Counselors the Patient Protection and Affordable Care Act

Counselors, the Patient Protection and Affordable Care Act, and more… Scott Barstow ACA Director of Public Policy and Legislation sbarstow@counseling. org -- 800 -347 -6647 x 234 (Carol’s title slide is later…)

PPACA and counselors: the Basics Essential Health Benefits (EHB) definition PPACA, EHB, and the Mental Health Parity and Addiction Equity Act (MHPAEA) Provider Nondiscrimination Preventive Services definition

Essential Health Benefits: A State, not Federal, issue? HHS says (Dec. 16 th guidance) it intends to let States determine what is in the essential health benefit (EHB) package, instead of setting a single national standard Comments are being accepted through January 31 st, and can be sent to Essential. Health. Benefits@cms. hhs. gov. Note that all submitted comments are likely to be made public Non-grandfathered health plans in the individual and small group markets, both inside and outside of the Exchanges, Medicaid benchmark and benchmark-equivalent, and Basic Health Programs must cover the EHB starting in 2014 EHB includes items and services in 10 benefit categories, including item number 5: mental health and substance use disorder services, including behavioral health treatment

How would States decide “Essential Health Benefits”? EHB defined by a benchmark plan selected by State, reflecting the scope and limits of services in "typical employer plan" in that state HHS: The following four benchmark plans "best reflect the statutory standards for EHB" for 2014 and 2015: 1 the largest plan by enrollment in any of the three largest small group insurance products in the state's small group market; 2 any of the largest three State employee health benefit plans by enrollment; 3 any of the largest three national FEHBP plan options by enrollment; or 4 the largest insured commercial non-Medicaid HMO operating in the state

Essential Health Benefits and the Mental Health Parity and Addiction Equity Act HHS (December 16, 2011 "Essential Health Benefits" bulletin): "Because the Affordable Care Act requires any issuer that must meet the coverage standard set in section 1302(a) to cover each of the 10 categories, all such plans must include coverage for mental health and substance use disorder services, including behavioral health treatment. Consistent with Congressional intent, we intend to propose that parity applies in the context of EHB. ” All Medicaid expansion plans must cover EHB

PPACA: Nondiscrimination against counselors! (beginning 2014) ‘‘SEC. 2706. NON-DISCRIMINATION IN HEALTH CARE (a) PROVIDERS. —A group health plan and a health insurance issuer offering group or individual health insurance coverage shall not discriminate with respect to participation under the plan or coverage against any health care provider who is acting within the scope of that provider’s license or certification under applicable State law. This section shall not require that a group health plan or health insurance issuer contract with any health care provider willing to abide by the terms and conditions for participation established by the plan or issuer. Nothing in this section shall be construed as preventing a group health plan, a health insurance issuer, or the Secretary from establishing varying reimbursement rates based on quality or performance measures. ”

PPACA: Preventive Services coverage Must be covered without copayment or co-insurance, when delivered by a network provider Current list (U. S. Preventive Services Task Force, online at http: //www. uspreventiveservicestaskforce. org) includes: For adults: alcohol misuse screening and counseling depression screening obesity screening and counseling for all adults sexually transmitted infection prevention counseling for adults at higher risk tobacco use cessation interventions for tobacco users

Preventive Services list, continued… For women, including pregnant women: • domestic and interpersonal violence screening and counseling (in plan years starting on or after 8/1/2012) • HIV screening and counseling, and sexually transmitted infections counseling, for sexually active women (in plan years starting on or after August 1, 2012) • "expanded counseling" for pregnant tobacco users For children: • • • alcohol and drug use assessments for adolescents behavioral assessments for children of all ages depression screening for adolescents obesity screening and counseling sexually transmitted infection prevention counseling and screening for adolescents at higher risk

Counselors and the feds (military) Three similar, but not identical federal descriptions: TRICARE independent practice recognition Army Substance Abuse Standards recognition VA

TRICARE independent practice standards Do. D Interim Final Rule (may change, likely won't. . . at least for awhile) "This rule is expected to encourage greater participation of MHCs in the TRICARE network, result in improved access to quality mental health treatment for TRICARE beneficiaries, and sets [sic] provider quality standards typical of other mental health providers authorized under TRICARE. ” comments being accepted if received by February 27 th: Federal e. Rulemaking Portal: mailto: http: //www. regulations. gov, or by mail: Federal Docket Management System Office 4800 Mark Center Drive 2 nd Floor, East Tower, Suite 02 G 09 Alexandria, VA 22350 -3100

