director of Primary Care, she was Chief Clinical Officer of NHS Bexley Clinical Commissioning Group (CCG). Nikki has held a range of positions within healthcare to support the development of innovative models of care, highly engaged clinical, patient and public leadership and is passionate about supporting primary care, improving service provision and population wellbeing. She is a member of The King's Fund General Advisory Council and holds a MSc in health care commissioning. With her sister she co-founded STEMMsisters, a social enterprise supporting young people to study science, technology, engineering, maths and medicine. She has two young children. NHS England NHS Improvement
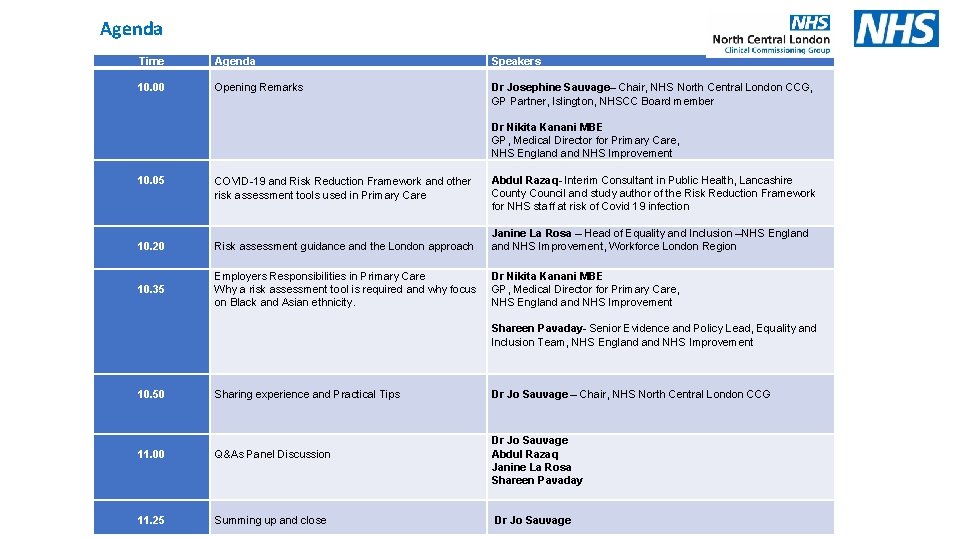
Agenda Time 10. 00 Agenda Opening Remarks Speakers Dr Josephine Sauvage– Chair, NHS North Central London CCG, GP Partner, Islington, NHSCC Board member Dr Nikita Kanani MBE GP, Medical Director for Primary Care, NHS England NHS Improvement 10. 05 COVID-19 and Risk Reduction Framework and other risk assessment tools used in Primary Care 10. 20 Risk assessment guidance and the London approach Janine La Rosa – Head of Equality and Inclusion –NHS England NHS Improvement, Workforce London Region 10. 35 Employers Responsibilities in Primary Care Why a risk assessment tool is required and why focus on Black and Asian ethnicity. Dr Nikita Kanani MBE GP, Medical Director for Primary Care, NHS England NHS Improvement Abdul Razaq- Interim Consultant in Public Health, Lancashire County Council and study author of the Risk Reduction Framework for NHS staff at risk of Covid 19 infection Shareen Pavaday- Senior Evidence and Policy Lead, Equality and Inclusion Team, NHS England NHS Improvement 10. 50 Sharing experience and Practical Tips Dr Jo Sauvage – Chair, NHS North Central London CCG 11. 00 Q&As Panel Discussion Dr Jo Sauvage Abdul Razaq Janine La Rosa Shareen Pavaday 11. 25 Summing up and close Dr Jo Sauvage

Aims of this session • To explore and share how risks to staff are being assessed during the COVID 19 • Understand how best to undertake risk assessments in a way to engage and support staff in primary care • Consider what GP Partners/Employers/Practice Managers can do for their workforce: - Amplify and value their voice - Building trustworthy working environment - Increase sense of belonging NHS England NHS Improvement

