Coronary artery bypass grafting CABG OPCAB Dr Luc

Coronary artery bypass grafting CABG - OPCAB Dr. Luc Tambeur
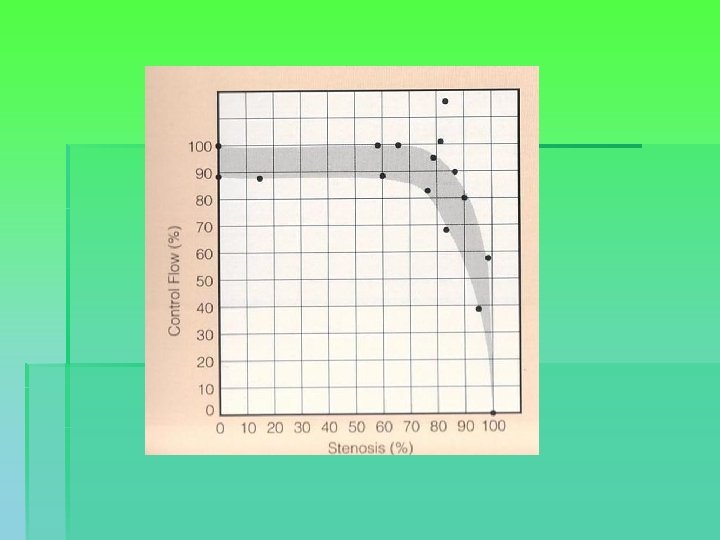
Coronary artery disease § Definition: § Narrowing of the coronary arteries § Caused by thickening and loss of elasticity of the arterial walls § Limiting blood flow to the myocardium § Flow reserve (effort) § At rest § Occlusion
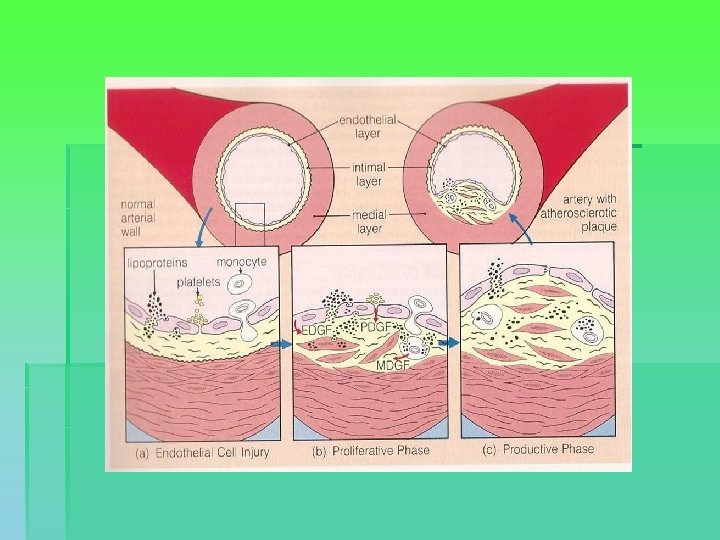
Coronary artery disease § Morphology and processes: § Focal intimal accumulation of lipids, blood elements, fibrous tissue, calcium etc. with associated changes in the media § → Plaque § → Stenosis § Regression of plaque and collateral formation § Plaque rupture and thrombosis § Usually affects multiple coronaries simultaneously, proximally and at bifurcations
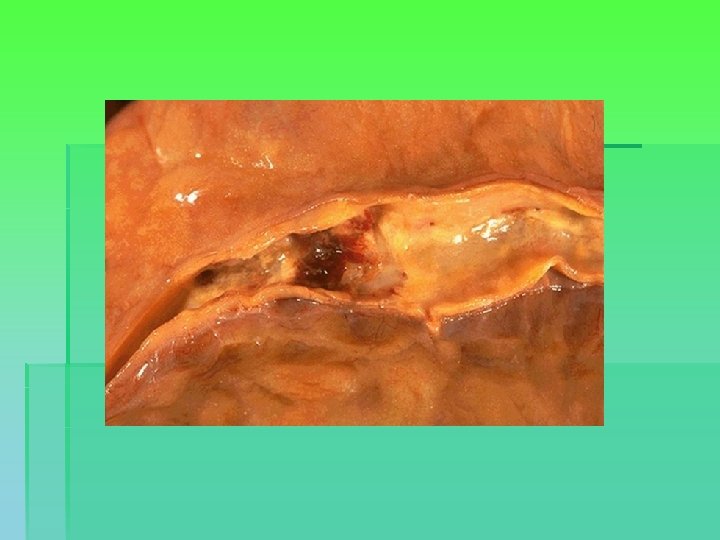
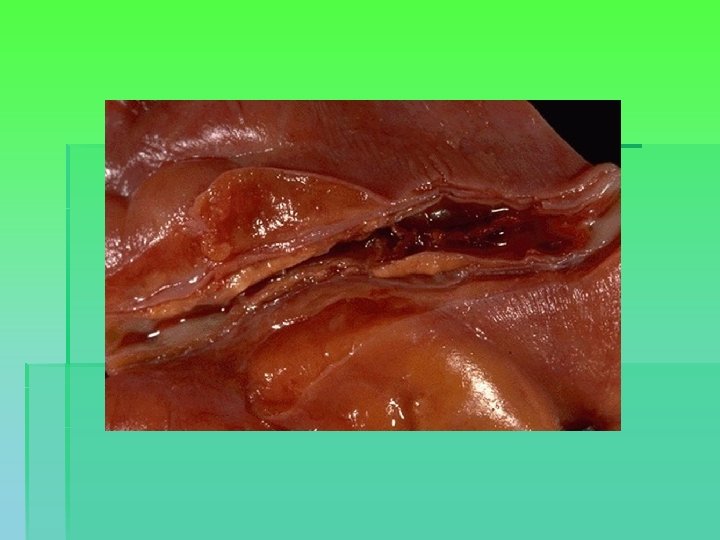
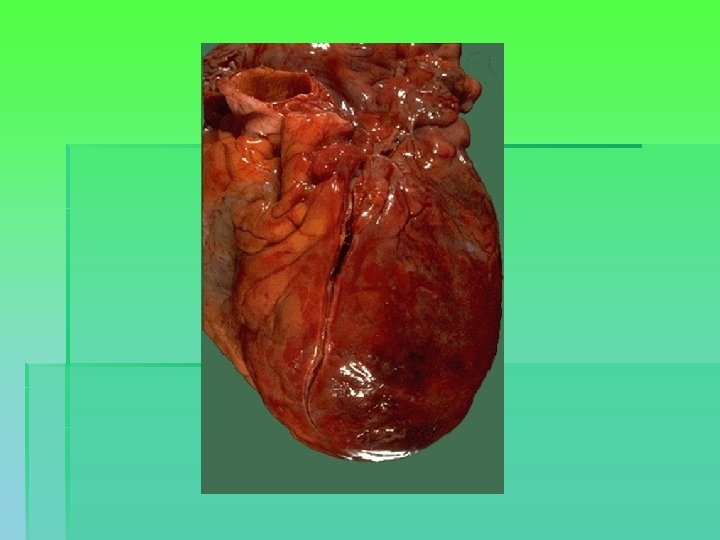