TRICARE independent practice requirements: now through 2014 Licensed counselors must: have a master's or higher-level degree “from a mental health counseling program of education and training accredited by CACREP” and pass the NCE, or have a master's or higher-level degree “from a mental health counseling program of education and training” from a regionally accredited (or CACREP) institution, and pass the NCMHCE; and have 2 years/3, 000 hours of supervised clinical practice, "provided by a mental health counselor who is licensed for independent practice in mental health counseling in the jurisdiction where practicing and must be conducted in a manner that is consistent with the guidelines for supervision of the American Mental Health Counselors Association”

TRICARE independent practice requirements: beginning 2015 Licensed counselors must: have passed the NCMHCE have a master's or higher degree from a mental health counseling program of education and training accredited by CACREP have 2 years/3, 000 hours of supervised clinical practice, under same requirements as on previous slide Independent practice only; practice under physician referral and supervision will no longer be allowed.

TRICARE independent practice requirements: some notes The rule includes language “…to allow the Director, TRICARE Management Activity to amend or modify existing requirements or add other qualifications or criteria in the future to accommodate professional quality and licensing standards as they may change over time. ” Unanswered questions: ◦ What does “degree from a mental health counseling program of education and training” mean? [NOTE: existing “…or allied mental health field” language no longer used] ◦ How are they planning on checking whether or not counselors’ supervision hours are consistent with AMHCA guidelines? What other supervision guidelines—if any—did they consider?

Army Substance Abuse Program (SAP) Army Directive 2011 -09 (subtitled “Employment of Licensed Professional Counselors as Fully Functioning Army Substance Abuse Program Practitioners”) issued 7/26/11 Authorizes ASAP “to employ licensed professional counselors and licensed mental health counselors as independent practitioners” Requirements: Master’s degree in counseling from a program accredited by CACREP (accreditation requirement waived for counselors already employed with ASAP or who have already entered application process for an ASAP counseling position) Pass the NCMHCE At highest clinical level of licensure

Comparing the federal standards Agency Education: master’s degree… Exam Supervision Dept of Veterans Affairs …in mental health counseling or related field from CACREP program, doctoral degrees not recognized -- -- TRICARE (post 2014) …from a mental health counseling program of education and training accredited by CACREP NCMHCE 2 years/3, 000 hrs, 100 hrs faceto-face, consistent with AMHCA guidelines Army SAP …in counseling from a program accredited by CACREP NCMHCE -- -- 2 years postmaster’s Medicare bill (S. In mental health counseling or a 604) related field ACA review of a sample of New York licensees found that no more than 13% of licensees had a CACREP degree

Institute of Medicine is skeptical of all mental health professionals’ preparation “Education, accreditation, licensure, certification, and clinical- experience requirements for mental health professionals are components of a quality-management system. However, they have little specificity with regard to knowledge of and experience with particular health problems or evidence-based practices. That generally limits the confidence that can be placed in the preparation of any of these professionals to diagnose and treat disorders that may be found in the TRICARE beneficiary population. Research regarding the quality of care for M/SU conditions indicates that there are widespread deficiencies in the training of providers and in the infrastructure that supports their practice. ” p. 9 IOM: “Provision of Mental Health Counseling Services Under TRICARE” – online at http: //www. iom. edu/Reports/2010/Provision-of-Mental -Health-Counseling-Services-Under-TRICARE. aspx

IOM Language on Social Workers Social work: “Practitioners must have a master’s degree (MSW, MSSA, or MSS) from an accredited program that includes coursework in clinical assessment, counseling, psychotherapy, and caseload management. ” [? ? ? ] (p. 24) Table 3. 1 Comparison of Preparation Requirements for the Mental Health Professions “Coursework required in professional social worker identity; ethical principles; critical thinking; diversity, difference; advancing human rights, social and economic justice; research-informed practice, practice-informed research; human behavior, social environment; policy practice; contexts that shape practice; engaging, assessing, intervening, evaluating individuals, families, groups, organizations, communities. ” (p. 95)

CSWE: A Good Yardstick? Educational Policy 2. 1. 10(c)—Intervention: “Social workers initiate actions to achieve organizational goals; implement prevention interventions that enhance client capacities help clients resolve problems; negotiate, mediate, and advocate for clients; and facilitate transitions and endings. ” Educational Policy M 2. 2—Advanced Practice: “In areas of specialization, advanced practitioners assess, intervene, and evaluate to promote human and social well-being. ”

An example: MSW Program at Washington University in St. Louis Six concentrations offered: Management Social and economic development Children, youth, and families Gerontology Health Mental health All are, presumably, CSWEaccredited. All qualify social workers for recognition by the VA and TRICARE.

