Correlates of Absorb Scaffold Thrombosis MultiStudy Registry Results

Correlates of Absorb Scaffold Thrombosis – Multi-Study Registry Results Could Better Patient Selection and Procedural Technique Have Saved the Program? Stephen G. Ellis, MD; Tommaso Gori, MD, Ph. D; Patrick W Serruys, MD, Ph. D; Holger Nef, MD, Giuseppe Steffenino, MD; Salvatore Brugaletta, MD, Ph. D; Thomas Munzel, MD; Cordula Feliz, MD; Gotz Schmidt, MD; Manel Sabate, MD; Yoshi Onuma, MD; R. J. van Geuns, MD; Run-Lin Gao, MD; Maurizio Menichelli, MD; Dean J. Kereiakes, MD; Gregg W. Stone, MD; Luca Testa, MD; Takeshi Kimura, MD; Alexandre Abizaid MD CRT 2018 SGE; 0917 -1, 1

Disclosures Research Grants: Abbott Vascular Medtronic Consultant/Advisory Board Abbott Vascular Boston Scientific Medtronic

Background • Initial results with the Absorb scaffold in stable patients and simple lesions suggested excellent results with a conservative implantation technique, often without postdilatation • Higher than expected early ST rates in larger experiences led to a reexamination of technique • Several modest-sized studies suggested the importance of both appropriate vessel sizing and aspects of postdilatation in reducing ST • We sought to collect the largest number of carefully characterized ST cases and study their correlates SGE; 0317 -1, 2

Ellis S. , et al. J Am Coll Cardiol Intv 2017; 10: 1809 -15 SGE; 0917 -4, 8
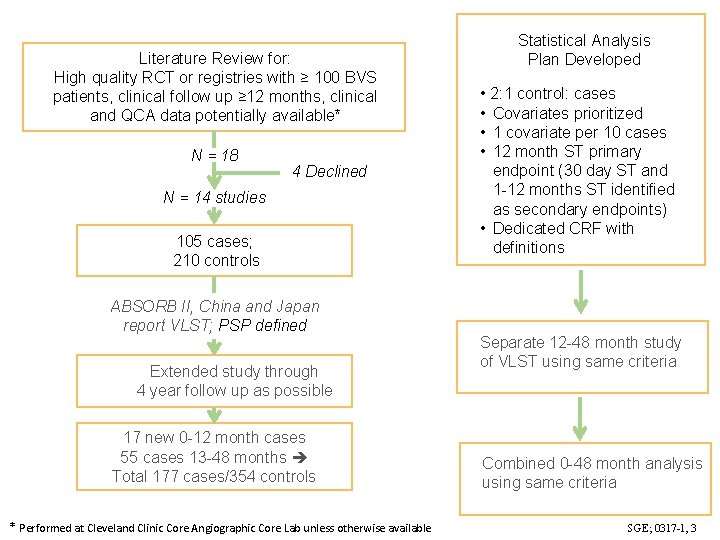
Literature Review for: High quality RCT or registries with ≥ 100 BVS patients, clinical follow up ≥ 12 months, clinical and QCA data potentially available* N = 18 4 Declined N = 14 studies 105 cases; 210 controls ABSORB II, China and Japan report VLST; PSP defined Extended study through 4 year follow up as possible 17 new 0 -12 month cases 55 cases 13 -48 months Total 177 cases/354 controls * Performed at Cleveland Clinic Core Angiographic Core Lab unless otherwise available Statistical Analysis Plan Developed • 2: 1 control: cases • Covariates prioritized • 1 covariate per 10 cases • 12 month ST primary endpoint (30 day ST and 1 -12 months ST identified as secondary endpoints) • Dedicated CRF with definitions Separate 12 -48 month study of VLST using same criteria Combined 0 -48 month analysis using same criteria SGE; 0317 -1, 3