10: 05 -10: 20 COVID-19 and Risk Reduction Framework and other risk assessment tools used in Primary Care Abdul Razaq Consultant in Public Health, Lancashire County Council Abdul Razaq has formerly held positions as Director of Public Health for fifteen years and has extensive senior executive Public Health experience in the NHS and local government in the UK. Abdul is the lead author of the CEBM BAME COVID deaths rapid review published 5 th May 2020 and a co-author of the NHS Risk Reduction Framework. He is currently Consultant in Public Health at Lancashire County Council and Visiting Senior Fellow, University of Suffolk. He is a member of the UK Faculty of Public Health Special Interest Group on Pakistan and is a Fellow of the UK Faculty of Public Health. NHS England NHS Improvement

10: 20 -10: 35 Risk Assessment Guidance and the London Approach Janine La Rosa Head of Equality and Inclusion–NHS E/I Workforce London Janine has led inclusive cultural transformation in organisations across the public, private and third sectors and is well-regarded ED&I Subject Matter Expert. She is the co-chair of the Pan London EDI network. Janine the team in May on secondment. She started in her substantive role as Deputy Director of Development at NELCSU in 2017. Leading the ED&I, OD and L&D teams she has focused on embedding a high performing and inclusive culture aligned with NHS values and delivering services that have a demonstrable and meaningful impact across the Health and Social Care system. Before moving into Culture and OD Janine’s background was management consultancy and project and programme management. She has delivered and led key strategic and high value projects at PA Consulting, BT and BSky. B. NHS England NHS Improvement
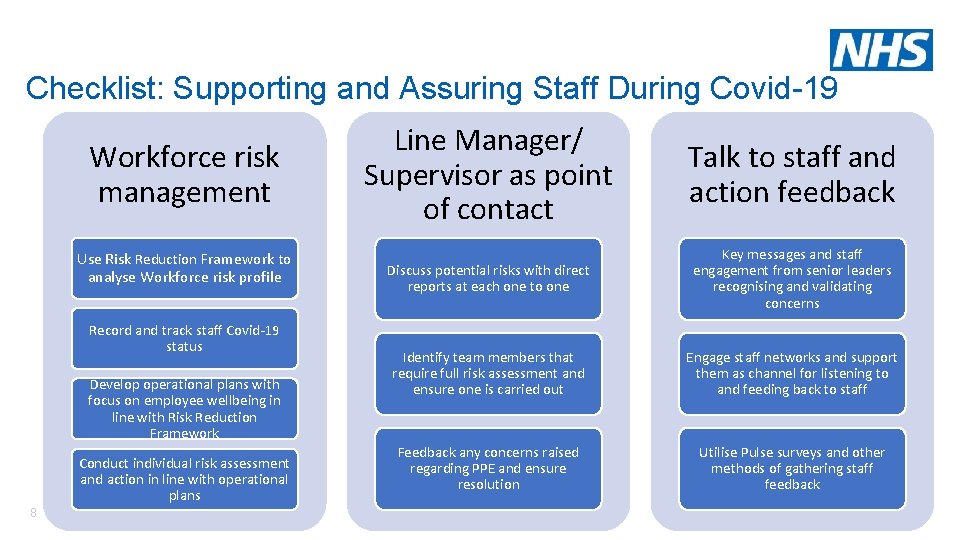
Checklist: Supporting and Assuring Staff During Covid-19 Workforce risk management Use Risk Reduction Framework to analyse Workforce risk profile Record and track staff Covid-19 status Develop operational plans with focus on employee wellbeing in line with Risk Reduction Framework Conduct individual risk assessment and action in line with operational plans 8 | Line Manager/ Supervisor as point of contact Talk to staff and action feedback Discuss potential risks with direct reports at each one to one Key messages and staff engagement from senior leaders recognising and validating concerns Identify team members that require full risk assessment and ensure one is carried out Engage staff networks and support them as channel for listening to and feeding back to staff Feedback any concerns raised regarding PPE and ensure resolution Utilise Pulse surveys and other methods of gathering staff feedback
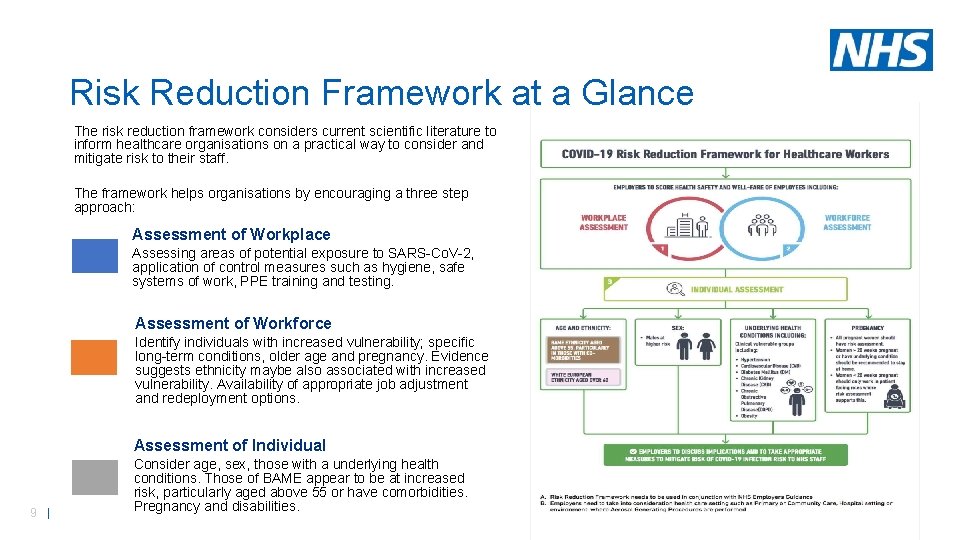
Risk Reduction Framework at a Glance The risk reduction framework considers current scientific literature to inform healthcare organisations on a practical way to consider and mitigate risk to their staff. The framework helps organisations by encouraging a three step approach: Assessment of Workplace Assessing areas of potential exposure to SARS-Co. V-2, application of control measures such as hygiene, safe systems of work, PPE training and testing. Assessment of Workforce Identify individuals with increased vulnerability; specific long-term conditions, older age and pregnancy. Evidence suggests ethnicity maybe also associated with increased vulnerability. Availability of appropriate job adjustment and redeployment options. Assessment of Individual 9 | Consider age, sex, those with a underlying health conditions. Those of BAME appear to be at increased risk, particularly aged above 55 or have comorbidities. Pregnancy and disabilities.