Rural access is an issue Ellis, Konrad, Thomas, and Morrissey: “County-level Estimates of Mental Health Professional Supply in the U. S. ” – Psychiatric Services, October, 2009, 1315 -1322 “In general, marriage and family therapists, counselors, and psychiatric nurses appeared to be less concentrated in higherincome urban areas, compared with providers in the other three professions [of psychiatry, psychology, and social work]. ” (p. 1319)

The Patient Protection and Affordable Health Care Act – Counselors’ Roles Carol Buchanan Jones, Ph. D, NCC, LPC-S, cjones@wmcarey. edu Director, Psychology and Counseling William Carey University, Tradition Co-Principal Investigator, MS Coastal Primary/Mental Health Collaborative, supported by a grant from the Robert Wood Johnson Foundation President, AASCB; Chair, MS Bd of Examiners for Licensed Professional Counselors AASCB Conference - January 2012
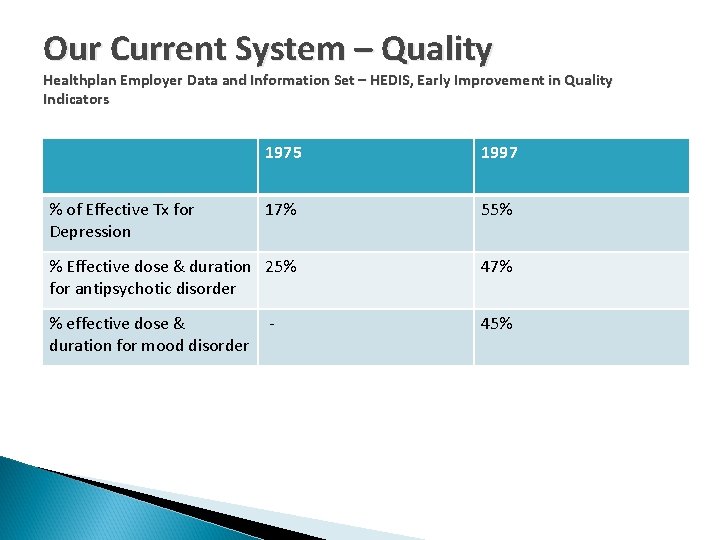
Our Current System – Quality Healthplan Employer Data and Information Set – HEDIS, Early Improvement in Quality Indicators 1975 1997 17% 55% % Effective dose & duration 25% for antipsychotic disorder 47% % effective dose & duration for mood disorder 45% % of Effective Tx for Depression

Quality
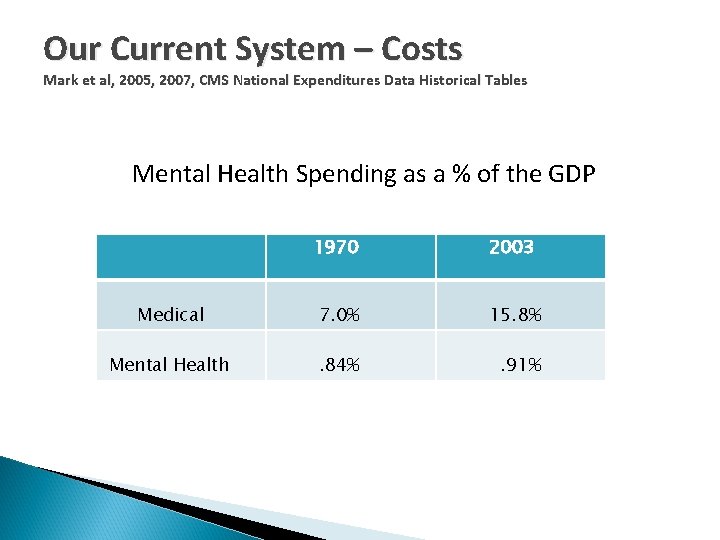
Our Current System – Costs Mark et al, 2005, 2007, CMS National Expenditures Data Historical Tables Mental Health Spending as a % of the GDP 1970 2003 Medical 7. 0% 15. 8% Mental Health . 84% . 91%