Myocardial infarction § Imbalance between oxygen supply and demand § Myocardial necrosis starts after 20 minutes § Border zone § Reperfusion within 3 -4 hours can limit the extent of myocardial necrosis § Scarring. LV systolic and diastolic dysfunction. Chronic heart failure.

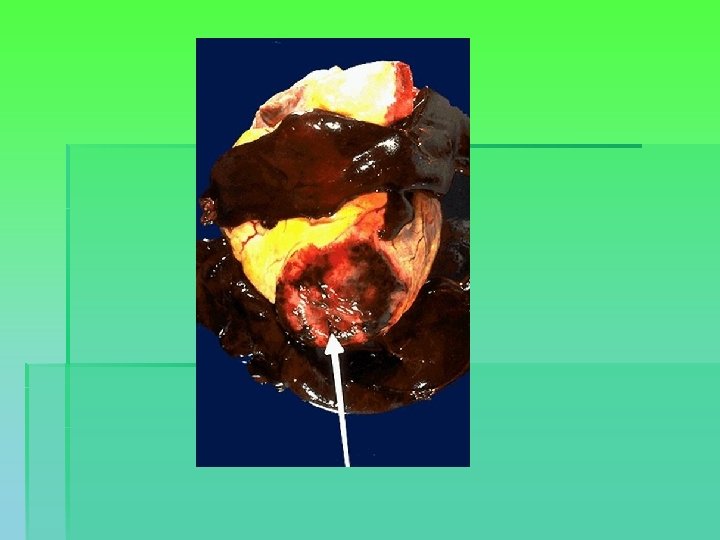

Diagnosis § Symptoms: Angina pectoris, acute myocardial infarction, chronic heart failure, sudden death, incidental finding on ECG § Noninvasive tests to identify and quantify CAD and sequelae: ECG, CXR, Labs, Exercise testing, Nuclear scans, Echocardiography, CT (Ca++)

Diagnosis § Associated conditions § Atherosclerosis: carotids, PAD § Definitive diagnosis: extent, distribution and severity of anatomic coronary artery disease § Coronary angiography § New modalities: CT (MRI)