Dr Nikki Kanani Medical Director for Primary Care, NHSE/I 10: 35 -10: 50 Employers Responsibilities in Primary Care Why a risk assessment tool is required and why focus on Black and Asian ethnicity? Shareen Pavaday Senior Policy and Evidence Lead, Equalities and Inclusion Team, NHSE/I With an extensive 17 years in the NHS, prior to her role in NHSE/I, Shareen has led a successful career as a Therapy Radiographer across various Trusts and more recently managing Cancer Services and Head of Equality, Diversity and Inclusion at North Middlesex University Hospital NHS Trust. NHS England NHS Improvement

COVID 19 - Assessing the Risks A webinar for Primary Care Employers Responsibilities in Primary Care Why a risk assessment tool is required and why focus on Black and Asian ethnicity Thursday 9 th July 2020 10 am-11. 30 am Dr Nikki Kanani, Medical Director for Primary Care Shareen Pavaday, Senior Policy & Evidence Lead, Equality & Inclusion NHS England NHS Improvement

Strategic Context • Evidence shows that people from BAME backgrounds are being disproportionately affected by COVID-19. The data shows increased risk of infection and increased mortality rates. • Whilst the reasons for this are not fully clear, we know we need to take steps now to ensure the safety and protection of our BAME staff, who represent a significant proportion of our primary care workforce. • Discrimination based on ethnicity is still an issue, including within the NHS. We need to create a culture where we enable and actively encourage open dialogue to understand this further and take action to address this, based on the lived experiences of our staff.