Costs
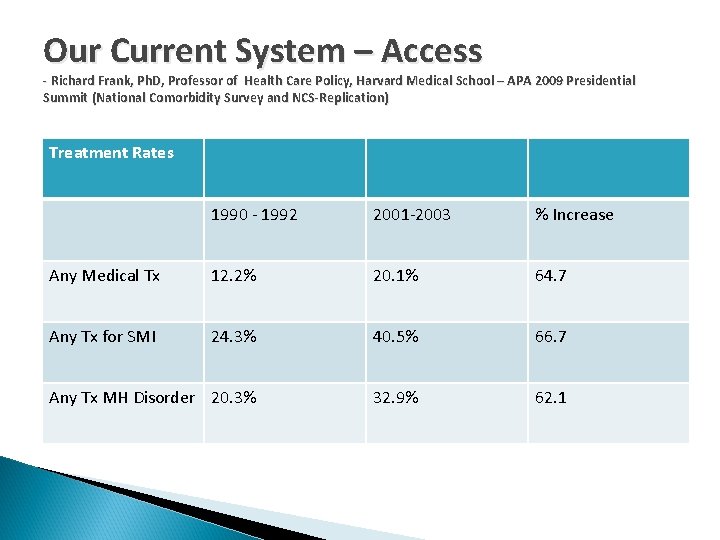

Our Current System – Access - Richard Frank, Ph. D, Professor of Health Care Policy, Harvard Medical School – APA 2009 Presidential Summit (National Comorbidity Survey and NCS-Replication) Treatment Rates 1990 - 1992 2001 -2003 % Increase Any Medical Tx 12. 2% 20. 1% 64. 7 Any Tx for SMI 24. 3% 40. 5% 66. 7 Any Tx MH Disorder 20. 3% 32. 9% 62. 1
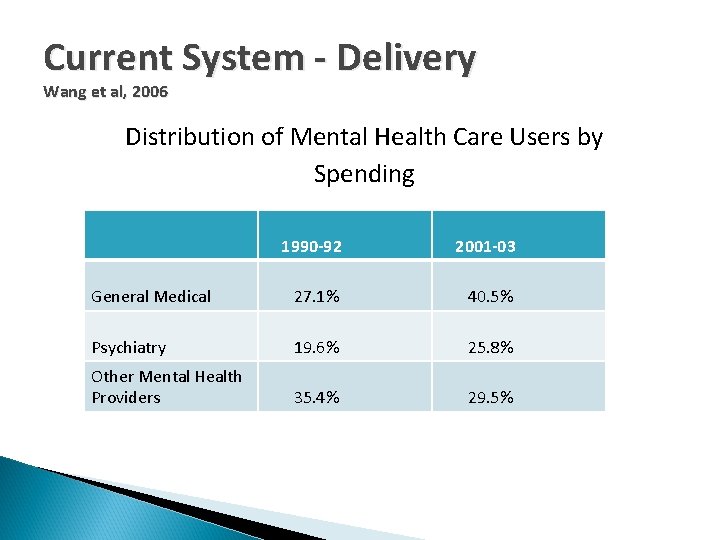
Current System - Delivery Wang et al, 2006 Distribution of Mental Health Care Users by Spending 1990 -92 2001 -03 General Medical 27. 1% 40. 5% Psychiatry 19. 6% 25. 8% Other Mental Health Providers 35. 4% 29. 5%

Mental Health Services Primary care providers now furnish over half of the mental health treatment in this country and approximately 25% of all primary care recipients have diagnosable mental disorders where most are depression or anxiety. Yet up to 50% of these mental health disorder are undiagnosed (Regier et, 1993). Examining children who do receive some mental health interventions, 80% of the work is done by individuals who have little or no training in mental health, frequently, the primary health care sector (Stroul, 2007).

Six Aims of High-Quality Health Care for Mental and Substance-Use Conditions (IOM, 2006) Safe Effective Patient-Centered Timely Efficient Equitable

The Quality Chasm’s Ten Rules to Guide the Redesign of Health Care (IOM, 2001) Care based in continuous healing relationships. Customization based on patient needs and values. The patient as the source of control. Shared knowledge and the free flow of information. Evidence-based decision making,

Ten Rules continued Safety as a system property. The need for transparency. Anticipation of needs. Continuous decrease in waste. Cooperation among clinicians.