Independent Correlates of 0 -12 Month Scaffold Thrombosis Odds Ratio p Model 1 Off DAPT 3. 47 0. 006 No Post Dilatation ≥ 1. 1 2. 29 0. 022 RVD <2. 40 2. 12 0. 036 Model p=0. 002 Mc. Fadden’s Rho-sq=0. 052 c-statistic-=0. 64 Model 2 MLD<1. 85 mm 3. 07 0. 004 Off DAPT 2. 49 0. 053 Mc. Fadden’s Rho-sq=0. 051 c-statistic-=0. 63 Model p=0. 003 SGE; 0317 -1, 20
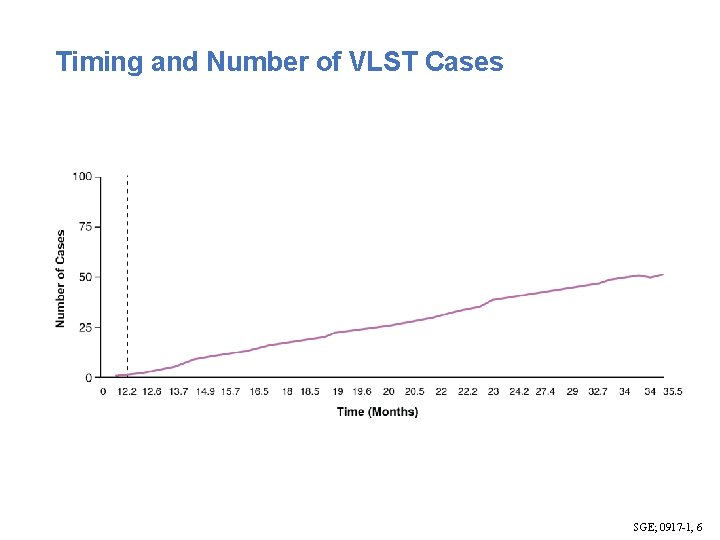
Timing and Number of VLST Cases SGE; 0917 -1, 6
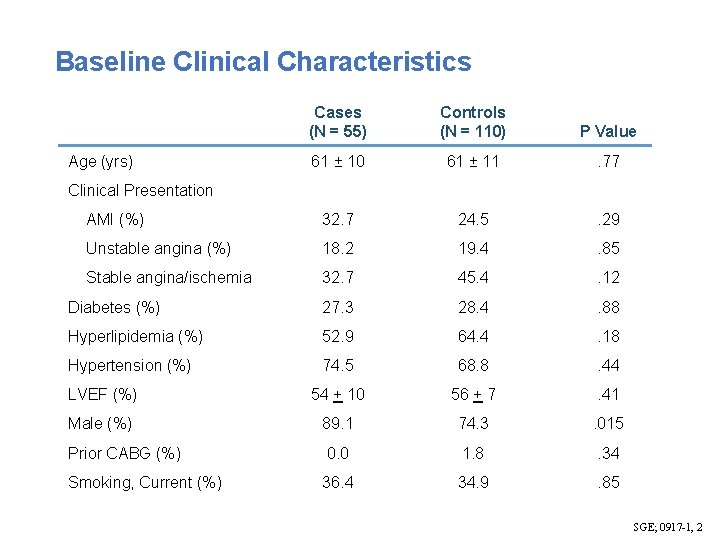
Baseline Clinical Characteristics Cases (N = 55) Controls (N = 110) P Value 61 ± 10 61 ± 11 . 77 AMI (%) 32. 7 24. 5 . 29 Unstable angina (%) 18. 2 19. 4 . 85 Stable angina/ischemia 32. 7 45. 4 . 12 Diabetes (%) 27. 3 28. 4 . 88 Hyperlipidemia (%) 52. 9 64. 4 . 18 Hypertension (%) 74. 5 68. 8 . 44 LVEF (%) 54 + 10 56 + 7 . 41 Male (%) 89. 1 74. 3 . 015 Prior CABG (%) 0. 0 1. 8 . 34 Smoking, Current (%) 36. 4 34. 9 . 85 Age (yrs) Clinical Presentation SGE; 0917 -1, 2
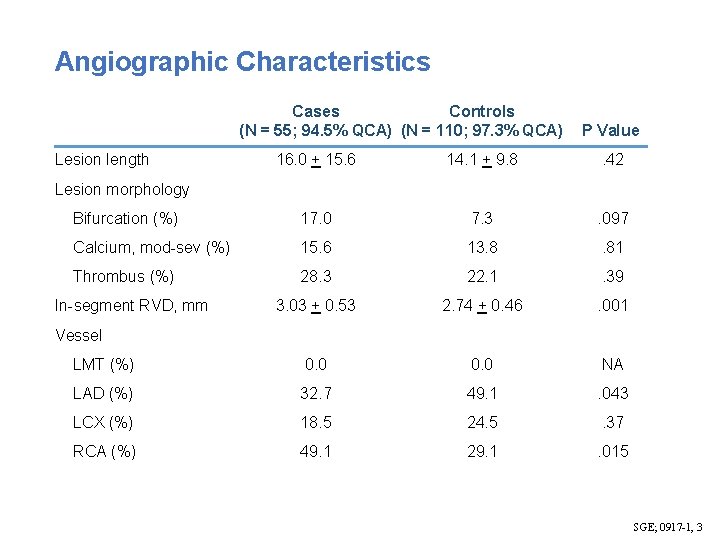
Angiographic Characteristics Cases Controls (N = 55; 94. 5% QCA) (N = 110; 97. 3% QCA) Lesion length P Value 16. 0 + 15. 6 14. 1 + 9. 8 . 42 Bifurcation (%) 17. 0 7. 3 . 097 Calcium, mod-sev (%) 15. 6 13. 8 . 81 Thrombus (%) 28. 3 22. 1 . 39 3. 03 + 0. 53 2. 74 + 0. 46 . 001 LMT (%) 0. 0 NA LAD (%) 32. 7 49. 1 . 043 LCX (%) 18. 5 24. 5 . 37 RCA (%) 49. 1 29. 1 . 015 Lesion morphology In-segment RVD, mm Vessel SGE; 0917 -1, 3