Compassionate leadership: being comfortable with the uncomfortable…
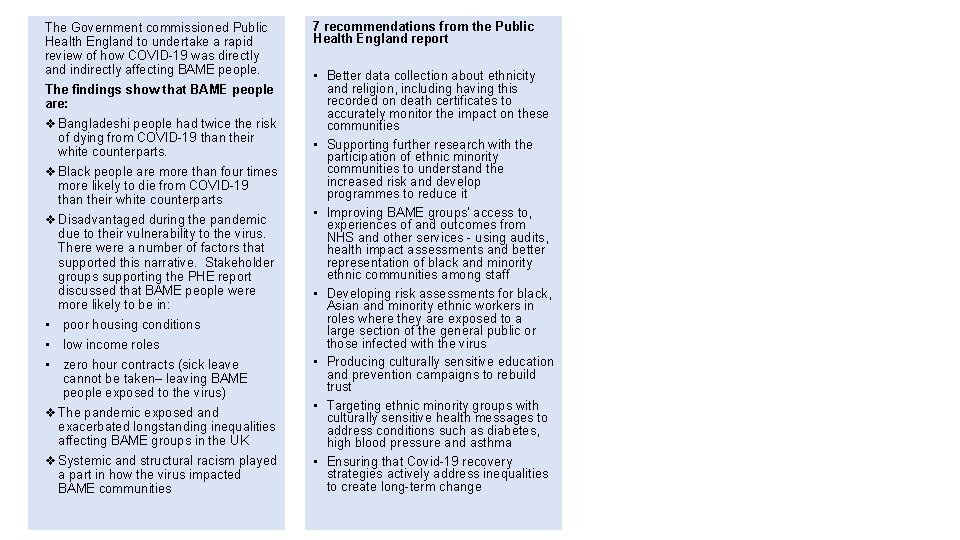
The Government commissioned Public Health England to undertake a rapid review of how COVID-19 was directly and indirectly affecting BAME people. The findings show that BAME people are: v Bangladeshi people had twice the risk of dying from COVID-19 than their white counterparts. v Black people are more than four times more likely to die from COVID-19 than their white counterparts v Disadvantaged during the pandemic due to their vulnerability to the virus. There were a number of factors that supported this narrative. Stakeholder groups supporting the PHE report discussed that BAME people were more likely to be in: • poor housing conditions • low income roles • zero hour contracts (sick leave cannot be taken– leaving BAME people exposed to the virus) v The pandemic exposed and exacerbated longstanding inequalities affecting BAME groups in the UK v Systemic and structural racism played a part in how the virus impacted BAME communities 7 recommendations from the Public Health England report • Better data collection about ethnicity and religion, including having this recorded on death certificates to accurately monitor the impact on these communities • Supporting further research with the participation of ethnic minority communities to understand the increased risk and develop programmes to reduce it • Improving BAME groups' access to, experiences of and outcomes from NHS and other services - using audits, health impact assessments and better representation of black and minority ethnic communities among staff • Developing risk assessments for black, Asian and minority ethnic workers in roles where they are exposed to a large section of the general public or those infected with the virus • Producing culturally sensitive education and prevention campaigns to rebuild trust • Targeting ethnic minority groups with culturally sensitive health messages to address conditions such as diabetes, high blood pressure and asthma • Ensuring that Covid-19 recovery strategies actively address inequalities to create long-term change Understanding the impact of COVID-19 on BAME groups 14
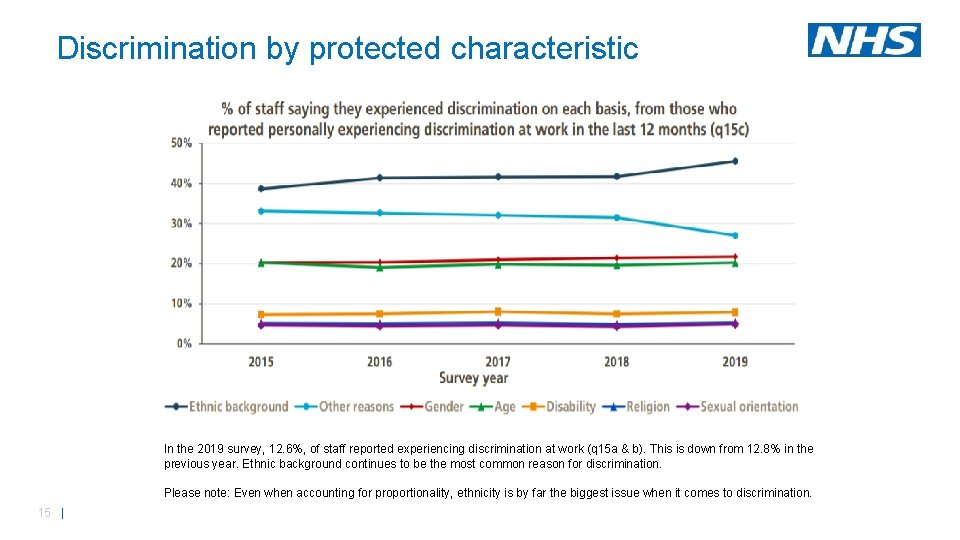
Discrimination by protected characteristic In the 2019 survey, 12. 6%, of staff reported experiencing discrimination at work (q 15 a & b). This is down from 12. 8% in the previous year. Ethnic background continues to be the most common reason for discrimination. Please note: Even when accounting for proportionality, ethnicity is by far the biggest issue when it comes to discrimination. 15 |
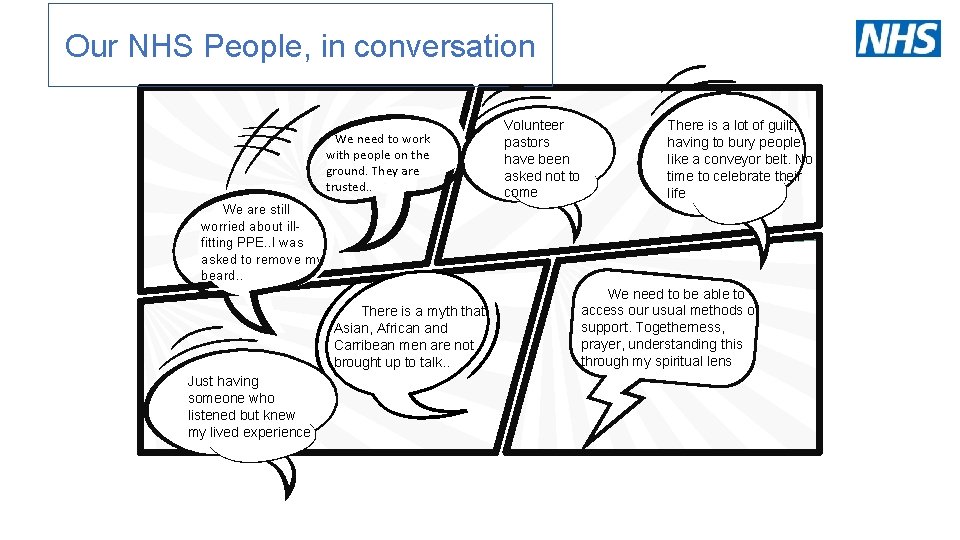
Our NHS People, in conversation V We need to work with people on the ground. They are trusted. . We are still worried about illfitting PPE. . I was asked to remove my beard. . There is a myth that Asian, African and Carribean men are not brought up to talk. . Just having someone who listened but knew my lived experience Volunteer pastors have been asked not to come There is a lot of guilt, having to bury people like a conveyor belt. No time to celebrate their life We need to be able to access our usual methods of support. Togetherness, prayer, understanding this through my spiritual lens