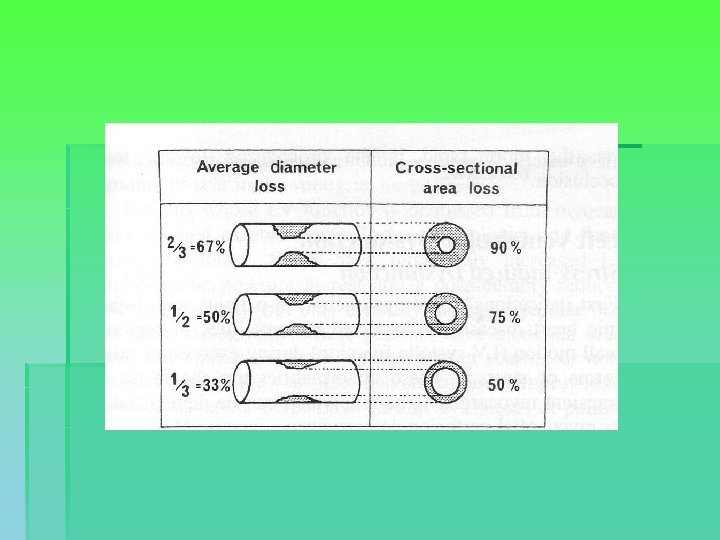
Coronary angiography § Grading of stenoses: § Moderate: 50% diameter = 75% crosssectional area loss § Severe: 67% diameter = 90% cross-sectional area loss § Distribution: § Single system / two system / three system § Left main
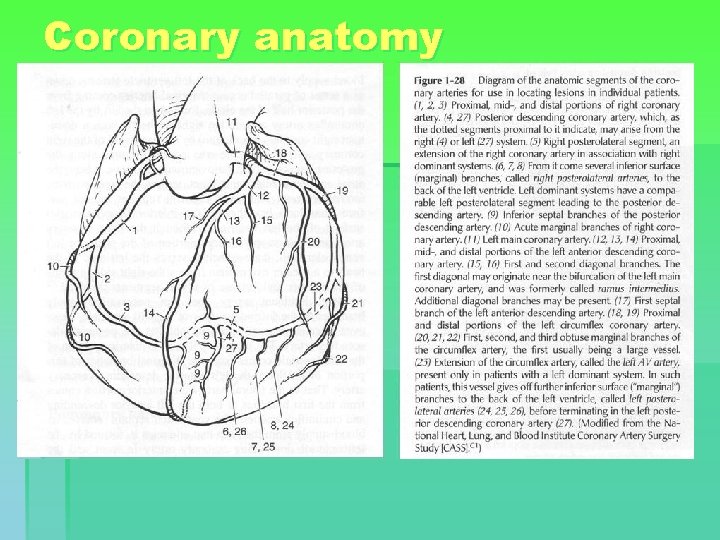
Coronary anatomy
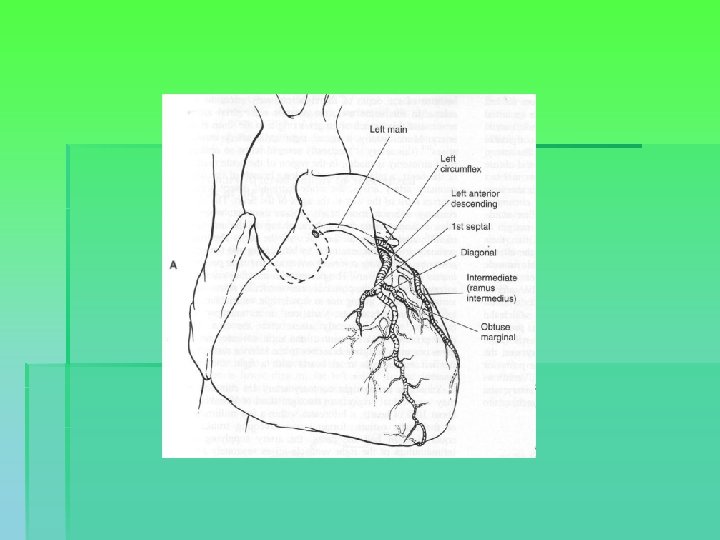
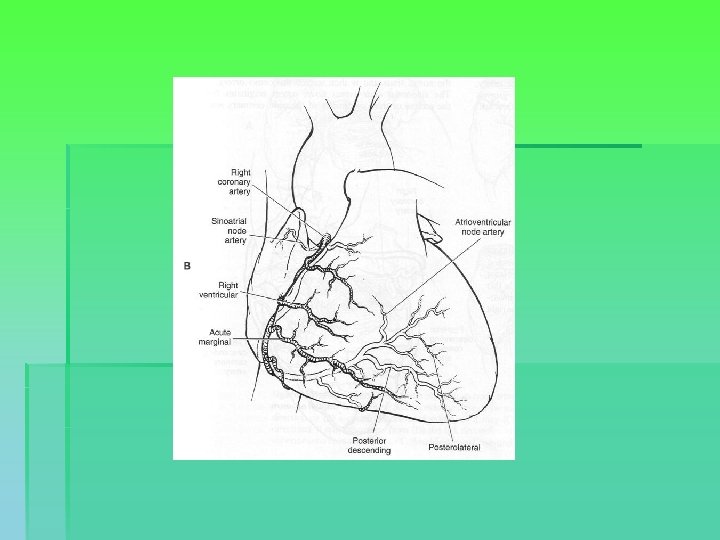
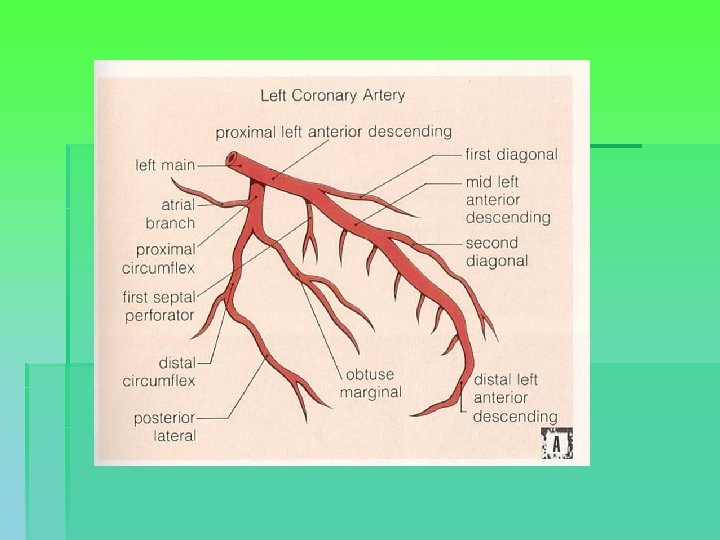
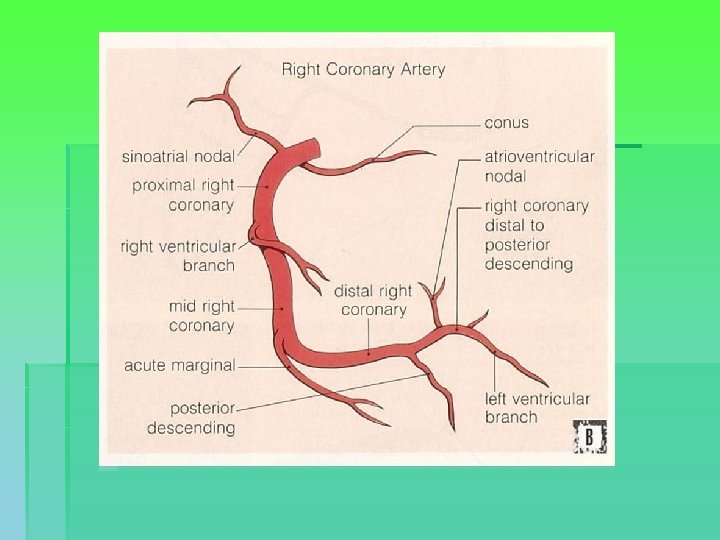
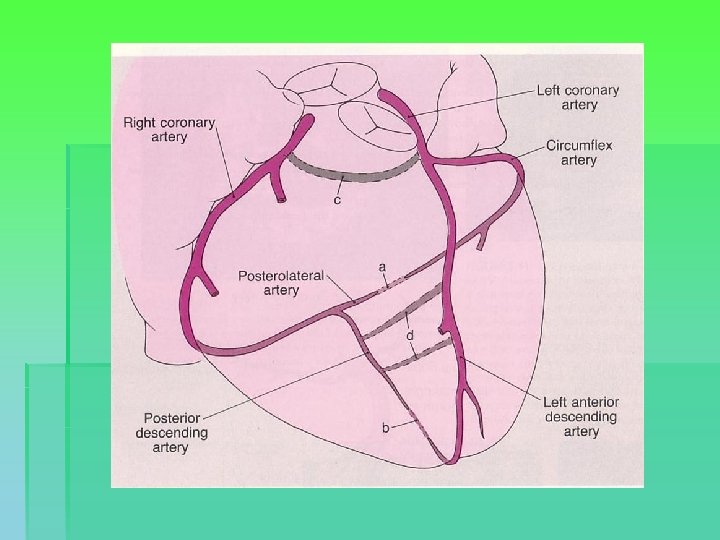