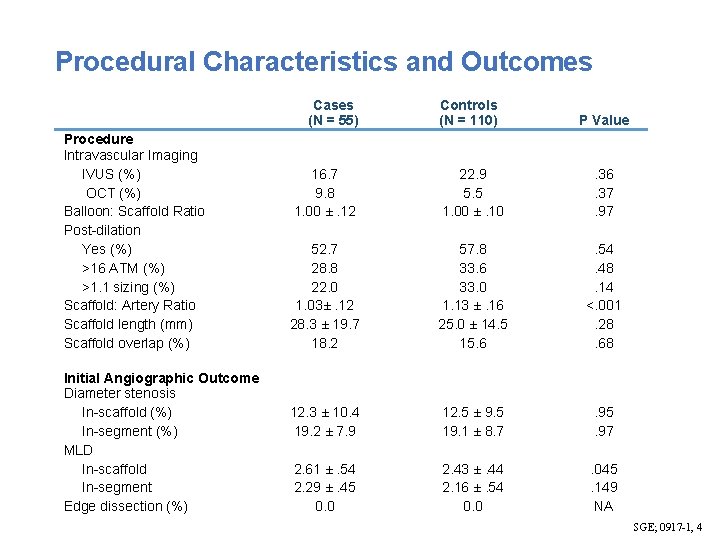
Procedural Characteristics and Outcomes Cases (N = 55) Procedure Intravascular Imaging IVUS (%) OCT (%) Balloon: Scaffold Ratio Post-dilation Yes (%) >16 ATM (%) >1. 1 sizing (%) Scaffold: Artery Ratio Scaffold length (mm) Scaffold overlap (%) Initial Angiographic Outcome Diameter stenosis In-scaffold (%) In-segment (%) MLD In-scaffold In-segment Edge dissection (%) Controls (N = 110) P Value 16. 7 9. 8 1. 00 ±. 12 22. 9 5. 5 1. 00 ±. 10 . 36. 37. 97 52. 7 28. 8 22. 0 1. 03±. 12 28. 3 ± 19. 7 18. 2 57. 8 33. 6 33. 0 1. 13 ±. 16 25. 0 ± 14. 5 15. 6 . 54. 48. 14 <. 001. 28. 68 12. 3 ± 10. 4 19. 2 ± 7. 9 12. 5 ± 9. 5 19. 1 ± 8. 7 . 95. 97 2. 61 ±. 54 2. 29 ±. 45 0. 0 2. 43 ±. 44 2. 16 ±. 54 0. 0 . 045. 149 NA SGE; 0917 -1, 4
![Univariate Correlates of VLST (by Quintiles [mm]) Also evaluated post-dilation at >16 ATM, post-dilation Univariate Correlates of VLST (by Quintiles [mm]) Also evaluated post-dilation at >16 ATM, post-dilation](http://slidetodoc.com/presentation_image_h2/e6726a669ffd0d837d167f61d9b8f8cf/image-11.jpg)
Univariate Correlates of VLST (by Quintiles [mm]) Also evaluated post-dilation at >16 ATM, post-dilation balloon/scaffold ratio, final % stenosis and DAPT use SGE; 0917 -1, 5