Key Provisions in the Patient Protection and Affordable Care Act Ensuring mandatory mental health coverage at parity; New opportunities in primary and integrated care; A New Center for Medicare and Medicaid Innovation; New Medicaid mental health mandated benefits and parity requirements; A national focus on preventions; Provider nondiscrimination.

New Opportunities for Counselors must “come to the table” along with other mental health professionals and participate or risk being left out when the “how” of implementation is decided. Larger patient population; New funding for training; Increased support for research.

New Opportunities in Integrated Care for Counselors In Accountable Care Organizations (ACO) and Patient-Centered Medical Home: Accountable Care Organizations (ACOs) are groups of doctors, hospitals, and other health care providers, who come together voluntarily to give coordinated high quality care to the Medicare patients they serve. The Patient Centered Medical Home is a health care setting that facilitates partnerships between individual patients, their personal physicians, mental health professionals, and when appropriate, the patient’s family. Care is facilitated by registries, information technology, health information exchange (HIE) and other means to assure that patients get the indicated care when and where they need and want it in a culturally and linguistically appropriate manner.

New Opportunities Emphasis on and demand for mental health professionals integrated into primary care, particularly, in community health centers. Prevention and Public Health Fund to support proven preventive and public health programs to address issues such as obesity and smoking. The Patient-Centered Outcomes Research Institute to discover how to effectively prevent, treat and manage health conditions.

Counselors’ Distinct Theoretical Foundation and Belief System Remley, T, Herlihy, B. (2010). Best perspective for assisting individuals resolve personal and emotional issues is the wellness model of mental health. Most of the issues individuals face are developmental in nature. Prevention and early intervention are superior in dealing with personal and emotional problems. The goal of counseling is to empower clients and client systems.

What is Mental Health Integration? Co-Location v. Integration Co-Location: - Model provides for a department or center inside a medical clinic; - Behavioral health professional does not have as much interaction with medical professional(s) other than a referral from the medical professional(s); - Patients may need to make more than one trip to the clinic for services; - Mental health services are typically provided in hour-long traditional therapy; - Medical/Mental health team functions in a fragmented fashion.

What? Integration: - Behavioral health professional might be in the medical exam room with the physician; - Approximately seventy per cent (70%) of behavioral health professional’s time is spent in screening and brief interventions; - Therapeutic interventions may include educational sessions; - Typically thirty percent (30%) of the behavioral health professional’s time is spent in hour-long traditional therapy - CBT, limited number of visits, and referral; - Patients see therapist on same day; - Patient support outside clinic hours is provided by trained volunteers from community agencies (NAMI, Interfaith, etc). - Frequent and ongoing consultations among PCP, BHP, and RN;

Essential Components of Mental Health Integration (Intermountain Healthcare) Primary Care Provider Behavioral Health Provider Care Manager Screening Instruments Electronic Medical Records Partner Community Agencies

Screening Most visits to primary care providers have a larger psychosocial component; Most poor health outcomes are related to behavioral issues; Primary care providers do a relatively bad job of uncovering mental health issues: Screening is not diagnosis; Positive screens are followed up with more comprehensive evaluation tools/DSM-IV criteria; Screening is face-to-face; Ratio of PCP to BHP - ? ? ?