Indications for surgery § Comparative benefit of surgery relative to no treatment / medical treatment / PCI § Enormous variability in CAD, impacting on risk calculation → patient-specific predictions § General indications: § § § Left main or left main equivalent 3 system disease 2 system disease with severe prox. LAD and LVEF < 50% or ischemia on non-invasive testing § 1 or 2 system disease with large area of viable myocardium and high-risk criteria
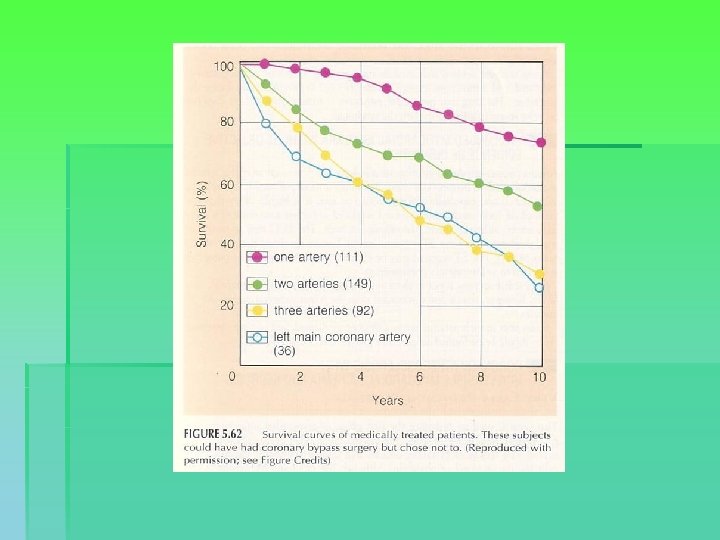