As a learning organisation – we have acted on the ‘precautionary principle’ On 15 th April, Simon Stevens convened a meeting of leaders in healthcare and representative bodies such as British Medical Association and Royal College of Nursing to discuss the emerging evidence and agree a plan of action including getting preliminary guidance out to the system. NHS Chief People Officer, Prerana Issar, launched a comprehensive programme to address the issue of impact of COVID-19 on our BAME workforce with five streams of work – protection of staff, rehab and recovery, communications, staff networks and representation in decision making - underpinned by three principles of protecting, supporting, and engaging our staff. 1. Staff Protection 2. Staff Engagement 17 | 3. Staff Support 404
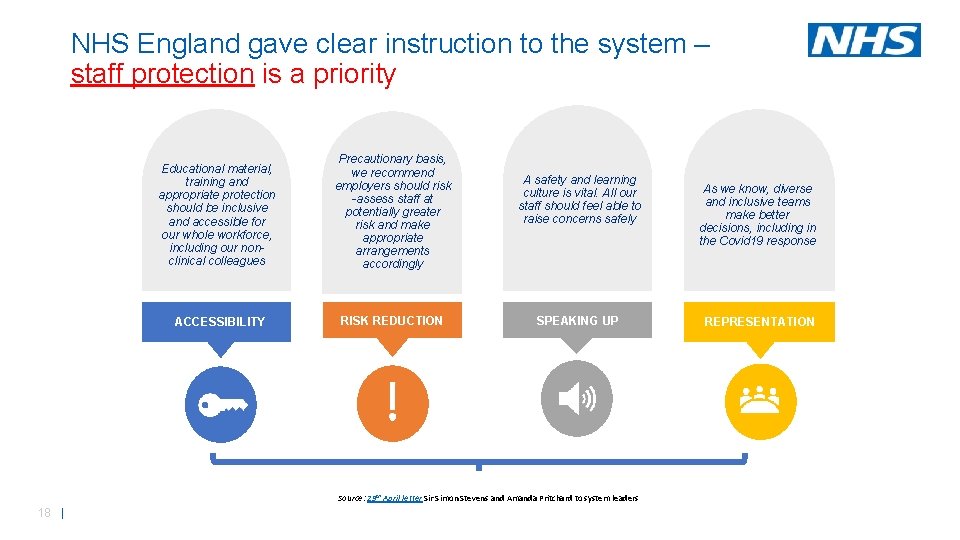
NHS England gave clear instruction to the system – staff protection is a priority Educational material, training and appropriate protection should be inclusive and accessible for our whole workforce, including our nonclinical colleagues ACCESSIBILITY Precautionary basis, we recommend employers should risk -assess staff at potentially greater risk and make appropriate arrangements accordingly RISK REDUCTION A safety and learning culture is vital. All our staff should feel able to raise concerns safely SPEAKING UP Source: 29 th April letter Simon Stevens and Amanda Pritchard to system leaders 18 | As we know, diverse and inclusive teams make better decisions, including in the Covid 19 response REPRESENTATION
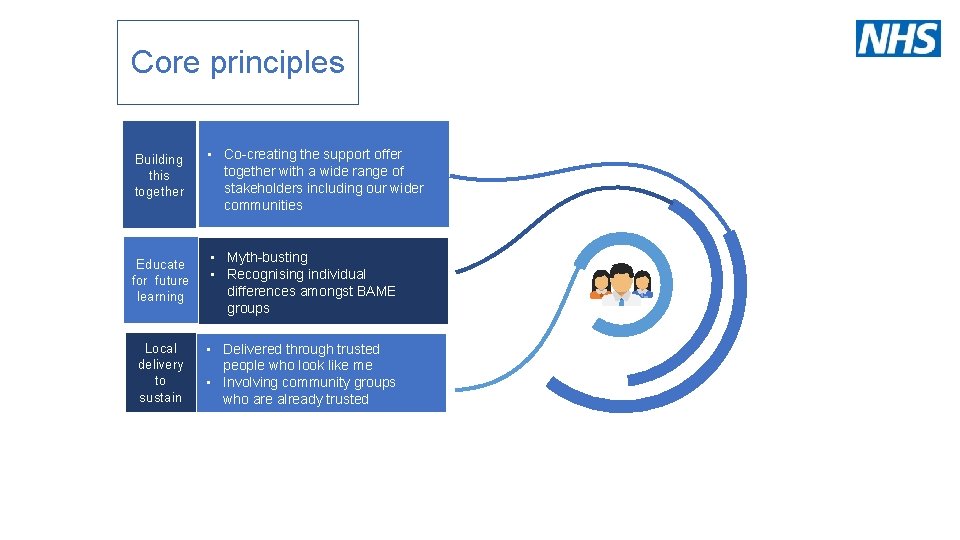
Core principles Building this together • Co-creating the support offer This is a sample text. Insert together with a wide range of your desired text here. stakeholders including our wider communities Educate for future learning • Myth-busting This is a sample text. Insert your desired text here. • Recognising individual differences amongst BAME groups Local delivery to sustain This is a sample text. Insert your desired text here. • Delivered through trusted people who look like me This is a sample text. Insert • Involving community groups your desired text here. who are already trusted