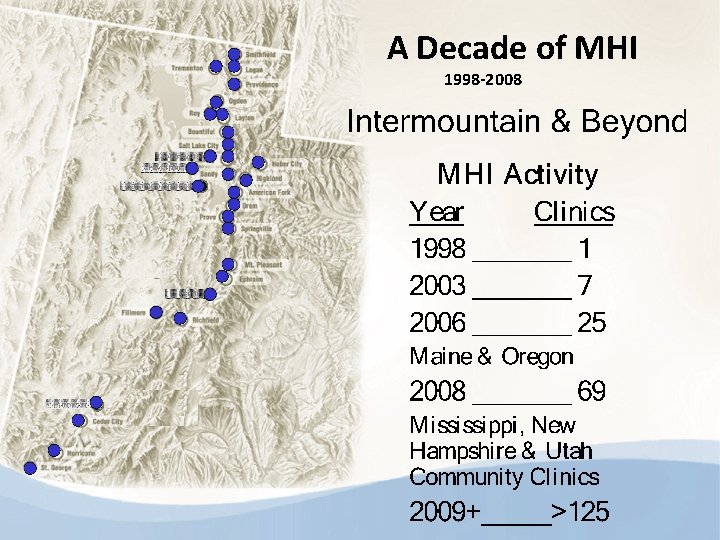
A Decade of MHI 1998 -2008

Mississippi MHI Behavioral Health Professionals work with physicians at Coastal Family Health Center (Coastal maintains seven sites and two mobile sites across five counties that serve over 34, 000 patients annually) in Biloxi to pilot and adapt Utah’s successful Intermountain Healthcare Mental Health Integration model. The pilot project began in June 2009. The goal of the project is the spread of the Mental Health Integration model in Mississippi. Community agencies participating along with Coastal Family Health Center are Gulf Coast Mental Health Center/Department of Mental Health, Gulf Coast Substance Abuse Task Force, Boys and Girls Club of the Gulf Coast, Interfaith Task Force, and MS NAMI.

Benefits of Behavioral Health Providers in Primary Care Benefits that behavioral health professionals provide in an integrated setting include helping patients: Cope with their medical illness. Adhere to medical regimens. Understand emotional influences on disease. Improve communication with their physician and nurse. To ultimately prevent the worsening or return of a disease.

Barriers to MHI Funding behavioral health providers in primary care/Medicaid reimbursement; Sharing the same space; Chaos of primary care setting v. structured therapy visits; “This is not how I was trained; ” “I need more time with my patients (behavioral health providers)!” Concept of confidentiality; Costs are incurred and savings are accrued in different places.

Barriers High costs of Electronic Medical Records that are the infrastructure that supports the integrated care and integration of screening instruments into existing EMR; Training (medical professionals and mental health professionals); Cultural differences in health-related beliefs and behaviors.

Barriers There are wide varieties of mental health professionals and their training. These variations effect quality and outcomes for mental health treatment (IOM, 2006). Two items critical for quality and outcome data are: 1. the use of evidence based treatment and 2. the skill and training of the practitioners.

What Can Counselors Do to “Be at the Table ? ” All politics are local! States will be determining: ◦ Possible Medicaid expansion; ◦ The creation of health insurance exchanges (HIE); ◦ Regulations governing insurance companies that offer products through the HIE’s; ◦ How to expand insurance coverage to the uninsured through Medicaid and HIE’s; ◦ Reduction of “fees for a service. ” These policies will be created at the state level.

Counselors “at the Table” It is critical for Counselors to be involved when these policy decisions are made: Spread awareness and information; State professional organizations are the vehicle for engagement; Contact Public Health/Human Services/Welfare/Medicaid Committees in your state’s House and Senate; Contact your state’s Health Department, Primary Care Associations, Bureau of Mental Health; Contact your Governor’s Office. Stay involved! Engage!

Mississippi “at the Table” Counselors and Coastal Family Health Center CEO testified before a joint Senate and House Mental Health Task Force in November 2009 about the importance of Licensed Professional Counselors in the MHI process. In January 2010 the MS Coastal Primary/Mental Health Collaborative met with Representatives and Senators from the Public Health and Welfare and Medicaid Committees regarding a demonstration project for Medicaid reimbursement for all licensed mental health professionals.

References Frank, R. (2009, May). National Comorbidity Survey and NCS-Replication. Paper presented at the APA 2009 Presidential Summit, San Antonio, TX. Freeland M. , and Cylus, J. (2005, 2007). CMS National Expenditures Data Historical Tables. Institute of Medicine. (2001). Crossing the Quality Chasm: A New Health System for the 21 st Century. Washington, DC: National Academy Press. Institute of Medicine. (2006). Improving the Quality of Health Care for Mental and Substance-Use Conditions. Washington, DC: National Academy Press. Regier, D. , Narrow, W. , Rae, D. , et al. (1993). The de facto US mental and additive disorders service systems: Epidemiology Catchment Area prospective 1 -year prevalence rates of disorders and services. Archives of General Psychiatry, 50, 85 -94. Remley, T. and Herlihy, B. (2010). Ethical, Legal, and Professional Issues in Counseling. (3 rd ed. ). Boston: Merrill/Pearson. Stroul, B. (2007). Integrating Mental Health Services into Primary Care Settings—Summary of the Special Forum Held at the 2006 Georgetown University Training Institutes. Washington, DC: Georgetown University Center for Child and Human Development, National Technical Assistance Center for Children’s Mental Health. Wang, P. S. , Simon, G. , Kessler, R. C. (2005). The economic burden of depression and the costeffectiveness of treatment. International Journal of Methods in Psychiatric Research, 12, 22 -33.
- Slides: 51