Bypass grafting § Full sternotomy and CPB (HLM): CABG § Full sternotomy, no CPB: OPCAB § Small sternotomy, parasternal access, thoracotomy, with or without CPB: e. g. MIDCAB

Bypass grafting § CABG = Golden standard and still most widely used (STS database ± 80%) § Objective: complete revascularisation by bypassing all severe stenoses in all affected coronary branches with ≥ 1 -1. 5 mm diameter § Most widely used conduits: LIMA, RIMA, SVG, radial artery, gastro-epiploic artery
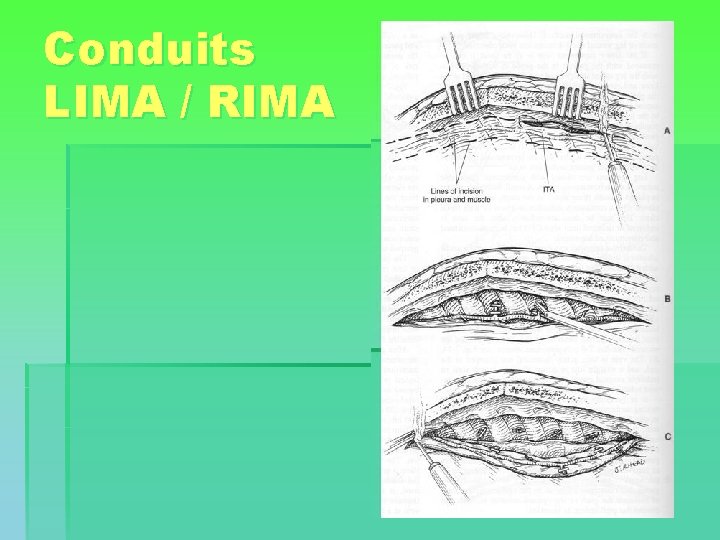
Conduits LIMA / RIMA
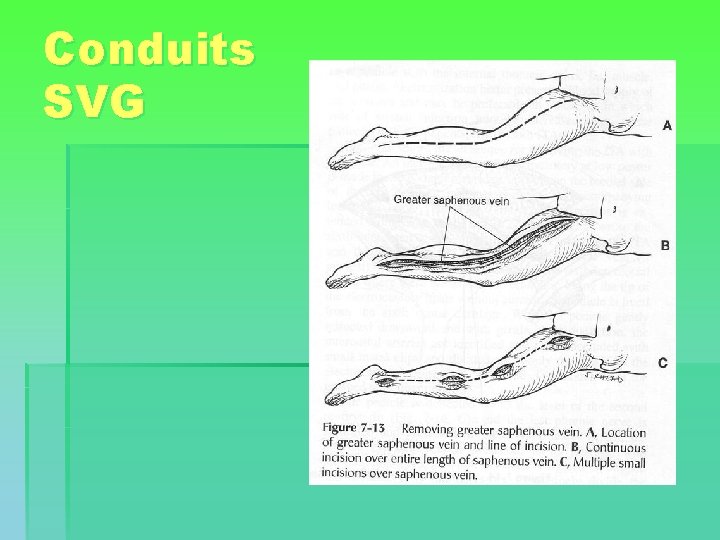
Conduits SVG

