Cord presentation This occurs when the umbilical cord

� Cord presentation � This occurs when the umbilical cord lies in front of the presenting part, with the fetal membranes still intact.

� The cord lies in front of the presenting part and the fetal membranes are ruptured � Occult cord prolapse � This is said to occur when the cord lies alongside, but not in front of, the presenting part.

high parity& High head : � High or ill-fitting presenting part: � If the membranes rupture spontaneously when the fetal head is high, a loop of cord may be able to pass between the uterine wall and the fetus resulting in its lying in front of the presenting part � -As the presenting part descends the cord becomes trapped and occluded. �

� The size of the fetus in relation to the pelvis and the uterus allows the cord to prolapse. � - Babies of very low birth weight (<1500 g) are particularly vulnerable for cord presentation.

The presenting part may not be engaged when the membranes rupture and malpresentation is more common. � Malpresentation � -Cord prolapse is associated with breech presentation, especially complete or footling breech. � -This relates to the ill-fitting nature of the presenting parts and also the proximity of the umbilicus to the buttocks. � -In this situation, the degree of compression may be less than with a cephalic presentation, but there is still a danger of asphyxia. �

� -Shoulder and compound presentation and transverse lie carry a high risk of prolapse of the cord, occurring with spontaneous rupture of the membranes. � -Face and brow presentations are less common causes of cord prolapse

� Multiple pregnancy � -Malpresentation, particularly of the second twin, is more common in multiple pregnancy. � -Polyhydramnios � The cord is liable to be swept down in a gush of liquor if the membranes rupture spontaneously. � -Controlled release of liquor during artificial rupture of the membranes is sometimes performed to try to prevent this.

� This is diagnosed on vaginal examination when the cord is felt behind intact membranes. � -It is, however, rarely detected but may be associated with aberrations in fetal heart monitoring such as decelerations, which occur if the cord becomes compressed.


� Under no circumstances should the membranes be ruptured. � -The midwife should discontinue the vaginal examination, in order to reduce the risk of rupturing the membranes. � -Medical aid should be summoned. To assess fetal well-being continuous electronic fetal monitoring should be commenced or the fetal heart should be auscultated as continuously as possible.

-The mother should be helped into a position that will reduce the likelihood of cord compression. � -Caesarean section is the most likely outcome. �

� Whenever there are factors present that predispose to cord prolapse a vaginal examination should be performed immediately on spontaneous rupture of membranes. � Bradycardia � - variable or prolonged decelerations of the fetal heart are associated with cord compression

� -The diagnosis of cord prolapse is made when the cord is felt below or beside the presenting part on vaginal examination. � -The cord may be felt in the vagina or in the cervical os or a loop of cord may be visible at the vulva


� the midwife should call for urgent assistance. � - The midwife should explain her findings and emergency measures that may be needed to the mother and her birth partner. � If an oxytocin infusion is in progress this should be stopped. � - If the cord lies outside the vagina, then it should be gently replaced to oxygenation

� prevent spasm � to maintain temperature � and prevent drying. � Administering oxygen to the mother by face mask at 4 L/min may improve fetal
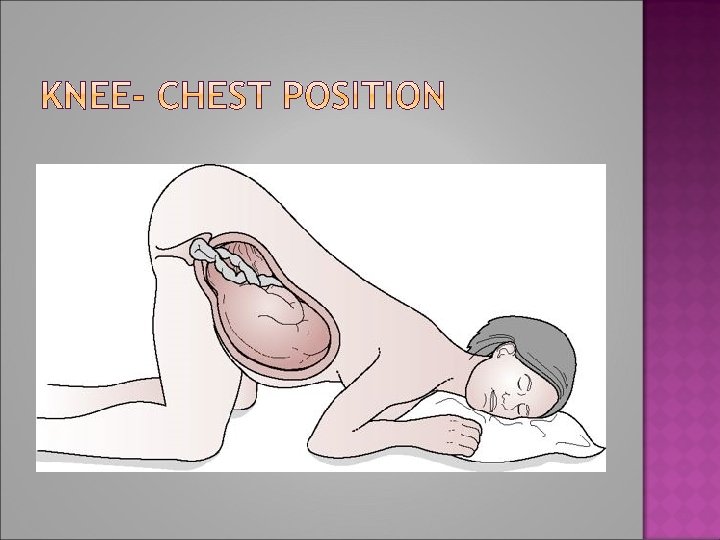

� -The risks to the fetus are hypoxia and death as a result of cord compression. � -The risks are greatest with prematurity and low birth weight � - The midwife may need to keep her fingers in the vagina and hold the presenting part off the umbilical cord, especially during a contraction. � -The mother can be helped to change position to further reduce pressure on the cord.

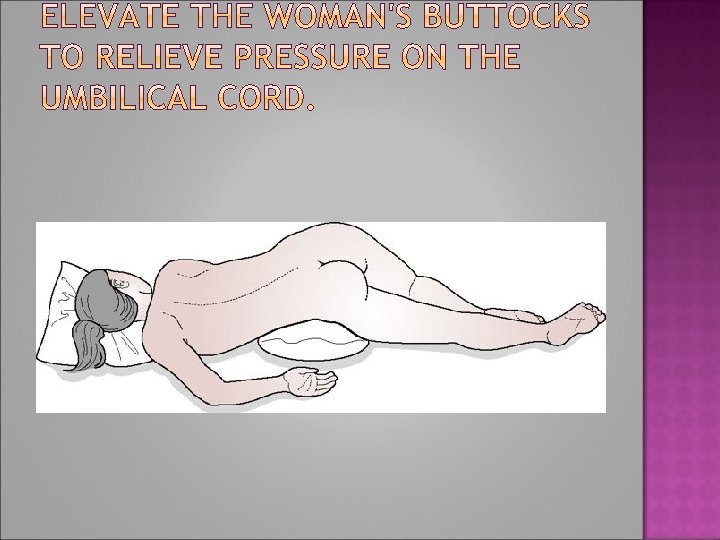
�- Raising her pelvis and buttocks or adopting the knee–chest position will cause the fetus to gravitate towards the diaphragm � - The foot of the bed may also be raised (Trendelenburg position) to relieve compression on the cord. � - Alternatively, the mother can be helped to lie on her left side, with a wedge or pillow elevating her hips (exaggerated Sims' position)

� -There is some evidence to suggest that bladder filling may also be an effective technique for managing cord prolapse � -A self-retaining 16 G Foley catheter is used to instil approximately 500– 700 m. L of sterile saline into the bladder. � -The full bladder can relieve compression of the cord by elevating the presenting part about 2 cm above the ischial spines

� -The bladder would be drained in theatre immediately before delivery. � -Birth must be expedited with the greatest possible speed to reduce the mortality and morbidity associated with this condition. � -Caesarean section is the treatment of choice in those instances where the fetus is still alive and vaginal birth is not imminent.

� -If cord prolapse is diagnosed in the second stage of labour, with a multiparous mother, the midwife may perform an episiotomy to expedite the birth. � -Where the presentation is cephalic, assisted birth may be achieved through ventouse or forceps. � -If cord prolapse occurs in the community, emergency transfer to hospital is essential.

�- The midwife should carry out the same procedures to relieve the compression on the cord. � -Consultant unit staff should be informed and be prepared to perform an emergency caesarean section.

- Slides: 25