We are reviewing protection for all staff in light of emerging risk factors Although initially focused on BAME as there is a disproportionate impact, we are reviewing provision for all staff through risk assessments and in conjunction with available scientific evidence. NHS Employers published guidance on 30 April, which was updated on 28 May, and we engaged a group of clinical experts to rapidly develop a risk reduction framework which has been published by the Faculty of Occupational Medicine. Other publications have been produced by organisations such as the Royal College of Psychiatrists. All organisations are to deploy a comprehensive education program focusing on social distancing, hand hygiene and PPE. This program should reach the whole workforce including lower grades where BAME staff are over represented. Alongside this, developing a central communications effort that helps to reach agency staff, support services and ancillary workforce– understanding that traditional learning tools such as e-learning may need to be modified to achieve penetration. We are working towards ensuring that both mask fit testing and staff testing are an inclusive experience for all. This will also be reflected in central communications effort. We are also asking for examples of best practice, where organisations are taking a ‘quality improvement’ approach to their processes, reviewing their approach, and building -in improvements. COVID-19 deaths data is now publicly available on the NHS England website including breakdown by ethnicity. For staff, we have a reporting process in place for providers and CCGs. We are currently ensuring that our returner data also considers ethnicity. All advice on staff protection applies to existing and returning staff. 20 |