Conduits Radial
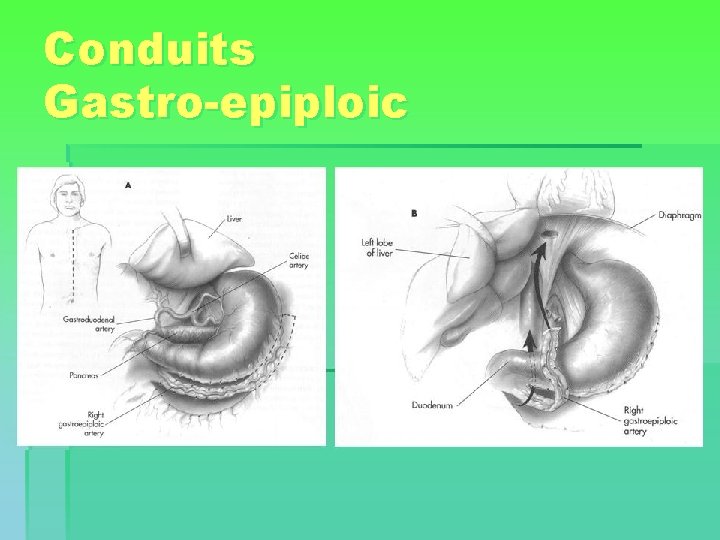
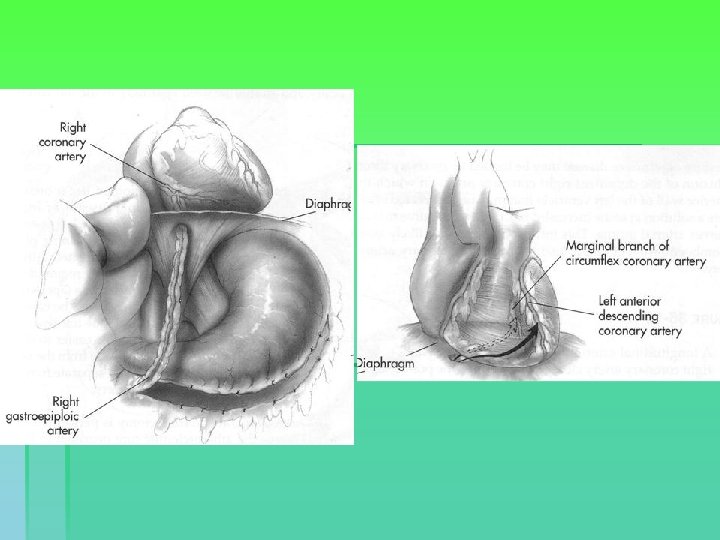
Conduits Gastro-epiploic
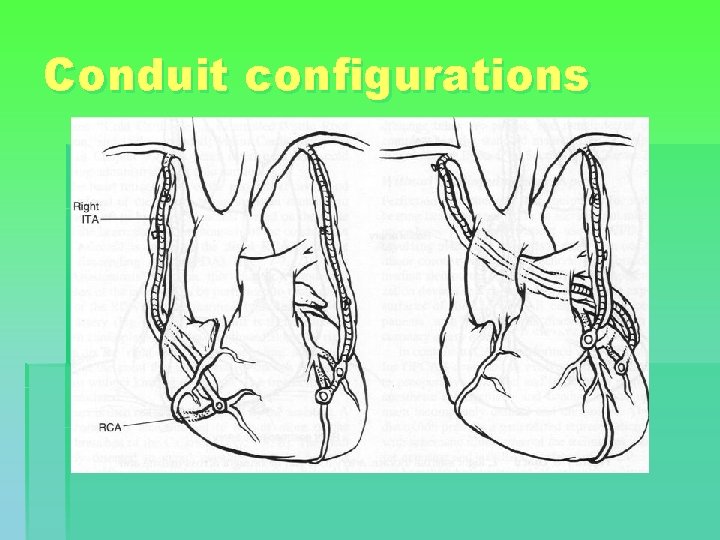
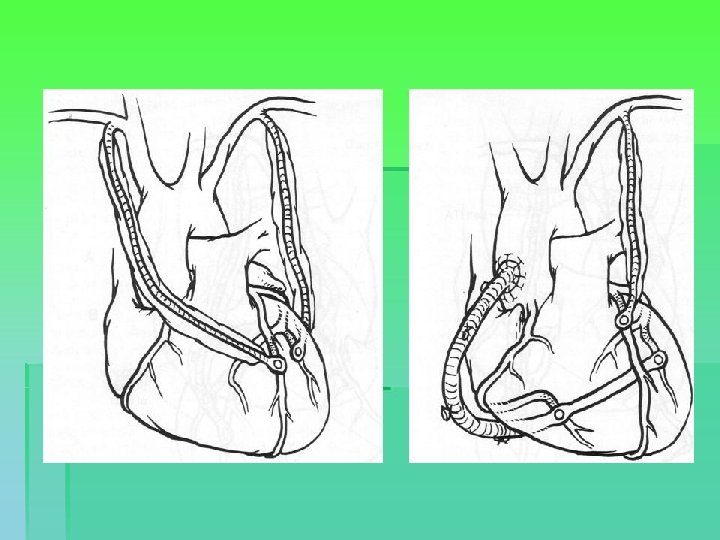
Conduit configurations
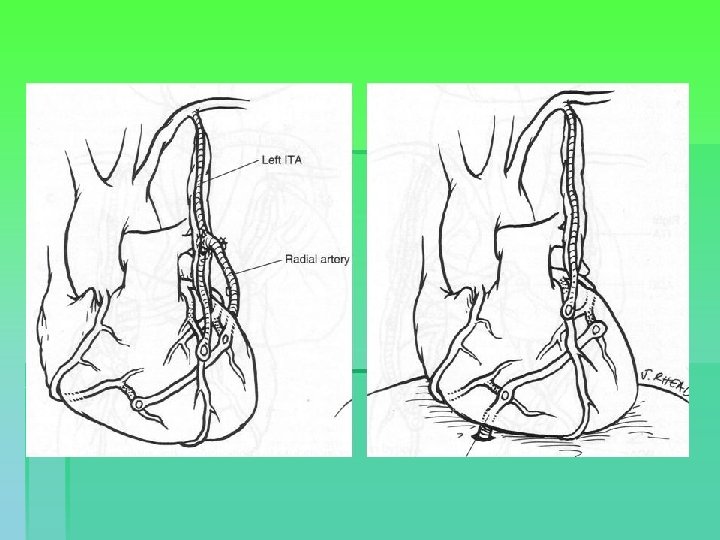