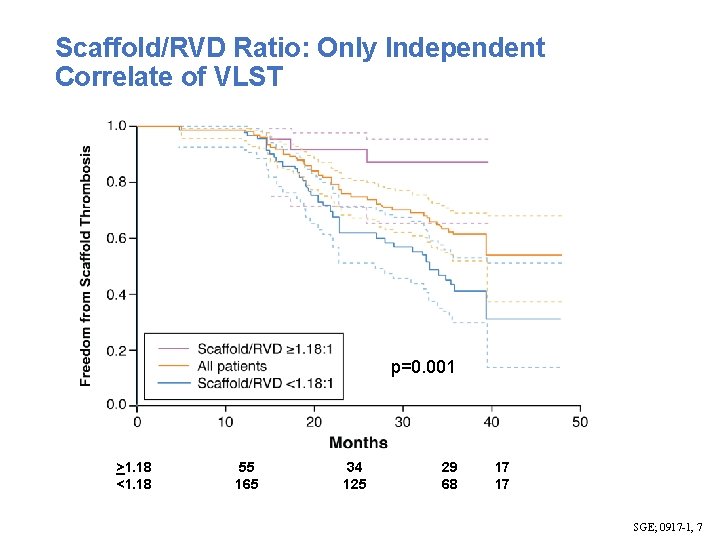
Scaffold/RVD Ratio: Only Independent Correlate of VLST p=0. 001 >1. 18 <1. 18 55 165 34 125 29 68 17 17 SGE; 0917 -1, 7
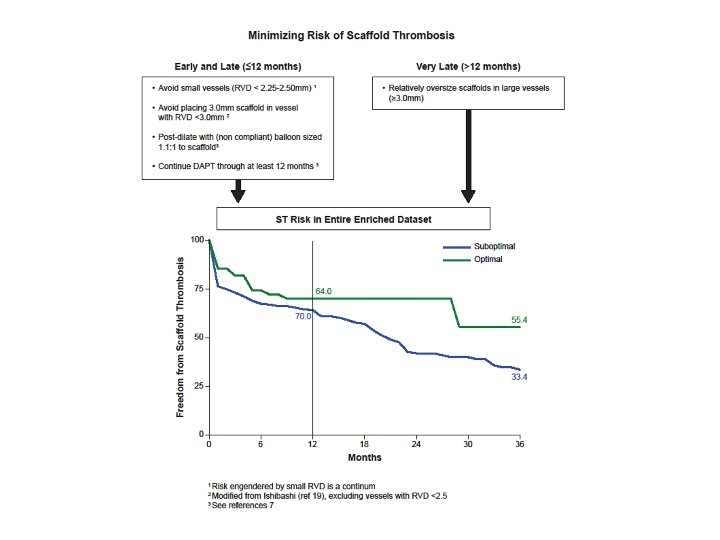
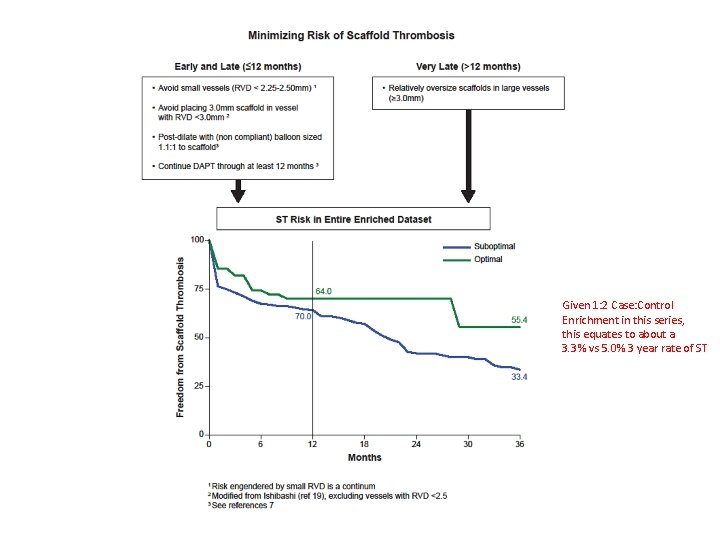
Given 1: 2 Case: Control Enrichment in this series, this equates to about a 3. 3% vs 5. 0% 3 year rate of ST

Limitations • QCA not available on all patients • Different QCA Core Labs • Uncertain use of intracoronary imaging (for cause vs routine vs for documentation only) • Possible over modeling • Limited number of cases SGE; 0317 -1, 19

Conclusions • Relative scaffold undersizing (<1. 18 x RVD), especially common in larger vessels, is the most prominent risk factor for scaffold thrombosis 12 -48 months after implantation • This finding is in contradistinction to the fact that scaffold thrombosis < 12 months after implantation is highly correlated with use in smaller vessels (<2. 4 mm in this series) • Thus overall recommendations following from these data are to avoid implantation in small vessels and to assure proper scaffold sizing • That said, even with optimal patient selection and best identified technique, the estimated 3. 3% 3 year ST is probably not satisfactory, unless rates of MACE after 3 -4 years are diminishingly low SGE; 0317 -1, 21
- Slides: 16