Useful tools and resources ALAMA: https: //alama. org. uk/covid-19 -medical-risk-assessment/ SAAD score 2: https: //abmacademy. com/wp-content/uploads/2020/05/SAAD-Score-2. pdf BAPIO: https: //www. bapio. co. uk/risk-assessment/ FOM Risk Reduction Framework: https: //www. fom. ac. uk/wp-content/uploads/Risk-Reduction-Framework-for-NHS-staff-at-risk-of-COVID-19 infection-12 -05 -20. pdf Simple Risk Stratification: https: //www. bma. org. uk/media/2768/bma-covid-19 -risk-assessment-tool-july 2020. pdf NHS Employers - range of materials to support risk assessment and the discussions needed to inform it: https: //www. nhsemployers. org/covid 19/health-safety-and-wellbeing/risk-assessments-for-staff

Protection: employers should risk assess staff at potentially greater risk Following the mid-April summit and acting on a precautionary principle, all employers are recommended to riskassess staff at potentially greater risk and make appropriate arrangements accordingly. With our support, on 30 April NHS Employers published risk assessment guidance signposted to NHS leaders, and since updated on 28 May. The risk assessment guidance has been complemented with case studies of deployment in primary care to provide further guidance on use. AT Medics is a primary care organisation that manages 35 GP practices employing over 800 staff, including 100 GPs in some of the most socio-economically disadvantaged areas of London. 22 |
Case study: AT Medics Primary Care Risk Assessment Primary care provider AT Medics collaborated with Brent Clinical Commissioning Group to provide a COVID-19 ‘hot hub’ (patient assessment centre) across Brent. AT Medics people managers used a risk assessment framework and NHS Employers’ guidance when deploying staff. Careful communication guided staff to work from home with enhanced IT support. For staff continuing to work in practice sites, the organisation coordinated early investment into adequate PPE, cleaning equipment and patient signage. AT Medics had to quickly establish remote working for over 800 staff within seven days. Solutions included cloud-based working, new laptops and support for staff using their own devices, and an online consultation platform, Dr. i. Q, for patients and staff. AT Medics’ training and education has been shared widely across England to support other COVID-19 hot hubs and general practices. “We knew the first step to helping patients was to reassure our own staff so they could use their professional skills safely and effectively. A risk assessment programme did not take long to set up, but quickly allowed our staff to concentrate on what they do best, in the hot hub itself, or working remotely. ” – Omar Din, CEO, AT Medics 23 |
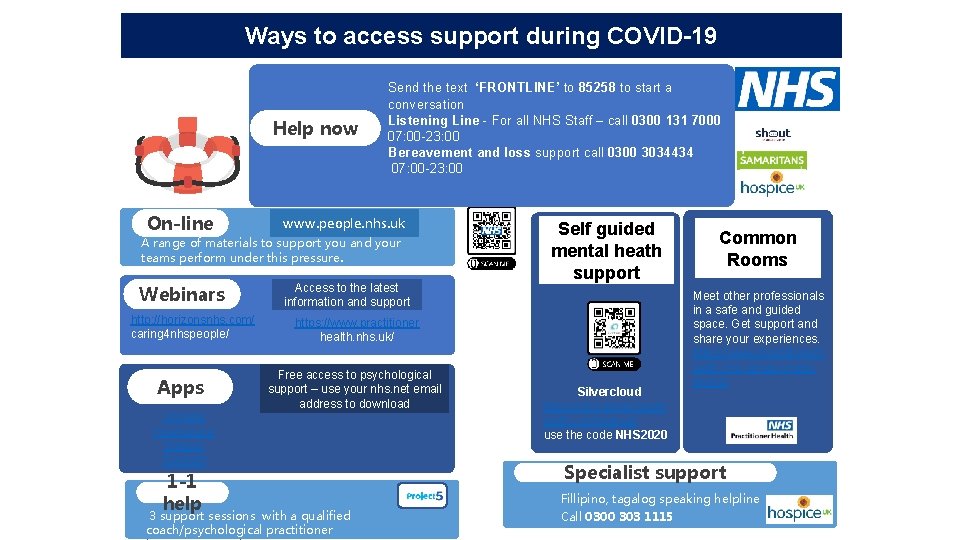
Ways to access support during COVID-19 Help now On-line Send the text ‘FRONTLINE’ to 85258 to start a conversation Listening Line - For all NHS Staff – call 0300 131 7000 07: 00 -23: 00 Bereavement and loss support call 0300 3034434 07: 00 -23: 00 www. people. nhs. uk A range of materials to support you and your teams perform under this pressure. Webinars http: //horizonsnhs. com/ caring 4 nhspeople/ Apps Access to the latest information and support https: //www. practitioner health. nhs. uk/ Free access to psychological support – use your nhs. net email address to download Unmind Headspace Sleepio Daylight 1 -1 help Self guided Emotional Common support mental heath Rooms support 3 support sessions with a qualified coach/psychological practitioner Silvercloud https: //nhs. silvercloudh ealth. com/signup/ use the code NHS 2020 Meet other professionals in a safe and guided space. Get support and share your experiences. https: //www. practitionerh ealth. nhs. uk/upcomingevents Specialist support Fillipino, tagalog speaking helpline Call 0300 303 1115

10: 50 -11: 00 Sharing Experience and Practical Tips Dr Jo Sauvage FRCGP Chair, NHS North Central London CCG NHS England NHS Improvement

COVID 19 - Assessing the Risks A webinar for Primary Care Q and A Panel 11: 00 -11: 25 Janine La Rosa Abdul Razaq Dr Jo Sauvage Shareen Pavaday NHS England NHS Improvement

11: 25 -11: 30 Summing up Dr Jo Sauvage FRCGP Chair, NHS North Central London CCG NHS England NHS Improvement

COVID 19 - Assessing the Risks A webinar for Primary Care THANK YOU! Special thanks to all the presenters and Riyad Karim, Keziah Bowers and Nicola Sage NHS England NHS Improvement
- Slides: 28