Endarterectomy

CABG § Median sternotomy § Conduit harvesting § Heparin, cannulation and CPB with mild to moderate hypothermia § Cross-clamping of the aorta and cardioplegia § Distal anastomoses. Rewarming started. § Cross-clamp removed. Proximal anast. using a partially occluding clamp. Clamp removed. De-airing. § CPB discontinued, cannulae removed, protamine. § Pacing wires, drainage tubes, hemostasis and closure.
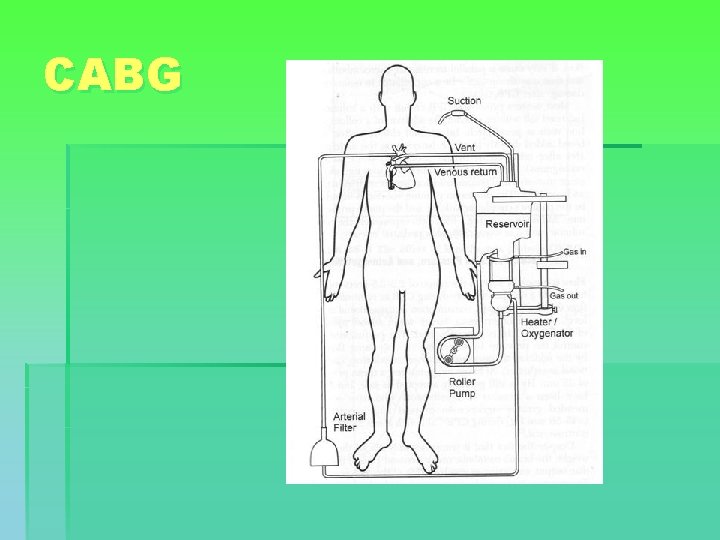
CABG
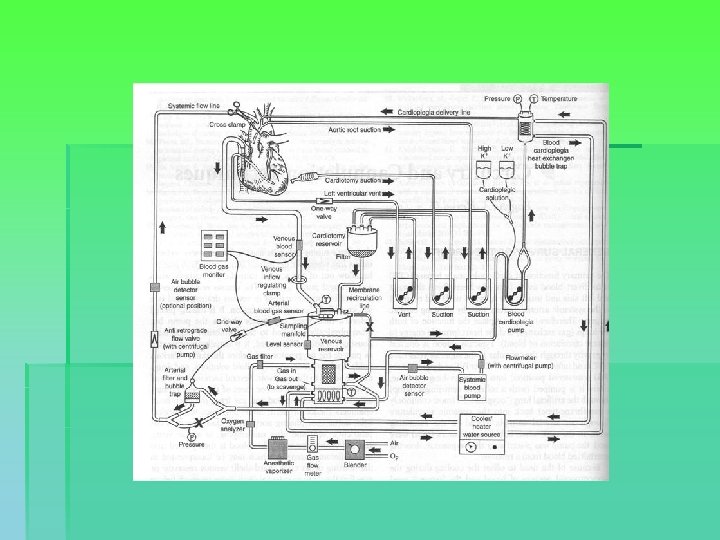
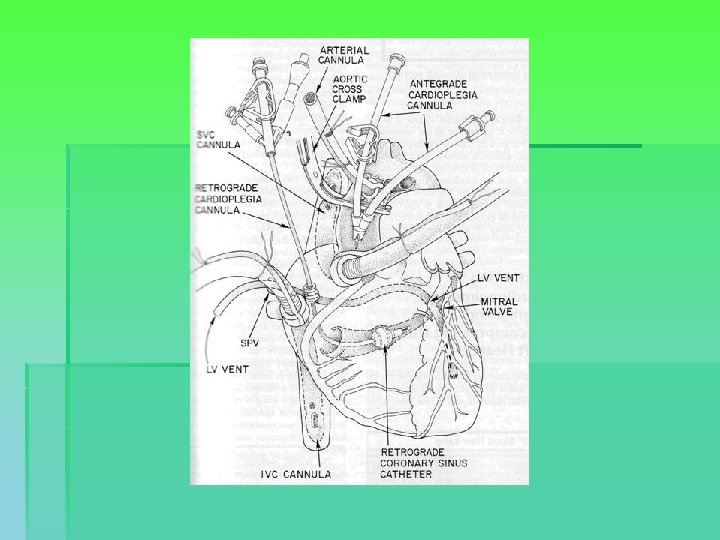

OPCAB § § § § § Attempt to maintain normothermia Median sternotomy Conduit harvesting Heparin. Pacing wires. Maneuvers to maintain hemodynamic stability (Trendelenburg, table, R pleura, . ) Pericardial sling Luxation. Stabilisation. Distal anastomoses with or without shunting. Proximal anastomoses. Protamine. Chest drains. Hemostasis. Closure.



Not discussed § § IABP and other support devices Emergency surgery Redo surgery Other modalities of bypass grafting: MIDCAB, robotic surgery, … § Adjunctive surgical treatment: TMLR, growth factors, cell transplantation § Combined surgery

Results § Early mortality can be predicted, using risk stratification models (Euroscore, STS) § Time-Related Survival, generally: § § § 1 month: 98% 1 year: 97% 5 year: 92% 10 year: 81% 15 year: 66% § NB: ± 25% of early and late deaths are not related to CAD or CABG
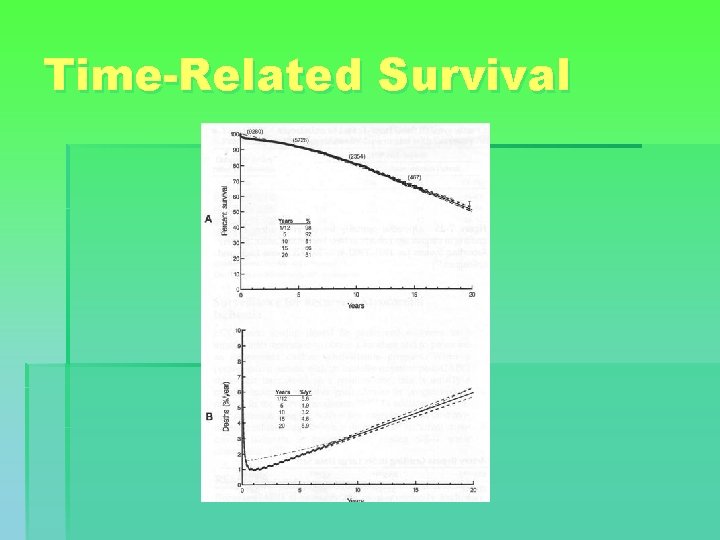
Time-Related Survival
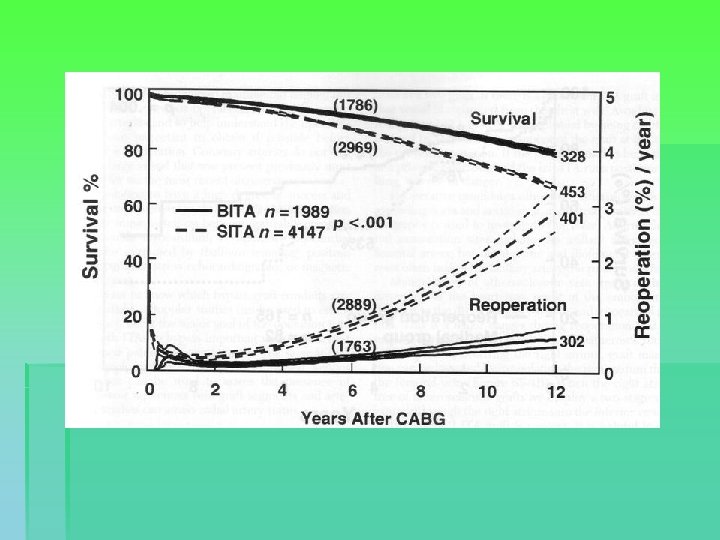

Results § § § Freedom from angina: 60% at 10 years Freedom from AMI: 86% at 10 years Freedom from sudden death: 97% at 10 years 80% of patients are working 1 year postop. Graft patency: § § LIMA (to LAD) ± 90% at 10 and 20 years. Radial artery ± 80% at 7 years Gastro-epiploic artery ± 60% at 10 years SVG ± 50 -60% at 10 years, 80% to LAD
- Slides: 48